Why Are My Gums Black? Causes, Treatments, and When to See a Dentist

Key points
- Sudden changes in the color, shape, or texture of your gums.
- A new black spot that appears suddenly.
- Pain, swelling, or bleeding accompanying the discoloration.
- Foul breath or a bad taste in your mouth that doesn't go away.
- Other symptoms throughout your body, such as fatigue or weight loss.
- Lesions that are raised, ulcerated, or bleed easily upon light probing.
Noticing your gums are black or have dark spots can be alarming. While healthy gums are typically thought of as coral pink, their color can vary widely, just like skin tones. For many, dark gums are a completely normal and harmless trait. However, a sudden change in gum color can sometimes signal an underlying health issue that needs attention. Understanding the complex interplay between genetics, systemic health, and environmental factors is essential for distinguishing normal anatomical variations from pathological conditions that require prompt clinical intervention.
This comprehensive guide will walk you through the various causes of black gums, helping you distinguish between benign pigmentation and signs of a potential medical condition. We'll cover everything from natural variations and lifestyle factors to specific diseases and available treatments. Additionally, we will explore diagnostic protocols, preventive strategies, and what to expect during a professional dental evaluation to ensure you are fully informed and empowered to maintain optimal oral health.
Why Are My Gums Black? Harmless vs. Concerning Causes
The reasons for black gums fall into two main categories: benign (harmless) pigmentation that doesn't require medical treatment, and pathological (disease-related) discoloration that does. Dental professionals evaluate gum discoloration by considering its onset, distribution, symmetry, texture, and accompanying clinical signs. Benign pigmentation tends to be stable, bilateral, and asymptomatic, whereas concerning lesions often appear asymmetrically, change rapidly, or present with ulceration, bleeding, or systemic symptoms.
Harmless and Benign Causes of Black Gums
In most cases, dark gums are not a sign of poor health. Here are the most common benign causes, each rooted in distinct physiological or environmental mechanisms.
Natural Melanin Pigmentation
Just as melanin determines the color of our skin and hair, it also influences the color of our gums. Individuals with more melanin, particularly those of African, Asian, and Hispanic descent, often have naturally dark brown or black gums. This is known as physiological pigmentation and is a normal genetic trait. If your gums have always been dark, there's no reason to worry.
The melanin is produced by melanocytes located in the basal layer of the oral epithelium. Unlike skin melanocytes, which respond dynamically to ultraviolet radiation, gingival melanocytes maintain a relatively stable level of melanin production throughout adulthood. The distribution and density of these cells are primarily governed by genetic polymorphisms, particularly in the MC1R gene. Consequently, gum pigmentation is often symmetrical, affecting both the maxillary and mandibular arches, with the anterior gingiva typically showing more pronounced coloration due to higher epithelial turnover and keratinization patterns.
The primary concern with naturally dark gums is that the pigmentation can sometimes make it harder to spot the early signs of gum disease, like redness and inflammation. This makes regular dental check-ups especially important. Dentists and periodontists rely on supplementary diagnostic tools such as probing depth measurements, bleeding indices, and radiographic imaging to assess tissue health when visual erythema is masked by heavy melanin deposition.
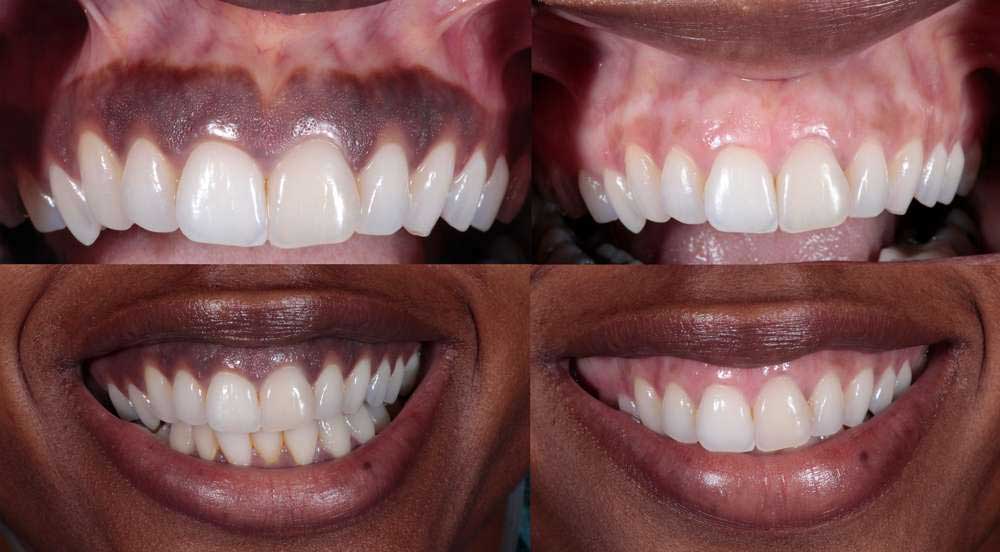 Image Source: CENTER for Advanced Periodontal & Implant Therapy
Image Source: CENTER for Advanced Periodontal & Implant Therapy
Smoker's Melanosis
Smoking and tobacco use can cause a condition called smoker's melanosis. Nicotine stimulates the body's pigment-producing cells (melanocytes) to create more melanin, leading to brown or black patches on the gums and the inside of the cheeks. This discoloration is directly linked to how much and how long a person has smoked. The chemical compounds in tobacco smoke, particularly polycyclic aromatic hydrocarbons, act as direct stimulants to melanogenesis while simultaneously inducing mild chronic inflammation in the gingival epithelium. The condition typically presents on the labial (front-facing) aspect of the anterior gingiva and can spread to the buccal mucosa and palate in heavy users. The good news is that these patches are benign and often fade or disappear completely within a few months to years after quitting smoking. The reversal timeline depends on the duration of tobacco exposure, baseline melanocyte activity, and individual metabolic clearance rates. Vaping and smokeless tobacco products can also contribute to localized mucosal discoloration, though the pathophysiology may differ slightly due to the absence of combustion byproducts.
Medication Side Effects
Certain medications are known to cause hyperpigmentation in the mouth. The antibiotic minocycline, often used to treat acne, is a common culprit. Minocycline-induced pigmentation occurs through the formation of insoluble iron-drug complexes that deposit in the connective tissue and epithelium, producing blue, gray, or black discoloration. Other drugs that can cause dark spots on the gums include some antimalarials, antipsychotics, chemotherapy agents, anticonvulsants, and medications used in cancer therapy. Heavy metal exposure from medications or occupational hazards can similarly lead to linear gingival pigmentation along the gumline. If you notice a change in your gum color after starting a new medication, discuss it with your doctor. Never discontinue prescribed therapy without medical supervision, as many drug-induced pigmentations resolve slowly after dose adjustment or alternative prescribing, and the systemic benefits of the medication typically outweigh cosmetic oral side effects.
Amalgam Tattoos
An amalgam tattoo is a small, flat, blue, gray, or black spot on the gums. It occurs when particles from a silver-colored (amalgam) dental filling accidentally get embedded in the soft tissue of your mouth during a dental procedure. This iatrogenic phenomenon is one of the most common localized oral pigmentations. The metallic particles become trapped within the lamina propria, where they remain inert but visible through the overlying mucosa. These "tattoos" are completely harmless and don't require removal unless for cosmetic reasons or if there's uncertainty in the diagnosis. Unlike melanocytic lesions, amalgam tattoos do not blanch under pressure and typically maintain their size and shape indefinitely. Radiographic imaging often reveals tiny metallic densities, providing a definitive non-invasive diagnostic confirmation.
Medical Conditions and Concerning Causes of Black Gums
While less common, a change in gum color can be a symptom of a health problem. It's crucial to see a dentist or doctor if you notice sudden darkening, especially if accompanied by other symptoms. Pathological pigmentation often requires interdisciplinary evaluation, involving dental specialists, dermatologists, endocrinologists, or oncologists to establish a definitive diagnosis and initiate appropriate management.
Acute Necrotizing Ulcerative Gingivitis (ANUG)
Also known as "trench mouth," ANUG is a severe and painful gum infection. It results from a rapid overgrowth of bacteria, often linked to stress, poor sleep, smoking, immunosuppression, and poor oral hygiene. The condition is characterized by a polymicrobial infection predominantly involving spirochetes like Treponema denticola and fusobacteria such as Fusobacterium nucleatum. These anaerobic organisms produce toxins that destroy interdental papillae, leading to tissue necrosis. ANUG can cause a layer of dead tissue to build up on the gums, which appears gray or black. Other symptoms include severe gum pain, fever, foul breath, and bleeding. The black or gray pseudomembrane consists of necrotic tissue, fibrin, leukocytes, and bacterial colonies. This condition requires immediate dental treatment, which usually involves a thorough debridement, oxygenating rinses like hydrogen peroxide, and a course of antibiotics such as metronidazole or amoxicillin. Without prompt intervention, the necrosis can progress to necrotizing periodontitis, resulting in permanent bone loss and tooth mobility.
Addison's Disease
Addison's disease is a rare disorder affecting the adrenal glands, which don't produce enough essential hormones like cortisol and aldosterone. The pathophysiology of oral hyperpigmentation in Addison's stems from a loss of negative feedback on the pituitary gland. Low cortisol levels trigger excessive secretion of adrenocorticotropic hormone (ACTH), which shares a common precursor (pro-opiomelanocortin) with melanocyte-stimulating hormone (MSH). Elevated MSH levels directly stimulate gingival melanocytes, causing diffuse or patchy hyperpigmentation. One of the tell-tale symptoms is hyperpigmentation, causing dark, blotchy patches on the gums and lips, as well as on the skin (often on knees, knuckles, and palm creases). The pigmentation is usually generalized but can be notably more pronounced in areas subject to friction or minor trauma. Other symptoms include fatigue, muscle weakness, weight loss, and low blood pressure. If black gums are accompanied by these symptoms, it's vital to see a medical doctor. Diagnosis typically involves morning serum cortisol, ACTH levels, and an ACTH stimulation test, followed by lifelong glucocorticoid and mineralocorticoid replacement therapy.
Peutz-Jeghers Syndrome
This is a rare, inherited genetic condition that causes non-cancerous polyps to grow in the gastrointestinal tract and increases the risk for certain types of cancer. It follows an autosomal dominant inheritance pattern and is primarily caused by mutations in the STK11/LKB1 tumor suppressor gene. The syndrome disrupts normal cellular signaling pathways, leading to abnormal melanocyte migration during embryonic development and subsequent polyp formation. A key early sign is the appearance of dark blue or dark brown freckle-like spots on the mouth, lips, gums, and on the skin of the fingers and toes. Unlike physiological pigmentation, these macules are often sharply demarcated and may appear clustered around the vermilion border. These spots typically develop in childhood and may fade in adulthood, but the underlying genetic predisposition requires lifelong surveillance. Dental professionals play a critical role in early recognition, often prompting referrals for genetic counseling, upper and lower endoscopy, and oncological screening protocols starting in early adolescence.
Oral Malignant Melanoma
In very rare instances, a new or changing black spot on the gums can be a sign of oral malignant melanoma, a type of oral cancer. It accounts for a very small percentage of all oral cancers (less than 1%) but carries a disproportionately poor prognosis due to early local invasion and distant metastasis. The maxillary anterior gingiva and hard palate are the most common sites. Clinicians evaluate suspicious lesions using the oral adaptation of the ABCDE criteria: Asymmetry, Border irregularity, Color variegation, Diameter greater than 6mm, and Evolution over time. Because of its aggressive nature, any new, irregularly shaped, or changing pigmented lesion in the mouth should be evaluated by a dentist or specialist immediately, who may perform a biopsy to rule out cancer. An incisional or excisional biopsy with histopathological analysis and immunohistochemical staining for markers like S-100, HMB-45, and Melan-A is essential for definitive diagnosis. Treatment requires a multidisciplinary approach, often combining wide surgical excision with adjuvant radiotherapy, targeted immunotherapy, or systemic chemotherapy.
At-a-Glance: Distinguishing Benign from Pathological Discoloration
This table provides a quick summary to help differentiate the potential causes of black gums.
| Condition | Cause | Clinical Appearance | Treatment Focus |
|---|---|---|---|
| Benign Causes | |||
| Physiological Pigmentation | Increased melanin | Uniform brown to black patches, present long-term | None required; cosmetic options available |
| Smoker's Melanosis | Nicotine stimulation | Diffuse brown to black patches | Smoking cessation |
| Drug-Induced Pigmentation | Medications (e.g., minocycline) | Brown, black, or blue-gray discoloration | Discontinuation of medication (consult doctor) |
| Amalgam Tattoo | Amalgam filling particles in tissue | Single blue, gray, or black spot | None required |
| Concerning Causes | |||
| Addison's Disease | Adrenal insufficiency | Dark patches on gums, lips, and skin | Hormone replacement therapy |
| Peutz-Jeghers Syndrome | Genetic disorder | Dark blue or brown freckle-like spots | Monitoring for polyps and cancer |
| Oral Malignant Melanoma | Malignant melanocytes | New or changing pigmented lesion, irregular borders | Surgical excision, other cancer therapies |
| ANUG (Trench Mouth) | Bacterial infection | Gray or black layer of dead tissue on gums, pain, fever | Antibiotics, professional dental cleaning |
When to See a Doctor or Dentist
If your gums have always been dark, it's likely normal. However, you should schedule an appointment with your dentist if you notice:
- Sudden changes in the color, shape, or texture of your gums.
- A new black spot that appears suddenly.
- Pain, swelling, or bleeding accompanying the discoloration.
- Foul breath or a bad taste in your mouth that doesn't go away.
- Other symptoms throughout your body, such as fatigue or weight loss.
- Lesions that are raised, ulcerated, or bleed easily upon light probing.
- Rapid enlargement or changes in surface architecture over a period of weeks.
Early diagnosis is key to effectively treating any underlying condition. During your appointment, your dentist will conduct a thorough extraoral and intraoral examination, review your medical and medication history, and assess your oral hygiene practices. If a lesion appears suspicious, they may recommend diagnostic imaging such as periapical radiographs or a soft tissue biopsy to examine the cellular architecture under a microscope. In cases where systemic disease is suspected, blood work or referrals to specialists may be necessary. Keeping a photographic record of any spots over time can also be incredibly helpful for your clinician to track progression or stability between visits.
Treatments for Black Gums
Treatment depends entirely on the underlying cause. If a medical condition like Addison's disease or ANUG is diagnosed, treating that condition is the first and most important step. Resolving the primary pathology often leads to gradual normalization or stabilization of the gum pigmentation. Addressing systemic issues, correcting nutritional deficiencies, and optimizing immune function form the foundation of any comprehensive treatment plan for pathological gingival discoloration.
For discoloration caused by lifestyle factors or for those seeking to lighten naturally dark gums for cosmetic reasons, several options are available. Cosmetic gingival depigmentation is an elective procedure and should only be considered after a clinician has thoroughly ruled out malignancy, inflammation, and systemic disease. Patient expectations, healing capacity, and financial considerations are all carefully weighed during the consultation process.
Lifestyle Changes and Home Care
- Quit Smoking: This is the most effective way to reverse smoker's melanosis. Utilizing nicotine replacement therapy, behavioral counseling, and prescription cessation medications can significantly improve success rates and accelerate mucosal healing.
- Practice Excellent Oral Hygiene: Brush twice a day, floss daily, and use an antiseptic mouthwash to prevent plaque buildup and infections like ANUG. Soft-bristled toothbrushes are recommended to prevent trauma that can exacerbate inflammation in heavily pigmented tissues.
- Maintain a Healthy Diet: A balanced diet rich in vitamins (particularly C, D, and B-complex), minerals, and antioxidants helps support gum health and tissue regeneration. Staying well-hydrated also maintains optimal salivary flow, which naturally cleanses the gingival sulcus.
- Manage Stress and Sleep: Chronic stress and sleep deprivation impair immune function and are significant triggers for conditions like ANUG. Incorporating mindfulness practices, adequate sleep hygiene, and regular physical activity can bolster both systemic and oral health.
While some home remedies like oil pulling or using green tea rinses are promoted online, their effectiveness in lightening gums is not scientifically proven. Always consult your dentist before trying any home treatments, as unregulated compounds or aggressive scrubbing can cause epithelial abrasion, chemical burns, or delayed wound healing that may inadvertently trigger reactive hyperpigmentation during the repair process.
Professional Cosmetic Treatments
After a dentist has confirmed that your dark gums are benign, you can explore cosmetic procedures to lighten them:
- Laser Gum Depigmentation: Also known as gum bleaching, this procedure uses a specialized dental laser to vaporize and remove the thin top layer of pigmented gum tissue, revealing the lighter pink tissue underneath. Modern practices frequently utilize erbium:YAG, diode, or CO2 lasers, which offer precise ablation with minimal bleeding and reduced postoperative discomfort. Local anesthesia ensures a painless experience, and the results are often long-lasting, though some repigmentation can occur over several years due to natural melanocyte activity.
- Surgical Gingivectomy: A periodontist can surgically remove the pigmented gum tissue with a scalpel or electrosurge unit. As the area heals, new, lighter-colored tissue forms. This traditional method allows for complete histological examination of the excised tissue, providing an extra layer of diagnostic safety, though it typically requires suturing and a slightly longer recovery period compared to laser techniques.
- Cryosurgery: This method involves freezing the pigmented areas to destroy the melanin-producing cells. Liquid nitrogen is applied via a specialized probe, causing controlled cellular necrosis. As the tissue sloughs off and regenerates, melanocyte density is reduced. Cryotherapy is less commonly used today due to less predictable tissue control and a higher risk of postoperative swelling, but it remains a viable option in specific clinical scenarios.
Recovery from any depigmentation procedure generally takes 7 to 14 days. Patients are advised to consume soft, lukewarm foods, avoid spicy or acidic substances, and maintain a gentle oral hygiene routine prescribed by their periodontist. Follow-up appointments are crucial to monitor epithelialization and ensure optimal aesthetic outcomes.
Black Gums in Children and Animals
Gum discoloration isn't limited to human adults. It's a phenomenon seen across different age groups and even in the animal kingdom. Understanding these variations helps parents and pet owners distinguish normal developmental stages from conditions requiring professional care.
- Black Gums in Kids: Dark spots on a child's gums can be alarming, but they are often harmless. They can be due to natural pigmentation appearing as they grow, which typically becomes more pronounced around age 10 to 12 and stabilizes by late adolescence. Another common cause is an eruption hematoma, which is a bluish-black blood blister that forms when a new tooth is about to break through the gums. It occurs due to minor trauma to the capillary network overlying the erupting crown and usually resolves on its own once the tooth pierces the mucosa. Maintaining routine pediatric dental visits ensures proper tracking of dental arch development and early intervention if cystic formations impede normal eruption.
- Black Spots on Cats' Gums (Lentigo): Orange, calico, and tortoiseshell cats often develop small, flat black spots on their lips, gums, and nose as they age. This harmless genetic condition is called lentigo and is the feline equivalent of freckles. It results from increased melanocyte activity in the epidermis and oral mucosa, unrelated to malignancy. Veterinarians recommend documenting the spots during annual exams to monitor for any changes in texture or rapid proliferation, which could indicate squamous cell carcinoma or melanocytic tumors, though these are exceedingly rare compared to benign lentigo.
- Fun Fact: Black Gums in the Animal Kingdom: Humans aren't the only ones! Several animals have black gums. For example, the Chinook salmon is known for its distinctive dark mouth and black gums, which helps distinguish it from other salmon species. In the wild, mucosal and gingival pigmentation often serves protective functions, such as shielding underlying tissues from intense ultraviolet radiation at high altitudes or shallow waters, providing camouflage, or enhancing tissue resilience against abrasive diets and environmental stressors. Many domestic dog breeds, including the Chow Chow, Shar-Pei, and Akitas, also exhibit naturally pigmented oral mucosa, which is considered a breed standard trait and a sign of genetic diversity.
Conclusion
Black gums are often a normal, healthy variation of human pigmentation. However, because they can occasionally signal a serious health concern, you should never ignore a sudden change in their color. By understanding the potential causes and knowing when to seek professional advice, you can ensure your gums—and your overall health—stay in top condition. The mouth serves as a highly visible window to systemic wellness, making regular observation of gingival color, contour, and consistency an essential component of holistic healthcare.
Proactive oral care, routine professional cleanings, and prompt evaluation of atypical lesions form the cornerstone of long-term periodontal health. Whether your dark gums are a lifelong genetic hallmark or a transient response to lifestyle factors, maintaining a strong partnership with your dental and medical providers will guarantee accurate monitoring, timely intervention when necessary, and ultimately, peace of mind. Regular dental visits are your best defense for early detection and peace of mind.
Frequently Asked Questions
Can black gums be reversed naturally?
In most cases, naturally occurring physiological melanin pigmentation cannot be permanently reversed through diet or natural remedies alone, as it is genetically determined. However, gum discoloration caused by smoking often fades gradually over several months to a year after complete tobacco cessation. Maintaining rigorous oral hygiene, consuming antioxidant-rich foods, and staying hydrated can support overall mucosal health, but significant cosmetic lightening typically requires professional dental procedures like laser therapy. Always consult a dentist before attempting aggressive natural remedies, which may irritate delicate oral tissues.
Is laser gum depigmentation a painful procedure?
No, laser gum depigmentation is generally not painful when performed correctly. Dentists administer local anesthesia to numb the treatment area completely before beginning the procedure. Patients typically report feeling mild pressure or vibration rather than pain during the session. Postoperatively, some minor discomfort, swelling, or sensitivity is normal for a few days, but this is easily managed with over-the-counter analgesics, cold compresses, and a prescribed antimicrobial rinse. Most individuals return to their normal dietary and social routines within 24 to 48 hours.
How long does it take for smoker's melanosis to disappear after quitting?
The timeline for smoker's melanosis to resolve varies significantly depending on the duration and intensity of tobacco use, individual metabolic rates, and baseline melanin production. Generally, patients begin to notice a gradual lightening of the gingiva within 3 to 6 months after quitting completely. Significant fading often occurs between 1 to 3 years, though some individuals may retain mild residual pigmentation. The oral mucosa undergoes continuous cellular turnover, and removing the continuous chemical stimulus allows melanocytes to gradually return to their baseline activity levels.
Should I be worried if only one side of my gums is dark?
Unilateral or highly asymmetric dark pigmentation warrants closer clinical evaluation. While physiological pigmentation is typically bilateral and symmetrical, isolated dark spots or patches can indicate localized conditions such as an amalgam tattoo, a benign melanotic macule, or, less commonly, a focal pathological process like oral melanoma. Any unilateral lesion that is new, growing, irregular in border, or associated with texture changes, bleeding, or discomfort should be examined promptly by a dental professional. Early biopsy and histopathological assessment are the gold standard for ruling out malignancy and establishing an accurate diagnosis.
Does having black gums increase my risk of gum disease?
Having naturally dark gums does not inherently increase your biological risk for developing periodontal disease. Gum disease is primarily driven by bacterial plaque accumulation, immune response, and genetic susceptibility, not by melanin levels. However, heavy pigmentation can sometimes mask the classic early warning sign of gingivitis: gingival erythema (redness). This visual masking makes clinical probing, bleeding indices, and regular professional cleanings even more critical for individuals with naturally dark gingiva, as inflammation may be present even when not immediately obvious to the naked eye.
References
- CENTER for Advanced Periodontal & Implant Therapy. (n.d.). Dark gums: 5 discoloration reasons and treatment. Retrieved from https://www.implantperiocenter.com/gums-dark-5-discoloration-reasons/
- Sissons, C. (2018). 7 causes of black gums. Medical News Today. Retrieved from https://www.medicalnewstoday.com/articles/321466
- Valeii, K. (2025). 8 Reasons for Black Gums and How to Treat Them. Verywell Health. Retrieved from https://www.verywellhealth.com/black-gums-5509450
- Colgate. (n.d.). What Causes Black Gums?. Retrieved from https://www.colgate.com/en-us/oral-health/adult-oral-care/what-causes-black-gums
- Fisheries and Oceans Canada. (2025). Identify your catch. Retrieved from https://www.pac.dfo-mpo.gc.ca/fm-gp/rec/identify-identifier-eng.html
- The Spruce Pets. (2025). What Are the Black Spots on My Orange Cat's Mouth & Nose?. Retrieved from https://www.thesprucepets.com/orange-tabby-black-spots-nose-lips-3384890

About the author
Benjamin Carter, MD, is a board-certified otolaryngologist specializing in head and neck surgery, with an expertise in treating throat cancer. He is an associate professor and the residency program director at a medical school in North Carolina.