Blown Vein: A Comprehensive Guide to Causes, Treatment, and Healing

Key points
- Skin Discoloration: The area will likely look red, purple, or blue due to the blood pooling under the skin. The color progression follows the natural breakdown of hemoglobin: starting as bright red or deep purple as oxygen-rich blood escapes, transitioning to blue or green as it degrades into biliverdin, and finally fading to yellow or brown before disappearing entirely.
- Swelling: Leaked fluid and blood cause the area to become puffy and swollen. Edema develops rapidly as interstitial fluid accumulates alongside the extravasated blood. The swelling is usually localized but can spread slightly depending on the volume of leakage and tissue laxity.
- Pain and Tenderness: The site may be sore, tender to the touch, or have a stinging sensation. The pain is typically described as a dull, throbbing ache or a sharp pressure that peaks within the first few hours and gradually diminishes as the hematoma stabilizes.
- Firmness: You might feel a firm lump under the skin, which is the collected blood (hematoma). As the blood clots, the lump often feels rubbery or firm to the touch. Over several days, as the body reabsorbs the trapped blood, the firmness will soften and gradually flatten.
- Tight Skin: The swelling may cause the skin to feel tight or stretched. This sensation usually correlates with the degree of edema and resolves naturally as fluid is reabsorbed into the lymphatic and venous systems.
Whether you've just had a blood draw or an IV line placed, seeing a dark bruise bloom under your skin can be alarming. This common occurrence is often due to a "blown vein." While the term sounds dramatic, it's typically a minor injury that heals on its own. Venipuncture and intravenous catheterization are among the most common medical procedures performed worldwide, and despite the skill of trained professionals, vessel injury remains a well-documented possibility. Understanding the underlying mechanics, recognizing the signs of proper healing, and knowing how to respond can transform an anxiety-inducing experience into a manageable one.
This comprehensive guide will walk you through what a blown vein is, what it looks and feels like, its causes, and how to treat it. We'll also cover the difference between a blown and a collapsed vein and explain when it's time to see a doctor. By exploring the physiological processes involved, reviewing evidence-based home care strategies, and highlighting preventive measures for both patients and clinicians, you'll gain the knowledge needed to navigate post-procedure recovery with confidence.
What is a Blown Vein?
A blown vein, medically known as a ruptured vein, happens when a needle punctures a vein and exits through the other side, causing blood to leak into the surrounding soft tissue. This leakage is what creates the characteristic bruise, or hematoma, under the skin. It's a frequent and usually harmless complication of intravenous (IV) therapy and venipuncture (blood draws). The venous system consists of thin-walled, low-pressure vessels designed to return deoxygenated blood to the heart. Unlike arteries, which have thick, muscular walls to withstand high-pressure systolic flow, veins have relatively fragile endothelial linings and less structural reinforcement. This anatomical reality makes them inherently susceptible to accidental perforation during needle insertion.
According to the Cleveland Clinic, a blown vein is a mild injury that occurs when something goes wrong during needle insertion. Once it happens, that vein cannot be used again until it has fully healed. The body immediately initiates its natural hemostatic response to contain the bleeding. Platelets aggregate at the site of the breach, and the coagulation cascade releases fibrin to form a temporary clot. Simultaneously, the leaked blood triggers a localized inflammatory reaction, bringing white blood cells to clear damaged tissue and growth factors to initiate vascular repair. In clinical settings, healthcare providers are trained to recognize the subtle signs of a blown vein—such as sudden loss of blood return in the catheter hub, immediate localized swelling, or patient-reported sharp discomfort—and respond promptly to minimize tissue irritation. While the visual presentation can be striking, the underlying physiology is a routine healing process that the body handles efficiently in the vast majority of cases.
What Does a Blown Vein Look and Feel Like? (Symptoms)
When a vein is blown, symptoms appear quickly at and around the needle insertion site. You can expect to experience:
- Skin Discoloration: The area will likely look red, purple, or blue due to the blood pooling under the skin. The color progression follows the natural breakdown of hemoglobin: starting as bright red or deep purple as oxygen-rich blood escapes, transitioning to blue or green as it degrades into biliverdin, and finally fading to yellow or brown before disappearing entirely.
- Swelling: Leaked fluid and blood cause the area to become puffy and swollen. Edema develops rapidly as interstitial fluid accumulates alongside the extravasated blood. The swelling is usually localized but can spread slightly depending on the volume of leakage and tissue laxity.
- Pain and Tenderness: The site may be sore, tender to the touch, or have a stinging sensation. The pain is typically described as a dull, throbbing ache or a sharp pressure that peaks within the first few hours and gradually diminishes as the hematoma stabilizes.
- Firmness: You might feel a firm lump under the skin, which is the collected blood (hematoma). As the blood clots, the lump often feels rubbery or firm to the touch. Over several days, as the body reabsorbs the trapped blood, the firmness will soften and gradually flatten.
- Tight Skin: The swelling may cause the skin to feel tight or stretched. This sensation usually correlates with the degree of edema and resolves naturally as fluid is reabsorbed into the lymphatic and venous systems.
A picture of a blown vein showing bruising and swelling on an arm. Image Source: Illumivein Vein Finder
It's important to distinguish between normal post-puncture reactions and atypical symptoms. Mild warmth and slight aching are expected, but severe burning, rapidly expanding bruising extending beyond the immediate vicinity, or symptoms that mimic nerve compression are not. In rare instances, patients with sensitive nerve endings may experience transient paresthesia (tingling) due to mild tissue swelling pressing on superficial cutaneous nerves. These sensations typically resolve within 24 to 48 hours. Tracking symptom progression is helpful; most patients notice significant improvement within three to five days, with complete cosmetic resolution following the standard two-week hematoma resolution timeline.
Common Causes of a Blown Vein
A blown vein is a result of the needle damaging the vein wall. This can happen for several reasons, which can be related to the procedure itself or the patient's individual physiology. Understanding these contributing factors is essential for improving vascular access success rates and minimizing patient discomfort.
Healthcare Procedure Factors
- Improper Angle: As noted by Medical News Today, inserting the needle at an angle greater than 30 degrees can increase the risk of puncturing through the vein. A steep insertion angle increases the downward force on the vessel wall, making it more likely for the bevel to pierce the posterior side before the catheter or needle tip is fully seated within the lumen.
- Incorrect Needle Size: Using a needle that is too large for the vein can easily cause a rupture. Peripheral veins in the forearm, hand, or antecubital fossa vary significantly in diameter. A 20-gauge catheter placed in a small, superficial metacarpal vein creates excessive mechanical stress, while a 22-gauge or 24-gauge may be safer for fragile or smaller-caliber vessels.
- "Fishing": If a healthcare professional moves the needle around under the skin to find the vein, it can cause accidental damage. Redirecting an inserted needle can create micro-tears along the venous wall, increase pain, and significantly raise the likelihood of perforation or hematoma formation.
- Going Through Both Vein Walls: The needle may accidentally pass through the top and bottom walls of the vein. This often occurs when advancing a catheter too quickly after flash (initial blood return) is achieved, or when failing to lower the angle sufficiently after initial penetration.
- Inadequate Tourniquet Application: Leaving a tourniquet on too long or applying it too tightly can cause venous distention beyond optimal capacity, increasing wall tension and making the vessel more prone to tearing upon needle entry.
Patient-Related Factors
- Patient Movement: Even a small flinch or movement as the needle is inserted can cause it to shift and puncture the vein wall. Sudden muscle contraction in the forearm or biceps can alter the anatomical relationship between the needle and the vessel, turning a successful stick into an accidental puncture.
- Fragile Veins: Healthline mentions that veins naturally become more fragile with age, making them more susceptible to blowing. As collagen and elastin degrade over time, venous walls lose structural integrity. Additionally, chronic conditions like diabetes, hypertension, and long-term corticosteroid use can thin vascular walls and reduce tissue resilience.
- "Rolling" Veins: Some veins move easily under the skin, making them a difficult target. Without adequate skin traction and proper stabilization techniques, these highly mobile vessels can slide away from the advancing needle tip, increasing the chance of grazing or piercing the sidewall.
- Vein Damage: Repeated needle use in the same area, such as from long-term IV therapy or nonmedical drug use, can cause scar tissue and weaken veins. Phlebosclerosis, or hardening of the vein wall from repeated trauma, creates non-compliant tissue that is prone to tearing rather than accommodating gentle puncture.
- Medication and Coagulopathy: Patients taking anticoagulants (e.g., warfarin, direct oral anticoagulants), antiplatelet agents (e.g., aspirin, clopidogrel), or high-dose NSAIDs experience prolonged bleeding times. While these medications don't directly cause the initial puncture, they amplify hematoma formation and make minor needle misplacements visually dramatic and more symptomatic.
Blown Vein vs. Collapsed Vein: What's the Difference?
Though sometimes used interchangeably in casual conversation, a blown vein and a collapsed vein are distinctly different clinical entities with varying pathophysiology, management approaches, and long-term prognoses. A blown vein represents an acute mechanical breach with active or recent bleeding into surrounding tissue, while a collapsed vein refers to a chronic structural failure where the lumen narrows or occludes entirely due to inflammation and scarring.
| Feature | Blown Vein | Collapsed Vein |
|---|---|---|
| Mechanism | The vein is punctured, causing blood leakage. | The vein walls cave inward, blocking blood flow. |
| Primary Cause | Improper needle insertion or fragile veins. | Repeated trauma and irritation to the same vein. |
| Appearance | Immediate bruising and swelling. | The vein may seem to "disappear"; bruising is not always present. |
| Prognosis | Usually heals completely in 10-12 days. | The damage is often permanent. |
| Severity | Generally a minor, less severe injury. | A more serious condition with potential long-term complications. |
The pathophysiology of a collapsed vein involves repetitive endothelial injury that triggers chronic inflammation. Over time, the venous wall thickens with fibrotic tissue (sclerosis), the lumen becomes progressively narrower, and blood flow is severely restricted or halted. This is frequently observed in patients with a history of frequent IV drug use, long-term antibiotic or chemotherapy infusions, or repeated blood draws in the same localized area without adequate site rotation. Clinically, a collapsed vein may feel cord-like, hardened, or entirely non-palpable. Unlike a blown vein, which presents acutely with swelling and discoloration, a collapsed vein develops insidiously. Diagnostic confirmation sometimes requires duplex ultrasound to assess lumen patency and rule out deep venous thrombosis. Management of collapsed veins is largely preventive, focusing on strict site rotation protocols, using the smallest appropriate catheter gauge, allowing adequate recovery time between cannulations, and, in severe cases, consulting a vascular specialist for possible intervention or alternative access planning.
How to Treat a Blown Vein at Home
If you have a blown vein, the healthcare professional will first stop the procedure, remove the needle, and apply gentle pressure to minimize bleeding and swelling. Once you're home, you can take these steps to promote healing:
- Apply a Cold Compress: For the first 24-48 hours, apply an ice pack wrapped in a towel to the area for 15-20 minutes at a time. This helps reduce swelling and constrict blood vessels to minimize bruising. Cryotherapy slows local metabolic activity, reduces capillary permeability, and limits the expansion of the hematoma by promoting vasoconstriction. Avoid placing ice directly on the skin to prevent superficial frostbite or tissue irritation.
- Elevate the Limb: If the blown vein is on your arm or hand, try to keep it elevated above the level of your heart. This uses gravity to help reduce swelling. Elevation decreases hydrostatic pressure in the venous and capillary networks, facilitating lymphatic drainage and preventing fluid from pooling in the injured area.
- Rest: Avoid strenuous activity or heavy lifting with the affected limb for a day or two to allow the area to heal. Mechanical stress from repetitive motion or weight-bearing increases venous pressure and can disrupt the forming clot, potentially prolonging recovery or enlarging the bruise.
- Switch to Warm Compresses: After the first 48 hours, applying a warm compress can help increase circulation to the area, which promotes healing and helps your body reabsorb the leaked blood. Thermotherapy induces localized vasodilation, enhancing oxygen delivery, macrophage activity, and enzymatic breakdown of trapped hemoglobin products.
The pain and discomfort should lessen within a couple of days, and the bruise should completely fade in about 10 to 12 days. During recovery, avoid massaging or rubbing the affected site, as mechanical manipulation can dislodge forming clots and exacerbate tissue trauma. Over-the-counter analgesics can be used if needed; however, acetaminophen is generally preferred during the first 24 to 48 hours, as NSAIDs like ibuprofen or naproxen can theoretically interfere with platelet aggregation and slightly prolong bleeding. Once the initial acute phase passes and no active swelling is expanding, NSAIDs may be used safely to address residual inflammation and soreness. Maintaining gentle range-of-motion exercises, avoiding tight clothing or restrictive jewelry near the site, and monitoring the area for normal healing progression will ensure a smooth recovery. If you notice the bruise changing unexpectedly in size, texture, or sensation, pause self-care measures and consult a clinician.
Potential Risks and Complications
While a blown vein is typically harmless, there are a few potential complications to be aware of. Prompt recognition and appropriate intervention can prevent minor issues from progressing to more serious medical events.
- Infiltration: This occurs when non-irritating IV fluids or medications leak into the surrounding tissue, causing swelling and discomfort. Infiltration is usually self-limiting and resolves once the IV is removed and fluids are naturally absorbed. Monitoring fluid volume is critical, as excessive accumulation can cause temporary tissue tension and mild discomfort.
- Extravasation: This is a more serious complication where irritating or damaging medications (such as chemotherapy drugs, vasopressors, or hypertonic solutions) leak from the vein. It can cause significant pain, blistering, and tissue damage. Extravasation requires immediate cessation of infusion, aspiration of residual medication through the catheter, elevation, and sometimes administration of specific antidotes or surgical consultation to prevent necrosis.
- Infection: Any puncture in the skin carries a small risk of infection. Keeping the area clean is important. Bacteria introduced during insertion or subsequent contamination can lead to localized cellulitis or, rarely, septic thrombophlebitis. Signs include spreading erythema, increasing warmth, purulent drainage, and systemic fever.
- Thrombophlebitis: In rare cases, the injury can cause inflammation of the vein (phlebitis) or lead to the formation of a blood clot (thrombosis). Superficial thrombophlebitis presents as a palpable, tender, erythematous cord along the vein's path. While generally benign and treated with conservative measures (warm compresses, elevation, NSAIDs), it warrants monitoring to ensure it does not propagate toward deeper venous structures.
- Compartment Syndrome: Although exceedingly rare following routine venipuncture, massive hematoma formation in a confined fascial space can increase interstitial pressure to dangerous levels. This medical emergency manifests as severe, unrelenting pain out of proportion to the injury, pain with passive stretch, pallor, paresthesia, and diminished distal pulses. Immediate surgical evaluation is required if these red flags appear.
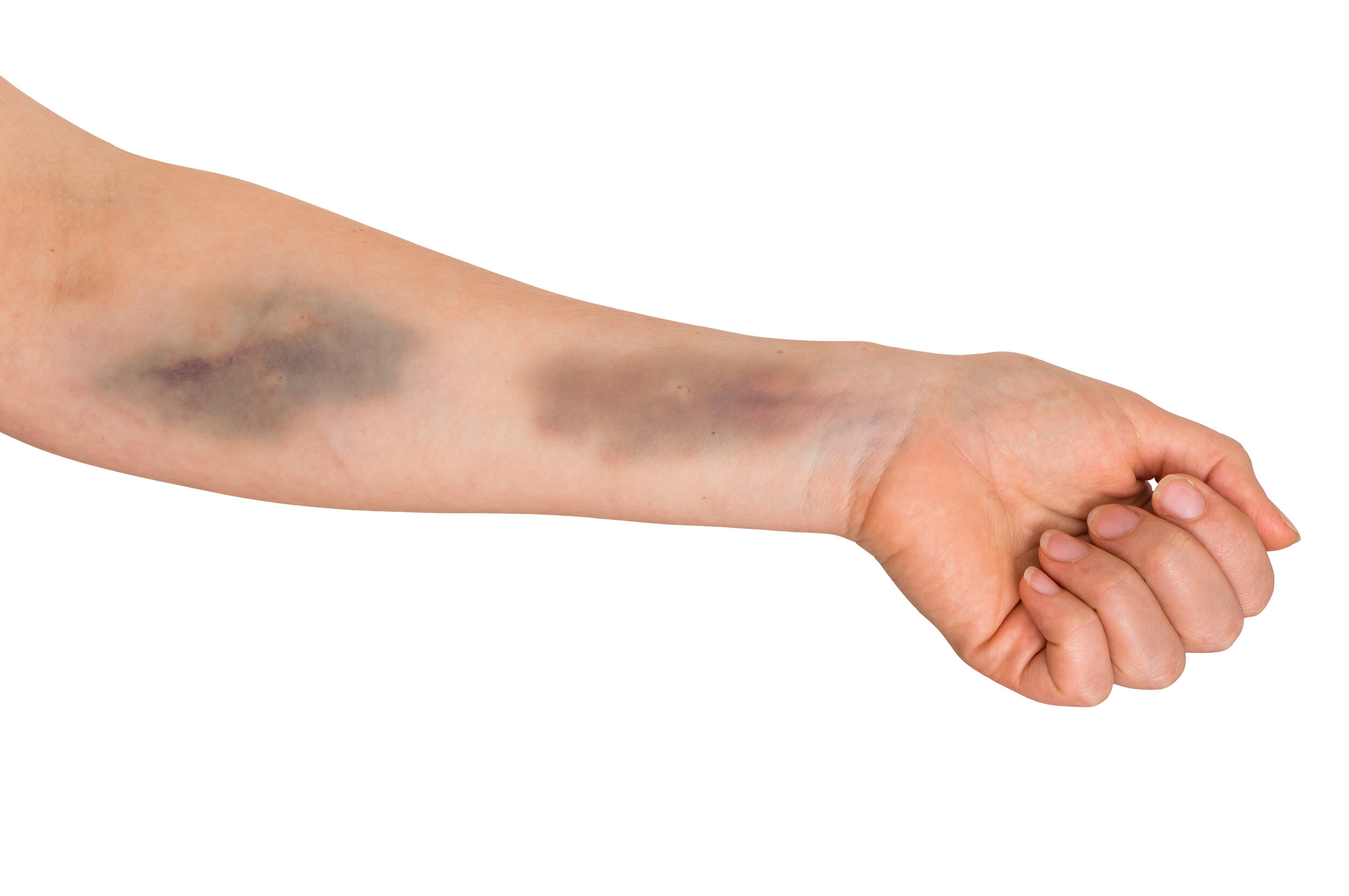 Image Source: The IV Guy
Image Source: The IV Guy
Understanding these complications underscores the importance of proper post-procedure monitoring and early intervention. Healthcare facilities implement strict protocols for IV site assessment, documentation of fluid compatibility, and staff training on extravasation management to mitigate these risks. For patients, maintaining vigilance and communicating any unusual symptoms promptly remains the most effective safeguard.
When to See a Doctor
You should contact a healthcare provider if you notice any of the following signs, as they could indicate a more serious problem:
- Severe or worsening pain that is not relieved by standard over-the-counter analgesics or rest, or pain that radiates significantly beyond the puncture site.
- Rapidly increasing swelling that expands noticeably within hours, feels extremely tense, or compromises joint mobility.
- Signs of infection, including spreading redness, skin that is warm to the touch, pus or drainage from the site, or a fever over 100.4°F (38°C).
- Numbness, tingling, or a "pins and needles" feeling in the affected limb that persists beyond the initial 24 hours, which could suggest nerve compression from edema or direct needle trauma.
- Difficulty moving your hand, wrist, or arm, especially if accompanied by weakness or loss of fine motor control.
- The area is not improving after a few days or seems to be getting worse despite appropriate home care measures.
- Unusual skin changes such as blistering, skin breakdown, dark blackening (necrosis), or the development of red streaks tracking up the limb.
When you seek medical evaluation, your provider will likely perform a thorough physical examination, assess neurovascular status (capillary refill, pulse, sensation, and motor function), and review your medical history, including any anticoagulant medications. In cases where deep vein involvement, significant fluid accumulation, or structural damage is suspected, diagnostic imaging such as a venous duplex ultrasound may be ordered to visualize blood flow, assess for thrombus, and evaluate surrounding soft tissue. Treatment will be tailored to the specific complication: antibiotics for confirmed infections, specialized wound care for extravasation injuries, or referral to a vascular specialist for persistent or complex vascular trauma. Do not hesitate to seek urgent care if symptoms escalate rapidly; early intervention significantly improves outcomes and minimizes long-term sequelae.
Can You Prevent a Blown Vein?
While not all blown veins are preventable, both patients and healthcare professionals can take steps to reduce the risk. Proactive preparation, optimized technique, and collaborative communication form the foundation of successful vascular access.
What You Can Do as a Patient
- Stay Hydrated: Drinking plenty of water makes your veins plumper and easier to access. Adequate hydration increases blood volume and venous distention, improving vessel palpability and reducing the need for multiple attempts. Aim for 8-10 glasses of water in the 24 hours preceding a scheduled blood draw or infusion.
- Communicate: Let the phlebotomist or nurse know if you have "difficult" veins, have a history of blown veins, or feel anxious about needles. Sharing past experiences, preferred sites, and successful stick locations helps clinicians tailor their approach and select the optimal vein.
- Stay Still: Try to remain calm and still during the needle insertion and removal. Sudden movements disrupt the delicate alignment between the needle bevel and the venous lumen. Practice slow, deep breathing techniques to manage anxiety-induced muscle tension or vasovagal responses.
- Warmth Application: Applying a warm pack or wearing long sleeves to keep the arms warm for 10-15 minutes before the procedure encourages peripheral vasodilation. Warmed skin and vessels are more pliable, less prone to spasm, and significantly easier to cannulate successfully on the first attempt.
- Avoid Caffeine and Smoking Pre-Procedure: Both caffeine and nicotine cause peripheral vasoconstriction, which can shrink superficial veins and make access more challenging. Limiting intake for a few hours prior to venipuncture can improve vessel visibility and reduce procedural difficulty.
Best Practices for Healthcare Professionals
- Careful Vein Selection: Choosing a stable, straight, and appropriately sized vein. Prioritize distal sites first to preserve proximal access, assess vein elasticity and turgor, and avoid areas of flexion or previous trauma. Ultrasound-guided venipuncture is recommended for patients with non-palpable, deep, or historically problematic vessels.
- Correct Technique: Using a 15 to 30-degree angle for insertion and stabilizing the vein. Apply adequate traction below the intended site to immobilize the vessel, advance the needle steadily, and lower the angle immediately upon blood return to prevent posterior wall puncture. Never redirect or "fish" with an inserted needle.
- Appropriate Equipment: Selecting the correct needle size for the patient and vein. Utilize smaller-gauge catheters (22G or 24G) for fragile or pediatric veins, and employ safety-engineered devices to minimize handling trauma and enhance procedural precision.
- Adequate Time and Environment: Ensuring proper lighting, patient positioning, and a calm atmosphere. Rushing increases error rates. Taking a moment to assess, prepare, and execute with deliberate control significantly improves first-stick success and reduces complication rates.
- Post-Insertion Verification: Securing the catheter properly, checking for blood flashback, flushing gently with saline, and assessing for signs of immediate infiltration or resistance before connecting IV lines. Documenting insertion details and monitoring the site regularly according to institutional protocols ensures early detection of complications.
In summary, a blown vein is a common and usually minor issue that resolves with simple home care. By understanding its causes, recognizing the symptoms, and knowing when to seek help, you can navigate the experience with confidence and ensure a smooth recovery.
Frequently Asked Questions
Can a blown vein cause permanent damage?
In the vast majority of cases, a blown vein does not cause permanent damage. The body's natural healing mechanisms efficiently repair the minor tear in the venous wall, and the surrounding hematoma is gradually reabsorbed. However, repeated injuries to the exact same vessel over months or years can lead to localized scarring (fibrosis) or chronic vein collapse, which may permanently compromise that specific segment. This is why healthcare providers rotate IV sites and avoid repeatedly cannulating recently injured veins. If a vein has collapsed due to chronic irritation, it may remain unusable for future access, but alternative veins in the same limb or opposite arm are typically unaffected and fully functional.
How long does it take for a blown vein to heal completely?
Most blown veins show significant symptomatic improvement within 3 to 5 days. The swelling and tenderness usually subside quickly as the acute inflammatory phase resolves. The visible bruising follows the standard hematoma timeline, transitioning through color changes and gradually fading over 10 to 14 days. Complete tissue remodeling and full restoration of normal vein wall integrity can take up to 2 to 3 weeks. During this period, it is generally advised to avoid using the same vein for subsequent procedures to allow adequate recovery time. Patients on blood thinners or with compromised immune systems may experience slightly prolonged healing trajectories and should monitor the site accordingly.
Is it safe to take ibuprofen or aspirin for the pain?
Acetaminophen (Tylenol) is typically recommended as the first-line analgesic for the first 48 hours following a blown vein. This is because ibuprofen, naproxen, and aspirin are nonsteroidal anti-inflammatory drugs (NSAIDs) and antiplatelet agents that can theoretically interfere with normal clotting mechanisms and potentially prolong minor bleeding or enlarge the initial bruise. Once the acute phase has passed (after 48 hours) and the hematoma has stabilized without expansion, switching to an NSAID is generally considered safe and can help reduce residual inflammation and soreness. Always follow dosage instructions and consult your pharmacist or physician if you have underlying gastrointestinal, renal, or bleeding disorders.
Can exercise make a blown vein worse?
Yes, engaging in strenuous exercise or heavy lifting with the affected limb too soon after a venipuncture injury can exacerbate the condition. Intense muscular contraction increases venous return pressure and can disrupt the delicate clot forming at the puncture site. This mechanical stress may cause additional blood leakage, expand the hematoma, prolong swelling, and delay healing. Light activities and normal daily movements are perfectly fine and can actually promote healthy circulation, but patients should avoid heavy resistance training, repetitive overhead motions, or prolonged weight-bearing with the injured arm for at least 24 to 48 hours. Gradually reintroducing exercise as pain and swelling resolve is the safest approach.
Why do some people get blown veins more often than others?
Susceptibility to blown veins is highly individual and influenced by a combination of anatomical, physiological, and clinical factors. Some individuals naturally have deeper, smaller-diameter, or highly mobile ("rolling") veins that are mechanically more difficult to cannulate successfully. Age-related vascular changes, including loss of collagen elasticity and thinning of the tunica media, make veins more fragile in older adults. Medical conditions like dehydration, chronic kidney disease, diabetes, and hypertension alter venous integrity and hemodynamics. Additionally, genetic predispositions to easy bruising (such as mild von Willebrand disease or platelet dysfunction), lifestyle factors like smoking, and regular use of anticoagulant medications significantly increase both the frequency and severity of blown veins. Experienced clinicians adapt their technique, equipment, and site selection to accommodate these patient-specific variables, but inherent biological differences inevitably affect individual risk profiles.
Conclusion
A blown vein, while visually striking and occasionally uncomfortable, is a routine and self-limiting complication of venipuncture and IV therapy. It occurs when a needle inadvertently perforates the venous wall, allowing blood to pool in surrounding tissues and form a localized hematoma. Thanks to the body's highly efficient hemostatic and inflammatory healing pathways, the vast majority of these injuries resolve completely within one to two weeks with conservative home management. Implementing immediate cold therapy, followed by gentle warmth, elevation, and temporary activity modification effectively minimizes swelling, accelerates bruise resolution, and promotes optimal tissue recovery.
Understanding the distinction between a blown vein and more serious conditions like collapsed veins, extravasation, or thrombophlebitis empowers patients to monitor their recovery accurately and recognize genuine red flags. While preventive strategies such as proper hydration, vein warming, clear communication with clinicians, and adherence to best-practice insertion techniques significantly reduce occurrence rates, occasional needle misplacement remains an accepted reality of invasive vascular procedures. Patients should approach post-procedure care with patience, avoid unnecessary site manipulation, and maintain open communication with healthcare providers regarding persistent pain, infection signs, or unusual swelling. With informed self-care and appropriate medical vigilance, the experience of a blown vein transitions from a momentary concern to a minor, well-managed step in overall healthcare maintenance.
References
- Cleveland Clinic. (2023). Blown Vein: What You Should Know. Retrieved from https://my.clevelandclinic.org/health/diseases/24599-blown-vein
- Healthline. (2019). Blown Vein: Causes, Symptoms, Treatment, and Prevention. Retrieved from https://www.healthline.com/health/blown-vein
- Medical News Today. (2020). Are blown veins harmful? Symptoms, causes, and treatment. Retrieved from https://www.medicalnewstoday.com/articles/blown-vein
- Southwest Family Medicine Associates. (2019). What Can Cause a Blown Vein and How to Treat It. Retrieved from https://www.southwestfamilymed.com/blog/what-can-cause-a-blown-vein-and-how-to-treat-it

About the author
Michael O'Connell, DO, is a board-certified emergency medicine physician working as an attending physician at a busy Level I Trauma Center in Philadelphia, Pennsylvania. He also serves as a clinical instructor for medical residents and is active in wilderness medicine.