Why Does the Back of My Ribs Ache? A Comprehensive Guide to Causes, Diagnosis, and Relief

Key points
- Sudden twisting motions
- Heavy lifting
- Intense exercise
- Forceful or persistent coughing
An ache in the back of the ribs is a confusing and often alarming symptom. The pain can range from a dull, persistent throb to a sharp, stabbing sensation that catches your breath. Because this area is a complex intersection of bones, muscles, nerves, and is in close proximity to vital organs, pinpointing the cause can be challenging.
This comprehensive guide will help you understand the potential sources of your pain, from common musculoskeletal strains to less common but more serious internal conditions. We will cover how this pain is diagnosed, when you must seek medical attention, and what you can do to find relief. Additionally, we will explore advanced diagnostic pathways, evidence-based rehabilitation strategies, and long-term prevention protocols to help you restore mobility and comfort.
Understanding the Anatomy: Where Your Ribs and Back Connect
Your rib cage is comprised of 12 pairs of ribs. In the back, each rib connects to one of the 12 vertebrae of your thoracic spine (mid-back). These connections, called the costovertebral and costotransverse joints, along with the surrounding muscles and ligaments, allow your rib cage to expand and contract as you breathe. As the Centeno-Schultz Clinic explains, this intricate relationship means that an issue in your mid-back can easily cause pain felt in your ribs, and vice versa.
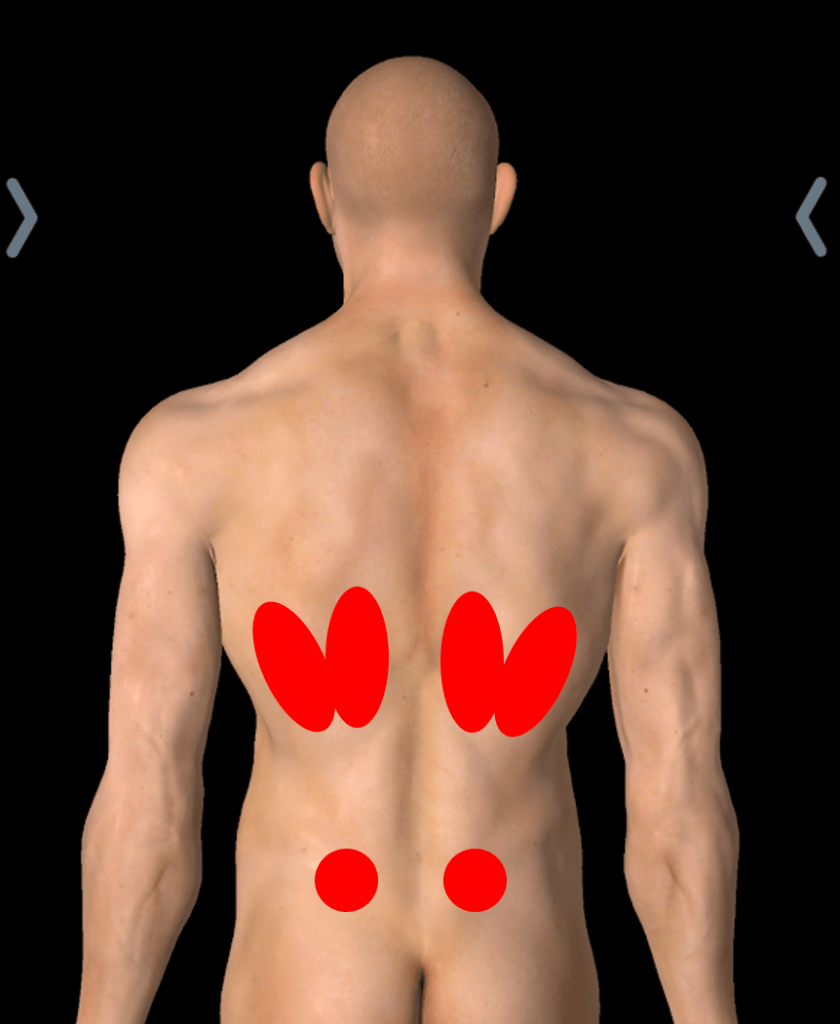 Source: Regenexx
Source: Regenexx
To fully appreciate how pain develops in this region, it is essential to understand the neurological and biomechanical networks at play. The intercostal nerves emerge from the spinal cord, travel between the rib pairs, and provide both motor innervation to the intercostal muscles and sensory feedback to the overlying skin and connective tissue. Because these nerves follow a specific dermatomal pattern, irritation at the spinal root can manifest as pain that wraps around the rib cage, often mimicking visceral or cardiac symptoms. Furthermore, the thoracic spine is structurally designed for stability rather than extreme mobility. It serves as an anchor for the rib cage and provides attachment points for the trapezius, rhomboids, erector spinae, and latissimus dorsi. When compensatory movement patterns force this stable region into excessive flexion, extension, or rotation, microtrauma accumulates in the facet joints and surrounding ligaments, leading to localized inflammation and referred ache.
The fascial system also plays a crucial role in rib and back pain. The thoracolumbar fascia is a dense connective tissue sheet that links the muscles of the mid-back, core, and pelvis. Restrictions or adhesions in this fascia, often caused by sedentary behavior, repetitive strain, or unresolved injuries, can transmit tension directly to the costovertebral joints. This explains why treating the local site of pain is sometimes insufficient; a comprehensive anatomical approach must consider the interconnected kinetic chain that spans from the neck and shoulders down to the hips and core.
Common Musculoskeletal Causes of Back Rib Ache
Most often, an ache in the back of the ribs originates from the musculoskeletal system. This type of pain is typically mechanical, meaning it worsens with certain movements or positions. Mechanical pain often responds predictably to positional changes, targeted exercises, and anti-inflammatory interventions. Understanding the specific biomechanical trigger is the first step toward effective management.
Muscle Strains and Sprains
The intercostal muscles are small muscles located between each rib. They can be easily strained or "pulled" by:
- Sudden twisting motions
- Heavy lifting
- Intense exercise
- Forceful or persistent coughing
An intercostal muscle strain can cause sharp, localized pain, stiffness, and muscle spasms in the upper back and ribs, as noted by Medical News Today. These muscles play a vital role in stabilizing the thorax during respiration and trunk movement. Grade I strains involve microscopic fiber tearing and typically resolve within 2–4 weeks with conservative care. Grade II and III strains involve partial or complete muscle tears, leading to more pronounced swelling, bruising, and functional limitation, often requiring 6–8 weeks of structured rehabilitation. The pain from a strain is usually reproducible with specific actions, such as rotating the torso, taking a deep inhalation, or applying direct pressure along the affected rib space.
Rib Injuries: Bruises and Fractures
A direct blow to the back or chest from a fall, car accident, or contact sport can bruise or fracture a rib. According to Mayo Clinic, a classic symptom of a fractured rib is sharp pain that intensifies when you take a deep breath, cough, laugh, or sneeze. While most rib fractures heal conservatively over 4 to 6 weeks, the risk of complications such as pneumothorax (collapsed lung) or pleural effusion increases with displaced fractures. Bruised ribs, though less severe, can cause prolonged discomfort due to the rich periosteal blood supply and dense nerve endings covering the rib bones. Proper pain management during the healing phase is critical to prevent splinting—a condition where shallow breathing to avoid pain leads to poor lung expansion and secondary pulmonary infections.
Costochondritis and Joint Inflammation
Costochondritis is the inflammation of the cartilage that connects your ribs to the breastbone (sternum). While the pain is most often felt in the front of the chest, it can radiate to the back. The pain is often described as sharp and may worsen with deep breaths or movement. Tietze syndrome is a closely related but less common variant that also presents with visible swelling at the costochondral junctions. Both conditions are frequently idiopathic but can be triggered by viral infections, upper respiratory illnesses, or repetitive mechanical stress from weightlifting, shoveling, or chronic poor posture. The inflammatory cascade involves cytokine release that sensitizes local nociceptors, making normal respiratory movements feel intensely painful. Differentiating this from cardiac or pulmonary conditions typically requires clinical evaluation, as the tenderness is usually reproducible upon palpation of the costosternal or costovertebral joints.
Thoracic Spine and Disc Issues
Problems within your mid-back can directly lead to back rib pain.
- Herniated Disc: A disc in the thoracic spine can bulge and press on a nerve, causing pain that radiates along the nerve's path around the rib cage.
- Spinal Arthritis (Osteoarthritis): The breakdown of cartilage in the facet joints of the spine can cause pain, stiffness, and limited movement, as described by New Jersey Spine Specialists.
Beyond these, degenerative disc disease, spinal stenosis, and vertebral compression fractures can all contribute to radiating rib pain. Thoracic disc herniations account for less than 2% of all symptomatic disc issues, but when they occur, they often cause radicular pain that follows a band-like pattern along the intercostal nerve distribution. Osteoarthritis of the thoracic spine typically develops gradually, characterized by morning stiffness that improves with gentle activity but worsens with prolonged static postures. In older adults, vertebral compression fractures secondary to osteoporosis can occur with minimal trauma, presenting as sudden, focal mid-back pain that may refer anteriorly or laterally along the rib margins. Advanced imaging is often required to visualize subtle nerve compression or structural compromise in these cases.
Posture and Lifestyle Factors
Your daily habits are a significant contributor to back rib ache. Poor posture, especially from prolonged sitting at a computer or looking down at a phone, puts continuous strain on your thoracic spine and the joints where the ribs attach. This can lead to chronic muscle tension and joint irritation, causing a persistent, dull ache. Forward head posture and rounded shoulders (thoracic kyphosis) alter the center of gravity, forcing the paraspinal muscles, trapezius, and rhomboids to work in a constantly lengthened, eccentric state to prevent further collapse. Over time, this leads to muscle fatigue, myofascial trigger points, and joint capsule contractures. The cumulative effect is a feedback loop of pain, stiffness, and compensatory breathing patterns that further strain the intercostal musculature and diaphragm. Addressing postural dysfunction requires a multifaceted approach combining ergonomic optimization, targeted strengthening of the deep cervical and scapular stabilizers, and regular mobility work to restore thoracic extension and rotational capacity.
Repetitive Strain and Overuse Syndromes
Beyond acute injuries, repetitive microtrauma from activities like rowing, swimming, golf, or heavy machinery operation can lead to cumulative rib and back dysfunction. These activities demand high-thoracic rotation and repetitive force transmission through the costovertebral joints. Without adequate recovery, tissue adaptation lags behind mechanical demand, resulting in chronic tendinopathy, periosteal irritation, or stress reactions in the rib cortex. Athletes and laborers often report a gradual onset of ache that becomes sharply exacerbated during peak performance phases. Early intervention through biomechanical analysis, load management, and sport-specific conditioning can prevent progression to full-thickness strains or chronic joint inflammation.
When Back Rib Ache Signals an Internal Issue (Visceral Referred Pain)
Sometimes, pain felt in the back is "referred" from an internal organ. The brain misinterprets the pain signal's origin because nerves from the organ and the back area share common pathways. This visceral pain is often unrelated to movement and may be accompanied by other systemic symptoms. Unlike musculoskeletal pain, which is typically reproducible with palpation or positional changes, visceral pain often presents as a deep, diffuse, and poorly localized ache that may be accompanied by nausea, diaphoresis, or changes in vital signs. Understanding the neuroanatomical basis of referred pain—convergence-projection theory—is key to recognizing when a symptom warrants urgent systemic evaluation rather than localized orthopedic care.
Lung-Related Conditions
- Pleurisy: Inflammation of the pleura, the lining around the lungs, causes sharp chest and back pain that worsens with breathing.
- Pulmonary Embolism (PE): This is a medical emergency where a blood clot (usually from the leg) travels to the lungs. It causes sudden, sharp chest or back pain, severe shortness of breath, a rapid heart rate, and may involve coughing up blood.
- Lung Cancer: In some cases, lung cancer can cause persistent pain in the chest, shoulders, or back.
Additional pulmonary considerations include pneumonia, which can cause localized pleuritic pain alongside fever, productive cough, and auscultatory crackles, and pneumothorax, where air leaks into the pleural space causing sudden unilateral chest/back pain and progressive dyspnea. Chronic obstructive pulmonary disease (COPD) exacerbations can also lead to secondary musculoskeletal strain due to increased work of breathing and accessory muscle recruitment, creating a hybrid presentation of visceral and mechanical rib ache. Pulmonary function testing and chest imaging are standard tools to differentiate these conditions from purely somatic sources.
Kidney and Gallbladder Problems
- Kidneys: Located just below the rib cage on either side of the spine, the kidneys can cause significant back and flank pain if you have kidney stones or an infection.
- Gallbladder: Gallstones or gallbladder inflammation can cause intense pain in the upper right abdomen that often radiates to the back and between the shoulder blades, particularly after eating a fatty meal.
Renal colic from nephrolithiasis typically presents as waves of excruciating, colicky flank pain that may radiate to the groin, often accompanied by hematuria, nausea, and restlessness. Pyelonephritis, a bacterial kidney infection, adds systemic signs like high fever, chills, costovertebral angle (CVA) tenderness, and dysuria. Biliary pathology, including cholecystitis or choledocholithiasis, frequently triggers referred pain via the phrenic nerve and shared splanchnic nerve pathways, manifesting as right upper quadrant discomfort that migrates to the right scapular region or mid-back. Hepatic conditions such as hepatitis or liver congestion can similarly cause right-sided capsular stretching that refers pain posteriorly. Differentiation relies on urinalysis, liver function panels, abdominal ultrasound, and clinical provocation tests like Murphy's sign for gallbladder assessment.
Other Conditions
- Shingles (Herpes Zoster): This viral infection causes a painful, blistering rash that often wraps around one side of your torso along a nerve path, which can feel like severe back rib pain even before the rash appears.
- Fibromyalgia: A chronic condition characterized by widespread musculoskeletal pain, fatigue, and tender points, which can include the rib cage.
- Osteoporosis: This condition weakens bones, making ribs more susceptible to fractures from minor events like a strong cough.
Gastroesophageal reflux disease (GERD) and peptic ulcers can occasionally refer pain to the mid-back, particularly when symptoms worsen after meals or when lying supine. Cardiac conditions, including angina pectoris, myocardial infarction, and pericarditis, may present with atypical back or interscapular pain, particularly in women, diabetics, and older adults. While not strictly "rib" pathology, diaphragmatic irritation from intra-abdominal inflammation or endometriosis can also generate upper back discomfort. Gynecological conditions like ovarian cysts or ectopic pregnancy typically refer to the pelvis, but severe cases or diaphragmatic involvement can cause shoulder tip or mid-back pain due to phrenic nerve stimulation. A thorough systemic review is always indicated when the pain lacks clear mechanical triggers or is accompanied by constitutional symptoms.
When to Seek Medical Attention for Back Rib Pain
While many cases of back rib ache resolve with self-care, it's crucial to recognize the signs that warrant a professional evaluation. The transition from benign, self-limiting discomfort to a condition requiring medical intervention is often marked by changes in pain intensity, functional limitation, or the emergence of systemic indicators. Early recognition of red flags can prevent complications, especially in cases involving neurovascular compromise, infection, or acute cardiopulmonary events.
See a Doctor If...
- The pain is severe, doesn't improve after a few days of home care, or is getting worse.
- The pain resulted from a significant trauma or fall.
- The pain is limiting your ability to take a deep breath.
- You have other symptoms like a fever or unexplained weight loss.
- You notice swelling, redness, or warmth localized to a specific rib or back area, suggesting infection or inflammatory arthritis.
- You experience numbness, tingling, or weakness in your torso, arms, or legs, which may indicate nerve root compression or spinal cord involvement.
Go to the Emergency Room Immediately If... (Red Flags)
According to multiple sources including the Physiopedia list of red flags, you should seek immediate emergency care if your back rib ache is accompanied by any of the following:
- Difficulty breathing or severe shortness of breath
- Chest pain, pressure, or tightness
- Coughing up blood
- High fever and chills
- Pain radiating to your arm or jaw
- Dizziness, lightheadedness, or rapid heart rate
- Yellowing of the skin or eyes (jaundice)
- New onset of pain if you are under 20 or over 50, or have a history of cancer or drug abuse.
- Sudden loss of bowel or bladder control, or saddle anesthesia, which may indicate cauda equina syndrome or severe thoracic myelopathy (though rare, it requires emergent decompression).
- Traumatic injury with suspected open fracture, paradoxical chest wall movement (flail chest), or signs of internal bleeding such as hypotension or tachycardia.
Prompt emergency intervention for these indicators is non-negotiable. Delaying care in the setting of a pulmonary embolism, acute coronary syndrome, or septic infection can lead to irreversible organ damage or fatality. Always err on the side of caution and utilize emergency medical services when systemic distress accompanies localized back-rib discomfort.
How Back of Ribs Ache is Diagnosed
To determine the cause of your pain, a doctor will follow a structured diagnostic pathway. Clinical diagnosis begins with a meticulous patient interview, followed by targeted physical examination maneuvers designed to isolate musculoskeletal, neurological, or visceral contributors. The goal is to systematically rule out life-threatening conditions before focusing on rehabilitative or localized treatment strategies.
- Medical History and Physical Exam: Your doctor will ask detailed questions about your pain (onset, location, character) and any recent injuries or activities. They will perform a physical exam, pressing on your back and ribs to check for tenderness and assessing your range of motion. Orthopedic tests such as the seated flexion test, rib spring test, and thoracic rotation assessment help pinpoint joint restrictions. Neurological screening evaluates dermatomal sensation, myotomal strength, and deep tendon reflexes to rule out radiculopathy. Visceral auscultation and abdominal palpation assess for referred pain patterns, hepatosplenomegaly, or CVA tenderness.
- Imaging and Tests: Depending on the initial findings, one or more tests may be ordered:
- X-ray: To check for rib fractures or obvious issues with the spine.
- CT Scan or MRI: To get detailed images of bones (CT) or soft tissues like muscles, ligaments, and discs (MRI).
- Ultrasound: To evaluate muscle, tendon, and ligament injuries.
- Blood Tests: To look for signs of infection, inflammation, or issues with internal organs.
Advanced diagnostic tools may include electrocardiography (ECG/EKG) and troponin panels to exclude cardiac ischemia, D-dimer testing and CT pulmonary angiography to rule out pulmonary embolism, and urinalysis with culture for suspected renal pathology. Diagnostic nerve blocks or facet joint injections can serve both therapeutic and diagnostic purposes; significant pain relief following an anesthetic injection confirms the targeted structure as the pain generator. In complex or refractory cases, electromyography (EMG) and nerve conduction studies (NCS) may be utilized to evaluate intercostal nerve entrapment or thoracic radiculopathy. Multidisciplinary collaboration between primary care physicians, orthopedists, pulmonologists, gastroenterologists, and physical therapists often yields the most accurate diagnosis, particularly when pain presentation overlaps multiple physiological systems.
Finding Relief: Treatment and Home Care Strategies
Treatment depends entirely on the diagnosis. A musculoskeletal issue will be managed very differently than a kidney stone. The overarching principle of effective management is to address both symptom relief and underlying pathology. Early, targeted intervention significantly reduces the risk of chronic pain syndromes, compensatory movement disorders, and prolonged disability.
At-Home Management for Minor Aches
For pain you suspect is from a minor muscle strain or poor posture:
- Rest: Avoid activities that aggravate the pain for a few days.
- Ice: Apply an ice pack wrapped in a towel for 15-20 minutes several times a day for the first 48 hours to reduce inflammation.
- Pain Relievers: Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen (Advil, Motrin) or naproxen (Aleve) can help.
- Gentle Movement: After the initial acute phase, gentle stretching can prevent stiffness. Focus on posture correction exercises.
- Avoid Compression: Do not wrap your chest tightly with bandages. The NHS advises this can restrict deep breathing and increase the risk of pneumonia.
- Breathing Exercises: Practice diaphragmatic breathing to retrain respiratory mechanics. Shallow, chest-dominant breathing perpetuates intercostal spasm and thoracic stiffness. Lie supine with knees bent, place one hand on your chest and the other on your abdomen, and focus on expanding the belly on inhalation while keeping the chest relatively still. This reduces strain on accessory muscles and promotes parasympathetic nervous system activation, aiding tissue recovery.
- Topical Analgesics: Menthol, camphor, or NSAID-based creams/gels can provide localized relief without systemic side effects, particularly useful for superficial muscle strains or fascial restrictions.
Medical Treatments
If home care isn't enough, your doctor may recommend:
- Physical Therapy: To strengthen core and back muscles, improve posture, and increase flexibility.
- Prescription Medications: Stronger pain relievers or muscle relaxants may be prescribed.
- Injections: Corticosteroid injections can reduce inflammation in a specific joint. Regenerative options like platelet-rich plasma (PRP) are also used for some injuries.
- Treating the Underlying Cause: This could involve antibiotics for an infection, blood thinners for a pulmonary embolism, or procedures to address gallstones or kidney stones.
- Multimodal Pain Management: For chronic presentations, clinicians may incorporate neuromodulating medications (e.g., gabapentin, pregabalin), cognitive behavioral therapy (CBT) for pain coping, and transcutaneous electrical nerve stimulation (TENS) to interrupt nociceptive signaling pathways.
- Manual Therapy: Osteopathic manipulative treatment (OMT), chiropractic adjustments, and myofascial release techniques performed by licensed practitioners can restore joint arthrokinematics, break fascial adhesions, and improve thoracic spine mobility. These interventions are most effective when combined with active rehabilitation and home exercise programs.
Prevention and Long-Term Rib Health Optimization
Preventing recurrent back rib ache requires a proactive, lifestyle-integrated approach. The thoracic region is highly susceptible to degenerative changes and mechanical overload, but consistent preventive habits can preserve joint integrity and muscular resilience.
Ergonomic optimization is foundational. Workstations should support neutral spinal alignment: screens at eye level, elbows supported at 90 degrees, feet flat on the floor, and lumbar/thoracic supports maintaining natural curves. Frequent movement breaks every 30–45 minutes prevent static muscle loading and fascial creep. Incorporating mobility drills such as cat-cow stretches, thread-the-needle rotations, and foam rolling for the thoracic extensors helps maintain intervertebral disc hydration and facet joint lubrication.
Nutritional support plays an underappreciated role in musculoskeletal health. Adequate protein intake supports muscle repair, while calcium and vitamin D3 are critical for bone density maintenance, particularly in perimenopausal and older populations. Omega-3 fatty acids and polyphenol-rich foods exert natural anti-inflammatory effects that may reduce chronic musculoskeletal pain. Hydration is equally vital, as intervertebral discs and connective tissues require adequate fluid balance to withstand compressive forces.
Stress management directly influences pain perception and muscle tone. Chronic psychological stress elevates cortisol and adrenaline, leading to sustained sympathetic nervous system activation. This results in global muscle guarding, particularly in the paraspinals, trapezius, and intercostals. Mindfulness practices, progressive muscle relaxation, yoga, and adequate sleep hygiene (7–9 hours nightly) downregulate central sensitization and improve tissue recovery capacity. Addressing the psychosocial dimensions of pain is essential for breaking the cycle of chronicity and achieving sustainable relief.
Special Considerations for Athletes and Pregnant Individuals
Certain populations face unique risk profiles and management considerations for back rib discomfort. High-performance athletes, particularly those involved in throwing sports, rowing, golf, and swimming, subject the thoracic cage to extreme rotational and compressive loads. Periodization of training, emphasis on rotator cuff and scapular stabilizer conditioning, and pre-participation screening for thoracic mobility deficits are essential to prevent overuse injuries. Postural screening and breathing mechanics optimization should be integrated into off-season programming.
Pregnant individuals experience profound biomechanical and hormonal shifts that predispose them to rib and back pain. Relaxin and progesterone soften ligaments, while the expanding uterus elevates the diaphragm, altering rib cage kinematics and increasing intercostal strain. Later-stage pregnancy often causes costal margin flaring and diaphragmatic pressure, leading to lateral or posterior rib ache. Management includes pelvic floor and core stabilization exercises, maternity support belts, modified yoga or aquatic therapy, and positional adaptations (e.g., side-lying with pillow support, avoiding prolonged supine positioning after the first trimester). Any prenatal rib pain accompanied by right upper quadrant swelling, visual disturbances, or severe headaches warrants immediate obstetric evaluation to rule out preeclampsia or HELLP syndrome.
References
- Medical News Today - Back rib pain: Causes and treatment
- Centeno-Schultz Clinic - Back Pain in Ribs
- New Jersey Spine Specialists - NJSS Treats Patients For Various Degrees Of Back Rib Pain
- Mayo Clinic
- Physiopedia - Thoracic Back Pain Red Flags
- NHS - Broken or bruised ribs
Frequently Asked Questions
How long does it take for a strained intercostal muscle to heal?
Mild to moderate intercostal muscle strains typically heal within 3 to 6 weeks with appropriate rest, ice, and gentle mobility work. Severe tears or complete avulsions may require 8 to 12 weeks or longer. Healing timelines depend on injury severity, age, baseline fitness, nutrition, and adherence to rehabilitation protocols. Returning to heavy lifting or high-impact activities before full tissue remodeling is complete significantly increases the risk of chronic strain or recurrent injury.
Can poor posture really cause rib pain in the mid-back?
Yes, prolonged poor posture is one of the most common culprits behind chronic back rib ache. Slouched sitting, forward head posture, and rounded shoulders place excessive tensile load on the posterior thoracic ligaments, facet joints, and intercostal musculature. Over time, this leads to adaptive shortening, fascial restrictions, and joint capsule inflammation. Correcting posture through targeted strengthening, ergonomic adjustments, and thoracic extension mobilization typically yields significant symptom relief within a few weeks of consistent practice.
What is the difference between musculoskeletal rib pain and visceral referred pain?
Musculoskeletal rib pain is typically localized, reproducible with palpation, and exacerbated by specific movements, deep breathing, or positional changes. Visceral referred pain, on the other hand, tends to be deeper, more diffuse, and less responsive to positional adjustments. It often presents with systemic symptoms such as fever, nausea, changes in bowel or urinary habits, or cardiovascular indicators. Visceral pain also lacks tenderness upon direct muscle palpation, though it may coincide with musculoskeletal guarding as a secondary response.
Are there specific stretches that help relieve back rib discomfort?
Yes, but stretching should only be initiated after the acute inflammatory phase subsides. Effective stretches include seated or standing thoracic rotations, open-book stretches lying on your side, child’s pose with lateral reach, and gentle intercostal expansion drills (inhaling deeply while laterally bending away from the painful side). It is crucial to avoid aggressive or ballistic stretching during acute injury. Pairing mobility work with strengthening of the deep stabilizers (multifidus, transverse abdominis, and serratus anterior) creates a balanced support system that prevents recurrence.
When should I consider seeing a specialist instead of a primary care doctor?
Primary care physicians are excellent for initial evaluation and management of uncomplicated cases. Referral to a specialist is warranted if pain persists beyond 4–6 weeks despite conservative treatment, if neurological symptoms (numbness, weakness, radiating pain) develop, if trauma caused suspected fractures or spinal injury, or if systemic red flags emerge. Orthopedic surgeons or spine specialists handle complex structural or disc-related issues, pulmonologists or cardiologists manage suspected organ pathology, and pain management specialists or physiatrists address chronic, refractory, or neuropathic pain syndromes requiring advanced interventions.
Conclusion
Back of the ribs ache is a multifaceted symptom that bridges musculoskeletal, neurological, and visceral systems. While most cases stem from manageable mechanical triggers like muscle strains, postural dysfunction, or joint irritation, the proximity to vital organs necessitates careful differentiation. Understanding the anatomical relationships, recognizing red flags, and pursuing timely, targeted diagnostics are essential steps toward accurate diagnosis and effective treatment. Conservative management emphasizing rest, controlled movement, physical therapy, and ergonomic optimization successfully resolves the majority of mechanical rib pain. When internal or systemic conditions are suspected, rapid medical evaluation prevents complications and ensures appropriate intervention. By integrating proactive lifestyle habits, stress management, and consistent mobility training, individuals can not only alleviate current discomfort but also build long-term thoracic resilience. Always consult a qualified healthcare professional for persistent, severe, or atypical pain to rule out serious pathology and establish a personalized recovery plan tailored to your specific needs.

About the author
Michael O'Connell, DO, is a board-certified emergency medicine physician working as an attending physician at a busy Level I Trauma Center in Philadelphia, Pennsylvania. He also serves as a clinical instructor for medical residents and is active in wilderness medicine.