Decoding Brown Stains on Teeth: Causes, Removal, and Prevention

Key points
- Foods and Drinks: Many popular foods and beverages contain intensely colored pigments called chromogens or acidic compounds called tannins that stick to tooth enamel. Over time, these can cause significant staining. Common culprits include coffee, tea, red wine, colas, dark berries, and sauces like soy or tomato sauce. The acidity in sodas, citrus fruits, and sports drinks plays a dual role: it erodes the protective enamel layer while simultaneously exposing the more porous subsurface layers to deeply colored molecules. Furthermore, sugary beverages feed oral bacteria, creating an acidic environment that accelerates demineralization and stain retention. To mitigate these effects, dental professionals recommend consuming staining beverages with meals rather than sipping them continuously throughout the day, as this allows saliva to neutralize acids and remineralize the tooth surface between exposures.
- Tobacco Use: Nicotine and tar from cigarettes, cigars, or chewing tobacco create stubborn yellow and brown stains that can become darker and harder to remove over time. When nicotine comes into contact with oxygen, it turns yellow, while tar deposits leave behind deep, penetrating brown or black discoloration. These compounds readily adhere to plaque deposits and enamel imperfections, creating a thick, uneven film that is notoriously difficult to eradicate. Beyond the cosmetic impact, tobacco use significantly increases the risk of periodontal disease, delayed healing, and oral cancer. The vasoconstrictive properties of nicotine also reduce blood flow to the gingival tissues, masking early signs of gum disease until it has progressed to advanced stages.
- Poor Oral Hygiene (Plaque and Tartar): When you don't brush and floss effectively, a sticky film of bacteria called plaque builds up. If not removed, plaque hardens into a rough, porous substance called tartar (or calculus). Tartar is typically yellow or brown and can only be removed by a dental professional. The calcification process begins within 24 to 72 hours after plaque formation, as calcium and phosphate ions from saliva precipitate into the bacterial matrix. Once mineralized, tartar creates a rough surface that readily traps additional stains and bacteria, creating a self-perpetuating cycle of discoloration and inflammation. If left unchecked, subgingival tartar can trigger chronic periodontitis, leading to bone loss, gum recession, and eventual tooth mobility.
- Chromogenic Bacteria: Your mouth contains a complex ecosystem of bacteria. Certain types, known as chromogenic bacteria, can produce dark pigments. While often associated with black stains, these bacteria can contribute to brown discoloration, especially along the gum line. Research indicates that these microorganisms produce hydrogen peroxide and iron-containing compounds that react with salivary proteins to form insoluble dark deposits. Interestingly, studies have observed that patients with pronounced chromogenic bacterial staining sometimes exhibit lower rates of dental caries, possibly due to altered salivary composition or bacterial competition that suppresses cariogenic species like Streptococcus mutans. Despite this potential protective correlation, professional cleaning remains necessary to remove the deposits and prevent associated gingival inflammation.
Noticing brown spots or stains on your teeth can be concerning, affecting both your confidence and your peace of mind. While these stains are often cosmetic, they can sometimes signal an underlying issue that needs attention. Understanding the cause is the first step toward restoring your bright, healthy smile.
This comprehensive guide, synthesizing information from leading health authorities and dental research, will help you identify the potential causes of brown stains, differentiate them from more serious issues like cavities, and explore safe and effective options for removal and prevention. Dental professionals emphasize that early intervention not only preserves the structural integrity of your teeth but also prevents more complex and costly procedures down the line. Whether you are dealing with a single isolated spot or widespread discoloration across multiple arches, this guide provides the clinical context and actionable steps necessary to navigate your oral health journey safely.
What Causes Brown Stains on Teeth?
Brown stains can appear as blotches, lines, or spots and can range from yellowish-brown to a very dark brown. They fall into two main categories: extrinsic (on the surface) and intrinsic (inside the tooth). Understanding the distinction between these categories is crucial for selecting the appropriate treatment pathway. Extrinsic stains are generally responsive to mechanical cleaning or chemical bleaching, whereas intrinsic discoloration often requires restorative dental work or specialized internal bleaching techniques. The severity, distribution, and texture of the stain provide valuable diagnostic clues about its origin and progression.
Extrinsic Stains: The Surface-Level Culprits
Extrinsic stains affect the outer layer of the tooth, called the enamel. These are the most common types of stains and are often caused by lifestyle and dietary factors. Enamel is not a perfectly smooth, impenetrable surface; at a microscopic level, it contains tiny pores and ridges. Over time, repeated exposure to pigmented substances allows chromogens to penetrate these micro-porosities, binding tightly to the hydroxyapatite crystals that make up your enamel matrix. Additionally, dietary acids can temporarily soften the enamel surface, making it even more receptive to staining agents. This biological interaction explains why certain habits lead to cumulative, stubborn discoloration that brushing alone cannot resolve.
- Foods and Drinks: Many popular foods and beverages contain intensely colored pigments called chromogens or acidic compounds called tannins that stick to tooth enamel. Over time, these can cause significant staining. Common culprits include coffee, tea, red wine, colas, dark berries, and sauces like soy or tomato sauce. The acidity in sodas, citrus fruits, and sports drinks plays a dual role: it erodes the protective enamel layer while simultaneously exposing the more porous subsurface layers to deeply colored molecules. Furthermore, sugary beverages feed oral bacteria, creating an acidic environment that accelerates demineralization and stain retention. To mitigate these effects, dental professionals recommend consuming staining beverages with meals rather than sipping them continuously throughout the day, as this allows saliva to neutralize acids and remineralize the tooth surface between exposures.
- Tobacco Use: Nicotine and tar from cigarettes, cigars, or chewing tobacco create stubborn yellow and brown stains that can become darker and harder to remove over time. When nicotine comes into contact with oxygen, it turns yellow, while tar deposits leave behind deep, penetrating brown or black discoloration. These compounds readily adhere to plaque deposits and enamel imperfections, creating a thick, uneven film that is notoriously difficult to eradicate. Beyond the cosmetic impact, tobacco use significantly increases the risk of periodontal disease, delayed healing, and oral cancer. The vasoconstrictive properties of nicotine also reduce blood flow to the gingival tissues, masking early signs of gum disease until it has progressed to advanced stages.
- Poor Oral Hygiene (Plaque and Tartar): When you don't brush and floss effectively, a sticky film of bacteria called plaque builds up. If not removed, plaque hardens into a rough, porous substance called tartar (or calculus). Tartar is typically yellow or brown and can only be removed by a dental professional. The calcification process begins within 24 to 72 hours after plaque formation, as calcium and phosphate ions from saliva precipitate into the bacterial matrix. Once mineralized, tartar creates a rough surface that readily traps additional stains and bacteria, creating a self-perpetuating cycle of discoloration and inflammation. If left unchecked, subgingival tartar can trigger chronic periodontitis, leading to bone loss, gum recession, and eventual tooth mobility.
- Chromogenic Bacteria: Your mouth contains a complex ecosystem of bacteria. Certain types, known as chromogenic bacteria, can produce dark pigments. While often associated with black stains, these bacteria can contribute to brown discoloration, especially along the gum line. Research indicates that these microorganisms produce hydrogen peroxide and iron-containing compounds that react with salivary proteins to form insoluble dark deposits. Interestingly, studies have observed that patients with pronounced chromogenic bacterial staining sometimes exhibit lower rates of dental caries, possibly due to altered salivary composition or bacterial competition that suppresses cariogenic species like Streptococcus mutans. Despite this potential protective correlation, professional cleaning remains necessary to remove the deposits and prevent associated gingival inflammation.
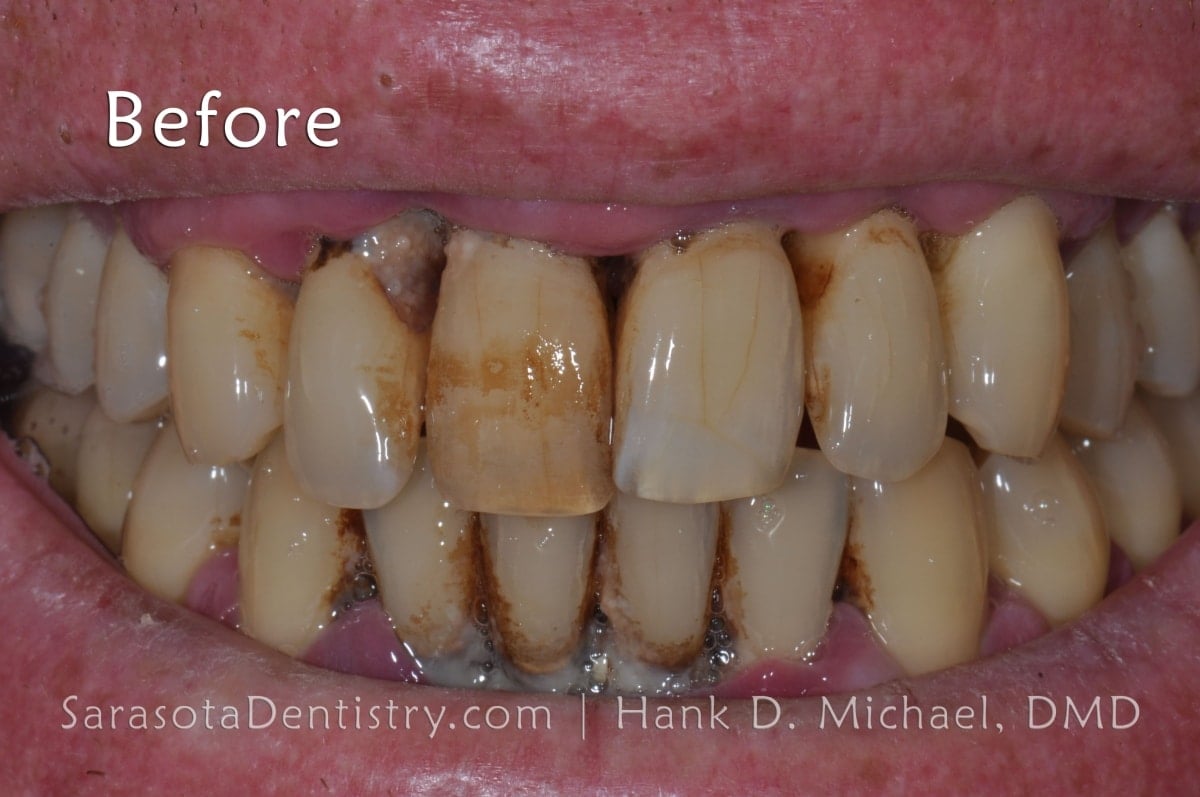 Image Source: Sarasota Dentistry
Image Source: Sarasota Dentistry
Understanding the microscopic architecture of your teeth helps clarify why stains behave differently. The enamel rod structure acts as a semi-permeable membrane, allowing small molecules to diffuse inward while attempting to maintain surface hardness. When this barrier is compromised by acid erosion, abrasion, or genetic variations, the rate of pigment accumulation increases exponentially.
Intrinsic Stains: Discoloration From Within
Intrinsic stains originate from within the tooth structure, making them more resistant to over-the-counter whitening products. Because the discoloration lies beneath the enamel, either within the dentin layer or the pulp chamber itself, surface cleaning agents cannot reach the source. These stains typically require internal dental interventions, such as non-vital bleaching, microabrasion, or restorative coverings. Intrinsic discoloration often reflects systemic conditions, developmental disruptions, or localized trauma, necessitating a comprehensive clinical evaluation to identify and address the root cause.
- Tooth Decay (Cavities): This is one of the most serious causes of brown spots. As bacteria produce acids that erode enamel, they can create a hole, or cavity. The decay process often appears as a brown or black spot on the tooth's surface. In its earliest stage, demineralization appears as a chalky white lesion. However, as the process advances, proteins and bacteria infiltrate the weakened matrix, creating brown pigmentation. Once decay penetrates the dentin, it spreads laterally along the dentinoenamel junction, potentially compromising the tooth's structural core. Early detection is critical, as remineralization therapies and fluoride varnishes can arrest initial lesions before they become cavitations requiring restorative drilling.
- Fluorosis: While fluoride is beneficial for teeth, excessive intake during childhood when teeth are developing can cause a condition called fluorosis. This can range from faint white lines to more severe brown spots and pitting on the enamel. Fluoride incorporates into the developing hydroxyapatite crystals, forming fluorapatite, which is more acid-resistant than natural enamel. However, chronic overexposure disrupts the enamel-forming ameloblast cells, leading to hypomineralization. The resulting porous enamel readily absorbs dietary pigments, transforming mild white striations into noticeable brown discoloration. Preventive guidance emphasizes monitoring total fluoride exposure, including toothpaste swallowing, fluoridated water, and dietary supplements, particularly in children under eight years old.
- Medications: Certain antibiotics, like tetracycline and doxycycline, can cause intrinsic staining if taken by children whose teeth are still forming. Some mouthwashes containing chlorhexidine can also cause surface staining. Tetracycline molecules have a high affinity for calcium and bind directly to developing dentin and enamel. When exposed to ultraviolet light, these complexes undergo photo-oxidation, shifting from yellow to dark brown or gray over time. The severity correlates directly with the dosage, duration of use, and stage of tooth development during administration. While chlorhexidine-induced staining is technically extrinsic, it forms tenacious complexes with dietary tannins and salivary proteins that require professional polishing for removal. Dentists carefully weigh the benefits against the cosmetic risks when prescribing these agents.
- Aging: Over time, the outer enamel layer naturally thins, revealing the yellowish layer of dentin underneath. This can make teeth appear darker or more yellow-brown. Decades of masticatory stress, acidic challenges, and natural attrition gradually wear down enamel at an estimated rate of a few micrometers per year. Simultaneously, the pulp chamber undergoes secondary dentinogenesis, reducing its volume and altering the tooth's optical properties. The increased translucency of aged enamel, combined with the naturally darker underlying dentin, creates a cumulative darkening effect that is entirely physiological. While this process cannot be reversed, modern adhesive dentistry and controlled whitening protocols can safely restore a brighter, more youthful appearance.
- Trauma: An injury to a tooth can damage the nerve and blood vessels inside, causing the tooth to "die" and turn dark brown, gray, or black. When the blood supply is severed or compromised following impact, red blood cells break down within the pulp chamber, releasing hemoglobin byproducts like hemosiderin. These iron-containing pigments infiltrate the dentinal tubules, resulting in a gradual darkening of the tooth structure. In some cases, the pulp may become necrotic and calcify, while in others, internal resorption can create localized pinkish or brown lesions. Prompt evaluation after dental trauma allows for timely interventions such as splinting, root canal therapy, or internal bleaching to preserve both function and aesthetics.
- Medical Conditions: Though less common, certain health issues can lead to tooth discoloration. Celiac disease, for example, can cause dental enamel defects that appear as white, yellow, or brown spots. The malabsorption of essential nutrients like calcium, phosphorus, and fat-soluble vitamins during critical periods of odontogenesis disrupts normal enamel mineralization. Additionally, untreated celiac disease can trigger autoimmune responses that cross-react with dental tissues. Other systemic conditions linked to intrinsic staining include porphyria, which deposits reddish-brown porphyrin metabolites into developing teeth, and hyperbilirubinemia (jaundice) in neonates, which can cause a greenish-brown discoloration of primary dentition. Recognizing oral manifestations of systemic disease enables earlier multidisciplinary intervention.
- Genetics: Your natural tooth color, enamel thickness, and susceptibility to staining can be inherited. Amelogenesis imperfecta and dentinogenesis imperfecta are hereditary conditions that fundamentally alter enamel and dentin structure, often resulting in yellow-brown or opalescent discoloration. These genetic mutations affect proteins like amelogenin and enamelin that are critical for proper crystal formation. Patients with thinner enamel or naturally higher dentin opacity will naturally exhibit a warmer baseline tooth shade and may stain more readily from external agents. While genetic predispositions cannot be altered, personalized preventive strategies and restorative planning can effectively manage their clinical and cosmetic impacts.
Is It a Benign Stain, Tartar, or a Cavity?
It can be difficult to tell the difference between a harmless stain and a more serious problem. While only a dentist can give you a definitive diagnosis, here are some visual clues:
- Benign Stain: Often appears as a uniform discoloration across the surface of multiple teeth, especially the front ones. The tooth texture feels smooth. These stains typically conform to the natural contours of the tooth and do not disrupt the structural integrity of the enamel. They often develop gradually over months or years and may lighten temporarily after a thorough brushing or dietary modification.
- Tartar: Looks like a hard, crusty deposit that is typically concentrated along the gum line and between the teeth. It cannot be brushed or flossed away. When probed gently, tartar feels rough, gritty, and firmly attached to the tooth surface. It often has an irregular, scalloped margin that traps plaque and irritates adjacent gingival tissues. Supragingival calculus is visible to the naked eye, while subgingival tartar may only be detected through professional probing, dental radiographs, or specialized transillumination techniques.
- Cavity: Often starts as a small, concentrated brown or black spot. The area may feel soft or sticky to a dental instrument, and it can be accompanied by sensitivity to hot, cold, or sweet foods. Cavities frequently localize in pit and fissure anatomy, proximal contact areas, or along existing restorations where plaque stagnation occurs. As demineralization progresses, the enamel surface may appear opaque or chalky before collapsing into an actual defect. Advanced lesions can cause lingering pain, visible fracturing of the crown, or spontaneous sensitivity without thermal or osmotic triggers.
Important: If you notice a new brown spot, especially if it's accompanied by pain or sensitivity, schedule a visit with your dentist immediately. Early diagnosis drastically improves prognosis, minimizes treatment invasiveness, and prevents irreversible pulp damage or periodontal breakdown.
Dental professionals utilize multiple diagnostic modalities to differentiate these conditions accurately. Visual examination under magnification reveals surface topography and color gradients. Tactile assessment with an explorer determines hardness versus stickiness. Radiographic imaging detects subsurface demineralization, proximal decay, and calculus deposits that are not visible clinically. Laser fluorescence devices and quantitative light-induced fluorescence (QLF) can quantify early mineral loss and stain depth, providing objective baseline data for monitoring progression over time. Self-diagnosis often leads to unnecessary anxiety or dangerous delays in care; trusting clinical expertise ensures appropriate management.
How to Remove Brown Stains from Teeth
The best method for removing brown stains depends entirely on the cause. A thorough diagnostic assessment allows your dental team to recommend a targeted approach that addresses both the symptom and its underlying etiology. Combining conservative therapies with advanced techniques often yields the most predictable and aesthetically pleasing outcomes. Patient compliance, baseline oral hygiene, and realistic expectations play equally important roles in long-term success.
At-Home and Over-the-Counter (OTC) Options
For mild, extrinsic stains, some at-home solutions may offer improvement. These modalities are generally safe for routine use but work best when integrated into a comprehensive preventive regimen. They are not designed to correct structural defects, intrinsic discoloration, or active disease processes.
- Excellent Oral Hygiene: Brushing twice a day with fluoride toothpaste and flossing daily is your first line of defense against plaque buildup and surface stains. Adopting the modified Bass technique, which involves angling the bristles at 45 degrees toward the gumline and using gentle vibratory motions, optimally disrupts bacterial biofilms without causing gingival recession. Interdental cleaning with floss, water flossers, or interdental brushes removes proximal plaque that toothbrush bristles cannot reach, preventing interproximal staining and early caries. Consistency matters far more than intensity; gentle, thorough cleaning preserves enamel integrity while maintaining a clean surface that resists pigment adhesion.
- Whitening Toothpastes: These products contain mild abrasives that can help scrub away surface stains but will not change the intrinsic color of your teeth. Ingredients like hydrated silica, calcium carbonate, and polyphosphates physically disrupt stain adhesion while chemical agents break down pellicle-bound pigments. When selecting a toothpaste, check the Relative Dentin Abrasivity (RDA) value to ensure it falls within safe limits (below 250, preferably under 100 for daily use). Overly abrasive formulations can cause enamel wear and increased dentin sensitivity, ultimately making teeth appear darker as thinner enamel reveals the yellowish dentin beneath.
- OTC Whitening Strips and Gels: These use low concentrations of peroxide to bleach surface stains. Look for products with the American Dental Association (ADA) Seal of Acceptance. Active ingredients like hydrogen peroxide or carbamide peroxide penetrate the enamel and oxidize large, pigmented organic molecules into smaller, colorless fragments. Treatment typically spans 7 to 14 days, with gradual shade improvements visible after the first few applications. Proper tray fit or strip placement ensures even distribution and minimizes gel contact with gingival tissues, which can cause temporary irritation. Always follow manufacturer instructions precisely to avoid overuse, which can lead to transient sensitivity and enamel dehydration.
A Word of Caution on "Natural" Remedies
Home remedies like activated charcoal, lemon juice, and apple cider vinegar are often promoted online. However, dental professionals advise against them. These substances are highly abrasive or acidic and can permanently damage your tooth enamel, leading to increased sensitivity and making your teeth more susceptible to future staining. Lemon juice and vinegar typically have a pH between 2 and 3, far below the critical demineralization threshold of 5.5, causing rapid calcium leaching from the enamel surface. Activated charcoal, despite marketing claims, lacks standardized particle size and often exhibits high abrasivity, acting like fine sandpaper that scratches the enamel and creates microscopic roughness where new stains readily accumulate. Evidence-based dentistry prioritizes clinically tested, regulated formulations over unverified DIY treatments that compromise long-term tooth structure.
Professional Dental Treatments
For effective, safe, and lasting results, professional treatments are the gold standard. These procedures are performed or supervised by licensed dental professionals who can customize protocols, monitor tissue response, and address complications immediately.
- Professional Dental Cleaning: This is the most effective way to remove stains caused by plaque and tartar. A dental hygienist uses special tools to scale away tartar and then polishes the teeth to remove surface stains. Ultrasonic scalers utilize high-frequency vibrations and water irrigation to safely fracture and flush away mineralized deposits, while hand instruments allow precise debridement in sensitive or anatomically complex areas. Following scaling, prophylactic paste polishing with a rubber cup or air-polishing device eliminates residual stains and smoothens the enamel surface, significantly delaying future biofilm and pigment accumulation.
- Professional Teeth Whitening: For deeper extrinsic stains, in-office bleaching or custom-fitted take-home trays from your dentist use higher-concentration, professional-grade bleaching agents for dramatic and reliable results. In-office procedures typically employ 25% to 40% hydrogen peroxide activated by specialized lights, heat, or lasers to accelerate oxidation, delivering noticeable shade improvements in a single 60 to 90-minute visit. Dentist-dispensed take-home trays use 10% to 20% carbamide peroxide worn for 1 to 4 hours daily over 10 to 14 days. Custom trays ensure uniform gel distribution and minimize soft tissue exposure, while professional oversight allows for desensitizing adjuncts like potassium nitrate or fluoride treatments before, during, and after the process.
- Dental Bonding: A tooth-colored composite resin can be applied to the tooth's surface to cover up severe or intrinsic stains that don't respond to whitening. This conservative, minimally invasive procedure involves etching the enamel with a mild acid, applying a bonding agent, and sculpting layered composite that is cured with a high-intensity blue light. The material is then shaped, polished, and color-matched to adjacent teeth. Bonding is particularly effective for localized discoloration, enamel hypoplasia, or fluorosis. While highly aesthetic, composite bonding may require periodic touch-ups or replacement after 5 to 7 years due to normal wear, staining at margins, or material fatigue.
- Porcelain Veneers: These are thin, custom-made ceramic shells that are bonded to the front of the teeth to completely mask deep discoloration and create a uniform, white appearance. Veneers require minimal enamel preparation, typically removing only 0.3 to 0.5 millimeters of tooth structure. The ceramic material is highly stain-resistant, biocompatible, and mimics the light-scattering properties of natural enamel, delivering exceptional aesthetic results. Indications include severe tetracycline staining, extensive fluorosis, traumatic necrosis, or cases where patients desire predictable, long-lasting cosmetic transformation. With proper care, veneers can last 10 to 20 years.
- Dental Crowns: If a tooth is both discolored and significantly weakened by decay or trauma, a crown (or cap) can be placed over the entire tooth to restore its strength and appearance. Full-coverage restorations require circumferential preparation, followed by impression or digital scanning to fabricate a restoration from zirconia, lithium disilicate, or porcelain-fused-to-metal. Crowns protect compromised tooth structure from fracture, re-establish proper occlusion, and completely conceal underlying discoloration. They represent the definitive restorative solution for teeth that have undergone root canal therapy, experienced massive structural loss, or suffered severe developmental anomalies.
How to Prevent Brown Stains on Your Teeth
Practicing preventive care is the easiest way to maintain a bright, stain-free smile. Prevention extends far beyond cosmetic benefits; it preserves enamel architecture, reduces caries risk, and supports lifelong periodontal health. A proactive approach minimizes the need for corrective interventions and maximizes the longevity of natural tooth structure.
- Practice Good Oral Hygiene: Brush for two minutes, twice a day, and floss daily. Consistency builds a resilient oral microbiome that discourages pathogenic colonization. Replace your toothbrush or brush head every 3 to 4 months, or sooner if bristles appear frayed, as worn filaments lose their cleaning efficacy. Incorporate an antimicrobial mouthwash if recommended, but avoid alcohol-based formulations if you experience dry mouth, as alcohol can exacerbate tissue dehydration and compromise the protective salivary pellicle.
- Get Regular Dental Cleanings: Visit your dentist every six months (or as recommended) for check-ups and professional cleanings to remove plaque and tartar before they cause significant staining. Patients with periodontal disease, orthodontic appliances, systemic conditions like diabetes, or high caries risk may benefit from 3 to 4 month maintenance intervals. These visits allow for early detection of enamel defects, occlusal wear patterns, and emerging stains before they become entrenched.
- Modify Your Diet: Limit your consumption of coffee, tea, red wine, and other staining foods and drinks. When you do consume them, pair them with water-rich, crunchy vegetables like celery, carrots, or cucumbers, which stimulate saliva flow and provide gentle mechanical cleansing. Reduce snacking frequency to allow salivary pH to normalize between meals, facilitating natural remineralization and reducing the window of enamel vulnerability.
- Use a Straw: When drinking dark beverages, a straw can help minimize their contact with your front teeth. Positioning the straw toward the posterior region of the mouth allows liquids to bypass the visible facial surfaces of anterior teeth. Opt for wide-bore silicone or stainless steel straws, which are durable, easy to clean, and environmentally sustainable compared to single-use plastics.
- Rinse with Water: After consuming staining foods or drinks, swish your mouth with water to help wash away staining compounds. This simple habit dilutes residual acids and pigments, restores oral pH balance, and reduces pigment adherence time. Chewing sugar-free xylitol gum for 10 to 15 minutes after meals further enhances salivary flow, buffers acids, and inhibits cariogenic bacterial metabolism through osmotic disruption and competitive inhibition.
- Quit Tobacco: Eliminating tobacco use is one of the best things you can do for your oral health and the appearance of your teeth. Within days of cessation, circulation to gingival tissues improves, and the oxidative stress burden on oral mucosa decreases. Seek support through nicotine replacement therapy, prescription medications, counseling programs, or digital cessation apps. The long-term benefits extend to dramatically reduced risks of periodontitis, implant failure, and oral malignancies.
When to See a Dentist
You should always consult a dentist to determine the cause of brown stains and discuss the safest treatment options. It is especially important to make an appointment if:
- The stains appeared suddenly.
- You have tooth pain or sensitivity.
- You see a visible pit or hole in your tooth.
- The stains are accompanied by bleeding or swollen gums.
- The stains don't improve after a few weeks of diligent oral hygiene.
A professional evaluation will ensure you're not just masking a more serious problem like a cavity and will help you choose the most effective path back to a healthy, confident smile. Dental emergencies involving discoloration with swelling, fever, or spontaneous throbbing pain require immediate attention, as these signs may indicate pulp necrosis, abscess formation, or spreading infection. For non-urgent concerns, scheduling a routine examination allows for comprehensive diagnostics, personalized treatment planning, and transparent cost discussions. Many practices offer cosmetic consultations that utilize digital smile design software to simulate potential outcomes before committing to irreversible procedures. Early intervention consistently yields better prognoses, shorter chair time, and more conservative therapeutic approaches.
References
- Cleveland Clinic. (n.d.). Tooth Discoloration.
- Huizen, J. (2020). What to do about brown spots on your teeth. Medical News Today.
- Whelan, C. (2017). Brown Spots on Teeth: Causes, Treatment, and Prevention. Healthline.
- Kumar, M., Madi, M., Vineetha, R. et al. (2025). Chromogenic bacterial staining of teeth: a scoping review. BMC Oral Health.
Frequently Asked Questions
Can brown stains on teeth be a sign of cancer?
While brown stains themselves are rarely indicative of oral cancer, certain oral malignancies or precancerous lesions can present as discolored patches on the gums, palate, or floor of the mouth. Squamous cell carcinoma and erythroplakia typically appear as red or speckled lesions, but pigment changes in surrounding tissues or unexplained ulcerations alongside discoloration warrant immediate professional evaluation. Risk factors include tobacco use, heavy alcohol consumption, and HPV infection. Any persistent, non-healing, irregularly bordered, or rapidly changing discoloration that does not correspond to known staining sources should be biopsied or closely monitored by an oral medicine specialist to rule out malignancy.
How long does it take for professional whitening results to become visible?
Most patients notice a measurable shade improvement after the first professional whitening session, with final results stabilizing approximately 2 to 14 days post-treatment. During this initial period, teeth undergo a dehydration phase where microscopic enamel pores temporarily close, causing the shade to appear slightly brighter than baseline immediately after the procedure. Over the following days, saliva rehydrates the enamel, and the true oxidized shade emerges. Take-home tray protocols require consistent nightly wear to achieve cumulative bleaching effects. Results typically last 1 to 3 years, depending on dietary habits, tobacco use, and adherence to touch-up regimens. Maintenance whitening and routine prophylaxis significantly extend the longevity of your investment.
Are brown stains on children's teeth different from those on adults?
Yes, pediatric discoloration often involves developmental, dietary, or hygiene-related factors distinct from adult staining patterns. Common causes in children include enamel hypoplasia, early childhood caries (often linked to prolonged bottle feeding or sugary sippy cups), fluorosis from excessive supplement or toothpaste ingestion, and iron supplement staining. Children's enamel is thinner and less mineralized than adult enamel, making it more porous and susceptible to rapid pigment penetration and demineralization. Pediatric dentists emphasize early intervention, as untreated decay in primary teeth can affect permanent tooth eruption, speech development, and nutritional intake. Treatment focuses on minimally invasive techniques, behavior guidance, and caregiver education to establish sustainable preventive routines.
Will dental bonding stain over time, and how can I maintain it?
Composite bonding materials are highly aesthetic but not entirely stain-proof. Over time, the resin matrix can absorb pigments from coffee, tea, red wine, and tobacco, particularly at the margins where the material interfaces with natural enamel. The surface polish may also gradually wear down, creating microscopic roughness that attracts plaque. To maximize longevity, maintain meticulous oral hygiene, limit exposure to intensely pigmented substances, and attend regular professional cleanings where hygienists use specialized polishing pastes safe for composites. Avoid biting on extremely hard objects like ice or pens, which can chip the material. With proper care, bonded restorations can maintain their appearance for 5 to 10 years before requiring resurfacing or replacement.
Can brown stains disappear on their own without treatment?
Benign extrinsic stains from dietary sources or mild plaque accumulation may lighten slightly with improved hygiene, professional cleaning, or temporary salivary pH normalization, but they rarely resolve completely without intervention. Intrinsic stains, cavities, fluorosis, and trauma-induced discoloration do not improve spontaneously and typically progress without professional management. Enamel does not regenerate, and once structural damage or deep pigmentation occurs, biological healing cannot reverse the visible change. Relying on the passage of time or unverified home remedies often allows underlying pathology to advance, increasing treatment complexity and cost. Proactive dental evaluation ensures accurate diagnosis and appropriate therapeutic intervention before irreversible changes occur.
Conclusion
Brown stains on teeth encompass a wide spectrum of etiologies, ranging from harmless surface discoloration caused by dietary pigments to clinically significant conditions like active decay, developmental anomalies, or traumatic pulp necrosis. Understanding the distinction between extrinsic and intrinsic discoloration is fundamental to selecting the most appropriate, effective, and safe treatment pathway. While over-the-counter products and improved home care can successfully manage mild surface staining, professional evaluation remains indispensable for accurate diagnosis, early disease detection, and customized restorative planning.
Prevention consistently outperforms correction when it comes to maintaining a bright, healthy smile. Consistent oral hygiene routines, mindful dietary choices, regular professional cleanings, and tobacco cessation collectively create an oral environment that resists pigment accumulation and structural breakdown. When stains do occur, modern dentistry offers a robust arsenal of conservative and advanced interventions—from professional prophylaxis and controlled bleaching to adhesive bonding and ceramic restorations—that can restore both aesthetics and function.
If you notice persistent, unexplained, or symptomatic discoloration, do not delay seeking professional guidance. Early intervention preserves natural tooth structure, minimizes treatment invasiveness, and safeguards your long-term oral health. By partnering with your dental care team, you can confidently navigate stain removal, implement sustainable preventive strategies, and achieve a resilient, radiant smile that enhances your overall well-being for years to come.

About the author
Benjamin Carter, MD, is a board-certified otolaryngologist specializing in head and neck surgery, with an expertise in treating throat cancer. He is an associate professor and the residency program director at a medical school in North Carolina.