Septic Pelvic Thrombophlebitis: Causes, Symptoms, and Treatment

Key points
- Ovarian Vein Thrombophlebitis: A localized clot and infection in an ovarian vein (usually the right).
- Deep Pelvic Septic Thrombophlebitis: A more diffuse clotting involving multiple smaller pelvic veins. This form is harder to visualize on imaging.
Introduction
Imagine a new mother who, after a difficult delivery, develops a persistent fever that doesn’t respond to the usual antibiotics. Doctors perform tests and discover an unusual culprit: an infected blood clot in her pelvic veins—a condition known as septic pelvic thrombophlebitis (SPT).
Septic pelvic thrombophlebitis—sometimes called postpartum ovarian vein thrombosis or puerperal ovarian vein thrombophlebitis—is a rare complication usually occurring after childbirth or pelvic surgery. “Thrombophlebitis” means inflammation of a vein due to a blood clot, and “septic” indicates an associated infection. In SPT, an infection in the pelvic region spreads to nearby veins, causing a clot that also becomes infected.
“We always consider septic pelvic thrombophlebitis in postpartum patients with persistent fever. Early recognition and treatment can be life-saving.” – Dr. Jane Smith, OB/GYN.
Although SPT is uncommon, it’s important for postpartum women and healthcare providers to be aware of it. Prompt treatment can cure the condition and prevent serious complications. Understanding the physiological changes that occur during pregnancy and the postpartum period helps clarify why certain women become vulnerable to venous stasis and subsequent thrombosis. The postpartum state is inherently prothrombotic, designed to protect against life-threatening hemorrhage during and immediately after delivery. However, when this natural protective mechanism intersects with bacterial invasion from a uterine or cervical source, the stage is set for a complex inflammatory and thrombotic cascade. Recognizing the subtle shifts in clinical presentation, from intermittent chills to unexplained tachycardia, allows clinicians to intervene before systemic sepsis or pulmonary complications develop. Patient education and vigilant postpartum monitoring remain the cornerstones of early detection.
*Video: Cardiovascular changes and complications like deep vein thrombosis and pulmonary embolism in maternity nursing.*What is Septic Pelvic Thrombophlebitis?
Septic pelvic thrombophlebitis is an inflammation of pelvic veins due to an infected thrombus (blood clot). It most commonly involves the ovarian veins, which drain blood from the ovaries. In about 80-90% of cases, the right ovarian vein is affected, likely due to anatomical differences. SPT was historically known as a cause of persistent postpartum fever that didn’t resolve with antibiotics alone.
The right ovarian vein is notably longer than its left counterpart and drains directly into the inferior vena cava at an acute angle, creating a hemodynamic environment more prone to sluggish blood flow and retrograde bacterial seeding. Additionally, the enlarged gravid uterus compresses the right common iliac vein more significantly during the third trimester, further contributing to venous stasis. When endometrial infection develops postpartum, bacteria readily ascend into the venous plexus surrounding the uterus and parametrial tissues. The resulting inflammatory response damages the endothelial lining of these vessels, triggering the coagulation cascade and forming a thrombus that becomes colonized by microorganisms. This process transforms a routine pelvic infection into a systemic vascular emergency.
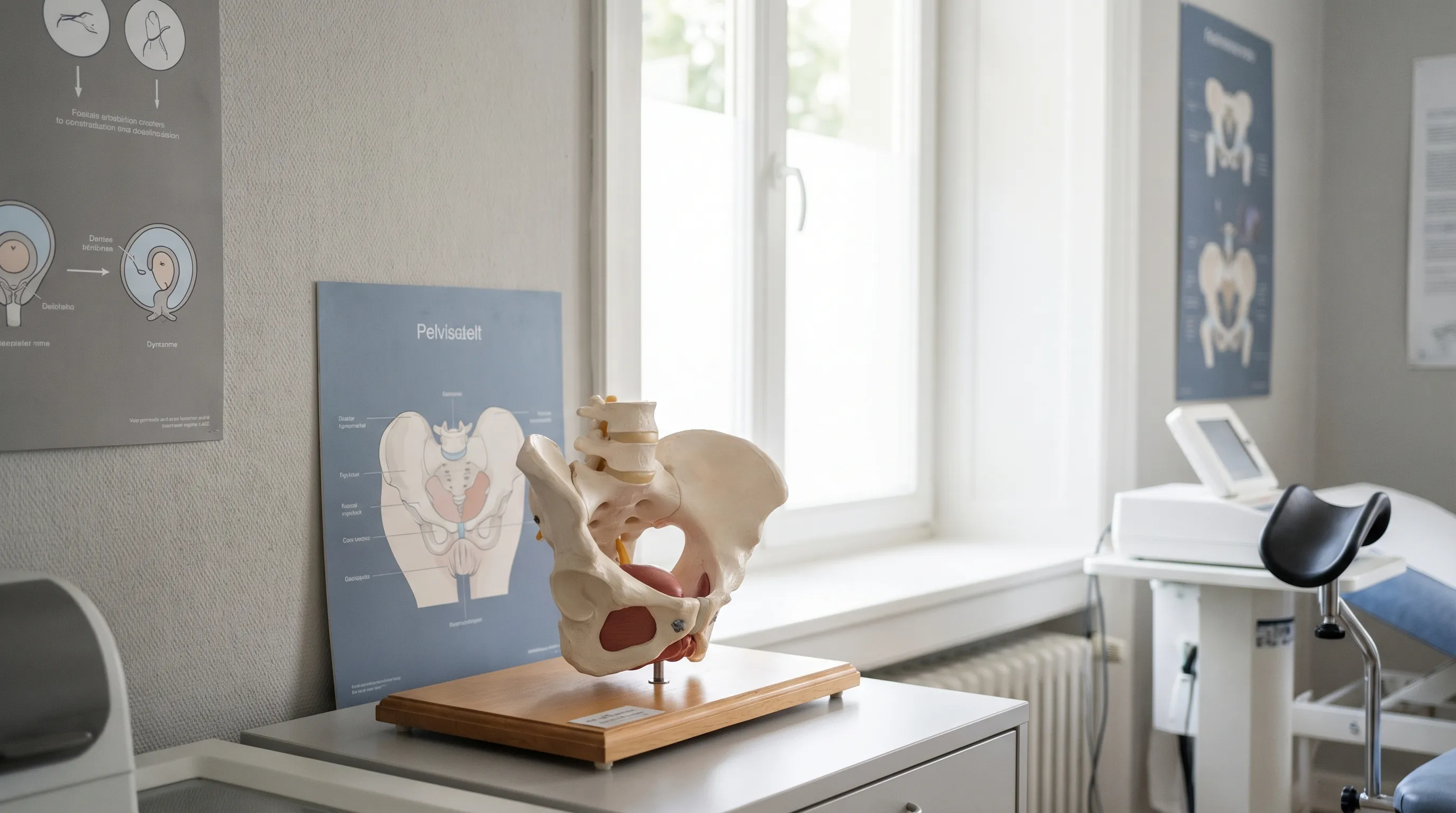 Image: Anatomy of the female reproductive system. Septic pelvic thrombophlebitis often involves a clot in the ovarian vein, typically on the right side.
Image: Anatomy of the female reproductive system. Septic pelvic thrombophlebitis often involves a clot in the ovarian vein, typically on the right side.
When and Why Does It Happen?
SPT usually occurs after childbirth (postpartum), especially following a C-section, and sometimes after pelvic surgery (like a hysterectomy). Here’s what typically happens:
- After delivery, bacteria can proliferate in the pelvic region, especially if there is an infection of the uterine lining (endometritis).
- These bacteria can invade the wall of a nearby vein, like the ovarian vein.
- The infection causes inflammation that triggers the formation of a blood clot (thrombophlebitis).
- The clot itself becomes a reservoir for the infection, defining it as septic pelvic thrombophlebitis.
The timeline of symptom onset typically falls between the second and seventh postpartum day, though cases have been documented up to two weeks following delivery or gynecological surgery. During labor and delivery, microtrauma to the cervical and vaginal tissues provides portals of entry for polymicrobial flora naturally residing in the lower genital tract. Once the placenta separates, the underlying decidual vessels are exposed, creating an ideal environment for bacterial proliferation if aseptic techniques are compromised or if prolonged rupture of membranes occurs. The subsequent inflammatory response releases cytokines that upregulate tissue factor expression, accelerating fibrin deposition and platelet aggregation. Without adequate venous flow, the localized clot becomes a nidus for continued microbial replication, perpetuating a cycle of fever, pain, and systemic inflammation.
How Common Is It?
SPT is quite rare, with estimates ranging from 1 in 3,000 to 1 in 10,000 deliveries. It may occur in up to 1-2% of women who develop severe postpartum endometritis. The incidence has declined significantly over the past few decades due to routine prophylactic antibiotic administration during cesarean sections and improved infection control practices in obstetric care. However, it remains an important diagnostic consideration in referral centers and high-risk maternity units. Epidemiological studies suggest a strong correlation with operative deliveries, with the rate rising to approximately 0.1-0.5% in women undergoing emergency or scheduled cesarean sections compared to vaginal births. Despite its rarity, SPT accounts for a disproportionate number of severe maternal morbidity cases when diagnosis is delayed.
Two Forms of SPT
Medical literature sometimes describes two forms:
- Ovarian Vein Thrombophlebitis: A localized clot and infection in an ovarian vein (usually the right).
- Deep Pelvic Septic Thrombophlebitis: A more diffuse clotting involving multiple smaller pelvic veins. This form is harder to visualize on imaging.
Both forms are managed similarly, and ovarian vein thrombophlebitis is the most common presentation. Deep pelvic septic thrombophlebitis, sometimes referred to as "silent" pelvic thrombophlebitis, presents with similar clinical features but often lacks focal abdominal signs or palpable masses. Imaging frequently reveals only subtle venous wall thickening or small, non-occlusive thrombi in the parametrial or paracervical venous plexuses. Because the deep pelvic form evades easy radiographic detection, diagnosis often relies more heavily on clinical response to therapeutic anticoagulation after antibiotics have failed to control fever. Clinicians must maintain a high index of suspicion when fever persists despite appropriate broad-spectrum coverage and negative workups for other common postpartum infectious sources.
Causes and Risk Factors
SPT is caused by a combination of infection and factors that promote clotting, known as Virchow’s triad:
- Hypercoagulability: Pregnancy and the postpartum period naturally make blood clot more easily to prevent hemorrhage during childbirth.
- Venous Stasis: Reduced mobility and the enlarged uterus can slow blood flow in pelvic veins.
- Endothelial Injury & Infection: Trauma from delivery or surgery can damage blood vessels. If bacteria from a uterine infection invade a vein, they cause inflammation that triggers clot formation.
The physiological adaptations of pregnancy profoundly impact all three components of Virchow’s triad. Plasma concentrations of coagulation factors I, II, VII, VIII, X, and von Willebrand factor increase significantly, while natural anticoagulants like protein S decrease. Simultaneously, progesterone-mediated venous smooth muscle relaxation reduces venous tone, while mechanical compression from the gravid uterus impedes venous return from the lower extremities and pelvis. When combined with the tissue disruption of delivery and the introduction of pathogenic or commensal bacteria into the sterile uterine cavity, these changes create a perfect storm for thrombotic infection. Microbiological cultures from affected veins most frequently isolate polymicrobial flora, including Bacteroides species, Peptostreptococcus, Gardnerella vaginalis, Escherichia coli, and Streptococcus species. The anaerobic predominance is particularly notable, reflecting the low-oxygen environment of necrotic decidua and thrombosed venous segments.
Common Risk Factors for SPT
- Postpartum Uterine Infection (Endometritis): The biggest risk factor, especially after a C-section.
- Cesarean Delivery: The risk of infection and clot formation is higher with surgery.
- Prolonged or Difficult Labor: Increases infection risk and pelvic trauma.
- Multiple Births or Large Uterus: Can stretch and compress pelvic veins.
- Pelvic Surgery: Procedures like hysterectomy can rarely lead to SPT if a post-surgical infection occurs.
- Pelvic Inflammatory Disease (PID): A severe PID can, in rare cases, cause SPT even in non-postpartum individuals.
Additional risk modifiers include maternal obesity, advanced maternal age, smoking history, and pre-existing inherited or acquired thrombophilias such as Factor V Leiden mutation or antiphospholipid syndrome. Prolonged intravenous catheterization, multiple cervical examinations during labor, internal fetal monitoring, and manual removal of the placenta further elevate the risk of introducing pathogens into the upper genital tract. Socioeconomic factors that delay access to prenatal or postpartum care also contribute to higher complication rates, as untreated subclinical infections can progress unchecked. Recognizing these overlapping risk factors enables healthcare teams to implement targeted surveillance and early intervention strategies for high-risk patients.
SPT almost never happens without an associated infection.
Symptoms and Signs
SPT symptoms can mimic other postpartum issues, making it tricky to diagnose. Key features include:
- Persistent Fever: This is the hallmark symptom. The fever continues for more than 48-72 hours despite broad-spectrum antibiotics, often spiking intermittently. Chills and malaise are common.
- Pelvic or Lower Abdominal Pain: Often localized to one side, frequently the right lower quadrant if the right ovarian vein is involved.
- Right-Sided Abdominal Mass or Tenderness: A tender, rope-like mass (the thrombosed vein) may occasionally be felt in the right lower abdomen.
- Tachycardia (Fast Heart Rate): The pulse is often elevated due to fever and infection.
- Symptoms of Pulmonary Embolism (in severe cases): If a piece of the clot travels to the lungs, it can cause chest pain, shortness of breath, and coughing. This is a life-threatening complication.
Beyond these classic manifestations, patients may experience nonspecific constitutional symptoms such as profound fatigue, night sweats, anorexia, and generalized weakness that interfere with early newborn care and breastfeeding initiation. Physical examination may reveal guarding or rebound tenderness over the affected ovarian vein pathway, though peritoneal signs are typically absent unless secondary bowel involvement or abscess formation occurs. The cervical motion tenderness and uterine subinvolution commonly seen in simple endometritis may persist or worsen. Importantly, the fever pattern in SPT is frequently "swinging" or spiking, often correlating with transient bacteremia episodes as microemboli seed the systemic circulation. Clinicians should carefully monitor vital signs and track temperature curves, as a sudden resolution of fever without anticoagulation initiation strongly suggests an alternative diagnosis, while rapid defervescence following heparin administration supports the SPT diagnosis.
The key red flag is a fever that does not resolve with standard antibiotic treatment.
*Video: Warning signs of blood clots that you need to know.*Diagnosis
Diagnosing SPT is challenging and often a process of exclusion after ruling out more common causes of postpartum fever like endometritis, urinary tract infections, and wound infections.
Clinical Suspicion
The diagnosis often begins with recognizing the pattern of a postpartum fever unresponsive to antibiotics. Historically, diagnosis was confirmed if the fever resolved after starting anticoagulants (blood thinners).
Modern clinical algorithms emphasize a stepwise approach. When a postpartum patient presents with persistent fever, clinicians first perform a comprehensive pelvic examination, assess surgical incisions or perineal lacerations for signs of infection, evaluate the breasts for mastitis, and order urinalysis and urine culture to exclude urinary tract pathology. Chest radiography may be utilized to rule out atelectasis or early pneumonia. If these investigations yield no definitive source and the patient fails to improve after 48-72 hours of appropriate parenteral antibiotic therapy, SPT moves to the forefront of the differential diagnosis. The therapeutic trial of anticoagulation, once a diagnostic cornerstone, is now largely replaced by confirmatory imaging due to the availability of advanced radiographic modalities. Nevertheless, rapid clinical improvement following heparin initiation remains a valuable supportive finding when imaging is equivocal or unavailable.
Imaging Studies
Modern imaging can directly visualize the clot:
- CT Scan: A CT scan of the abdomen and pelvis with contrast dye is one of the most effective methods to detect an ovarian vein thrombosis.
- MRI: An MRI with contrast is another excellent tool, particularly if CT contrast is contraindicated.
- Ultrasound: While less sensitive than CT or MRI, ultrasound can sometimes detect a clot in the ovarian vein, especially on the right side.
Contrast-enhanced CT typically reveals a dilated ovarian vein with a characteristic filling defect surrounded by a hyperenhancing venous wall, reflecting active inflammation. The clot may appear hypodense relative to the surrounding enhanced blood pool. MRI provides superior soft-tissue contrast without ionizing radiation, making it particularly advantageous in breastfeeding patients or those with contrast allergies. T2-weighted sequences can highlight edema within the vessel wall, while MR venography clearly delineates venous patency. Transabdominal or transvaginal Doppler ultrasound is often employed as a first-line, radiation-free screening tool, though its utility is limited by operator dependence, bowel gas interference, and the retroperitoneal location of the ovarian veins. When ultrasound results are inconclusive but clinical suspicion remains high, cross-sectional imaging should not be delayed.
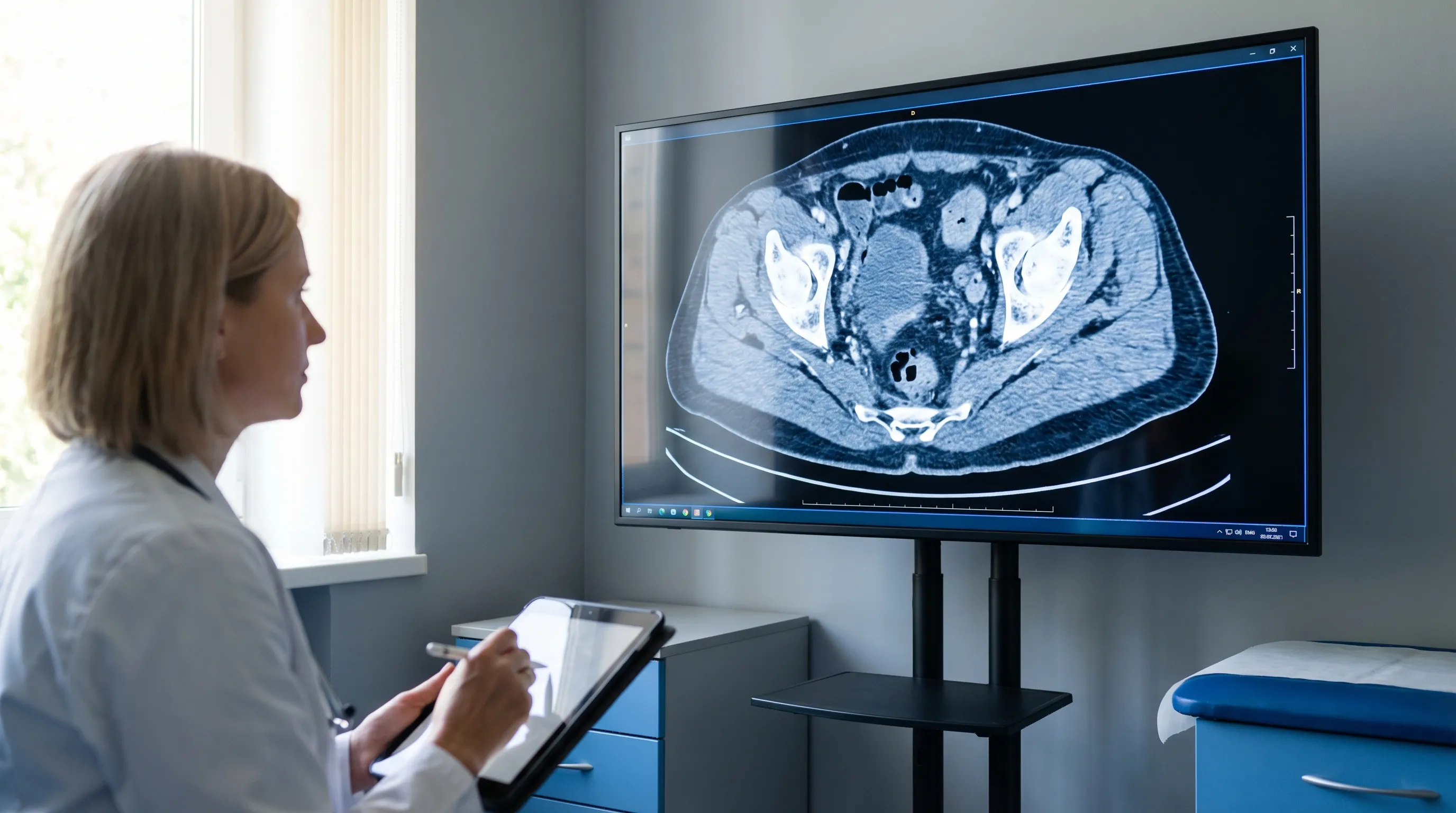 Image: CT scan showing pelvic venous structures. Modern imaging is vital for identifying septic pelvic thrombophlebitis.
Image: CT scan showing pelvic venous structures. Modern imaging is vital for identifying septic pelvic thrombophlebitis.
Laboratory Tests
Lab work can support the diagnosis but is not definitive:
- Blood Counts: Often show an elevated white blood cell count (WBC).
- Blood Cultures: May be positive for bacteria but can also be negative.
- Inflammatory Markers: C-reactive protein (CRP) and ESR are typically high.
- D-dimer: Usually elevated due to the clot, but it is also normally elevated in the postpartum period, making it non-specific.
A left shift in the differential white blood cell count, indicating increased band forms, often accompanies the leukocytosis and signals ongoing acute bacterial infection. Serial CRP measurements are highly valuable for tracking treatment response; a declining CRP trajectory typically parallels clinical improvement and can guide the transition from intravenous to oral antimicrobials. Liver function tests may occasionally show mild transaminitis or hypoalbuminemia as part of the systemic inflammatory response. Importantly, blood cultures are positive in only about 30-50% of SPT cases, largely due to prior antibiotic exposure and the localized, sequestered nature of the thrombus-bound infection. A comprehensive metabolic panel should be obtained to establish renal function prior to initiating nephrotoxic antibiotics or contrast imaging. Urine pregnancy testing or serial quantitative beta-hCG monitoring may also be considered in atypical presentations to exclude retained products of conception or gestational trophoblastic disease, which can occasionally present with overlapping clinical features.
Treatment
Treatment for SPT targets both the infection and the blood clot.
1. Antibiotic Therapy
Broad-spectrum intravenous (IV) antibiotics are used to cover the wide range of bacteria that cause postpartum infections. Common regimens include:
- Clindamycin and Gentamicin: A standard combination for endometritis.
- Piperacillin-tazobactam or a carbapenem: Used for broader coverage or more severe cases.
Antibiotics should ideally be initiated as soon as blood cultures are drawn, with empirical coverage targeting Gram-negative rods, anaerobes, and facultative Gram-positive cocci. The addition of ampicillin is sometimes warranted if enterococcal coverage is deemed necessary, particularly in patients with prolonged membrane rupture or multiple prior antibiotic exposures. Dosing adjustments are critical in the postpartum period due to rapid shifts in extracellular fluid volume, glomerular filtration rate normalization, and potential renal or hepatic impairment secondary to severe infection. Renal function and gentamicin trough levels should be monitored closely to prevent ototoxicity or nephrotoxicity. Antimicrobial stewardship principles guide the de-escalation of therapy once culture sensitivities return or when clinical stability is achieved.
Antibiotics are typically given for 7-10 days, sometimes transitioning from IV to oral medication to complete the course as detailed in professional guides like the Merck Manual.
2. Anticoagulation (Blood Thinners)
Anticoagulants are crucial to stop the clot from growing, help the body dissolve it, and prevent pulmonary embolism.
- IV Heparin or Low Molecular Weight Heparin (LMWH): Treatment is usually started with an injectable anticoagulant like unfractionated heparin or enoxaparin (LMWH).
- Transition to Oral Anticoagulant: Patients may be transitioned to an oral medication like warfarin for the remainder of the treatment course.
- Duration: Anticoagulation typically continues for 6 weeks to 3 months, similar to the treatment for a deep vein thrombosis (DVT).
LMWH is generally preferred over unfractionated heparin due to its more predictable pharmacokinetics, once- or twice-daily dosing, lower risk of heparin-induced thrombocytopenia, and compatibility with breastfeeding. Direct oral anticoagulants (DOACs) such as rivaroxaban or apixaban are increasingly utilized in non-lactating patients due to their oral administration and lack of monitoring requirements, though data on their safety during breastfeeding remains limited. Warfarin requires careful INR monitoring and is highly compatible with breastfeeding, as it does not cross into breast milk in clinically significant amounts. The choice of anticoagulant is individualized based on patient comorbidities, renal function, bleeding risk, cost, and postpartum recovery trajectory.
3. Supportive Care
Patients often receive supportive care in the hospital, including:
- Fever control with medications like acetaminophen.
- IV fluids for hydration.
- Pain relief.
- Monitoring for complications.
Adequate hydration is essential to maintain optimal intravascular volume and support renal clearance of inflammatory byproducts and antibiotic metabolites. Antipyretics improve maternal comfort and facilitate early mobilization, which in turn promotes venous return. Nutritional support, often involving consultation with a registered dietitian, helps meet the increased metabolic demands of infection, healing, and lactation. Lactation specialists can assist with establishing feeding routines while the patient receives treatments, as most antibiotics and LMWH are considered safe for nursing. Psychological support should not be overlooked; a complicated postpartum course can precipitate anxiety, depression, or feelings of maternal inadequacy, warranting early social work or psychiatric consultation when indicated.
4. Rare Interventions
Surgery is rarely needed but may be considered in extreme cases where medical therapy fails. An IVC filter, which catches clots before they reach the lungs, may be placed if anticoagulation is contraindicated.
Surgical options include ovarian vein ligation, thrombectomy, or even hysterectomy with bilateral salpingo-oophorectomy in catastrophic, life-threatening scenarios involving necrotizing infection or uncontrollable hemorrhage. These interventions are reserved for patients who exhibit clinical deterioration despite optimal medical management, develop large abscesses requiring drainage, or experience recurrent septic pulmonary emboli while on therapeutic anticoagulation. Endovascular techniques, such as catheter-directed thrombolysis, are occasionally explored in refractory cases but carry significant bleeding risks in the immediate postpartum period. Multidisciplinary tumor boards or maternal-fetal medicine, hematology, interventional radiology, and vascular surgery consensus is typically required before proceeding with invasive procedures.
The combination of antibiotics and anticoagulation is highly effective. A patient's fever often resolves within 48-72 hours of starting heparin.
Recovery and Prognosis
With timely treatment, the prognosis for SPT is excellent. Most women make a full recovery without long-term consequences.
Recovery Timeline
- Within Days: Fever and pain typically improve within 2-3 days of starting treatment.
- Several Weeks: The body gradually dissolves the clot over 4-6 weeks. Anticoagulation is often discontinued after 6 weeks to 3 months.
- Long-Term: There are usually no lasting health issues. Fertility is generally not affected.
Follow-up appointments are typically scheduled within one to two weeks of hospital discharge to assess wound healing, review laboratory trends, and evaluate tolerance to oral medications. Repeat imaging is not routinely required unless symptoms recur or the patient exhibits signs of treatment failure. Serial ultrasound or CT scans may be ordered at the completion of anticoagulant therapy in complex cases to document venous recanalization, though many thrombosed veins remain chronically occluded without causing clinical sequelae. Gradual resumption of normal activities is encouraged, with specific guidance provided regarding heavy lifting, strenuous exercise, and prolonged immobility. Most patients report a full return to baseline energy levels and physical function within four to six weeks post-treatment initiation.
Potential Complications if Untreated
- Pulmonary Embolism (PE): The most serious risk, where a piece of the clot travels to the lungs.
- Extension of Clot: The clot could grow into larger veins.
- Persistent Infection/Abscess: The infection could spread or form an abscess requiring drainage.
Other potential complications include sepsis with multi-organ dysfunction, septic arthritis or vertebral osteomyelitis from hematogenous seeding, pelvic abscess formation, ovarian vein rupture with retroperitoneal hemorrhage, and chronic pelvic pain secondary to venous hypertension or adhesions. The development of post-thrombotic syndrome is theoretically possible but exceedingly rare in the pelvic venous system due to the extensive collateral venous drainage. Early recognition and aggressive management drastically mitigate these risks, transforming what was once a frequently fatal condition into a highly manageable postpartum complication.
Future Pregnancies
Having SPT once may place you at a higher risk for clots in future pregnancies. Your doctor may recommend preventive measures, such as prophylactic heparin shots, after subsequent deliveries.
A thorough thrombophilia workup may be indicated, particularly if the event occurred without classic obstetric risk factors or if there is a strong personal or family history of venous thromboembolism. Genetic counseling can help clarify inheritance patterns and recurrence probabilities. For subsequent pregnancies, obstetricians typically recommend close antenatal surveillance, early postpartum ambulation protocols, mechanical prophylaxis with graduated compression stockings, and extended postpartum anticoagulation prophylaxis. The mode of future deliveries is determined by standard obstetric indications rather than SPT history alone, as successful vaginal births are entirely possible after prior SPT episodes.
Can Septic Pelvic Thrombophlebitis be Prevented?
There is no guaranteed way to prevent SPT, but certain measures can reduce the risk:
- Prevent and Treat Infections Promptly: Giving prophylactic antibiotics during C-sections is standard practice. Any postpartum signs of infection (fever, foul discharge) should be reported immediately.
- Early Mobilization: Getting up and walking soon after delivery helps improve blood flow and reduce clot risk.
- Hydration: Staying well-hydrated is important for circulatory health.
Institutional quality improvement initiatives focus on standardized perioperative antibiotic timing, typically administered within 60 minutes prior to surgical incision, and redosing protocols for prolonged procedures. Sequential compression devices (SCDs) should be applied preoperatively and worn continuously during hospitalization for cesarean deliveries. Enhanced recovery after cesarean (ERAC) protocols emphasize early oral intake, scheduled analgesia, and supervised ambulation within 12-24 hours post-surgery to minimize venous stasis. Patient education pamphlets distributed at discharge should clearly outline warning signs of infection, proper wound care techniques, and guidelines for when to contact a healthcare provider. Community-based postpartum support programs can bridge care gaps for high-risk populations, ensuring timely follow-up and adherence to prophylactic measures.
Awareness among both patients and providers is key to catching any potential complications early.
Expert Insights and Quotes
Dr. Maria Gonzalez, MD, Maternal-Fetal Medicine Specialist: “Septic pelvic thrombophlebitis is uncommon, but it’s something we keep at the back of our minds for a postpartum patient with fever. The classic scenario is a woman who had a tough delivery or C-section, develops endometritis, is on the right antibiotics, yet the fever isn’t going away. That’s when we say, okay, let’s look for an ovarian vein clot.”
Dr. Alan Thompson, MD, Radiologist: “From a radiologist’s perspective, identifying ovarian vein thrombosis on a CT scan is crucial because it changes management. If I see a dilated ovarian vein with a clot in a postpartum woman, I call the obstetric team right away. We know that adding anticoagulation to the treatment regimen will likely cure the patient.”
The collaborative approach emphasized by these specialists underscores the necessity of clear communication between radiologists, obstetricians, infectious disease specialists, and pharmacists. Multidisciplinary rounds during the initial hospitalization ensure that treatment plans are dynamically adjusted based on daily clinical response, laboratory trends, and imaging findings. This integrated model of care not only optimizes maternal outcomes but also streamlines hospital stays and reduces readmission rates. Ongoing education for residents and midwives on recognizing atypical presentations of postpartum fever remains vital for sustaining low complication rates and maintaining high standards of maternal safety.
Resources and Further Reading
- Radiopaedia – Ovarian Vein Thrombosis: An article with imaging examples of ovarian vein thrombosis. (ovarian vein thrombosis)
- Merck Manual (Professional) – Septic Pelvic Thrombophlebitis: A professional overview of the condition. (Merck Manual)
- Medscape – Septic Pelvic Thrombophlebitis: An in-depth article intended for healthcare professionals. (septic pelvic thrombophlebitis)
- Review Article (PDF): “Septic pelvic thrombophlebitis: a review of the literature” – An open-access review from the National Institutes of Health. (Download PDF via PMC)
- Wikipedia – Ovarian Vein Thrombosis: A general overview that overlaps with SPT. (Wikipedia)
Frequently Asked Questions
How long does it take for septic pelvic thrombophlebitis to fully resolve?
Clinical symptoms such as fever and localized pain typically improve within 48 to 72 hours after initiating combined antibiotic and anticoagulant therapy. However, complete radiographic resolution of the thrombus and normalization of inflammatory markers can take several weeks to a few months. Most patients complete a 7-10 day course of antibiotics and continue anticoagulation for 6 weeks to 3 months to ensure full stabilization and prevent clot propagation.
Is septic pelvic thrombophlebitis hereditary or genetic?
The condition itself is not inherited, as it is an acquired complication of infection and postpartum physiological changes. However, underlying inherited thrombophilias such as Factor V Leiden, prothrombin gene mutation, or protein C and S deficiencies can significantly increase an individual's susceptibility to developing venous thrombosis. If SPT occurs without typical obstetric risk factors, clinicians may recommend a genetic or hematologic workup to identify these predisposing conditions.
Can I breastfeed while being treated for this condition?
Yes, breastfeeding is generally safe and strongly encouraged during treatment. Low molecular weight heparin (LMWH), warfarin, and the most commonly used broad-spectrum antibiotics for SPT do not pass into breast milk in clinically significant amounts and are considered compatible with lactation. It is important to inform your healthcare provider that you are nursing so they can select medications with established safety profiles and adjust dosing if necessary to support optimal milk production.
What are the warning signs that the condition is not improving?
If fever persists or spikes higher after 3-4 days of appropriate treatment, or if you develop worsening abdominal pain, new-onset shortness of breath, chest pain, rapid heart rate, lightheadedness, or increased swelling in your legs, seek immediate medical attention. These symptoms may indicate treatment failure, secondary abscess formation, or a pulmonary embolism, all of which require urgent clinical reassessment and potential adjustment of your therapeutic regimen.
Will septic pelvic thrombophlebitis affect my ability to get pregnant again?
In the vast majority of cases, SPT does not impact future fertility or pregnancy outcomes. The ovaries and uterine blood supply typically remain fully functional, and most women go on to conceive normally. However, because a prior episode indicates a higher baseline risk for venous thromboembolism during pregnancy, your obstetric provider will likely recommend a tailored prophylactic plan for any subsequent pregnancies to ensure both maternal and fetal safety.
Conclusion
Septic pelvic thrombophlebitis is a rare but critical diagnosis to be aware of in the postpartum period. While it represents a serious complication, the encouraging news is that it is highly treatable once recognized. Most women recover quickly and completely with a combination of antibiotics and anticoagulants. The evolution of maternal medicine, coupled with advanced imaging techniques and refined antimicrobial stewardship, has transformed what was historically a life-threatening diagnosis into a manageable clinical entity. Ongoing research continues to optimize anticoagulant dosing protocols, evaluate the efficacy of direct oral anticoagulants in breastfeeding populations, and refine diagnostic algorithms to minimize unnecessary radiation exposure while maximizing detection accuracy.
If you have recently given birth, pay close attention to your body. A persistent high fever, severe pain, or any symptom that feels wrong should prompt a call to your healthcare provider. Advocating for your health by asking questions can ensure that rare conditions like SPT are considered and diagnosed promptly. Maintaining open dialogue with your care team, adhering to prescribed treatment regimens, and attending all scheduled postpartum follow-up appointments are essential steps toward a smooth and healthy recovery. Remember that every postpartum journey is unique, and vigilance paired with professional guidance offers the best path forward.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. If you have concerns about your health, please consult a qualified healthcare professional.

About the author
Sofia Rossi, MD, is a board-certified obstetrician-gynecologist with over 15 years of experience in high-risk pregnancies and reproductive health. She is a clinical professor at a top New York medical school and an attending physician at a university hospital.