Why Is My Tongue Numb? A Medically Reviewed Guide to Causes & Treatments

Key points
- Sudden weakness or numbness in your face, arm, or leg, especially on one side of the body.
- Facial drooping on one side when you try to smile.
- Difficulty speaking, slurred speech, or trouble understanding others.
- Swelling of the tongue, lips, or throat.
- Difficulty breathing or swallowing.
- A sudden, severe headache, dizziness, or loss of balance.
Feeling numbness or a "pins-and-needles" sensation in your tongue can be a strange and unsettling experience. Known medically as lingual paresthesia, this symptom can arise from a vast array of causes, from something as simple as biting your tongue to being a warning sign of a serious medical condition. The tongue is a highly vascular, densely innervated muscular organ, meaning it serves as both a sensitive indicator of localized trauma and a potential window into systemic neurological, vascular, or metabolic dysfunction. Because the tongue receives sensory innervation from multiple cranial nerves—primarily the lingual branch of the trigeminal nerve (V3) for general sensation, the chorda tympani for taste, and the glossopharyngeal nerve for posterior sensation—identifying the precise origin of numbness often requires a careful evaluation of symptom patterns, duration, and accompanying clinical signs.
This comprehensive guide, synthesized from medical reports and expert sources, will help you understand the potential causes of tongue numbness, differentiate the symptoms, and know when it's crucial to seek medical attention. Whether you are experiencing a fleeting tingle after eating spicy food or dealing with persistent, unexplained numbness that disrupts your speech and eating habits, understanding the underlying mechanisms and appropriate clinical pathways is essential for effective management and peace of mind.
When to Seek Immediate Medical Attention
While many causes of tongue numbness are not emergencies, some are. If you experience sudden tongue numbness along with any of the following symptoms, call 911 or go to the nearest emergency room immediately. These can be signs of a stroke, TIA ("ministroke"), or a severe allergic reaction (anaphylaxis).
- Sudden weakness or numbness in your face, arm, or leg, especially on one side of the body.
- Facial drooping on one side when you try to smile.
- Difficulty speaking, slurred speech, or trouble understanding others.
- Swelling of the tongue, lips, or throat.
- Difficulty breathing or swallowing.
- A sudden, severe headache, dizziness, or loss of balance.
The F.A.S.T. acronym is a critical tool for recognizing a stroke:
- Face: Does one side of the face droop?
- Arms: Is one arm weak or numb?
- Speech: Is speech slurred?
- Time: Time to call 911 immediately.
Sudden-onset neurological deficits, including unilateral tongue numbness or deviation when protruding the tongue, are hallmark signs of cerebrovascular compromise. When blood flow to specific regions of the motor cortex or brainstem is interrupted, the delicate signaling pathways that control oral and pharyngeal musculature can fail rapidly. Similarly, anaphylaxis triggers massive histamine release, leading to rapid vasodilation, capillary leakage, and tissue edema in the upper airway. Tongue swelling in this context is particularly dangerous because it can completely occlude the glottis. If you suspect either condition, do not drive yourself to the hospital. Lay flat if dizzy, keep the airway clear, and use an epinephrine auto-injector immediately if you have been prescribed one for known severe allergies. Emergency medical technicians can administer advanced airway management, intravenous corticosteroids, antihistamines, and clot-busting therapies (if eligible for stroke) that are time-dependent and life-saving.
Common and Temporary Causes of a Numb Tongue
Often, the reason for a numb tongue is temporary and resolves on its own. These common causes include:
Minor Injuries and Oral Irritations
- Accidental Bites: Biting your tongue while eating or speaking can cause temporary numbness and pain. The trauma creates localized edema and inflammation that compresses superficial nerve endings in the mucosal layer. As the tissue begins to heal, damaged axons may fire erratically, producing tingling or a "dead" sensation until epithelial regeneration and nerve recovery are complete.
- Burns: Hot food or beverages can scald your tongue, leading to a tingling or numb sensation as the tissue heals. Thermal injury denatures proteins in the superficial papillae and can temporarily stun the nerve endings. The subsequent sloughing of the damaged epithelial layer (often appearing as a white or gray film) exposes underlying sensitive tissue before gradual remodeling restores normal sensation over several days.
- Canker Sores and Cold Sores: These painful ulcers can cause localized tingling or numbness in the immediate area before and during their appearance. Aphthous ulcers and herpes simplex outbreaks trigger a localized inflammatory cascade. The release of cytokines and prostaglandins heightens nerve sensitivity initially, followed by temporary nerve hypoesthesia as the ulcer crater forms. Stress, acidic foods, or minor mucosal abrasions often precipitate these episodes.
 Canker sores can cause localized tingling and numbness. Source: MedicalNewsToday
Canker sores can cause localized tingling and numbness. Source: MedicalNewsToday
Allergic Reactions
A tingling or numb tongue is a classic symptom of an allergic reaction.
- Oral Allergy Syndrome (OAS): This occurs when your immune system mistakes proteins in certain raw fruits, vegetables, or nuts for allergy-causing pollen. It can cause a sudden, itchy or tingly sensation in your mouth and on your tongue. This cross-reactivity, known as pollen-food syndrome, typically involves birch, ragweed, or grass pollen IgE antibodies reacting to homologous plant proteins. Cooking or canning the offending food usually denatures the proteins, preventing the reaction. Symptoms generally remain confined to the oral mucosa and resolve within minutes to a few hours.
- Food Allergies: Allergies to foods like shellfish or nuts can also trigger numbness and swelling. Unlike OAS, true IgE-mediated food allergies can progress systemically. The numbness results from localized mast cell degranulation and fluid shifts into the interstitial spaces. Careful monitoring for progression to respiratory distress, gastrointestinal cramping, or hypotension is essential.
Dehydration and Dry Mouth
When you're dehydrated, your body produces less saliva, leading to dry mouth (xerostomia). This lack of moisture can cause a rough, sticky, or even numb feeling on the tongue. Saliva contains mucins that coat and protect the lingual epithelium, along with enzymes and electrolytes that maintain tissue homeostasis. Chronic dehydration, mouth breathing, or Sjögren's-like symptoms can strip this protective layer, leading to micro-abrasions, altered pH, and impaired nerve signal transmission. Over-the-counter saliva substitutes, humidifiers, sugar-free xylitol lozenges, and consistent water intake can often restore comfort and sensation quickly.
Medication Side Effects
Certain prescription medications, such as some blood pressure drugs or antibiotics, can list paresthesia as a side effect. If you suspect your medication is the cause, consult your doctor. Never stop taking a prescribed medication without medical advice. Common culprits include ACE inhibitors (which may also cause angioedema), fluoroquinolone antibiotics (associated with peripheral neuropathy), certain antiepileptics, and chemotherapeutic agents. Drug-induced paresthesia often stems from altered neurotransmitter balance, direct neurotoxicity, or electrolyte disturbances like hypokalemia. A thorough medication reconciliation with a pharmacist or prescribing physician is a critical first step.
Dental Anesthesia and Procedures
While not explicitly listed above, it is important to note that local dental anesthetics (like lidocaine with epinephrine) are the most frequent cause of short-term tongue numbness. The anesthetic blocks voltage-gated sodium channels in nerve axons, preventing action potential propagation. Depending on the injection site, volume, and individual metabolism, sensation can take anywhere from 1 to 5 hours to return. Prolonged numbness beyond 24 hours warrants a follow-up with the dentist to rule out nerve compression from swelling or direct needle trauma.
Medical Conditions Linked to Tongue Numbness
If the numbness is persistent, recurrent, or accompanied by other symptoms, it may be linked to an underlying medical condition. Chronic paresthesia requires a differential diagnosis approach that considers systemic, neurological, and metabolic etiologies.
Nutritional Deficiencies
Your nerves require specific vitamins and minerals to function properly. A deficiency in any of the following can lead to nerve-related symptoms like tongue numbness:
- Vitamin B12: Crucial for nerve health. Deficiency can also cause a sore, red tongue and fatigue. B12 is essential for myelin sheath synthesis and maintenance. Deficiency, common in strict vegans, older adults with reduced gastric acid, or individuals with pernicious anemia or gastrointestinal malabsorption, leads to subacute combined degeneration of the spinal cord and peripheral neuropathy. Early signs often include glossitis and symmetric distal paresthesias that can ascend or involve cranial nerves.
- Folate (Vitamin B9) works synergistically with B12 in DNA synthesis and red blood cell formation. Deficiency can cause macrocytic anemia and mucosal changes that compromise oral nerve endings.
- Iron, Zinc, or Phosphorus deficiencies can alter mucosal integrity and impair cellular metabolism in rapidly dividing epithelial cells and supporting Schwann cells.
- Calcium (Hypocalcemia): Low blood calcium can cause tingling around the mouth, as well as in the hands and feet. Calcium ions regulate neuronal excitability. Hypocalcemia lowers the threshold for nerve depolarization, leading to spontaneous firing and characteristic perioral numbness, muscle cramps, or Chvostek's sign. Causes include parathyroid dysfunction, vitamin D deficiency, or severe magnesium depletion.
Neurological Conditions
The nerves that provide sensation to your tongue originate in the brain. Any condition affecting these nerves can cause numbness.
- Stroke and TIA: As mentioned, these are emergencies where blood flow to the brain is blocked. TIAs are transient, typically resolving within an hour without permanent tissue infarction, but they serve as critical warnings of impending major cerebrovascular events.
- Multiple Sclerosis (MS): An autoimmune disease where the immune system attacks the protective covering of nerves. Numbness or tingling in the face, tongue, or other body parts is a common symptom, often referred to as "MS tongue." These symptoms can come and go. MS demyelinating plaques frequently occur in the brainstem or trigeminal nerve pathways. The numbness may be episodic during relapses or persistent in progressive disease. Corticosteroids are used for acute flares, while disease-modifying therapies reduce long-term progression.
- Bell's Palsy: This condition causes sudden, temporary weakness or paralysis of the facial muscles on one side. As one woman shared in her story with Bell's palsy recovery information (Mayo Clinic), her experience began with her tongue going numb before half of her face stopped working. The inflammation of the facial nerve (CN VII) as it passes through the stylomastoid foramen can also affect the chorda tympani branch, which carries taste sensation from the anterior two-thirds of the tongue. Loss of taste often accompanies or precedes the motor paralysis.
- Migraine with Aura: Some people experience sensory disturbances, known as an aura, before or during a migraine headache. This can include a tingling or numb sensation in the tongue, lips, or face that typically lasts less than an hour. Migraine auras are believed to result from cortical spreading depression, a wave of neuronal depolarization followed by suppression that moves across the cerebral cortex at 3-5 mm per minute. Trigeminal activation contributes to the referred sensation in the oral cavity.
- Nerve Damage: The lingual nerve, which controls sensation in the tongue, can be damaged during dental procedures (like wisdom tooth removal), oral surgery, or from a tongue piercing. This can result in persistent, long-term numbness. Iatrogenic injury may involve neuropraxia (temporary conduction block), axonotmesis (axonal disruption with intact sheath), or neurotmesis (complete transection). Recovery timelines vary widely, from spontaneous resolution in weeks to permanent deficits requiring neurosurgical intervention or compensatory training.
Metabolic and Autoimmune Disorders
- Hypoglycemia (Low Blood Sugar): A sudden drop in blood sugar can cause numbness or tingling in the tongue and lips, often accompanied by shakiness, sweating, and anxiety. Glucose is the primary fuel for neurons. When serum glucose falls below 70 mg/dL, the brain triggers autonomic responses and neuroglycopenic symptoms. Diabetics on insulin or sulfonylureas are at highest risk, but prolonged fasting, excessive alcohol intake without food, or insulinoma can also precipitate episodes.
- Raynaud's Phenomenon: This condition causes blood vessels, usually in the fingers and toes, to spasm and narrow in response to cold or stress. In rare cases, it can affect the tongue. A fascinating case reported by NBC News detailed a woman who photographed her tongue turning completely white and numb during an attack. Lingual Raynaud's is exceptionally rare but occurs when sympathetic overactivity or endothelial dysfunction triggers vasospasm in the lingual artery branches, leading to transient ischemia, pallor, and sensory loss.
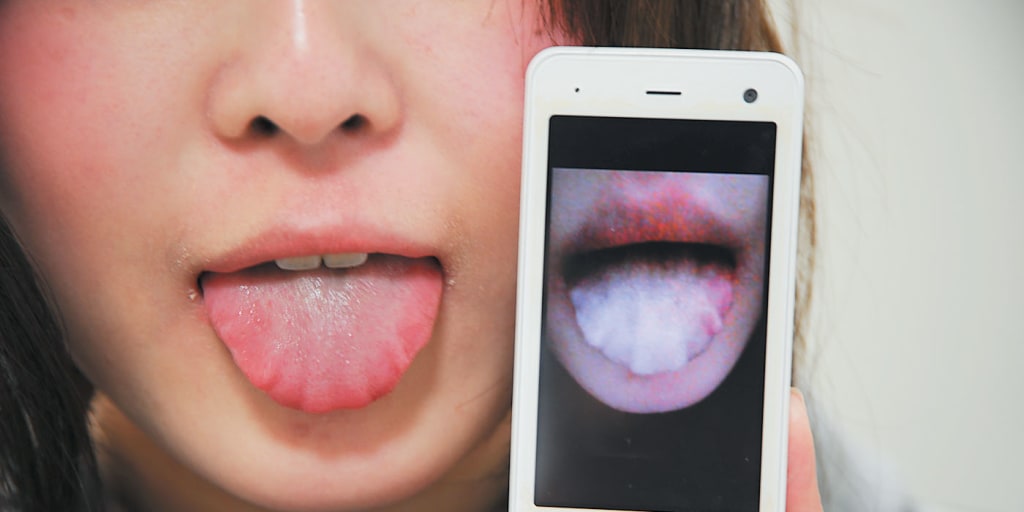 A photo taken by a patient showing lingual Raynaud's phenomenon, where the tongue turns white and numb due to lack of blood flow. Source: NBC News / New England Journal of Medicine
A photo taken by a patient showing lingual Raynaud's phenomenon, where the tongue turns white and numb due to lack of blood flow. Source: NBC News / New England Journal of Medicine
- Diabetic Neuropathy: Long-standing or poorly controlled diabetes can cause peripheral and cranial neuropathy. Microvascular damage and advanced glycation end-products accumulate, injuring small sensory fibers. While typically presenting in the lower extremities, cranial nerve involvement can cause bilateral or patchy tongue numbness, altered taste, and reduced gag reflex.
- Hypothyroidism: An underactive thyroid slows metabolic processes and can lead to mucopolysaccharide deposition in tissues (myxedema), which may compress nerves. Patients often report a swollen, thick tongue with reduced mobility and altered sensation, alongside fatigue, weight gain, and cold intolerance.
- Gastroesophageal Reflux Disease (GERD): Chronic acid exposure can cause microscopic mucosal erosion and neurogenic inflammation in the oral cavity. Some patients report a metallic taste, burning sensation, or intermittent numbness secondary to vagal nerve irritation or altered oral pH affecting nerve thresholds.
Psychological Factors
- Anxiety: High levels of stress or anxiety can trigger physical symptoms. A tingling or numb tongue can be a manifestation of the body's "fight-or-flight" response, a condition sometimes called psychogenic oral paresthesia. Hyperventilation lowers arterial carbon dioxide, causing respiratory alkalosis and reduced ionized calcium, which directly stimulates peripheral nerves. Chronic anxiety can also heighten somatic awareness, causing benign sensations to be perceived as distressing numbness.
- Burning Mouth Syndrome (BMS): A chronic and complex condition characterized by a burning or tingling sensation in the mouth, often without a clear cause. Numbness can also be a symptom. Anxiety and depression are often linked with BMS. Pathophysiology likely involves small-fiber neuropathy, altered dopamine receptor function, and central sensitization. Diagnosis is one of exclusion, and management often requires a multidisciplinary approach including topical clonidine, alpha-lipoic acid, or cognitive behavioral therapy.
The Diagnostic Process: What to Expect from Your Doctor
If you see a doctor for unexplained tongue numbness, they will follow a systematic pathway to identify the cause. The evaluation begins in the primary care setting but may quickly branch out to neurology, otolaryngology, dentistry, or gastroenterology depending on preliminary findings.
- Patient History: Expect questions about when the numbness started, whether it's constant or intermittent, and if you have other symptoms. Your doctor will also review your medical history, medications, and diet. Detailed questioning focuses on laterality (unilateral vs. bilateral), progression, associated taste changes, trauma history, dental work timeline, dietary restrictions, and family history of autoimmune or neurological diseases. Keeping a symptom diary noting triggers, duration, and accompanying signs can significantly expedite diagnosis.
- Physical Exam: An examination of your tongue, mouth, and head, along with a neurological assessment to check your reflexes and muscle strength. The clinician will inspect for lesions, coating, discoloration, asymmetry, atrophy, fasciculations, or geographic patterns. Cranial nerve testing (V, VII, IX, X, XII) assesses sensory distribution, motor function, gag reflex, and tongue protrusion symmetry. Orthostatic vitals, skin turgor, and peripheral nerve checks help identify systemic involvement.
- Diagnostic Tests: Depending on the suspected cause, your doctor may order:
- Blood Tests: To check for vitamin deficiencies, low calcium or glucose, and signs of infection or autoimmune disease. Panels often include CBC, comprehensive metabolic panel, HbA1c, B12, folate, ferritin, thyroid-stimulating hormone (TSH), free T4, ESR/CRP, and sometimes autoimmune markers like ANA or rheumatoid factor.
- Imaging: An MRI or CT scan of the brain may be used to rule out a stroke, MS, or other neurological issues. High-resolution MRIs can visualize brainstem lesions, cranial nerve pathways, and microvascular ischemic changes. If dental or maxillofacial trauma is suspected, a cone-beam CT or panoramic X-ray may be ordered.
- Allergy Testing: Skin-prick or blood tests can identify potential allergens. Specific IgE panels or elimination diets help confirm OAS or IgE-mediated reactions.
- Advanced Neurological Testing: Nerve conduction studies (NCS) or electromyography (EMG) are rarely used for the tongue itself but can assess peripheral neuropathy. Quantitative sensory testing or biopsy of minor salivary glands may be considered if Sjögren's or small-fiber neuropathy is suspected.
Treatment and Management of Tongue Numbness
Treatment is entirely dependent on the underlying cause. A targeted, etiology-driven approach yields the best outcomes, and patients should avoid self-medicating without professional guidance, especially when neurological deficits are present.
- For Deficiencies: Vitamin or mineral supplements (oral or injections). B12 deficiency often requires high-dose oral supplementation (1000-2000 mcg daily) or intramuscular hydroxocobalamin/cyanocobalamin injections for severe cases or pernicious anemia. Iron and calcium supplementation must be guided by lab values to avoid toxicity or malabsorption interference.
- For Allergies: Antihistamines and avoidance of the trigger. Second-generation H1 blockers (cetirizine, loratadine) and H2 blockers can mitigate histamine release. Strict allergen avoidance, carrying epinephrine, and considering immunotherapy for pollen allergies can prevent recurrence.
- For Infections: Antibiotic or antiviral medications. Bacterial oral infections require targeted antimicrobials, while herpes outbreaks respond to acyclovir, valacyclovir, or famciclovir, especially if initiated within 72 hours of symptom onset. Antifungals like nystatin or fluconazole address oral candidiasis.
- For Hypoglycemia: Consuming a fast-acting source of sugar, followed by a protein-rich meal. The "15-15 rule" (15g carbs, recheck in 15 mins) is standard. Long-term management involves adjusting diabetes medications, regular meal scheduling, and continuous glucose monitoring.
- For Neurological Conditions (MS, Migraines): Specific prescription medications to manage the condition. Migraine prophylaxis may include beta-blockers, tricyclic antidepressants, or CGRP antagonists. Acute attacks respond to triptans or NSAIDs. MS management relies on immunomodulators, physical therapy, and symptom-specific neuropathic pain agents.
- For Anxiety: Stress management techniques, psychotherapy, and sometimes anti-anxiety medication can help alleviate physical symptoms. Cognitive behavioral therapy (CBT), mindfulness-based stress reduction, and diaphragmatic breathing retrain autonomic responses. SSRIs/SNRIs may be prescribed for chronic anxiety or comorbid depression, though initial side effects may include temporary paresthesia.
- For Nerve Damage: The numbness may improve over time. In some cases, oral physiotherapy or medications for nerve pain (like gabapentin) may be recommended. Early intervention with alpha-lipoic acid, B-complex vitamins, and gentle sensory re-education exercises (texture mapping, thermal discrimination training) can promote neuroplasticity. Surgical nerve repair is considered only in cases of confirmed transection with no spontaneous recovery after 3-6 months.
For temporary relief at home, you can try staying hydrated, avoiding irritants like very spicy foods and alcohol, and maintaining good oral hygiene. Switching to sodium lauryl sulfate-free toothpaste, using a soft-bristled brush, and rinsing with warm saltwater or diluted baking soda can soothe irritated mucosa. Applying a cold compress or sucking on ice chips can temporarily numb overactive nerve endings and reduce inflammation.
For chronic cases, establishing a multidisciplinary care team is highly beneficial. A primary care physician coordinates baseline labs and referrals, a neurologist evaluates central and peripheral nerve pathways, a dentist or oral surgeon assesses structural or iatrogenic damage, and a dietitian ensures nutritional adequacy. Regular follow-ups allow clinicians to adjust treatments based on symptom trajectories and prevent complications like nutritional decline from altered eating habits or psychological distress from chronic discomfort.
Ultimately, a numb tongue is a symptom, not a disease. While it can be caused by minor issues, it should not be ignored. Paying attention to other accompanying signs and consulting a healthcare professional is the best way to ensure your health and peace of mind.
Frequently Asked Questions
How long does it take for a numb tongue from biting or burning to heal?
Minor trauma or thermal injury to the tongue typically resolves within 7 to 14 days. The oral mucosa has one of the fastest cellular turnover rates in the body, allowing superficial burns or abrasions to heal rapidly. During the initial 48 hours, swelling may cause a lingering numb or "thick" feeling. Maintaining excellent oral hygiene, rinsing with mild saline, and avoiding hot, acidic, or rough-textured foods can accelerate recovery. If numbness persists beyond two weeks without improvement, or if an ulcer fails to heal after three weeks, medical evaluation is warranted to rule out secondary infection or atypical pathology.
Can vitamin supplements immediately fix tongue numbness?
No, vitamin supplementation is not an instant fix. Nerve repair is a slow biological process that depends on remyelination and axonal regeneration, which can take weeks to months. If a documented deficiency exists, appropriate supplementation will halt further nerve damage and create the biochemical environment necessary for recovery. Symptomatic improvement often begins after 2 to 4 weeks of consistent treatment, but full sensory restoration may require sustained supplementation over 3 to 6 months, particularly in cases of severe B12 deficiency or malabsorption syndromes. Over-supplementation without medical guidance is not recommended and can cause adverse effects.
Is tongue numbness always a sign of a serious neurological condition?
Absolutely not. While tongue numbness can be associated with serious conditions like stroke, MS, or tumors, the vast majority of cases are benign, temporary, or related to manageable systemic issues. Minor trauma, dehydration, allergic reactions, medication side effects, nutritional gaps, and anxiety-related hyperventilation account for most clinical presentations. The key differentiator is the symptom profile: serious neurological conditions typically present with additional red flags such as unilateral facial droop, limb weakness, slurred speech, severe headache, or progressive neurological decline. Isolated, transient tingling without systemic symptoms rarely indicates a dire emergency.
What type of doctor should I see for persistent tongue numbness?
Start with a primary care physician (PCP) or general practitioner. They can conduct an initial comprehensive evaluation, order baseline blood work, review medications, and assess for common metabolic or nutritional deficiencies. Based on findings, they may refer you to a neurologist (for suspected nerve damage, MS, or migraines), an otolaryngologist/ENT specialist (for structural, infectious, or reflux-related causes), an oral and maxillofacial surgeon or dentist (for trauma, dental nerve injury, or oral pathology), or an allergist/immunologist (for OAS or IgE-mediated reactions). If anxiety or burning mouth syndrome is suspected, a referral to a specialist in orofacial pain or a behavioral health provider may be highly beneficial.
Can stress or panic attacks cause my tongue to feel numb?
Yes, stress and panic attacks are well-documented causes of oral paresthesia. During periods of acute anxiety, the sympathetic nervous system activates, leading to rapid, shallow breathing (hyperventilation). This expels carbon dioxide too quickly, causing respiratory alkalosis. The resulting shift in blood pH decreases the level of ionized calcium, which increases neuronal excitability and commonly manifests as perioral tingling, numbness in the lips and tongue, and tingling in the fingertips. Additionally, heightened somatic vigilance during anxiety amplifies normal physiological sensations, making mild tingling feel pronounced. Grounding techniques, paced breathing (inhaling for 4 seconds, holding for 4, exhaling for 6), and addressing underlying anxiety through therapy or medication typically resolve these symptoms.
Conclusion
Tongue numbness, or lingual paresthesia, is a multifaceted symptom that spans a broad clinical spectrum, ranging from trivial, self-limiting irritations to complex neurological or systemic disorders. Understanding the underlying anatomy, recognizing emergency warning signs, and systematically evaluating contributing factors are the cornerstones of effective management. While minor bites, thermal injuries, dehydration, and transient allergic reactions are the most common culprits and often resolve with conservative home care, persistent or recurrent numbness demands a thorough medical workup. Nutritional deficiencies, metabolic imbalances, medication side effects, cranial nerve injuries, and chronic conditions like multiple sclerosis, diabetes, or burning mouth syndrome all require targeted, evidence-based interventions.
The diagnostic journey typically begins with a detailed clinical history and physical examination, followed by strategic laboratory testing, imaging, or specialist referrals. Treatment success hinges on accurately identifying the root cause, whether that means supplementing a missing nutrient, adjusting a medication regimen, managing a chronic autoimmune disease, or implementing stress-reduction techniques. Importantly, patients should not ignore accompanying red-flag symptoms such as facial asymmetry, speech difficulties, swallowing problems, or sudden severe headaches, as these necessitate immediate emergency evaluation. By maintaining open communication with healthcare providers, adhering to recommended follow-ups, and implementing preventive lifestyle adjustments, most individuals can achieve symptom relief and restore normal oral function. Ultimately, a proactive, informed approach to tongue numbness ensures both physical recovery and lasting reassurance.
References
- MedicalNewsToday: Tingling tongue: Causes and when to see a doctor
- WebMD: Tingling Tongue: Possible Causes
- Vinmec International Hospital: Why Have You Lost Sensation in Your Tongue?
- Bell's palsy recovery information (Mayo Clinic)
- NBC News: The curious case of a numb tongue
- Mass General Brigham: MS Swallowing Problems and MS Tongue

About the author
Benjamin Carter, MD, is a board-certified otolaryngologist specializing in head and neck surgery, with an expertise in treating throat cancer. He is an associate professor and the residency program director at a medical school in North Carolina.