Blood Pooling in Hands: Causes, Symptoms, and Treatment

Key points
- Injury and Bruising (Hematoma): An injury can cause blood to pool under the skin, forming a bruise (hematoma). Trauma disrupts capillary integrity, allowing whole blood to extravasate into subcutaneous spaces. Initial management follows RICE principles (Rest, Ice, Compression, Elevation), with ice applied for 15-minute intervals during the first 48 hours to limit hematoma expansion.
- Blood Clots in the Arm: Though rare, a clot in an arm vein (deep vein thrombosis or DVT) can cause sudden, significant swelling, redness, and pain in one arm. This is a medical emergency. Upper extremity DVT often relates to repetitive overhead motion (effort thrombosis or Paget-Schroetter syndrome), central venous catheters, or underlying hypercoagulable states. Prompt anticoagulation is critical to prevent pulmonary embolism.
- Heart or Kidney Conditions: Heart failure or kidney disease can cause systemic fluid retention (edema), which can lead to swelling in the hands. Reduced cardiac output activates the renin-angiotensin-aldosterone system (RAAS), promoting sodium and water retention. Diuretics, dietary sodium restriction, and targeted management of the underlying organ dysfunction typically resolve the peripheral swelling.
- Medications: Some drugs, like certain blood pressure medications, can cause swelling in the hands and feet as a side effect. Calcium channel blockers (e.g., amlodipine), NSAIDs, corticosteroids, and certain diabetes medications (thiazolidinediones) are common culprits. Drug-induced edema is usually dose-dependent and often resolves with dosage adjustment or medication substitution under medical supervision.
- Hormonal Fluctuations: Estrogen and progesterone significantly influence vascular permeability and sodium retention. Many women experience cyclical hand swelling during the luteal phase of the menstrual cycle, pregnancy, or perimenopause. Progesterone promotes smooth muscle relaxation in venous walls, while elevated estrogen increases capillary permeability. These changes are physiologic and typically resolve postpartum or post-menopause.
Have you ever noticed your hands turning red, swollen, or your veins bulging after they’ve been hanging down for a while or after a brisk walk? You might have experienced "blood pooling in the hands." It can be a little alarming, but what does it really mean? In this comprehensive guide, we’ll explore what blood pooling in the hands is, why it happens, what causes it, and how to manage or prevent it. For many individuals, this phenomenon is an occasional, harmless quirk of human physiology, but understanding the underlying mechanisms can help distinguish between normal vascular responses and signs that warrant medical evaluation.
What Is Blood Pooling in the Hands?
Blood pooling in the hands refers to a situation where blood accumulates in the veins of your hands (and sometimes fingers) instead of circulating back promptly to your heart. This can cause your hands to appear reddish or bluish, swell up slightly, or feel heavier or warmer than usual. It is important to distinguish true venous blood pooling from generalized edema, which involves fluid leaking from capillaries into the interstitial tissue spaces. While both can cause swelling, blood pooling specifically relates to venous stasis or delayed venous return, often visible as distended, ropey veins on the dorsal surface of the hands.
The Basics of Blood Circulation
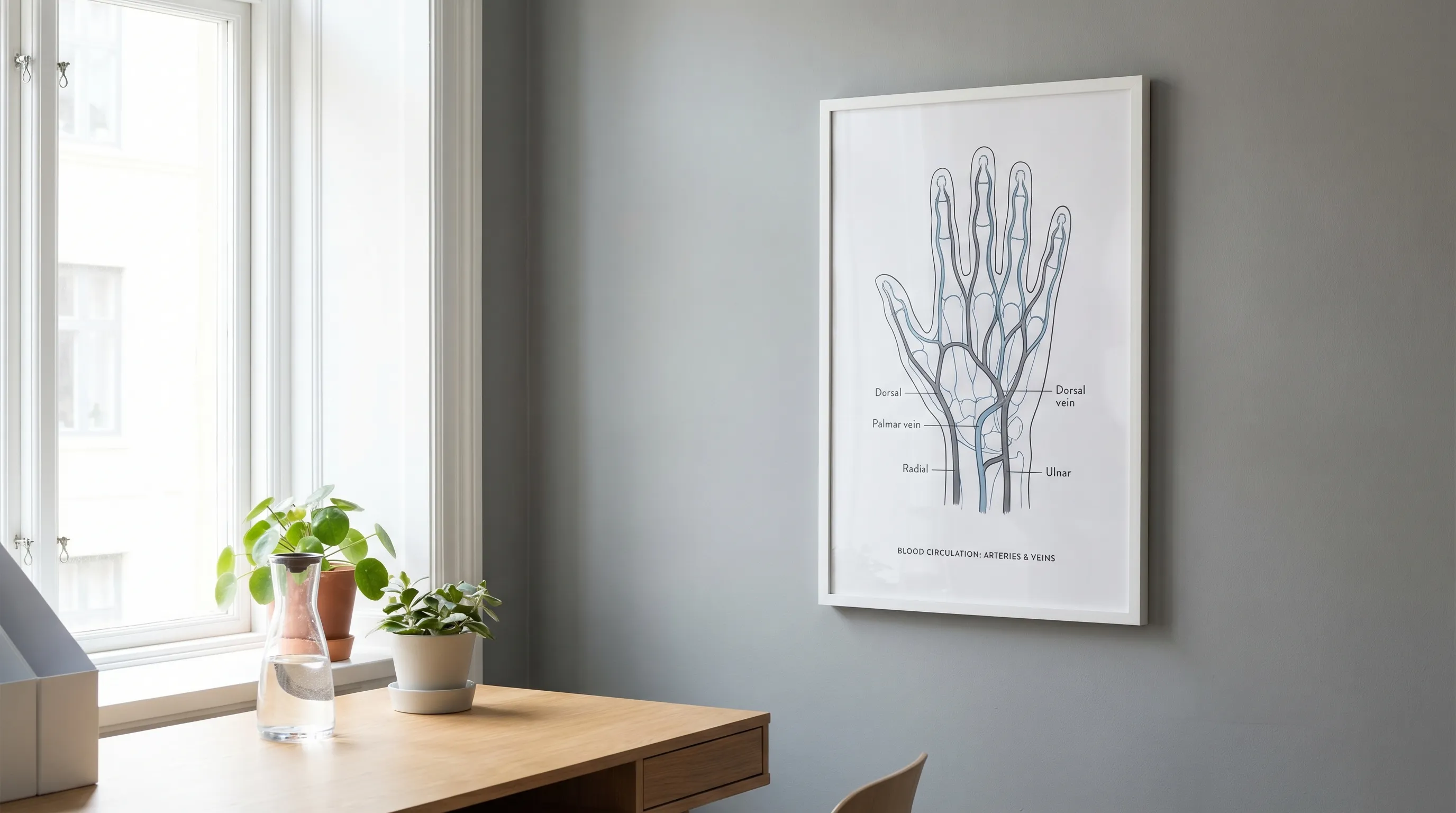
To understand blood pooling, let's review how blood normally flows. The heart pumps oxygen-rich blood through arteries to your tissues. After delivering oxygen, the blood returns to the heart through veins.
Veins have one-way valves that help keep blood moving upward, against gravity. When you move your muscles (like swinging your arms or clenching your fists), they squeeze the veins and help push blood along. This is often called the “muscle pump”. Without regular muscular contraction, especially in the forearms and fingers, venous blood lacks the mechanical assistance needed to overcome gravitational pull efficiently.
However, if your arms are hanging down motionless for a long time, gravity can make it harder for blood to flow back up. Blood might start to “pool” in the hand, leading to swelling, redness, or a throbbing sensation. This temporary stasis increases hydrostatic pressure within the capillary beds, which can cause mild fluid transudation into the surrounding tissues, explaining why the skin may feel tight or puffy.
The lymphatic system also plays a crucial supporting role in this process. Tiny lymphatic vessels run parallel to veins and help drain excess interstitial fluid, proteins, and cellular debris. When venous pooling occurs, the lymphatic vessels may become temporarily overwhelmed, exacerbating the feeling of heaviness and puffiness. Fortunately, the lymphatic system relies heavily on muscle contraction and rhythmic breathing to move fluid centrally, which is why raising your arms and taking deep breaths often provides rapid relief.
In many cases, occasional mild blood pooling in the hands is normal. But sometimes, frequent or severe pooling can signal underlying health issues that may need attention. Recognizing the difference between physiological adaptation and pathological venous dysfunction is key to maintaining long-term vascular health.
Why Do My Hands Feel Swollen or Look Discolored?
Several factors can cause blood to pool in your hands. Some are harmless and temporary, while others may indicate a circulatory problem. The interplay between environmental conditions, anatomical variations, and systemic health dictates how prominently this symptom presents.
1. Gravity and Prolonged Arm Position
The simplest reason is gravity. When your arms hang down for extended periods, your heart must work against gravity to pump blood back up. Without muscle movement to help, blood flow can slow down, causing your hands to become red, swollen, or veiny. The venous pressure in the hands can easily double when the arms are fully extended downward compared to when they are resting at heart level.
For example, after a long walk or standing for a while, you might notice your fingers getting puffier. This is a form of mild blood pooling. Once you raise your hands or move them, the swelling usually subsides. This phenomenon is particularly common in professions requiring prolonged standing or static postures, such as retail work, teaching, or assembly line tasks. Wearing tight sleeves or restrictive wristbands can further impede venous return and exacerbate the effect.
Patient Story: “I noticed every time I went for a long walk, my fingers would swell and turn a bit red. I learned that it was due to blood and fluid pooling in my hands while they hung by my sides. Now, I make a point to wiggle my fingers and raise my arms above my head occasionally during walks. It’s made a big difference!” – Jane, 34
To combat positional pooling, consider incorporating periodic positional changes into your daily routine. If you work at a desk, ensure your wrists remain in a neutral, slightly elevated position relative to your elbows. Using ergonomic supports can prevent chronic low-grade venous stasis that might otherwise accumulate over an 8-hour workday.
2. Warm Weather and Exercise (Vasodilation)
When you’re hot or exercising, your blood vessels widen (dilate) in a process called vasodilation to release heat and cool your body. This increased blood flow near the skin can make your hands appear flushed and slightly swollen. This is generally harmless and resolves after you cool down. The body's thermoregulatory center in the hypothalamus triggers cutaneous vasodilation, shunting blood away from the core toward the extremities to facilitate heat dissipation through radiation and convection.
To minimize hand swelling during exercise, try periodically extending your arms overhead and opening and closing your fists. Staying hydrated and doing a proper cool-down also helps.[^1] Hydration maintains optimal blood viscosity; when you are dehydrated, blood becomes thicker and more resistant to flow, paradoxically worsening venous stasis despite lower total blood volume. Conversely, overhydration without adequate electrolyte balance can lead to dilutional hyponatremia, which may exacerbate peripheral swelling. Electrolytes like sodium and potassium are essential for maintaining proper vascular tone and cellular fluid exchange.
Additionally, cooling strategies like splashing cool water on the wrists or using a damp cloth around the neck can trigger reflexive vasoconstriction, rapidly reducing hand swelling. Athletes in endurance sports like marathon running or cycling frequently experience this "exercise-induced hand edema," which typically peaks mid-race and resolves within a few hours post-activity.
3. Aging and Vein Elasticity
As we age, our blood vessels lose elasticity, and the valves in our veins can weaken. This can make veins in the hands more prominent and appear to "pool" with blood when hands are held down. Usually, this is a normal sign of aging and not dangerous, as long as it isn't painful. Collagen and elastin production naturally decline after age 40, causing the tunica media and tunica adventitia layers of the venous walls to thin. Subcutaneous fat loss in the dorsal hands further unmasks these superficial vessels, creating the visual impression of pooling even when venous pressure is normal.
However, if hand veins become painful, very swollen, or hard, it could indicate an issue like superficial thrombophlebitis (a blood clot in a surface vein) and should be checked by a healthcare provider. Aging also coincides with changes in endothelial function, reducing nitric oxide bioavailability and impairing the vein's ability to dynamically adjust its diameter. Maintaining skin health with adequate sun protection and moisturization won't prevent venous changes but can improve overall hand comfort and mask minor discoloration.
4. Poor Circulation and Venous Insufficiency
"Poor circulation" is a general term for when blood flow to the extremities is suboptimal. A more specific condition is Chronic Venous Insufficiency (CVI), where weakened or damaged vein valves struggle to send blood back to the heart. While more common in the legs, CVI can sometimes affect the arms. Secondary upper extremity CVI is often linked to prior trauma, repeated heavy lifting, or prior venous catheterization that may have damaged valve leaflets. When valves become incompetent, blood regurgitates backward (reflux), creating a vicious cycle of venous hypertension and capillary leak.
Maintaining good cardiovascular health through regular exercise and not smoking can improve overall circulation.[^2] Vascular conditioning enhances endothelial shear stress, which upregulates anti-inflammatory and anti-thrombotic pathways. For individuals with mild upper extremity venous insufficiency, targeted resistance training can hypertrophy the surrounding musculature, providing external support to venous walls and improving the efficiency of the skeletal muscle pump.
Expert Insight: “The circulatory system works against gravity to return blood to the heart. When circulation is sluggish or veins aren’t functioning perfectly, you might notice blood pooling in extremities. Simple lifestyle changes like staying active and elevating the hands can often alleviate mild symptoms. However, persistent or painful swelling should be evaluated.” – Dr. Maria Gonzalez, MD, Vascular Medicine Specialist
In clinical practice, venous duplex ultrasound is the gold standard for quantifying reflux time and valve competence. If CVI is confirmed in the arms, compression therapy and lifestyle modification remain first-line, though surgical interventions like valve repair or venous ablation are rarely required for the upper extremities compared to the lower legs.
5. Postural Orthostatic Tachycardia Syndrome (POTS)
POTS is a disorder of the autonomic nervous system where blood pools in the lower body upon standing, causing a rapid heart rate and dizziness. While it primarily affects the legs, the pooling can affect the hands too, causing them to turn red or purple when hanging down. The autonomic nervous system normally coordinates vasoconstriction and heart rate adjustments to maintain cerebral perfusion during positional changes. In POTS, this feedback loop is impaired, leading to excessive peripheral blood pooling and compensatory tachycardia.
If you experience these symptoms along with palpitations or fainting spells, it’s important to see a doctor.[^3] Many individuals with POTS also experience acrocyanosis, a benign but noticeable condition where the hands and feet adopt a persistent bluish-red hue due to dysregulated cutaneous blood flow. Management typically focuses on increasing blood volume (through high fluid and sodium intake, as medically advised), wearing graduated compression garments, and utilizing specialized exercise protocols like the Levine or CHOP programs that prioritize recumbent cardio to avoid orthostatic stress during initial conditioning.
*"What is POTS?" – An informational video from Dysautonomia International.*6. Raynaud’s Phenomenon
If your fingers turn white or blue in the cold, then turn red and swell as they warm up, you might have Raynaud’s phenomenon. This condition involves spasms in small blood vessels that limit blood flow. When blood rushes back in, it can cause redness, tingling, and a sensation of pooling. Raynaud’s is often managed by protecting hands from cold, but in severe cases, medication may be necessary.[^4] Primary Raynaud's is idiopathic and generally benign, while secondary Raynaud's can be associated with connective tissue diseases like scleroderma, lupus, or rheumatoid arthritis.
 , followed by a rush of blood causing redness and swelling as they warm up (right).")
, followed by a rush of blood causing redness and swelling as they warm up (right).")
During the reactive hyperemia phase of Raynaud's, the sudden return of blood flow to previously ischemic tissues can feel like intense throbbing or burning, often mistaken for infection or inflammatory arthritis. Keeping a symptom diary noting triggers, duration, and color changes can help clinicians differentiate between primary vascular dysregulation and autoimmune-driven vasculopathy. In refractory cases, topical nitrates or systemic calcium channel blockers may be prescribed to blunt the exaggerated vasoconstrictive response.
7. Other Medical Conditions and Factors
- Injury and Bruising (Hematoma): An injury can cause blood to pool under the skin, forming a bruise (hematoma). Trauma disrupts capillary integrity, allowing whole blood to extravasate into subcutaneous spaces. Initial management follows RICE principles (Rest, Ice, Compression, Elevation), with ice applied for 15-minute intervals during the first 48 hours to limit hematoma expansion.
- Blood Clots in the Arm: Though rare, a clot in an arm vein (deep vein thrombosis or DVT) can cause sudden, significant swelling, redness, and pain in one arm. This is a medical emergency. Upper extremity DVT often relates to repetitive overhead motion (effort thrombosis or Paget-Schroetter syndrome), central venous catheters, or underlying hypercoagulable states. Prompt anticoagulation is critical to prevent pulmonary embolism.
- Heart or Kidney Conditions: Heart failure or kidney disease can cause systemic fluid retention (edema), which can lead to swelling in the hands. Reduced cardiac output activates the renin-angiotensin-aldosterone system (RAAS), promoting sodium and water retention. Diuretics, dietary sodium restriction, and targeted management of the underlying organ dysfunction typically resolve the peripheral swelling.
- Medications: Some drugs, like certain blood pressure medications, can cause swelling in the hands and feet as a side effect. Calcium channel blockers (e.g., amlodipine), NSAIDs, corticosteroids, and certain diabetes medications (thiazolidinediones) are common culprits. Drug-induced edema is usually dose-dependent and often resolves with dosage adjustment or medication substitution under medical supervision.
- Hormonal Fluctuations: Estrogen and progesterone significantly influence vascular permeability and sodium retention. Many women experience cyclical hand swelling during the luteal phase of the menstrual cycle, pregnancy, or perimenopause. Progesterone promotes smooth muscle relaxation in venous walls, while elevated estrogen increases capillary permeability. These changes are physiologic and typically resolve postpartum or post-menopause.
Symptoms of Blood Pooling in the Hands
Common signs and symptoms include:
- Redness or Discoloration: Hands may look red, bluish, or purple. The exact hue depends on the oxygenation level of the pooled blood and skin tone.
- Swelling: Fingers or the entire hand may appear puffy. Swelling is often symmetric if related to systemic or positional causes, but asymmetric if vascular or traumatic.
- Visible Veins: Veins on the back of the hand may bulge. Prominent dorsal veins are often mistaken for pathology but are frequently a normal variant, especially in individuals with low body fat.
- Warmth or Throbbing: The hands may feel warm or have a pulsing sensation. Increased cutaneous blood flow elevates local skin temperature.
- Tingling or Numbness: Swelling can sometimes press on nerves. Transient compression of the median or ulnar nerves due to fluid accumulation can cause paresthesias, mimicking mild carpal tunnel symptoms.
- Heaviness: A feeling of fullness or tightness in the hands. Patients frequently report difficulty making a tight fist or removing rings during episodes of pooling.
Most of these symptoms are temporary and resolve with movement or a change in position. Tracking symptom onset, duration, and associated activities can be invaluable during clinical evaluations, helping to distinguish benign positional pooling from progressive vascular or systemic disease.
When Is Blood Pooling in the Hands a Concern?
While often harmless, certain red flags warrant medical evaluation:
- One-Handed Swelling: Sudden, painful swelling in just one hand could signal a blood clot, infection, or injury. Unilateral symptoms always require prompt vascular assessment to rule out thrombotic or compressive etiologies.
- Sudden Onset with Pain: Rapid, painful swelling could indicate a serious vascular issue. Acute venous occlusion or arterial compromise demands immediate imaging.
- Chronic Symptoms: If you regularly experience pooling without an obvious trigger, it may point to an underlying health problem. Persistent venous hypertension can eventually lead to skin changes like hyperpigmentation or lipodermatosclerosis, even in the upper extremities.
- Accompanying Systemic Symptoms: If hand swelling occurs with fatigue, fainting, chest pain, or shortness of breath, seek medical advice immediately. These systemic red flags suggest cardiopulmonary compromise, severe autonomic dysfunction, or widespread inflammatory processes.
Additionally, monitor for functional impairment. If swelling consistently limits your ability to perform fine motor tasks, type, or grasp objects comfortably, a clinical evaluation is warranted to assess for structural compression or chronic venous pathology. Family history of clotting disorders, autoimmune conditions, or early-onset varicose veins should also prompt earlier screening.
How is the Cause of Hand Blood Pooling Diagnosed?
A healthcare provider will likely:
- Take a Medical History: Ask about your symptoms, lifestyle, and medical conditions. Clinicians will inquire about occupational exposures, exercise habits, medication lists, hormonal status, and any family history of vascular or autoimmune disease.
- Perform a Physical Exam: Check your hands and arms for color, temperature, swelling, and pulses. The physician will assess for pitting vs. non-pitting edema, palpate venous cords, perform capillary refill tests, and listen for arterial bruits. Specific maneuvers like the Allen test may assess collateral circulation if arterial compromise is suspected.
- Order Tests (if needed):
- Doppler Ultrasound: Uses sound waves to check for blood clots or blockages. Venous duplex imaging maps flow direction and velocity, quantifying valvular reflux and ruling out deep or superficial thrombosis.
- Blood Tests: To check for inflammation, clotting disorders, or conditions like diabetes. Panels often include CBC, metabolic panel, D-dimer, ANA, rheumatoid factor, thyroid function tests, and hemoglobin A1c to screen for underlying systemic contributors.
- Tilt Table Test: To diagnose POTS if you experience dizziness upon standing. The patient is secured to a motorized table that tilts to a 70-degree angle while continuous ECG and blood pressure monitoring track autonomic responses.
 uses sound waves to create images of blood flow, helping diagnose conditions like blood clots that can cause blood pooling.")
uses sound waves to create images of blood flow, helping diagnose conditions like blood clots that can cause blood pooling.")
In complex cases, advanced imaging like CT venography or MR angiography may be ordered to visualize thoracic outlet anatomy or identify subtle extrinsic compressions on the subclavian or axillary veins. Referral to a vascular specialist, rheumatologist, or neurologist (for dysautonomia) is guided by initial test results and symptom patterns.
Treatment and Management of Blood Pooling in Hands
Treatment depends on the underlying cause. A stepwise approach typically begins with conservative lifestyle and ergonomic modifications before progressing to pharmacological or procedural interventions if indicated.
A. Home Care and Lifestyle Tips
For mild, occasional pooling:
- Move Your Muscles: Swing your arms, rotate your wrists, or open and close your fists to activate the muscle pump. Frequent micro-breaks of 2-3 minutes every 30-60 minutes during sedentary work can prevent cumulative venous stasis.
- Elevate Your Hands: Raise your hands above heart level for a few minutes to let gravity help drain the blood. Positioning hands on pillows while sleeping or resting can significantly reduce overnight fluid accumulation.
- Stay Hydrated: Drinking enough water helps maintain healthy blood volume and circulation. Aim for pale yellow urine as a hydration marker, adjusting intake for activity level and climate.
- Massage and Stretching: Gently massage your hands and arms toward your heart to encourage blood flow. Use effleurage strokes (light, sweeping pressure) starting at the fingertips and moving proximally to assist lymphatic and venous return without causing capillary trauma.
- Temperature Contrast Therapy: Alternating warm and cool water immersion can train vascular smooth muscle responsiveness and improve endothelial function. A common protocol involves 3 minutes of warm water followed by 1 minute of cool water, repeated 3-5 times.
B. Medical Treatments
If an underlying condition is the cause:
- Medication: For POTS, medications like fludrocortisone or midodrine may be prescribed. For Raynaud's, calcium channel blockers can help. For blood clots, anticoagulants (blood thinners) are used.* Emerging therapies include beta-blockers to control tachycardia, serotonin norepinephrine reuptake inhibitors (SNRIs) for neuropathic pain in autonomic disorders, and topical vasodilators for localized Raynaud's attacks. All pharmacological interventions require careful titration and monitoring for side effects like fluid retention, hypotension, or rebound symptoms.
- Physical Therapy: Specific exercises can improve blood and lymph flow. Therapists may utilize myofascial release, manual lymphatic drainage techniques, and graded compression therapy. For effort thrombosis or thoracic outlet syndrome, targeted stretching of the pectoralis minor and scalene muscles can relieve anatomical compression.
- Treatment for Systemic Issues: Managing conditions like heart or kidney disease will help reduce associated swelling. This may involve diuretic optimization, dietary modifications, and specialist co-management. In autoimmune-related vascular dysfunction, disease-modifying antirheumatic drugs (DMARDs) or biologic agents may be necessary to halt progressive endothelial damage.
Preventing Blood Pooling in the Hands
- Stay Active: Aim for at least 150 minutes of moderate exercise per week to improve overall circulation.[^2] Incorporate both aerobic conditioning and resistance training to enhance cardiovascular efficiency and venous return mechanics.
- Incorporate Upper Body Movements: During walks or runs, consciously move your arms. Avoid holding heavy weights or keeping arms completely static for prolonged durations.
- Avoid Extreme Temperatures: Keep hands warm in cold weather and stay cool in hot weather. Wear insulated gloves in freezing conditions to prevent vasospasm, and use breathable, moisture-wicking fabrics during summer to avoid excessive vasodilation.
- Don’t Smoke: Smoking damages blood vessels and impairs circulation. Nicotine causes acute vasoconstriction, while chronic exposure accelerates arterial stiffness and endothelial dysfunction, severely compromising microcirculatory reserve.
- Maintain a Healthy Diet and Hydration: A balanced diet and adequate water intake support vascular health. Emphasize foods rich in nitric oxide precursors (leafy greens, beets), flavonoids (berries, citrus, dark chocolate), and omega-3 fatty acids, which have anti-inflammatory and vasoprotective properties. Limit excessive sodium and alcohol, both of which can exacerbate peripheral fluid retention.
- Optimize Ergonomics and Gear: Ensure workstations are set up to keep wrists in neutral alignment. Avoid excessively tight watches, jewelry, or sleeves that can act as tourniquets during prolonged activity. When flying or traveling, consider wearing light compression sleeves designed for the upper extremity to counteract cabin pressure changes and immobility.
Simple Hand Exercise for Better Circulation:
- Hand Elevation and Fist Pumping: Raise your arms above your head. Open and close your fists 10-15 times.
- Wrist Rotations: Extend your arms and rotate your wrists in circles, 10 times in each direction.
- Finger Stretch and Flex: Spread your fingers wide, hold for a few seconds, then relax. Repeat 10 times.
- Prayer and Reverse Prayer Stretch: Press palms together in front of chest, lower slowly. Then press backs of hands together and raise slightly. Hold each for 15 seconds to stretch forearm flexors and extensors, releasing potential fascial restrictions.
- Tendon Glides: Start with fingers straight, make a full fist, then transition to a hook fist, and finally a straight fist. Repeat 5-10 times to mobilize flexor tendons and stimulate venous sinus drainage in the forearm.
Frequently Asked Questions
Can wearing compression gloves help with hand blood pooling?
Yes, lightweight graduated compression gloves can be beneficial for many individuals. They apply gentle external pressure that supports venous return and reduces capillary fluid leakage without restricting arterial inflow. Look for gloves offering 15-20 mmHg of compression, which is considered mild to moderate and suitable for daily wear. They are particularly helpful during air travel, long drives, or for people with mild Raynaud’s or POTS-related pooling. However, they should not be worn if you have severe peripheral arterial disease, active infection, or open wounds. Always consult a healthcare provider if you have an underlying vascular condition before starting compression therapy.
Why do my hands pool blood more after eating a high-sodium meal?
High sodium intake triggers the kidneys to retain water to maintain osmotic balance, leading to increased extracellular fluid volume and expanded blood plasma volume. This temporary hypervolemia increases hydrostatic pressure within the peripheral capillary beds, making fluid more likely to leak into surrounding tissues and venous blood to pool, especially in gravity-dependent areas like the hands. The effect is usually noticeable within a few hours of a salty meal and typically resolves within 24 hours as the kidneys excrete the excess sodium and water. Reducing processed foods, reading nutrition labels for hidden sodium, and increasing potassium-rich foods can help mitigate this response.
Is blood pooling in the hands linked to arthritis?
Blood pooling itself does not cause arthritis, but inflammatory arthritis (like rheumatoid arthritis or psoriatic arthritis) can cause hand swelling that mimics or exacerbates venous pooling. Chronic synovial inflammation increases local blood flow and vascular permeability, leading to persistent puffiness and warmth. Additionally, joint deformities or muscle weakness from arthritis can reduce the effectiveness of the skeletal muscle pump in the hands and wrists, indirectly worsening venous stasis. Conversely, vascular conditions like vasculitis can present with joint pain and skin discoloration, making accurate diagnosis crucial. If you have arthritis and notice new or worsening hand discoloration, discuss it with your rheumatologist to rule out overlapping vascular issues or medication side effects.
How long does it take for pooled blood to drain when I elevate my hands?
In healthy individuals, raising the hands above heart level typically initiates noticeable improvement within 5 to 10 minutes. The exact timeframe depends on several factors, including baseline venous pressure, degree of vasodilation, hydration status, and whether there is concurrent interstitial edema. Venous blood drains relatively quickly once gravity is reversed, but interstitial fluid takes longer to re-enter the capillaries and lymphatics. For optimal results, combine elevation with gentle finger movements and deep breathing. If elevation for 30 minutes yields no improvement, or if swelling worsens, seek medical evaluation to rule out obstructive or systemic causes.
Can stress or anxiety cause my hands to feel swollen and red?
Absolutely. Stress activates the sympathetic nervous system and triggers the release of catecholamines like adrenaline and cortisol, which profoundly affect vascular tone and fluid balance. Acute stress can cause peripheral vasoconstriction followed by reactive vasodilation once the stressor passes, leading to a warm, flushed, or "swollen" sensation. Chronic anxiety may also alter breathing patterns (leading to hyperventilation and changes in blood pH) and promote muscle tension that restricts lymphatic and venous return in the neck and shoulders, indirectly impairing upper extremity drainage. Stress-induced symptoms often improve with relaxation techniques like diaphragmatic breathing, progressive muscle relaxation, or mindfulness meditation. If anxiety-related symptoms significantly impact daily life, cognitive behavioral therapy (CBT) and medical evaluation for autonomic dysfunction may be warranted.
Conclusion
Blood pooling in the hands is often a benign response to gravity, heat, or exercise. Simple adjustments like moving your muscles or changing your posture can resolve it. However, persistent or severe symptoms can be a sign of a more serious issue, such as POTS, Raynaud’s phenomenon, or even a blood clot.
By staying active, hydrated, and mindful of your posture, you can manage and prevent most cases of mild blood pooling. If you are ever concerned about your symptoms, don't hesitate to speak with a healthcare professional for a proper diagnosis and treatment plan. Early evaluation ensures that any underlying vascular, neurological, or systemic conditions are addressed promptly, preserving both function and long-term circulatory health.
Helpful Resources & Further Reading
- Mayo Clinic – Raynaud’s Disease: A detailed overview of Raynaud’s phenomenon, its causes, symptoms, and treatments.
- Cleveland Clinic – Poor Circulation: An easy-to-understand guide on causes and symptoms of poor circulation.
- Johns Hopkins Medicine – Thoracic Outlet Syndrome: Information about a condition that can compress blood vessels and cause arm DVT.
- American Heart Association – Warm-Up, Cool-Down: Expert advice on the importance of cooling down to help circulation after exercise.
- NHS – Oedema (Edema): An overview of swelling and its causes from the UK National Health Service.
(Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice. If you have concerns about your health, please seek advice from a licensed healthcare provider.)
References:
[^1]: Mayo Clinic Staff. (2022). Aerobic exercise: How to warm up and cool down. MayoClinic.org [^2]: American Heart Association. (2021). American Heart Association Recommendations for Physical Activity in Adults and Kids. heart.org [^3]: Dysautonomia International. (2021). What is POTS?. DysautonomiaInternational.org [^4]: National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS). (2020). Raynaud’s Phenomenon. NIAMS Health Topics
[*] National Blood Clot Alliance. (n.d.). Upper Extremity Deep Vein Thrombosis. Cleveland Clinic

About the author
Marcus Thorne, MD, is a board-certified interventional cardiologist and a fellow of the American College of Cardiology. He serves as the Chief of Cardiology at a major metropolitan hospital in Chicago, specializing in minimally invasive cardiac procedures.