Fuzzy or Blurred Vision in One Eye: Causes and When to Worry

Key points
- Sudden, severe headache (often described as the "worst headache of my life" or thunderclap in nature)
- Numbness or weakness on one side of your face or body
- Difficulty speaking or understanding speech
- Dizziness, confusion, or loss of balance
- A sudden increase in eye floaters or flashes of light
- The appearance of a dark curtain or shadow over your field of vision
Experiencing fuzzy or blurred vision in just one eye can be a disorienting and alarming event. While it's sometimes a sign of a common, correctable issue, it can also be a warning of a serious medical emergency. Understanding the potential causes and knowing when to seek immediate help is crucial for protecting both your eyesight and your overall health. The human visual system relies on a complex network of structures, including the cornea, lens, vitreous humor, retina, and optic nerve, all working in tandem to transmit clear images to the brain. When any component in one eye malfunctions or experiences trauma, the resulting asymmetry can be particularly noticeable and disruptive. Unilateral visual disturbances differ significantly from bilateral blurring, as they often point to localized ocular pathology, vascular compromise, or neurological issues affecting one side of the visual pathway.
This comprehensive guide synthesizes information from leading health authorities and ophthalmologists to help you understand the causes of unilateral blurred vision, differentiate between urgent and non-urgent situations, and know what to do next. Whether you are a patient experiencing symptoms for the first time, a caregiver supporting a loved one, or simply someone looking to safeguard your long-term ocular health, this resource will provide the evidence-based information you need to make informed decisions.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
When is Blurred Vision in One Eye an Emergency?
The most critical factor is the onset and accompanying symptoms. According to experts at Optometrists.org, sudden blurry vision can be a sign of a medical emergency. Time is of the essence when visual pathways are compromised. In vascular events like strokes or retinal artery occlusions, every minute without proper blood flow results in irreversible neuronal death. Similarly, pressure-related emergencies like acute angle-closure glaucoma can cause permanent optic nerve damage within hours. Recognizing the difference between a gradual, age-related decline and a sudden, alarming visual change is the first step in triaging your own health. If symptoms appeared abruptly, especially if they are painless yet severe, do not wait to see if they improve.
Seek immediate medical attention or call 911 if you experience blurred vision in one eye along with any of the following red flag symptoms:
- Sudden, severe headache (often described as the "worst headache of my life" or thunderclap in nature)
- Numbness or weakness on one side of your face or body
- Difficulty speaking or understanding speech
- Dizziness, confusion, or loss of balance
- A sudden increase in eye floaters or flashes of light
- The appearance of a dark curtain or shadow over your field of vision
- Severe eye pain
- Nausea and vomiting
- Seeing halos or rainbows around lights
These symptoms can indicate a life-threatening condition like a stroke or a sight-threatening one like retinal detachment or acute glaucoma. If you encounter any of these warning signs, avoid driving yourself to the hospital. Have a family member or friend accompany you, or use emergency medical services so paramedics can begin stabilization and documentation en route. While waiting for help, note the exact time the symptoms began, refrain from eating or drinking in case emergency procedures are required, and keep your head elevated if you suspect a pressure-related issue or retinal concern. Do not rub or apply pressure to the affected eye, as this can worsen certain conditions like corneal injuries or increase intraocular pressure.
Potential Emergency Causes of Unilateral Blurred Vision
If you have any of the red flag symptoms above, one of these serious conditions could be the cause. Prompt diagnosis and intervention are critical to preserving both vision and neurological function. Below is a detailed breakdown of these high-acuity conditions, including their underlying mechanisms, risk factors, and standard treatment pathways.
Stroke or TIA (Transient Ischemic Attack)
A stroke occurs when blood flow to the brain is blocked. As noted by Johns Hopkins Medicine, vision problems, including sudden blurred vision in one or both eyes, can be a primary sign. A TIA, or "mini-stroke," causes similar symptoms that are temporary but serves as a major warning sign for a future stroke. When a clot or plaque disrupts circulation to the occipital lobe or the retinal artery (amaurosis fugax), visual processing is immediately impaired. The retinal artery is a direct branch of the internal carotid artery, meaning retinal symptoms often mirror broader cerebrovascular issues. Risk factors include hypertension, atrial fibrillation, high cholesterol, smoking, obesity, and diabetes. Treatment for acute ischemic stroke may involve thrombolytic therapy (tPA) if administered within a strict time window, typically 3 to 4.5 hours from symptom onset. Endovascular thrombectomy may also be considered for large vessel occlusions. Post-acute management focuses heavily on secondary prevention, including antiplatelet therapy, statins, blood pressure management, and lifestyle modifications to drastically reduce the risk of recurrence.
Retinal Detachment
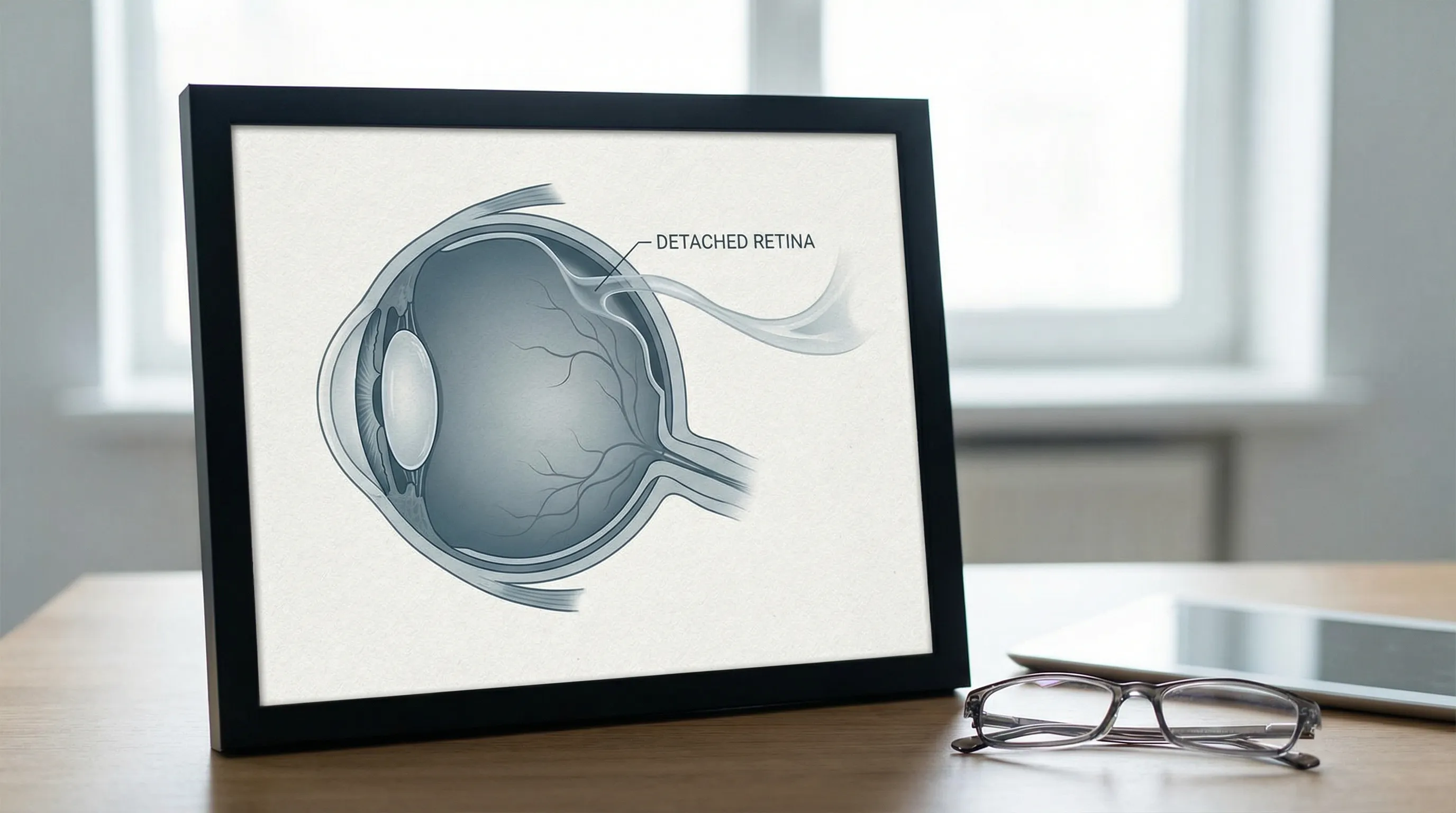
This is a medical emergency where the retina—the light-sensitive tissue at the back of the eye—pulls away from its normal position. According to The EyeDoctors Optometrists, this can cause sudden blurred vision, flashes of light, floaters, and a shadow in your peripheral vision. Without prompt treatment, it can lead to permanent vision loss. Retinal detachments are frequently preceded by a posterior vitreous detachment (PVD), a natural aging process where the gel-like vitreous shrinks and separates from the retinal surface. If the vitreous pulls too forcefully, it can tear the retina, allowing fluid to seep underneath and detach it. High myopia (nearsightedness), previous cataract surgery, significant eye trauma, and a family history of retinal detachments significantly increase susceptibility. Surgical repair methods include pneumatic retinopexy (injecting a gas bubble to push the retina back into place), scleral buckling (placing a silicone band around the eye to relieve traction), and vitrectomy (removing the vitreous gel and replacing it with a gas or silicone oil). Success rates are high when treated early, typically within 24 to 72 hours of symptom onset, though visual recovery depends on whether the macula was involved before surgery.
 :max_bytes(150000):strip_icc()/sudden-blurry-vision-5092267.FINAL-c7abefa2797241c89b08e9f4a6e0b82b.jpg)
Sudden vision changes can signal serious conditions like retinal detachment. Source: Mayo Clinic
:max_bytes(150000):strip_icc()/sudden-blurry-vision-5092267.FINAL-c7abefa2797241c89b08e9f4a6e0b82b.jpg)
Sudden vision changes can signal serious conditions like retinal detachment. Source: Mayo Clinic
Acute Angle-Closure Glaucoma
This rare but serious condition occurs when the fluid drainage channels in the eye become blocked, causing a rapid and painful spike in eye pressure. This can damage the optic nerve within hours. The eye continuously produces aqueous humor to maintain intraocular pressure (IOP). In healthy eyes, this fluid drains through the trabecular meshwork located in the angle where the iris meets the cornea. When the angle is anatomically narrow, pupil dilation (which can occur in dim lighting, stress, or after taking certain medications like antihistamines or decongestants) can cause the iris to block this drainage pathway entirely. IOP can skyrocket from a normal 12-21 mmHg to 50 mmHg or higher. This extreme pressure compromises blood flow to the optic nerve and can permanently destroy retinal ganglion cells. Immediate treatment involves emergency lowering of IOP using oral medications (like acetazolamide), intravenous agents, topical prostaglandins, beta-blockers, and alpha-agonists. Once the acute attack is controlled and the cornea clears, a laser peripheral iridotomy is typically performed to create a small drainage hole in the iris, bypassing the blockage and preventing recurrence.
Wet Macular Degeneration
While age-related macular degeneration (AMD) is often a slow process (the "dry" form), the "wet" form can cause sudden and severe vision loss. This happens when abnormal blood vessels leak fluid or blood into the macula, the part of the retina responsible for sharp, central vision. This neovascularization is driven by an overexpression of vascular endothelial growth factor (VEGF). The leaked fluid causes swelling and distortion (metamorphopsia), making straight lines appear wavy or bent. Wet AMD is considered an eye emergency requiring prompt treatment to preserve sight. The gold standard treatment involves regular intravitreal injections of anti-VEGF medications, such as ranibizumab, aflibercept, or faricimab. These injections inhibit abnormal blood vessel growth and reduce leakage. With consistent monitoring and timely treatment, many patients can stabilize their vision and maintain functional independence. Patients at high risk are encouraged to use an Amsler grid daily to monitor for early signs of macular distortion.
Common and Less Urgent Causes
More often, blurry vision in one eye is caused by a condition that, while requiring a doctor's attention, is not an immediate emergency. These conditions typically develop gradually or present with mild discomfort, but left unaddressed, they can still significantly impact quality of life, safety, and long-term ocular health.
Refractive Errors
The most common reason for blurred vision is a refractive error. This means the shape of your eye prevents light from focusing correctly on the retina. These include:
- Astigmatism: An imperfectly curved cornea or lens causes vision to be blurry at all distances. It's common for astigmatism to be different in each eye, a condition known as anisometropia. When the difference is significant, the brain may struggle to merge the two images, leading to eye strain, headaches, or even suppression of vision in the blurrier eye.
- Nearsightedness (Myopia): Distant objects appear blurry due to an elongated eyeball or overly curved cornea.
- Farsightedness (Hyperopia): Close-up objects appear blurry because the eye is too short or the focusing system is underpowered. Mild hyperopia in younger individuals may go unnoticed as the lens compensates through accommodation, but this constant muscular effort can lead to fatigue and intermittent blurring.
- Presbyopia: An age-related hardening of the lens that typically begins in the early 40s, making near vision increasingly difficult. These are easily corrected with eyeglasses, contact lenses, or refractive surgery (LASIK, PRK, SMILE). Regular comprehensive exams are essential, as uncorrected refractive errors in children can lead to amblyopia ("lazy eye"), where the brain permanently ignores the blurrier input.
Cataracts
A cataract is a clouding of the eye's natural lens, which is a very common part of aging. As detailed by ophthalmologist Eduardo Besser, MD, cataracts can develop at different rates in each eye, leading to one eye becoming significantly blurrier than the other. Symptoms include cloudy vision, glare, faded colors, double vision in a single eye, and difficulty seeing at night. Beyond aging, cataracts can be accelerated by prolonged UV exposure, smoking, chronic steroid use, ocular trauma, and poorly controlled diabetes. While early-stage cataracts can be managed with stronger eyeglass prescriptions, brighter lighting, and anti-glare coatings, surgery becomes necessary when visual impairment interferes with daily activities. Modern phacoemulsification cataract surgery is highly successful, using ultrasound waves to break up and remove the cloudy lens, which is then replaced with a clear, artificial intraocular lens (IOL). Advanced IOL options now allow patients to correct distance, intermediate, and near vision simultaneously.
Dry Eye Syndrome & Digital Eye Strain
When your eyes don't produce enough quality tears, the surface of the eye can become irritated and your vision can temporarily blur. Staring at digital screens for long periods reduces our blink rate by up to 60%, exacerbating dry eye and causing digital eye strain, which can also lead to fuzzy vision. The tear film consists of three layers: lipid (oil), aqueous (water), and mucin. Dysfunction in any layer disrupts ocular surface health. Meibomian gland dysfunction (MGD) is particularly common, where the oil-producing glands along the eyelids become clogged, leading to rapid tear evaporation. Symptoms include gritty sensation, redness, burning, fluctuating vision that improves with blinking, and excessive watering (a compensatory response to irritation). Management strategies include practicing the 20-20-20 rule (every 20 minutes, look at something 20 feet away for 20 seconds), using preservative-free artificial tears, applying warm compresses to melt meibomian gland oils, and considering prescription medications like cyclosporine or lifitegrast for chronic cases. Environmental adjustments, such as using a humidifier and avoiding direct air conditioning or heater vents blowing into the face, can also provide significant relief.
Eye Infections
Various infections can cause inflammation and blurry vision in one eye.
- Conjunctivitis (Pink Eye): Inflammation of the outer membrane of the eyeball. Bacterial conjunctivitis typically presents with thick yellow or green discharge that can crust the eyelids shut, while viral conjunctivitis often accompanies cold symptoms and features watery discharge. Allergic conjunctivitis, triggered by pollen, dust, or pet dander, causes intense itching and redness but is not contagious.
- Keratitis: Inflammation of the cornea, often linked to improper contact lens wear. Sleeping in lenses, swimming with them, or using tap water for cleaning can introduce pathogens like Acanthamoeba, which can cause severe, vision-threatening corneal damage.
- Uveitis: Inflammation of the uvea, the middle layer of the eye. It can be anterior, intermediate, or posterior, often associated with autoimmune diseases or systemic infections. Symptoms include deep eye ache, light sensitivity, and blurred vision. Treatment depends entirely on the etiology: bacterial infections require prescription antibiotic drops, viral cases are typically managed with cool compresses and time, while fungal or parasitic keratitis demands aggressive, specialized antimicrobial therapy. Strict hygiene, frequent handwashing, and proper contact lens disinfection are critical preventative measures.
Corneal Abrasion (Scratched Cornea)
A scratch on the clear front surface of the eye (the cornea) can be painful and cause light sensitivity and blurred vision. While minor scratches often heal, it's important to see a doctor to prevent infection. The corneal epithelium is rich in nerve endings, making even microscopic scratches incredibly painful. Common causes include fingernails, tree branches, makeup applicators, foreign debris, and poorly fitted contact lenses. Healing typically occurs within 24 to 72 hours, as the cornea has remarkable regenerative capacity. Treatment usually involves antibiotic ointment to prevent infection, cycloplegic drops to relieve ciliary muscle spasms, and oral pain relievers. Contrary to older practices, patching the eye is generally avoided unless specifically directed by a doctor, as it creates a warm, dark environment that can promote bacterial growth, particularly from Pseudomonas aeruginosa in contact lens wearers. Avoid rubbing the eye, and never attempt to remove embedded foreign objects yourself.
Retinal Migraine
A retinal migraine causes temporary episodes of visual disturbances, including blurred vision, twinkling lights, or even temporary blindness in one eye. According to the American Migraine Foundation, these symptoms typically last less than an hour and may occur before or during a headache. Unlike migraine with aura, which affects the visual cortex and impacts both eyes, retinal migraines are believed to stem from vasospasm or reduced blood flow specifically in the retinal or ophthalmic artery. Triggers can mirror traditional migraines: stress, certain foods (aged cheeses, processed meats, artificial sweeteners), hormonal fluctuations, bright lights, and dehydration. While typically benign, recurrent episodes warrant neurological and ophthalmological evaluation to rule out transient ischemic attacks or underlying vascular disorders. Management focuses on trigger avoidance, lifestyle stabilization, and in severe or frequent cases, preventive medications like calcium channel blockers or low-dose aspirin under medical supervision.
*Video: Dr. EyeGuy discusses five potential causes of sudden blurry vision in one eye. Source: [YouTube](https://www.youtube.com/watch?v=5oI9jK6fdhU)*A Window to Your Overall Health: Systemic Diseases and Blurred Vision
Sometimes, a blurry eye is the first sign that something is wrong elsewhere in your body. Unilateral blurred vision can be an early indicator of a systemic disease. The eyes are the only place in the body where doctors can directly visualize blood vessels and nerves in their natural, living state without surgical incision. Consequently, changes in the retinal vasculature often precede or mirror systemic complications. Early detection through routine eye exams can be life-saving, as ocular findings often prompt comprehensive medical workups that catch diseases before irreversible organ damage occurs.
- Diabetes: High blood sugar can damage the tiny blood vessels in the retina, a condition called diabetic retinopathy. This can cause swelling and fluid leakage, leading to blurred vision. Diabetic retinopathy progresses through stages: non-proliferative (weakened capillary walls leaking fluid) and proliferative (growth of fragile new vessels that can bleed into the vitreous). Diabetic macular edema (DME) specifically involves fluid accumulation in the central macula, causing significant central vision blurring. Strict glycemic control, with an HbA1c target generally below 7%, along with blood pressure and cholesterol management, dramatically slows disease progression. Annual dilated eye exams are mandatory for all diabetic patients, regardless of whether symptoms are present.
- High Blood Pressure (Hypertension): Chronically high blood pressure can also damage retinal blood vessels (hypertensive retinopathy), leading to vision problems. Elevated systemic pressure forces the retinal arterioles to constrict, which can lead to arteriovenous nicking, cotton wool spots (infarcts in the nerve fiber layer), flame-shaped hemorrhages, and in severe cases, papilledema (swelling of the optic disc). Malignant hypertension requires immediate medical intervention. Managing hypertension through diet, exercise, and antihypertensive medications often stabilizes retinal findings, though chronic damage may leave residual visual changes.
- Autoimmune Conditions: Diseases like Multiple Sclerosis (MS) can cause optic neuritis—inflammation of the optic nerve—leading to painful, blurred vision in one eye. Optic neuritis is frequently the first presenting symptom of MS, characterized by vision loss, washed-out color perception, and pain exacerbated by eye movement. Lupus (SLE), Sarcoidosis, Rheumatoid Arthritis, and Sjögren's syndrome can also cause severe ocular surface disease, uveitis, scleritis, or retinal vasculitis. Treatment typically involves a multidisciplinary approach, combining ophthalmology with rheumatology to manage underlying inflammation using corticosteroids, immunosuppressants, or biologic therapies.
Diagnosis and Treatment
If you experience any change in your vision, your first step should be to schedule a comprehensive eye exam with an optometrist or ophthalmologist. They can properly diagnose the cause through various tests, including:
- A visual acuity test: Using a Snellen or logMAR chart to measure clarity at various distances.
- A slit-lamp examination: A high-magnification microscope that allows detailed inspection of the anterior segment (cornea, iris, lens, and anterior chamber).
- Measuring your eye pressure: Utilizing Goldmann applanation tonometry, non-contact "puff" tonometry, or handheld devices to screen for glaucoma.
- Dilating your pupils to examine your retina and optic nerve: Drops widen the pupil, enabling a thorough view of the posterior segment using an ophthalmoscope or indirect lens.
Beyond these foundational tests, your doctor may employ advanced diagnostic technologies. Optical Coherence Tomography (OCT) provides high-resolution cross-sectional images of the retina, crucial for detecting macular edema, glaucomatous nerve damage, and subtle retinal layers issues. Fluorescein angiography involves injecting a dye into the arm vein and photographing its passage through retinal vessels to identify leaks, blockages, or abnormal vascularization. Visual field testing maps peripheral vision to detect glaucomatous blind spots or neurological deficits. If a systemic or neurological origin is suspected, your eye doctor may coordinate with your primary care physician or neurologist for MRI, CT scans, carotid ultrasounds, or comprehensive blood panels.
Treatment will vary widely depending on the diagnosis, ranging from a new eyeglass prescription to medicated eye drops, injections, laser procedures, or surgery. For example, mild dry eye may resolve with over-the-counter lubricants and environmental modifications, while wet AMD requires ongoing intravitreal injections. Corneal infections demand targeted antimicrobial therapy, and cataracts are definitively resolved through lens replacement surgery. Post-treatment care is equally vital. Patients must adhere to prescribed medication schedules, attend follow-up appointments to monitor healing or disease stability, and report any recurrent symptoms immediately. Vision rehabilitation services are also available for those who experience permanent vision loss, offering training with low-vision aids, mobility training, and adaptive technologies to maintain independence.
Key Takeaways
- Don't Ignore It: Fuzzy or blurred vision in one eye should always be evaluated by a professional. Even mild or intermittent symptoms can indicate progressive conditions that are easier to treat in early stages.
- Know the Red Flags: Sudden onset accompanied by pain, headache, numbness, or flashes of light is a medical emergency. Time-sensitive interventions dramatically improve outcomes for strokes, retinal detachments, and glaucoma attacks.
- Common Causes are Treatable: Many cases are due to simple refractive errors, dry eye, or cataracts. Routine corrective measures, lifestyle adjustments, or elective surgeries can restore excellent visual function.
- It Can Signal Deeper Issues: Your eyes can reveal systemic health problems like diabetes and high blood pressure. An eye exam is essentially a non-invasive window into your cardiovascular and neurological health.
- Prevention and Monitoring Are Crucial: Regular comprehensive eye exams, proper management of chronic conditions, and protective habits significantly reduce the risk of severe unilateral vision loss.
Protecting your vision means being proactive. By understanding the potential causes and acting quickly when symptoms arise, you can ensure your eyes—and your body—stay healthy. Incorporate routine eye checkups into your wellness schedule just as you would dental visits or annual physicals. The earlier a problem is detected, the broader the range of effective treatments and the higher the likelihood of preserving your sight for decades to come.
Prevention and Long-Term Eye Health Strategies
Safeguarding your vision extends far beyond reacting to symptoms. Implementing evidence-based lifestyle habits can significantly reduce your risk of developing many of the conditions associated with unilateral blurred vision.
Nutritional Support for Ocular Health: Diet plays a profound role in retinal health. Leafy green vegetables like kale, spinach, and collard greens are rich in lutein and zeaxanthin, antioxidants that accumulate in the macula and filter harmful blue light. Fatty fish (salmon, mackerel, sardines) provide omega-3 fatty acids that support tear film stability and reduce dry eye symptoms. The AREDS2 formula (a specific blend of vitamins C, E, zinc, copper, lutein, and zeaxanthin) has been clinically proven to slow the progression of intermediate to advanced AMD in at-risk individuals. Consult your physician before starting any high-dose supplements, as they are not recommended for early-stage disease or healthy individuals without risk factors.
Environmental and Occupational Protection: Ultraviolet radiation accelerates cataract formation and contributes to macular degeneration. Wear sunglasses that block 100% of UVA and UVB rays whenever you are outdoors, regardless of cloud cover. Wide-brimmed hats add an extra layer of protection. In occupational or recreational settings where eye trauma is possible (construction, woodworking, sports, laboratory work), always wear ANSI-approved safety goggles or polycarbonate protective eyewear. Over 90% of sports-related and industrial eye injuries are preventable with proper protection.
Optimizing Digital Habits: Prolonged screen time is a major contributor to digital eye strain and meibomian gland dysfunction. Position your computer monitor slightly below eye level to encourage a partially closed eyelid, reducing tear evaporation. Ensure ambient lighting is roughly half as bright as typical office lighting to minimize glare and contrast strain. Use blue light filtering lenses or screen filters if you experience significant discomfort, though research indicates their primary benefit is improving sleep cycles rather than preventing retinal damage. Take scheduled micro-breaks to blink fully and deliberately, ensuring the meibomian glands express their protective oils.
Lifestyle Modifications and Chronic Disease Management: Smoking is one of the most significant modifiable risk factors for cataracts, AMD, optic neuropathy, and thyroid eye disease. Quitting at any age halts further vascular and oxidative damage. Regular aerobic exercise improves systemic circulation, lowers intraocular pressure naturally, and helps regulate blood glucose and blood pressure. Maintain a consistent sleep schedule, as chronic sleep deprivation can exacerbate dry eye and increase intraocular pressure fluctuations. Keep systemic conditions like hypertension, diabetes, and hyperlipidemia within target ranges through medication adherence, dietary modifications, and stress management techniques.
Frequently Asked Questions
Can stress and anxiety cause temporary blurred vision in one eye?
Yes, stress and anxiety can contribute to temporary visual disturbances, though they more commonly affect both eyes simultaneously. High stress levels trigger the release of cortisol and adrenaline, which can cause pupil dilation, increased intraocular pressure, and muscle tension around the eyes and jaw. This tension can lead to accommodative spasms, making it difficult to focus properly. Additionally, stress can trigger ocular migraines or exacerbate dry eye symptoms due to reduced blinking rates and altered tear composition. While stress-induced vision changes are typically reversible with relaxation, rest, and stress management techniques, any unilateral or persistent visual change should still be evaluated by an eye care professional to rule out underlying pathology.
How long should I wait to see if unilateral blurry vision resolves on its own?
You should not wait if the blurring is sudden, severe, painless, or accompanied by any red flag symptoms like flashes, floaters, pain, or neurological deficits. These require immediate emergency evaluation. For gradual, mild blurring that correlates with screen time, dryness, or known uncorrected refractive error, you may try lubricating eye drops, taking a visual break, or using corrective lenses for a few hours to a day. If the vision does not return to baseline within 24-48 hours, or if it worsens, schedule an appointment with an optometrist or ophthalmologist. The rule of thumb in ophthalmology is that any new, unexplained change in vision warrants professional assessment to prevent permanent damage or missed systemic disease.
Is fuzzy vision in one eye contagious?
The symptom of blurry vision itself is not contagious. However, if the underlying cause is an infectious agent like viral or bacterial conjunctivitis, or certain types of keratitis (such as herpes simplex keratitis), the infection itself can spread to the other eye or to other people through direct contact, shared towels, makeup, or contact lens solutions. Strict hygiene practices—frequent handwashing, avoiding touching the eyes, using separate bedding and towels, and not sharing eye cosmetics or contact lens supplies—are essential until a doctor confirms the condition and clears you. If only one eye is infected, be extremely careful not to transfer the infection to the healthy eye when applying medication or washing your face.
Should I stop wearing contact lenses if I experience blurred vision in one eye?
Absolutely. The moment you notice unexplained blurring, discomfort, redness, or light sensitivity in one eye while wearing contact lenses, remove the lenses immediately. Do not wear them again until an eye doctor has examined you and identified the cause. Sleeping in lenses, using expired solution, or wearing damaged lenses significantly increases the risk of microbial keratitis, a severe corneal infection that can rapidly lead to scarring and permanent vision loss. Switch to glasses until your appointment, and bring your contact lenses, solution, and case to your examination so your doctor can test them for contamination. Never attempt to "tough out" contact lens-related vision problems.
Can children develop unilateral blurred vision, and what are the warning signs?
Yes, children can develop unilateral blurred vision, and it requires prompt attention because their visual system is still developing until around age 8-10. Prolonged unilateral blur during this critical period can lead to amblyopia (lazy eye), where the brain permanently suppresses input from the blurrier eye, causing irreversible vision loss if untreated. Common causes in children include significant uncorrected refractive errors (especially astigmatism or anisometropia), strabismus (eye misalignment), congenital cataracts, or ptosis (drooping eyelid). Warning signs include squinting, covering one eye, tilting the head, poor depth perception, frequent eye rubbing, sitting too close to screens, or declining academic performance. Pediatric vision screenings are essential, and any suspected unilateral blur should trigger an immediate comprehensive pediatric eye exam.
References:
- American Migraine Foundation. (n.d.). Retinal Migraine. https://americanmigrainefoundation.org/retinal-migraine/
- Assil Gaur Eye Institute. (2024, July 3). Vision Suddenly Blurry? You May Be Having a Medical... https://assileye.com/blog/causes-of-blurry-vision/
- Besser, E. (n.d.). Blurry Vision In One Eye. Eduardo Besser, MD. https://www.eduardobessermd.com/blog/when-one-eye-sees-clearly-and-the-other-doesnt-causes-of-blurry-vision-in-one-eye
- Lazarus, R. (n.d.). 11 Causes of Blurry Vision in One Eye. Optometrists.org. https://www.optometrists.org/general-practice-optometry/guide-to-eye-health/11-causes-of-blurry-vision-in-one-eye/
- The EyeDoctors Optometrists. (n.d.). Causes of Blurry Vision in One Eye. https://www.theeyedoctors.net/eye-care-resources/eye-health/causes-of-blurry-vision-in-one-eye

About the author
Michael O'Connell, DO, is a board-certified emergency medicine physician working as an attending physician at a busy Level I Trauma Center in Philadelphia, Pennsylvania. He also serves as a clinical instructor for medical residents and is active in wilderness medicine.