Arterial vs. Venous Ulcers: Key Differences in Symptoms and Treatment

Key points
- Smoking: The most potent modifiable risk factor. Tobacco chemicals cause direct endothelial damage, promote inflammation, increase platelet aggregation, and trigger arterial vasospasm.
- Diabetes: Chronic hyperglycemia accelerates atherosclerosis and causes microvascular disease, while diabetic neuropathy masks early warning pain, delaying treatment until tissue damage is severe.
- High cholesterol and high blood pressure: Elevated LDL cholesterol contributes to plaque formation, while hypertension increases shear stress on arterial walls, accelerating structural damage.
- Advanced age: Arterial elasticity naturally decreases over time, and cumulative plaque burden typically peaks in individuals over 65.
- History of heart disease or stroke: Systemic atherosclerosis means that if plaques affect the heart or brain, they are highly likely to affect peripheral arteries as well.
- Obesity and a sedentary lifestyle: Excess weight increases cardiovascular strain, while physical inactivity reduces collateral circulation development and calf muscle pump function.
Leg ulcers are open sores on the lower leg or foot that are slow to heal. While they may appear similar to the untrained eye, the two most common types, arterial ulcers and venous ulcers, stem from completely opposite circulatory problems. Understanding their differences is critical because the treatment for one can be harmful, or even catastrophic, for the other. Misdiagnosis can lead to delayed healing, severe infection, tissue necrosis, or limb loss.
This guide explores the causes, symptoms, pathophysiology, and clinical characteristics of arterial vs. venous ulcers to help you recognize the signs, understand diagnostic testing, and comprehend the appropriate treatment approach for each. With an estimated prevalence affecting up to 1% of the adult population and significantly higher rates in individuals over 60, chronic leg ulcers represent a substantial healthcare burden that requires timely, specialized intervention.
What is an Arterial Ulcer?
An arterial ulcer, also known as an ischemic ulcer, is an open wound caused by poor blood flow through the arteries. Arteries carry oxygen-rich blood from the heart to the rest of the body. When arteries in the legs become narrowed or blocked, typically due to peripheral artery disease (PAD), tissues are starved of oxygen and nutrients. This deprivation causes tissue to break down and die, forming a painful ulcer that struggles to heal. Without adequate oxygen delivery (tissue hypoxia), cellular metabolism falters, immune function in the local area is compromised, and even minor trauma can escalate into a chronic, non-healing wound.
Arterial ulcers are often a sign of critical limb ischemia (CLI), a severe stage of PAD characterized by rest pain, non-healing wounds, and a high risk of amputation if left untreated. The progression from initial claudication to tissue breakdown reflects a systemic atherosclerotic process that frequently coexists with coronary artery disease and cerebrovascular disease.
Causes and Risk Factors
The primary cause is atherosclerosis (hardening of the arteries), a progressive condition where plaque composed of fat, cholesterol, calcium, and other substances builds up along the inner arterial walls. Over time, this narrows the lumen and stiffens the vessel, reducing distal perfusion. Key risk factors include:
- Smoking: The most potent modifiable risk factor. Tobacco chemicals cause direct endothelial damage, promote inflammation, increase platelet aggregation, and trigger arterial vasospasm.
- Diabetes: Chronic hyperglycemia accelerates atherosclerosis and causes microvascular disease, while diabetic neuropathy masks early warning pain, delaying treatment until tissue damage is severe.
- High cholesterol and high blood pressure: Elevated LDL cholesterol contributes to plaque formation, while hypertension increases shear stress on arterial walls, accelerating structural damage.
- Advanced age: Arterial elasticity naturally decreases over time, and cumulative plaque burden typically peaks in individuals over 65.
- History of heart disease or stroke: Systemic atherosclerosis means that if plaques affect the heart or brain, they are highly likely to affect peripheral arteries as well.
- Obesity and a sedentary lifestyle: Excess weight increases cardiovascular strain, while physical inactivity reduces collateral circulation development and calf muscle pump function.
Additional factors include hyperhomocysteinemia, chronic kidney disease (which promotes vascular calcification), and a high-fat diet. Genetic predispositions also play a role, particularly in families with premature peripheral vascular disease.
Symptoms and Appearance
Arterial ulcers have several distinct features that reflect underlying tissue ischemia:
- Location: Most often found on the toes, heels, outer ankle, or between the toes—areas farthest from the heart and most vulnerable to hypoperfusion. They frequently develop at pressure points where shoes or bed linens rub against poorly perfused skin.
- Appearance: They have a characteristic "punched-out" look, appearing small, round, and deep with well-defined, sharp edges. The wound base is often pale, gray, or yellow-tan and covered in black, necrotic (dead) tissue or a thick eschar. These ulcers are typically dry with little to no drainage due to severely reduced capillary filtration.
- Surrounding Skin: The skin around the ulcer may look shiny, tight, thin (atrophic), and pale, with noticeable hair loss on the leg and foot. The foot often feels cool or cold to the touch due to reduced cutaneous blood flow. Capillary refill time is typically delayed (>3 seconds).
- Pain: Arterial ulcers are typically very painful, especially at night or when the legs are elevated. Patients often experience relief by dangling their foot off the side of the bed, as gravity helps pull a small amount of blood into the foot. This is known as "rest pain." Claudication (cramping calf pain during walking that resolves with rest) often precedes ulcer formation.
- Pulses: The pulses in the foot (dorsalis pedis or posterior tibial) are usually weak, thready, or completely absent on palpation.
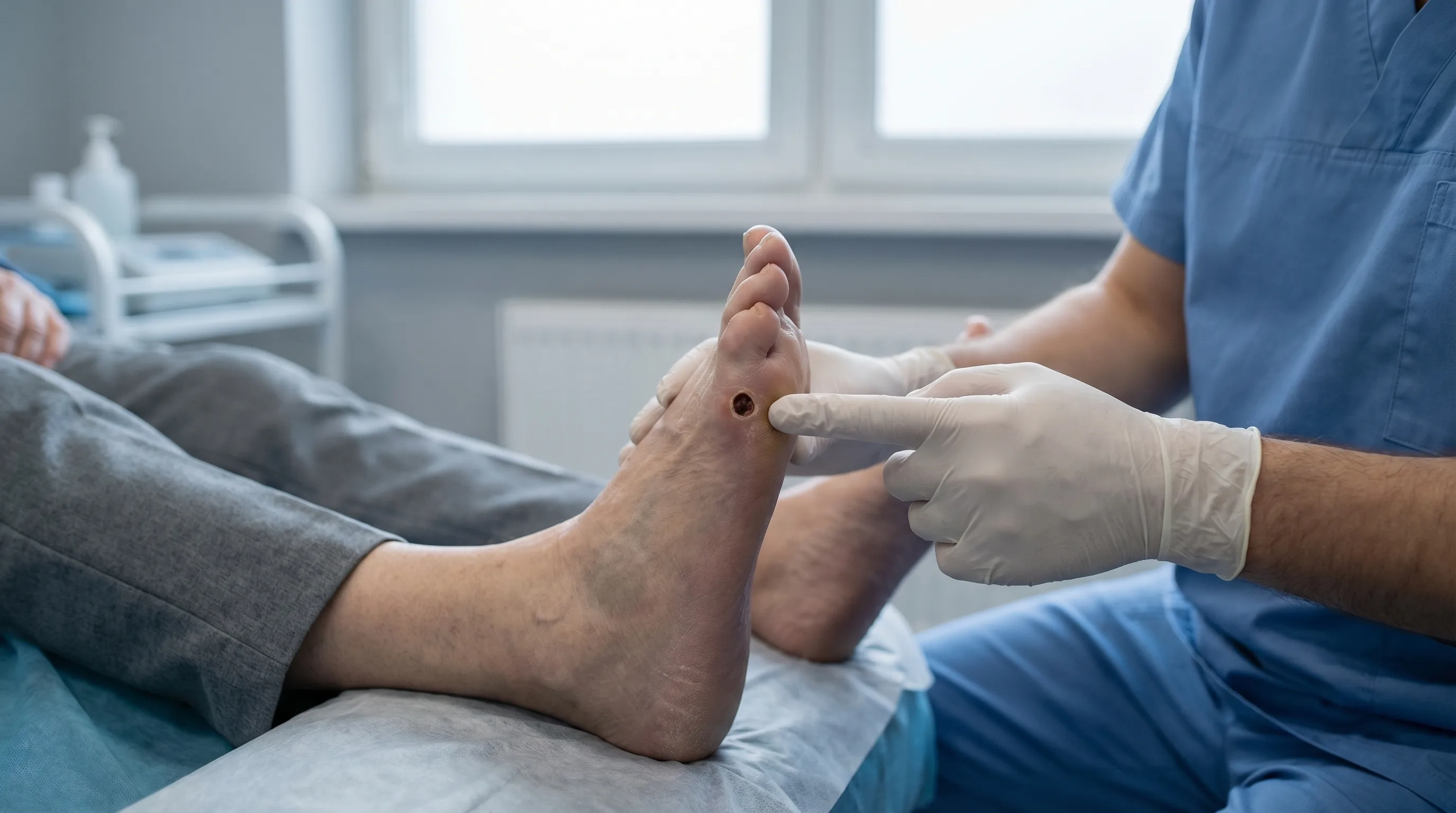 An example of an arterial ulcer on the toe. Note the well-defined edges and the dead tissue in the wound bed, which are classic signs of poor arterial blood supply.
An example of an arterial ulcer on the toe. Note the well-defined edges and the dead tissue in the wound bed, which are classic signs of poor arterial blood supply.
Clinicians often use the Fontaine or Rutherford classification systems to stage PAD, with tissue loss (ulcers/gangrene) representing Stage IV (Fontaine) or Category 6 (Rutherford). Early recognition of these stages can prompt vascular referral before irreversible tissue loss occurs.
What is a Venous Ulcer?
A venous ulcer, or stasis ulcer, is the most common type of leg ulcer, accounting for approximately 70% of all chronic lower extremity wounds. It develops due to poor blood circulation in the veins. Veins are responsible for returning deoxygenated blood from the legs back to the heart against gravity, aided by one-way valves and the contraction of calf muscles. When the one-way valves in these veins become weak or damaged (chronic venous insufficiency), blood flows backward (reflux) and pools in the lower legs. This creates high pressure within the venous system (venous hypertension), causing fluid, proteins, and inflammatory mediators to leak into surrounding tissues. The resulting swelling and chronic low-grade inflammation eventually lead to skin breakdown and the formation of an ulcer.
The pathophysiology involves a complex inflammatory cascade. White blood cells become trapped in the capillary beds, releasing reactive oxygen species, proteolytic enzymes, and pro-inflammatory cytokines. Over time, this damages the microcirculation, disrupts extracellular matrix remodeling, and creates a hostile wound environment that resists normal healing processes.
Causes and Risk Factors
The primary cause is chronic venous insufficiency (CVI), which can be primary (congenital valve weakness or vein wall abnormalities) or secondary (post-thrombotic damage). Key risk factors include:
- History of deep vein thrombosis (DVT) or blood clots: Post-thrombotic syndrome permanently damages venous valves, leading to chronic reflux and hypertension. Up to 20-30% of venous ulcers are post-thrombotic.
- Varicose veins: Superficial venous dilation often indicates underlying valve incompetence, contributing to increased hydrostatic pressure.
- Obesity: Excess abdominal and pelvic fat increases intra-abdominal pressure, impeding venous return from the legs.
- Multiple pregnancies: Hormonal changes (progesterone-induced venodilation) and mechanical pressure from the growing uterus strain venous valves.
- Prolonged standing or sitting: Occupational immobility reduces calf muscle pump activity, allowing gravitational pooling to overwhelm valvular function.
- Advanced age and family history of vein disease: Connective tissue naturally weakens with age, and genetic predispositions to valve laxity or collagen defects increase susceptibility.
- Previous leg trauma or surgery: Can damage perforating veins that normally shunt blood from superficial to deep venous systems.
Lack of mobility due to neurological conditions (stroke, spinal cord injury) or severe arthritis also significantly elevates risk by diminishing the physiological muscle pump required for venous return.
Symptoms and Appearance
Venous ulcers present very differently from arterial ulcers, reflecting chronic venous congestion rather than ischemia:
- Location: Typically found on the lower leg, particularly around the inner ankle (medial malleolus), in an area known as the "gaiter region." Less commonly, they appear laterally or circumferentially around the calf.
- Appearance: The wound is usually shallow with irregular, sloping edges that lack clear demarcation. The base is often red or pink with healthy-looking granulation tissue but may be covered with a yellowish fibrin slough. Venous ulcers tend to be wet and weepy, with moderate to heavy serous or serosanguinous fluid drainage due to elevated capillary filtration pressure.
- Surrounding Skin: The skin around the ulcer often shows signs of chronic venous stasis, including brownish or purplish discoloration (hemosiderin staining from red blood cell breakdown), significant swelling (edema), and a hardened, woody, or leathery texture (lipodermatosclerosis). Atrophie blanche (white, atrophic, starburst-shaped scars) may also be present. The skin is frequently itchy (stasis dermatitis) and prone to scaling or eczema-like flares.
- Pain: The pain is often described as a dull ache, throbbing, or a heavy sensation in the leg, which worsens with prolonged standing or sitting and improves significantly with leg elevation. Unlike arterial pain, it rarely wakes patients at night unless edema is severe.
- Pulses: Foot pulses are typically normal and easy to palpate, as the macrovascular arterial system remains intact. However, in advanced mixed disease, pulses may be dampened.
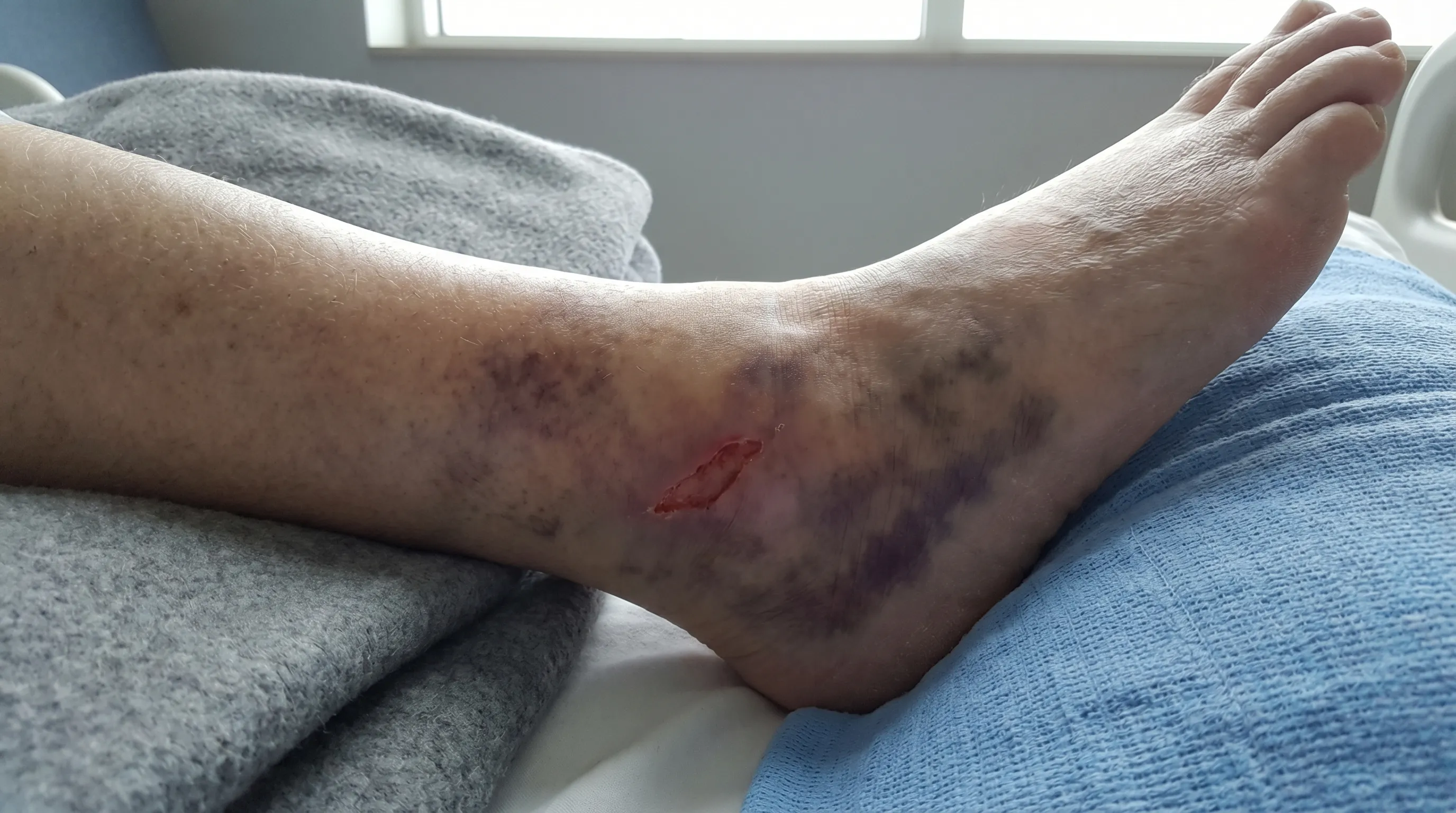 An example of a venous ulcer above the inner ankle. Note the irregular shape, shallow depth, and the characteristic brown skin discoloration from chronic blood pooling.
An example of a venous ulcer above the inner ankle. Note the irregular shape, shallow depth, and the characteristic brown skin discoloration from chronic blood pooling.
The Clinical-Etiology-Anatomy-Pathophysiology (CEAP) classification is often used to grade venous disease severity. Ulceration represents C6 (active ulcer), while C5 indicates a healed ulcer, emphasizing that venous disease is chronic and lifelong management is required to prevent recurrence.
Arterial vs. Venous Ulcers: A Side-by-Side Comparison
| Feature | Arterial Ulcer (Ischemic) | Venous Ulcer (Stasis) |
|---|---|---|
| Primary Cause | Poor arterial blood supply (lack of oxygenated blood) | Poor venous blood return (blood pooling in legs) |
| Location | Toes, feet, heels, outer ankle | Inner ankle, lower calf ("gaiter area") |
| Appearance | Deep, "punched-out," with well-defined edges | Shallow, with irregular, sloping edges |
| Wound Base | Pale, gray, or black (necrotic); typically dry | Red or pink; typically wet or oozing |
| Pain | Severe, sharp pain; worse with leg elevation | Dull, aching pain; better with leg elevation |
| Surrounding Skin | Cool, pale, shiny, hairless | Warm, swollen, brownish discoloration, hardened |
| Foot Pulses | Weak or absent | Normal |
| Core Treatment | Restore blood flow (e.g., surgery). No compression. | Improve venous return. Compression is key. |
Understanding this comparison is the foundation of clinical assessment. However, approximately 15-20% of leg ulcers are mixed etiology, displaying overlapping features of both PAD and CVI. These require careful hemodynamic evaluation to balance revascularization needs with modified compression therapy.
Diagnosis and When to See a Doctor
Proper diagnosis is crucial because treatments are fundamentally different. A healthcare provider, often a vascular specialist or wound care nurse, will perform a comprehensive physical exam, review your medical history, assess wound dimensions, and order diagnostic tests:
- Ankle-Brachial Index (ABI): A simple, non-invasive test using Doppler probes to compare systolic blood pressure in the ankle to the arm. A normal ratio is 1.0–1.4. Values below 0.9 suggest PAD, below 0.5 indicate severe ischemia, and values above 1.3 often indicate non-compressible, calcified arteries (common in diabetes and chronic kidney disease).
- Toe-Brachial Index (TBI): Used when ABIs are falsely elevated due to calcification. Toe arteries rarely calcify, making TBI highly reliable in diabetic patients.
- Duplex Ultrasound: Combines traditional ultrasound imaging with Doppler flow studies. It maps arterial blockages, evaluates venous valve function, measures reflux duration, and identifies deep or superficial venous incompetence.
- Transcutaneous Oximetry (TcPO2): Measures oxygen tension at the skin surface. Values below 30 mmHg predict poor healing potential without revascularization.
- Angiography/CTA/MRA: Advanced imaging reserved for pre-surgical planning to visualize the exact location, length, and severity of arterial blockages.
You should seek medical help immediately if:
- You have an open sore on your leg or foot that isn't healing within 2–4 weeks despite proper home care.
- The wound shows signs of infection, such as increased redness, warmth, pus, a foul odor, expanding cellulitis, or fever.
- You experience severe leg pain, especially at rest or at night, disrupting sleep.
- Your foot becomes cold, pale, blue, or numb, which may indicate acute limb ischemia—a surgical emergency.
- You notice sudden, severe swelling and redness, which could signal a new DVT or rapidly progressing infection.
Early intervention dramatically reduces the risk of osteomyelitis (bone infection), sepsis, and major amputation. A multidisciplinary approach involving vascular surgery, dermatology, wound care specialists, and primary care yields the best outcomes.
Treatment Options for Leg Ulcers
Treating Arterial Ulcers
The primary goal is to restore blood flow to the affected limb, as wounds cannot heal without adequate oxygen and nutrient delivery.
- Revascularization: This is the definitive treatment. Endovascular techniques like balloon angioplasty, stenting, or atherectomy are preferred for shorter lesions. For long-segment disease or multiple blockages, surgical bypass (e.g., femoral-to-tibial bypass using autologous vein grafts) offers durable results.
- Wound Care: The wound is kept clean and protected with non-adherent, moisture-maintaining dressings. Sharp or aggressive debridement (removal of dead tissue) is typically contraindicated or delayed until circulation is objectively improved, as removing the protective eschar in ischemic tissue can expose deeper structures and rapidly worsen necrosis. Autolytic or enzymatic debridement may be used cautiously.
- Lifestyle Changes: Quitting smoking is non-negotiable for improving microcirculation and surgical outcomes. Structured exercise programs (supervised walking therapy) stimulate collateral vessel growth. Managing diabetes, blood pressure, and cholesterol slows disease progression.
- Medications: Antiplatelet drugs (aspirin, clopidogrel) reduce cardiovascular events. Statins stabilize plaques and improve endothelial function. Cilostazol may improve walking distance in mild-to-moderate claudication. Broad-spectrum antibiotics are prescribed only for confirmed infection, not prophylactically.
- Important: Compression therapy should NOT be used on arterial ulcers, as it can further restrict already compromised arterial inflow, accelerate ischemia, and precipitate gangrene. If ABI is below 0.8, compression is generally avoided or heavily modified.
Treating Venous Ulcers
The cornerstone of treatment is to improve venous return, reduce ambulatory venous hypertension, and manage exudate.
- Compression Therapy: The gold standard. Multi-layer compression bandaging systems (providing 30–40 mmHg at the ankle) significantly improve healing rates. Once healed, prescription-grade graduated compression stockings (20–30 mmHg or 30–40 mmHg) are worn daily to prevent recurrence. Intermittent pneumatic compression pumps are useful for patients unable to tolerate bandages.
- Leg Elevation: Elevating the legs above heart level for 30 minutes, 3-4 times a day, utilizes gravity to drain pooled fluid. Proper positioning involves reclining with feet propped higher than hips.
- Wound Care: The wound is cleaned with gentle saline irrigation. Dressing choice depends on exudate levels: highly absorbent foams, alginates, or hydrofibers manage heavy drainage while preventing maceration. The goal is a balanced moist wound environment. Silver or iodine-impregnated dressings may be used temporarily for high bacterial loads or critical colonization.
- Exercise: Walking and simple ankle flexion/extension exercises activate the calf muscle pump, enhancing venous ejection and reducing stasis. Supervised exercise programs improve calf function and ulcer healing times.
- Pharmacological & Procedural Adjuncts: Pentoxifylline improves blood rheology and is FDA-approved as an adjunct to compression for healing venous ulcers. Topical or oral corticosteroids/antihistamines may manage severe stasis dermatitis itch. For non-healing or recurrent ulcers, early endovenous ablation (laser, radiofrequency) or ultrasound-guided sclerotherapy of superficial refluxing veins is now strongly recommended and accelerates closure.
Additional Considerations for Both Types
Infection control, nutritional optimization (adequate protein, vitamins A, C, zinc), and blood glucose management are universal requirements. Negative pressure wound therapy (NPWT) may be considered for large, clean wounds once perfusion is adequate. Biologics or skin substitutes can be deployed for stalled ulcers after underlying pathophysiology is addressed.
For a visual guide, you can watch videos from reliable medical sources that explain these differences.
Watch an animated video explaining the circulatory differences between arterial and venous ulcers.
Prevention Strategies
Preventing recurrence is just as important as initial healing, as chronic leg ulcers have high relapse rates.
- For Arterial Ulcers: Focus on comprehensive cardiovascular risk reduction. Quit smoking through behavioral counseling or pharmacotherapy. Maintain a healthy weight via a Mediterranean-style diet. Exercise regularly (30 minutes of brisk walking 5 days/week) to promote collateral circulation. Strictly manage blood pressure, LDL cholesterol, and blood sugar. Inspect your feet and legs daily using a mirror to check for cracks, blisters, or discoloration between the toes and on the heels. Wear properly fitted, seamless, cushioned footwear to prevent friction injuries. Avoid walking barefoot and never use heating pads or hot water soaks on insensate or poorly perfused limbs, as they increase metabolic demand and burn risk.
- For Venous Ulcers: Manage vein health proactively. Wear medical-grade compression stockings daily, putting them on before getting out of bed while edema is minimal. Replace stockings every 3–6 months as elastic fibers degrade. Avoid prolonged periods of standing or sitting; if your job requires it, take movement breaks every 30–45 minutes to contract calf muscles. Maintain a healthy weight to reduce abdominal pressure on pelvic veins. Elevate your legs above heart level whenever resting. Keep skin hydrated with fragrance-free emollients to maintain barrier function and prevent fissures, but avoid applying heavy creams between the toes. Treat new varicose veins or episodes of cellulitis promptly. Consider early vein ablation if superficial reflux is documented, as it significantly reduces ulcer recurrence.
- General Wound Vigilance: Seek professional evaluation for any skin breakdown that doesn't show signs of improvement within 2 weeks. Chronic ulcers can occasionally undergo malignant transformation (Marjolin’s ulcer), so any wound that rapidly enlarges, becomes increasingly painful, or develops raised, everted edges should be biopsied. Regular follow-ups with a vascular specialist or wound care clinic ensure ongoing monitoring of perfusion status and dressing compliance.
Frequently Asked Questions
Can a leg ulcer be both arterial and venous at the same time?
Yes, mixed etiology ulcers are relatively common, particularly in older adults with long-standing chronic venous insufficiency who also develop age-related or lifestyle-related peripheral artery disease. These wounds display overlapping features, such as irregular borders but dry wound beds, or location near the medial ankle but cool, hairless surrounding skin. Diagnosis requires careful ABI/TBI testing and duplex ultrasound. Treatment typically involves cautious, low-pressure compression (if ABI is >0.6 and <0.8) or referral for revascularization before implementing full compression protocols.
How long does it typically take for each type of ulcer to heal?
Healing timelines vary significantly based on ulcer size, patient comorbidities, and treatment adherence. Venous ulcers, when treated with appropriate compression and wound care, often show measurable improvement within 4–6 weeks and may heal completely in 12–24 weeks. Arterial ulcers will rarely heal without revascularization. Once blood flow is successfully restored, healing typically takes 8–16 weeks, but extensive tissue loss or uncontrolled diabetes can extend this timeline. Consistency in offloading, dressing changes, and lifestyle modifications directly impacts closure rates.
Is surgery always required to heal an arterial ulcer?
Not always, but it is frequently necessary for moderate-to-severe arterial insufficiency. Mild cases with an ABI between 0.7 and 0.9 may respond to aggressive medical management, structured exercise therapy, smoking cessation, and meticulous wound care. However, if the ABI is below 0.5, if rest pain is present, or if the ulcer fails to show progress after 4–6 weeks of conservative therapy, surgical or endovascular revascularization becomes essential to prevent limb loss.
Do venous ulcers increase the risk of blood clots?
Venous ulcers themselves do not cause deep vein thrombosis (DVT), but they share the same underlying risk factors. Chronic venous insufficiency, immobility, and inflammation create a prothrombotic environment that can predispose patients to new DVTs or post-thrombotic syndrome exacerbations. Additionally, severe infection or sepsis stemming from an ulcer can trigger systemic coagulation activation. Wearing prescribed compression, staying mobile, and adhering to anticoagulation (if previously prescribed) significantly mitigate these risks.
What is the best dressing for each ulcer type?
Dressing selection should match the wound bed environment and exudate level. Arterial ulcers are typically dry and require dressings that maintain moisture without adhering to fragile tissue. Non-adherent silicone meshes, hydrogels, or simple petroleum-impregnated gauze are often appropriate until perfusion improves. Venous ulcers produce moderate to heavy exudate; therefore, highly absorbent dressings like calcium alginate, hydrofiber, or polyurethane foam are preferred to manage moisture, prevent maceration, and protect periwound skin. Antimicrobial dressings may be added temporarily if infection is suspected, but standard moist wound healing principles remain the foundation for both.
Conclusion
Differentiating between arterial and venous ulcers is a fundamental step in effective wound management and limb preservation. Arterial ulcers, driven by oxygen deprivation from peripheral artery disease, present as deep, dry, and exquisitely painful wounds distal on the foot or toes, demanding prompt vascular assessment and revascularization while strictly avoiding compression. Venous ulcers, stemming from chronic venous insufficiency and valvular reflux, manifest as shallow, moist, and irregular wounds near the inner ankle, responding best to sustained compression therapy, leg elevation, and targeted vein procedures when necessary.
Accurate diagnosis through clinical examination, ABI measurement, and vascular imaging ensures that patients receive the correct, targeted intervention. Mismanagement not only delays healing but actively worsens tissue damage. A proactive, multidisciplinary approach combining medical therapy, specialized wound care, lifestyle modification, and patient education offers the highest likelihood of successful closure and long-term prevention. If you notice any persistent skin breakdown on your lower legs or feet, consult a healthcare provider promptly. Early recognition, correct classification, and consistent adherence to prescribed therapy can restore mobility, prevent serious complications, and significantly improve your overall quality of life.

About the author
Elena Vance, MD, is a double board-certified dermatologist and pediatric dermatologist. She is an assistant professor of dermatology at a leading medical university in California and is renowned for her research in autoimmune skin disorders.