The Ultimate Guide to Compression Stockings for Varicose Veins

Key points
- Improves Blood Flow: The graduated pressure gently squeezes the leg tissues and vein walls, helping to push blood back up toward the heart and preventing it from pooling. By reducing the caliber (diameter) of distended superficial veins, the stockings improve blood velocity and reduce venous stasis, which is a major risk factor for inflammation and clot formation.
- Supports Vein Valves: The external support helps the weakened valves function more effectively. When the external pressure reduces venous diameter, the valve leaflets can coapt (close) more completely, minimizing retrograde blood flow (reflux) and restoring more efficient venous return.
- Reduces Swelling: By improving circulation and reducing pressure in the veins, compression helps move excess fluid out of the leg tissues, significantly decreasing swelling (edema). The external pressure counteracts capillary filtration forces, reducing the leakage of plasma into the interstitial space and promoting lymphatic drainage.
If you're dealing with the discomfort of varicose veins—the aching, swelling, and heavy feeling in your legs—you've likely heard about compression stockings. These specially designed garments are more than just tight socks; they are a first-line medical tool for managing symptoms and improving quality of life.
Varicose veins affect approximately 23% of all adults and over 50% of those over the age of 50, making it one of the most prevalent chronic vascular conditions worldwide. The impact on daily life can be profound, limiting mobility, disrupting sleep, and causing significant emotional distress. While surgical and minimally invasive treatments have advanced considerably, conservative management remains the cornerstone of care for millions of patients globally. At the center of this conservative approach are medical-grade compression garments.
This comprehensive guide synthesizes medical expertise, scientific research, and practical user experience to cover everything you need to know, from how they work and how to choose the perfect pair to the critical safety information often overlooked. Whether you have been newly diagnosed with early-stage chronic venous disease or are seeking relief from long-standing venous insufficiency, understanding the proper use, selection, and physiological impact of compression therapy is essential for achieving optimal outcomes.
How Compression Stockings Work for Varicose Veins
Varicose veins occur when the one-way valves inside your leg veins weaken or fail, causing blood to flow backward and pool. This increases pressure, making the veins bulge and twist. The underlying condition, often termed chronic venous insufficiency (CVI), disrupts the normal unidirectional flow of blood toward the heart and places abnormal hydrostatic stress on the superficial venous system.
Compression stockings apply external pressure to your legs in a specific way to counteract this process. The key is graduated compression: the stockings are tightest at the ankle and the pressure gradually decreases as they go up the leg. This pressure gradient typically follows a specific ratio, with approximately 100% of the prescribed compression at the ankle, 70-90% at the mid-calf, and 50-60% at the upper thigh (for thigh-high models).
This mechanism accomplishes several things:
- Improves Blood Flow: The graduated pressure gently squeezes the leg tissues and vein walls, helping to push blood back up toward the heart and preventing it from pooling. By reducing the caliber (diameter) of distended superficial veins, the stockings improve blood velocity and reduce venous stasis, which is a major risk factor for inflammation and clot formation.
- Supports Vein Valves: The external support helps the weakened valves function more effectively. When the external pressure reduces venous diameter, the valve leaflets can coapt (close) more completely, minimizing retrograde blood flow (reflux) and restoring more efficient venous return.
- Reduces Swelling: By improving circulation and reducing pressure in the veins, compression helps move excess fluid out of the leg tissues, significantly decreasing swelling (edema). The external pressure counteracts capillary filtration forces, reducing the leakage of plasma into the interstitial space and promoting lymphatic drainage.
Furthermore, compression stockings enhance the function of the calf muscle pump, often referred to as the "second heart." When you walk, your calf muscles contract and expand. The external compression amplifies this mechanical action, forcefully expelling venous blood from the lower leg into the deeper, healthier venous system. This synergistic effect between external pressure and muscle contraction is what makes compression therapy so physiologically effective.
As explained by medical experts at Yale Medicine, this external pressure can effectively reduce the swelling and leg fatigue caused by varicose veins [[1]].
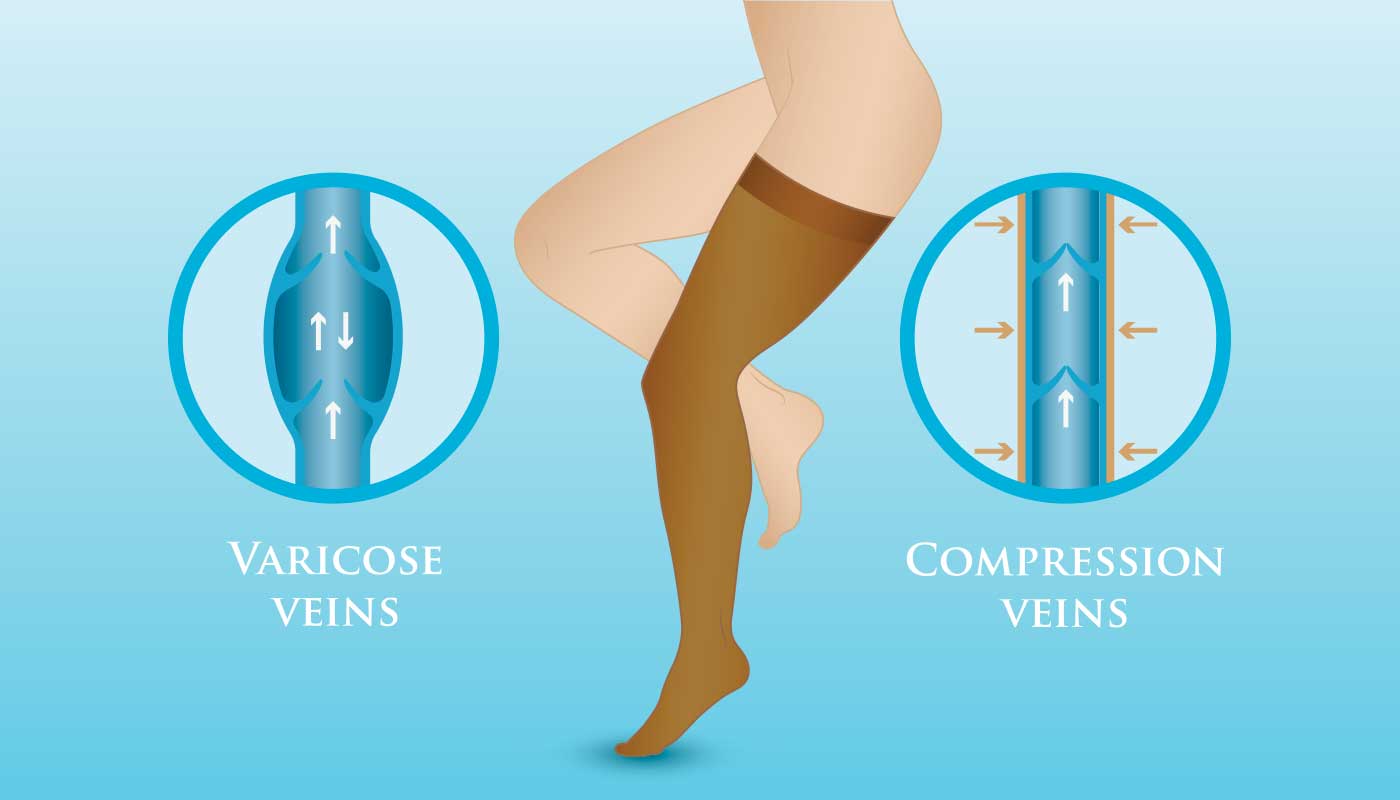 Image Source: Miami Vein Center [2]
Image Source: Miami Vein Center [2]
The Benefits: From Symptom Relief to Disease Management
The effectiveness of compression stockings extends across a spectrum, from immediate comfort to long-term health benefits. Modern vascular medicine recognizes compression therapy not merely as a palliative measure, but as an active intervention that alters disease progression and improves microcirculatory function.
Immediate Symptom Management
The most noticeable benefit is relief from the daily symptoms of varicose veins. According to research cited by the National Institutes of Health (NIH), graduated compression hosiery is a widely used first-line treatment that can significantly reduce pain, heaviness, swelling, and cramping [4]. Many patients report noticeable improvement within days of consistent use. The reduction in transmural pressure across the venous wall alleviates the stretching and irritation of nerve endings, which directly correlates with decreased aching, throbbing, and the sensation of restless legs often experienced in the evening hours.
Preventing Progression and Complications
While compression therapy may not prevent the initial formation of varicose veins, it plays a vital role in managing the progression of Chronic Venous Disease (CVD). CVD is typically classified using the CEAP system (Clinical, Etiological, Anatomical, Pathophysiological), ranging from C1 (spider veins) to C6 (active venous ulcers). Compression therapy is applicable across multiple stages of this classification.
- Slowing Disease Progression: By improving venous hemodynamics, compression can help mitigate the progressive dysfunction of your venous system. It reduces venous hypertension, which is the primary driver of inflammatory cascades that damage the venous wall and surrounding tissues over time.
- Preventing Ulcers: For individuals with severe CVD, compression is proven to reduce the risk of developing venous leg ulcers and is critical in preventing their recurrence. The reduction in edema improves local tissue oxygenation, allowing the skin to remain intact and better withstand minor trauma.
- Managing Post-Thrombotic Syndrome (PTS): After a deep vein thrombosis (DVT), wearing compression stockings is recommended to help prevent the long-term complication of PTS, which causes chronic leg pain and swelling. By maintaining venous patency and supporting the remaining functional valve network, compression helps patients maintain mobility and reduce post-DVT discomfort.
Aiding Post-Intervention Recovery
If you undergo a procedure like surgery or sclerotherapy for your varicose veins, your doctor will likely recommend wearing compression stockings for a period afterward. This helps reduce post-operative pain, swelling, and bruising, leading to a more comfortable recovery. Following endovenous laser ablation (EVLA) or radiofrequency ablation (RFA), compression ensures that treated veins remain closed and minimizes the formation of superficial thrombophlebitis. It also helps appose the treated vessel walls together, promoting optimal fibrosis and healing. Most vascular specialists advise continuous wear (day and night) for the first 24-72 hours post-procedure, followed by daytime-only wear for two to four weeks.
Choosing the Right Compression Stockings: A Complete Guide
Selecting the right pair of stockings is crucial for both comfort and therapeutic effect. It involves more than just picking a color and size. The market is flooded with over-the-counter options that range from inexpensive athletic socks to clinically engineered medical devices, making it essential for patients to understand the distinctions.
Understanding Compression Levels (mmHg)
Pressure is measured in millimeters of mercury (mmHg). The right level depends on your specific condition, clinical diagnosis, and physician recommendations. Self-prescribing higher compression levels can lead to complications, which is why proper staging of your venous disease is recommended before purchase.
- Mild Support (8-15 mmHg): Good for minor leg fatigue and travelers. Not typically sufficient for managing existing varicose veins. Often marketed as "travel socks" or "light support," these provide gentle comfort for individuals who sit or stand for prolonged periods but do not yet exhibit visible venous disease.
- Moderate Compression (15-20 mmHg): An over-the-counter option for preventing varicose veins during pregnancy or managing very mild swelling and aching. This range is frequently recommended for early-stage reticular veins, mild edema, and occupational venous stress. It serves as a transitional step for patients moving toward higher-grade medical therapy.
- Medical Grade Class I (20-30 mmHg): This is the most frequently prescribed level for varicose veins. It is effective for managing swelling, spider veins, post-surgical recovery, and mild-to-moderate CVI. It provides substantial hemodynamic correction and is generally well-tolerated by most patients once they adapt to the fit.
- Medical Grade Class II (30-40 mmHg): A prescription-strength level for more severe varicose veins, moderate edema, lymphedema, and DVT management. This level is indicated for patients with active symptoms of venous hypertension, post-thrombotic syndrome, and early venous ulceration. Medical supervision is highly recommended.
- Medical Grade Class III (40-50 mmHg): A high-level compression used for severe venous conditions, typically under strict medical supervision. It is reserved for advanced lymphedema, severe post-thrombotic syndrome, refractory venous ulcers, and patients with extensive venous malformations. Due to the high pressure, arterial assessment (Ankle-Brachial Index testing) is mandatory before use.
Getting the Perfect Fit: Measurement is Key
An improper fit can render the stockings ineffective or even harmful. Stockings that are too loose will slide down and fail to provide therapeutic pressure. Stockings that are too tight can cause skin breakdown, nerve compression, or arterial restriction. For the best results, you must measure your legs.
- When to Measure: Take measurements first thing in the morning, before swelling occurs. Leg volume can increase by 10-20% throughout the day due to gravity and fluid accumulation.
- What to Measure:
- Ankle: Measure the circumference at the narrowest point, just above the ankle bone (malleolus). This is where the maximum therapeutic pressure is intended to be concentrated.
- Calf: Measure the circumference at the widest part of your calf. For patients with pronounced calf musculature or significant swelling, custom garments may be necessary.
- Length: For knee-highs, measure from the floor to the bend of your knee. For thigh-highs, measure from the floor to the gluteal fold. Length ensures the fabric isn't stretched excessively, which would compromise the mmHg gradient.
- Thigh (for thigh-highs): Measure the circumference at the widest part of your thigh.
Use these measurements to consult the sizing chart provided by the stocking manufacturer. If you are unsure, a professional at a medical supply store can help. It is also worth noting that if your leg circumference varies significantly between the two legs, you may need to purchase mismatched sizes for each leg to maintain optimal therapeutic gradients.
 Image Source: MedicalNewsToday [5]
Image Source: MedicalNewsToday [5]
Selecting Style and Material
- Style: Knee-high stockings are the most common and are sufficient if your varicose veins are below the knee. If they extend higher, thigh-highs or pantyhose are necessary. Waist-high pantyhose provide abdominal compression and stay up better for some patients, but they can be more difficult to don and doff. Open-toe styles are popular for patients who have foot edema, toe arthritis, or simply prefer the comfort and breathability of their own footwear. Closed-toe styles offer better heel coverage and prevent slipping inside shoes.
- Material: Modern compression stockings come in a variety of materials, from opaque fabrics for durability to sheer options for a more cosmetic look. Look for breathable materials like nylon-spandex blends, microfibers, and bamboo-infused textiles that wick moisture away from the skin. Advanced fabrics now incorporate silver-ion or copper-ion threads for natural antimicrobial and odor-control properties, which are particularly beneficial for patients who wear their garments daily in warm climates.
- Grip Technology: For thigh-high stockings, silicone grip bands or adhesive strips are used to prevent rolling down. While silicone grips are highly effective, they can sometimes cause skin irritation in sensitive individuals. In such cases, garter belt attachments or pantyhose styles with built-in compression gradients may be better alternatives.
How to Correctly Wear and Care for Your Stockings
Proper application and care will maximize the benefits and extend the life of your garments. The therapeutic pressure of compression stockings relies entirely on their elastic integrity and correct positioning. Improper donning or poor maintenance can rapidly degrade the fabric's ability to maintain the prescribed mmHg levels.
Step-by-Step Guide to Putting on Compression Stockings
Because they are so snug, putting them on can be a challenge. Developing a consistent routine will significantly reduce frustration and protect the fabric.
- Start Early & Dry: Put them on in the morning before your legs swell. Ensure your skin is completely dry. Applying a bit of cornstarch or talcum powder can help. Patients with particularly dry skin or those who experience morning stiffness should consider moisturizing the night before and allowing it to fully absorb to prevent skin slippage inside the garment.
- Turn Inside-Out: Reach inside the stocking and grab the heel. Pull the stocking inside-out, stopping at the heel. This technique allows you to slide the foot portion on smoothly without stretching the calf and ankle sections prematurely.
- Position Your Foot: Slide your foot into the stocking until your heel is perfectly positioned in the heel pocket. Make sure there are no wrinkles under your arch or toes. For open-toe varieties, align your toes with the designated opening.
- Unroll, Don't Pull: Gently unroll the rest of the stocking up your leg. Work in small increments, smoothing as you go. Avoid yanking or rolling the top band, which can overstretch the fabric and destroy the pressure gradient. If you have long nails or wear rings, remove them temporarily to prevent snagging the delicate fibers.
- Smooth It Out: Adjust the fabric so it is smooth and free of wrinkles. Wrinkles or bunching can create a tourniquet effect and be dangerous. Do not fold the top band over. If the stocking feels uneven, take it off and start over. A perfectly smooth garment ensures uniform pressure distribution.
For those with arthritis or limited strength, rubber gloves can provide a better grip, and a special device called a "stocking donner" can make the process much easier. Stocking donners are cone-shaped frames that hold the garment in place, allowing you to slide your leg through without excessive pulling.
Daily Wear and Care Routine
- Wear Duration: Wear your stockings all day, from the time you get up until you go to bed. The moment you lie down and elevate your legs, venous pooling decreases, making continuous daytime wear essential for maintaining symptom control.
- Hygiene: Remove them at night and for bathing. It's recommended to have at least two pairs so you can wear one while the other is being washed. Alternating pairs allows the elastic fibers to fully relax and recover, extending the garment's lifespan.
- Washing: Hand wash them daily in lukewarm water with a mild soap and hang them to air dry. This preserves their elasticity. Avoid bleach, fabric softeners, and harsh detergents, as these chemicals degrade the spandex and microfiber components. If machine washing is absolutely necessary, use a delicate mesh bag and the gentlest cycle. Never use a clothes dryer; the heat rapidly breaks down the elastic polymers.
- Replacement: Compression stockings lose their compressive strength over time. They should be replaced every 3 to 6 months to ensure they continue to provide the correct medical-grade pressure. Signs that your stockings need replacing include visible thinning, loss of the snug fit, frequent rolling down despite correct sizing, or the appearance of shiny patches where the fabric has become overstretched. Keeping a purchase calendar helps you track replacement intervals.
Important Safety Considerations: Risks and Contraindications
While highly beneficial for many, compression stockings are not safe for everyone and can cause harm if used improperly. It is crucial to consult a healthcare professional before using moderate to firm compression stockings (20 mmHg and above). A thorough clinical evaluation, including a peripheral arterial assessment, is standard practice to ensure safe application.
Who Should NOT Wear Compression Stockings?
There are several absolute contraindications that must be respected to prevent iatrogenic harm:
- Severe Peripheral Arterial Disease (PAOD): The external pressure can worsen already compromised blood flow in the arteries, leading to severe pain and tissue damage. If your Ankle-Brachial Index (ABI) is below 0.8, compression therapy is generally contraindicated. Arterial insufficiency requires increased blood delivery to tissues, and compression directly opposes this by restricting arterial inflow.
- Decompensated Heart Failure: The increased blood flow returning to the heart can overload an already weakened cardiac system. Sudden mobilization of peripheral edema back into the central circulation can precipitate acute pulmonary edema or exacerbate congestive symptoms.
- Advanced Peripheral Neuropathy: Individuals who cannot feel pain or pressure in their legs (often due to diabetes) may not notice if the stockings are causing injury. Without protective sensation, patients are at high risk for undetected pressure ulcers, blistering, and skin breakdown. Diabetic patients with neuropathy should only use light-to-moderate compression under strict podiatric supervision.
- Certain Skin Conditions: Active cellulitis, weeping dermatoses, or allergies to the stocking material are also contraindications. Compression applied over infected or severely compromised skin can trap bacteria, worsen inflammation, and accelerate tissue necrosis.
Risks of Improper Use
- Skin Damage: Incorrectly sized or wrinkled stockings can create excessive pressure over bony areas (like the shin or ankle), leading to skin irritation, blisters, or even tissue necrosis (tissue death). Patients with fragile, aging skin or those on long-term corticosteroid therapy are particularly vulnerable to shear forces and micro-tears.
- Nerve Damage: Persistent, focused pressure near the top of the calf can potentially damage the common peroneal nerve, leading to numbness or foot drop. The fibular head is anatomically vulnerable, and ill-fitting thigh-high stockings that dig into this area must be adjusted immediately.
- Discomfort and Pain: Stockings that are too tight or bunched can be painful and may actually restrict circulation. New users often experience initial tightness, but sharp pain, tingling, or cold extremities are warning signs that the garment must be removed and reassessed.
Daily skin checks are essential. When you remove your stockings, inspect your legs and feet for any signs of irritation or damage. Maintain a strict moisturizing routine to preserve the skin barrier, but always allow lotions to absorb completely before donning compression. Keep a journal of your symptoms, noting any changes in skin color, temperature, or sensation, and share these observations with your vascular specialist during routine follow-ups.
Beyond Stockings: Complementary Lifestyle Changes
Compression stockings are most effective when combined with other healthy habits. As recommended by the Mayo Clinic, these lifestyle changes can help manage varicose veins:
- Get Regular Exercise: Walking is excellent for promoting blood circulation in your legs. Low-impact aerobic activities like cycling, swimming, and yoga specifically target the calf muscle pump without placing excessive joint stress. Avoid high-impact exercises that cause sudden, heavy pounding if you have active venous symptoms.
- Manage Your Weight: Losing excess pounds reduces pressure on your veins. Adipose tissue in the abdomen and pelvic region increases intra-abdominal pressure, which directly impedes venous return from the lower extremities. Even a modest weight reduction of 5-10% can significantly alleviate venous hypertension and improve symptom profiles.
- Elevate Your Legs: When resting, raise your legs above the level of your heart several times a day. Gravity works in your favor during elevation, facilitating rapid venous drainage and reducing capillary filtration pressure. Use pillows or a wedge cushion to achieve proper alignment without straining your lower back.
- Avoid Prolonged Sitting or Standing: Change your position frequently to encourage blood flow. If your occupation requires long hours at a desk or workstation, take a two-minute walking or calf-stretching break every 30-60 minutes. If standing is unavoidable, shift your weight from foot to foot, perform subtle heel raises, or use an anti-fatigue mat to engage the calf musculature.
- Choose Proper Footwear: Avoid high heels, which can alter your calf muscle pump function. Opt for low-heeled, supportive shoes that allow full range of motion in the ankle joint. The natural flexion and extension of the ankle during walking is what drives venous emptying from the lower leg.
- Dietary Modifications: A high-fiber, low-sodium diet supports venous health. Fiber prevents constipation, which reduces straining and subsequent intra-abdominal pressure spikes that stress pelvic and leg veins. Reducing sodium intake helps minimize systemic fluid retention and peripheral edema. Staying adequately hydrated also maintains healthy blood viscosity, promoting smoother venous flow.
Frequently Asked Questions
Can I sleep in my compression stockings?
Generally, medical professionals advise against sleeping in standard graduated compression stockings. When you lie flat at night, the effect of gravity on your lower extremity venous system is neutralized, meaning venous pressure drops significantly. Adding compression while supine can unnecessarily restrict arterial blood flow to your feet and may cause discomfort or numbness. Exceptions exist for patients who must keep their legs elevated but cannot, or immediately following certain vein procedures where doctors specifically instruct 24/7 wear for the first few days. Always follow your physician's exact post-procedure protocol.
Do compression stockings make veins worse if you stop wearing them?
No, compression stockings do not cause dependency or worsen underlying venous disease when discontinued. They function mechanically while worn, providing external support and improving hemodynamics, but they do not permanently alter vein anatomy or valve function. If you stop wearing them, your symptoms will gradually return to their baseline state because the underlying venous insufficiency remains. They are a management tool, not a cure. Consistent use, however, effectively delays disease progression and prevents complications during the time you wear them.
Are there any natural alternatives to medical-grade compression stockings?
While over-the-counter support socks, herbal supplements (like horse chestnut seed extract or Diosmin), and leg elevation can provide mild symptom relief, they do not replicate the precise, graduated pressure gradients required to treat chronic venous insufficiency or prevent venous ulcers. Support socks typically offer uniform compression, which can actually trap blood at the ankle rather than promoting upward flow. Supplements may reduce capillary permeability and mild edema, but they cannot mechanically support failing valves. For diagnosed varicose veins with symptomatic venous hypertension, medically graded compression remains the gold standard conservative therapy.
How do I know if my stockings are too tight or too loose?
Properly fitted compression stockings should feel snug but not painful. If they leave deep red indentations that persist more than 15-20 minutes after removal, cause numbness, tingling, cold toes, or visible skin discoloration (bluish or pale), they are too tight. Conversely, if they constantly slip down the leg, form large wrinkles around the calf, or fail to provide noticeable symptom relief after two weeks of consistent daytime use, they are likely too loose or have lost their elastic integrity. A well-fitted medical-grade stocking should feel like a firm, supportive hug that becomes more comfortable as you move and walk throughout the day.
Can men wear compression stockings for varicose veins?
Absolutely. Varicose veins are a physiological condition, not a gender-specific cosmetic issue. While marketing has historically targeted women, men develop venous disease at significant rates, particularly those with occupations requiring prolonged standing, athletes with high lower-body muscle mass, or men with a family history of venous insufficiency. Many medical brands offer masculine styles, colors, and materials, including crew-length socks, athletic compression garments, and neutral-toned medical hose. The therapeutic principles, sizing, and care instructions are identical regardless of gender.
Conclusion
Compression stockings remain one of the most effective, non-invasive, and scientifically validated interventions for managing varicose veins and chronic venous insufficiency. By understanding the physiological principles of graduated compression, patients can actively participate in their vascular health, experiencing meaningful relief from pain, swelling, and heaviness. The key to successful therapy lies in proper selection, accurate measurement, correct donning techniques, and diligent garment maintenance.
While these garments do not eliminate existing varicose veins, they play a critical role in halting disease progression, preventing serious complications like venous ulcers and deep vein thrombosis, and improving overall quality of life. When combined with targeted lifestyle modifications, regular physical activity, and professional medical guidance, compression therapy becomes a powerful component of a comprehensive vascular care plan. Always consult a qualified healthcare provider to determine the appropriate compression level for your specific condition, ensure arterial safety, and integrate stockings effectively into your long-term health strategy. With consistent use and informed care, you can significantly reduce venous symptoms and maintain active, comfortable mobility for years to come.
References
[1] Yale Medicine. (2024). Blood Clots, Varicose Veins, and Sore Legs: Can Compression Socks Help? https://www.yalemedicine.org/news/blood-clots-varicose-veins-sore-legs-compression-socks-help
[2] Miami Vein Center. Compression Stockings for Varicose Veins. https://www.miamivein.com/compression-stockings-for-varicose-veins/
[4] National Center for Biotechnology Information (NCBI). (n.d.). Conservative Management - Varicose Veins in the Legs. https://www.ncbi.nlm.nih.gov/books/NBK328015/
[5] MedicalNewsToday. (2023). Compression stockings for varicose veins: Benefits and risks. https://www.medicalnewstoday.com/articles/321662
[6] Emory Healthcare. (2022). Will Compression Hose Help My Varicose Veins? https://www.emoryhealthcare.org/stories/heart-health/will-compression-hose-help-my-varicose-veins
[7] Mayo Clinic. (2024). Varicose veins - Diagnosis and treatment. https://www.mayoclinic.org/diseases-conditions/varicose-veins/diagnosis-treatment/drc-20350649
[8] Harvard Health Publishing. (2025). Could you benefit from wearing compression socks? https://www.health.harvard.edu/staying-healthy/could-you-benefit-from-wearing-compression-socks

About the author
Marcus Thorne, MD, is a board-certified interventional cardiologist and a fellow of the American College of Cardiology. He serves as the Chief of Cardiology at a major metropolitan hospital in Chicago, specializing in minimally invasive cardiac procedures.