Why You Have Acne on Your Jawline (And How to Finally Treat It)

Key points
- Menstrual Cycles: Many women experience flare-ups in the week before their period as hormone levels shift. Specifically, during the luteal phase, progesterone rises and then plummets alongside estrogen just before menstruation. This sudden drop removes estrogen's natural calming effect on sebum production, allowing androgens to temporarily dominate the hormonal landscape and trigger breakouts.
- Polycystic Ovary Syndrome (PCOS): This endocrine condition often involves higher levels of androgens, making persistent acne a common symptom, according to research on hormonal acne treatments. Women with PCOS may also experience irregular ovulation, weight changes, and hirsutism alongside recalcitrant jawline acne.
- Pregnancy and Menopause: Major hormonal shifts during these life stages can trigger or worsen acne. Pregnancy introduces surges in progesterone and estrogen, while menopause is characterized by declining estrogen levels, which can unmask relative androgen excess and lead to late-onset adult acne.
- Starting or Stopping Birth Control: Changes in hormonal medication can temporarily disrupt your body's balance, leading to breakouts. It typically takes 3 to 6 months for the endocrine system to recalibrate after initiating or discontinuing oral contraceptives.
Acne along the jawline can be one of the most stubborn and frustrating skin concerns. Unlike scattered pimples that come and go, jawline breakouts often feel deep, painful, and cyclical, reappearing in the same spots month after month. This pattern isn't a coincidence; it’s a strong clue about the underlying causes.
While all acne involves clogged pores, oil, and bacteria, breakouts on the lower third of the face are frequently tied to internal factors, primarily your hormones. Understanding these triggers is the first step toward finding a treatment that finally clears your skin for good. The lower face and jawline possess a uniquely high density of androgen-sensitive sebaceous glands, which means this specific facial zone reacts more intensely to internal biochemical shifts than other areas like the cheeks or forehead. Furthermore, jawline acne often presents as inflammatory papules, nodules, or deep cysts because the follicular openings in this region are narrower and more prone to becoming trapped beneath the skin surface, leading to increased pressure, pain, and a higher risk of permanent scarring if mismanaged.
What Causes Acne on the Jawline?
Jawline acne develops when hair follicles become clogged with excess oil (sebum) and dead skin cells, creating an environment for bacteria to thrive. However, several specific factors make the jawline particularly prone to these breakouts. The pathophysiology of jawline acne revolves around a process known as follicular hyperkeratinization, where the skin cells lining the hair follicle shed abnormally and stick together instead of shedding naturally. When combined with sebum overproduction and colonization by Cutibacterium acnes (formerly P. acnes), this creates the perfect storm for comedone formation, inflammation, and visible lesions.
The Primary Culprit: Hormonal Fluctuations
If you notice your jawline acne flares up cyclically, hormones are the most likely cause. This is so common that dermatologists often refer to this pattern as the "beard of acne" in women.
The main driver is a group of hormones called androgens, such as testosterone. While considered male hormones, they are present in everyone. An increase in androgens—or even a shift in the ratio of androgens to other hormones like estrogen—can send your oil glands into overdrive. This excess oil is what leads to clogged pores. At the cellular level, androgens bind to receptors within the sebaceous glands, triggering increased lipid synthesis. The enzyme 5-alpha-reductase converts testosterone into dihydrotestosterone (DHT), a much more potent androgen that dramatically stimulates sebum production and thickens follicular walls. When sebum oxidizes upon exposure to air, it can further irritate the surrounding tissue and promote an inflammatory immune response.
This hormonal link explains why jawline acne is common during:
- Menstrual Cycles: Many women experience flare-ups in the week before their period as hormone levels shift. Specifically, during the luteal phase, progesterone rises and then plummets alongside estrogen just before menstruation. This sudden drop removes estrogen's natural calming effect on sebum production, allowing androgens to temporarily dominate the hormonal landscape and trigger breakouts.
- Polycystic Ovary Syndrome (PCOS): This endocrine condition often involves higher levels of androgens, making persistent acne a common symptom, according to research on hormonal acne treatments. Women with PCOS may also experience irregular ovulation, weight changes, and hirsutism alongside recalcitrant jawline acne.
- Pregnancy and Menopause: Major hormonal shifts during these life stages can trigger or worsen acne. Pregnancy introduces surges in progesterone and estrogen, while menopause is characterized by declining estrogen levels, which can unmask relative androgen excess and lead to late-onset adult acne.
- Starting or Stopping Birth Control: Changes in hormonal medication can temporarily disrupt your body's balance, leading to breakouts. It typically takes 3 to 6 months for the endocrine system to recalibrate after initiating or discontinuing oral contraceptives.
!A woman touching her jawline, where acne commonly appears due to hormonal changes.:max_bytes(150000):strip_icc()/GettyImages-1493956084-529be22b44fe4d508300fa9c56a3ee1c.jpg) Image Source: Cleveland Clinic
Lifestyle and Environmental Factors
While hormones set the stage, your daily habits can contribute to the problem. External irritants and behavioral patterns frequently compound internal triggers, turning mild congestion into full-blown inflammatory lesions. The skin barrier plays a crucial role here; when compromised, it allows environmental aggressors to penetrate more easily and disrupts the natural shedding process, accelerating clog formation.
- Stress: When you're stressed, your body releases cortisol, which can increase inflammation and oil production, worsening breakouts. Chronic stress elevates corticotropin-releasing hormone (CRH), which directly stimulates sebocytes to produce more lipids and inflammatory cytokines, creating a vicious cycle of stress-induced breakouts and acne-related anxiety.
- Friction and Pressure (Acne Mechanica): Anything that repeatedly rubs against your jaw can trap sweat, oil, and bacteria, leading to irritation and pimples. Common culprits include chin straps on helmets, violin placement, tight collars, and even resting your chin on your hands. The recent prevalence of prolonged mask-wearing has also introduced "maskne" (acne mechanica) to the lower face, where humidity, friction, and trapped exhaled air create a microenvironment that promotes bacterial overgrowth and follicular occlusion.
- Skincare and Hair Products: Thick, oily, or heavily fragranced products can clog pores. Look for products labeled "non-comedogenic," which means they are formulated to not block pores. Hair styling products containing heavy silicones, petroleum derivatives, or coconut oil can migrate to the jawline and cause pomade acne. Similarly, failing to properly remove sunscreen and makeup at the end of the day leaves a film of occlusive agents and oxidized lipids on the skin.
- Medications: Certain drugs, including corticosteroids, lithium, and some anticonvulsants, can list acne as a side effect. Anabolic steroids and high-dose B vitamins (particularly B12) have also been clinically documented to trigger sudden, severe acne flares by altering follicular cell metabolism and microbial populations.
The Diet-Acne Connection: What the Science Says
For years, the link between diet and acne was debated, but a growing body of research suggests a connection. While food isn't a direct cause for everyone, it can be a significant trigger for some. Nutritional dermatology has increasingly recognized that systemic inflammation and glycemic load profoundly influence skin homeostasis.
- High-Glycemic Foods: Diets high in sugar and refined carbohydrates (like white bread, pastries, and soda) can spike blood sugar and insulin levels. This hormonal surge can increase oil production and inflammation. Studies have shown that a low-glycemic diet can lead to fewer breakouts for some people. High insulin levels stimulate the insulin-like growth factor 1 (IGF-1) pathway, which enhances keratinocyte proliferation and androgen signaling, directly worsening follicular clogging.
- Dairy: Some research has found a correlation between milk consumption, especially skim milk, and acne. This may be due to hormones and growth factors in milk that can influence your own hormonal balance. Even in the absence of added hormones, bovine milk contains natural whey and casein proteins that can elevate insulin and IGF-1 levels. Fermented dairy products like yogurt and aged cheeses appear to have a lower acneogenic potential due to their probiotic content and reduced lactose concentration.
It's important to remember that diet is a highly individual factor. If you suspect a food is triggering your acne, consider eliminating it for a few weeks to see if your skin improves. Incorporating anti-inflammatory nutrients, such as omega-3 fatty acids (found in salmon, walnuts, and flaxseeds), zinc, and antioxidant-rich vegetables, can help modulate systemic inflammation and support skin barrier integrity. Emerging research also highlights the gut-skin axis, suggesting that maintaining a diverse gut microbiome through fiber-rich foods and fermented products may indirectly improve inflammatory skin conditions by reducing intestinal permeability and systemic cytokine release.
Jawline Acne in Men: Distinct Causes and Solutions
While hormonal influences affect men too, jawline acne in men is often tied to specific grooming and lifestyle habits. Men typically have larger sebaceous glands and higher baseline sebum production due to naturally elevated testosterone levels, making them more susceptible to comedonal and inflammatory acne in the beard region. The physical act of hair removal, combined with thicker, coarser terminal hairs, introduces unique dermatological challenges that differ significantly from female-pattern hormonal acne.
- Shaving: This is a major trigger. Dull razor blades can drag bacteria across the skin, and improper technique can lead to irritation and ingrown hairs that become inflamed and look like acne cysts. Shaving against the grain, using alcohol-heavy aftershaves, or applying excessive pressure compromises the stratum corneum, leading to micro-tears and subsequent bacterial entry.
- Folliculitis: Sometimes, what appears to be acne is actually folliculitis—an infection of the hair follicle. This is common in the beard area and can be caused by bacteria or ingrown hairs. Pseudofolliculitis barbae occurs when sharply cut beard hairs curl back into the skin, provoking a foreign-body inflammatory response that mimics pustular acne but requires different management strategies.
- Friction: Just like in women, chin straps from helmets or athletic gear can cause acne mechanica. Additionally, frequent beard grooming, heavy balms, and waxes can create occlusive layers that trap dead skin and bacteria.
To combat this, men should focus on a clean shaving routine: use a sharp, single- or double-blade razor, shave in the direction of hair growth, and use a gentle, non-comedogenic shaving cream. Pre-softening the beard with warm water and a hydrating shave gel reduces friction, while post-shave application of a soothing, alcohol-free product containing ingredients like aloe vera, centella asiatica, or niacinamide can calm inflammation and reinforce the skin barrier. For those with chronic razor bumps or recurrent folliculitis, switching to an electric trimmer that leaves a slight hair stubble can dramatically reduce ingrown hairs and pseudofolliculitis barbae. Regular chemical exfoliation with salicylic acid or glycolic acid (applied at least 6-8 hours after shaving to avoid severe irritation) can also keep follicles clear and promote healthy hair growth.
Effective Treatments for Jawline Acne
Because jawline acne has multiple causes, a combination of treatments is often most effective. Addressing the underlying hormonal drivers while simultaneously managing surface inflammation, bacterial colonization, and barrier function yields the most sustainable results. Treatment success heavily depends on patient adherence, realistic expectations, and proper product application techniques.
Over-the-Counter (OTC) Solutions
For mild to moderate acne, start with accessible OTC ingredients. Consistency is paramount; most active ingredients require 6 to 12 weeks of uninterrupted use to demonstrate meaningful clinical improvement, as skin cell turnover naturally takes approximately 28 days in younger adults and lengthens with age.
- Benzoyl Peroxide: Kills acne-causing bacteria and helps unclog pores. It's available in cleansers and spot treatments. Benzoyl peroxide works by releasing free radical oxygen into the follicle, creating an aerobic environment that C. acnes cannot survive. It also exhibits mild keratolytic properties that help shed clogged cells. Start with a 2.5% or 5% concentration, as studies show it is equally effective as 10% formulations but significantly less irritating. Be cautious with fabric bleaching; it can permanently lighten towels, pillowcases, and colored clothing.
- Salicylic Acid: An exfoliant that dissolves oil and dead skin cells inside the pore to prevent clogs. As a beta-hydroxy acid (BHA), salicylic acid is lipid-soluble, allowing it to penetrate deep into sebum-filled pores where water-soluble acids cannot reach. It also possesses inherent anti-inflammatory properties that can soothe existing red, swollen lesions. It is best used in leave-on toners or serums 2-3 times weekly, gradually increasing frequency as tolerance builds.
- Adapalene (e.g., Differin Gel): A topical retinoid that regulates skin cell turnover to prevent pores from becoming blocked. It was previously prescription-only but is now available OTC. Adapalene binds specifically to retinoic acid receptors (RAR-beta and RAR-gamma), normalizing desquamation and reducing the formation of microcomedones. Initial use often causes a "retinization" phase characterized by dryness, peeling, and sometimes a temporary acne flare (purging) as deeply trapped congestion rapidly surfaces to the epidermis. This typically resolves within 4-8 weeks. To minimize irritation, apply a pea-sized amount to the entire face (not just spots) on dry skin, using the "sandwich method" (moisturizer-adapalene-moisturizer) if sensitivity occurs.
Prescription Medications and Treatments
If OTC products aren't enough after several weeks, a dermatologist can offer stronger options tailored to hormonal acne. Prescription regimens are typically customized based on acne severity, lesion type, patient sex, contraindications, and reproductive plans.
- Topical Treatments: Prescription-strength retinoids (like Tretinoin), topical antibiotics, and dapsone gel can reduce inflammation and prevent new breakouts. Tretinoin (all-trans retinoic acid) is more potent than adapalene and highly effective for comedonal acne. Combination topicals like clindamycin/benzoyl peroxide or adapalene/benzoyl peroxide offer synergistic antibacterial and comedolytic effects while reducing the risk of antibiotic resistance. Clascoterone (Winlevi) is a newer topical anti-androgen that directly competes with DHT for receptors in sebaceous glands, offering a targeted approach for hormonal breakouts without systemic side effects.
- Oral Medications:
- Antibiotics: Reduce bacteria and inflammation for more widespread or severe acne. Tetracycline-class antibiotics like doxycycline and minocycline are first-line systemic options. They should always be paired with a topical benzoyl peroxide to prevent bacterial resistance, and their use is generally limited to 3-4 months due to microbiome disruption and potential side effects.
- Hormonal Therapies: For women, oral contraceptives (birth control pills) can regulate hormones. Spironolactone, a medication that blocks the effects of androgens on oil glands, is another highly effective option for hormonal acne, as noted by Tufts Medicine. Typically dosed between 25-150 mg daily, spironolactone can take 2-3 months to show noticeable improvement. Common side effects include mild diuresis, menstrual irregularities, and breast tenderness. It is strictly contraindicated during pregnancy due to the risk of feminization of a male fetus.
- Isotretinoin: Reserved for severe, cystic, and scarring acne that hasn't responded to other treatments. This potent oral retinoid shrinks sebaceous glands, dramatically reduces oil production, and normalizes follicular shedding. It requires strict monitoring via the iPLEDGE program (in the US), monthly pregnancy tests for females of reproductive age, and periodic liver function and lipid panels due to potential hepatotoxicity and hypertriglyceridemia.
In-Office Procedures by a Dermatologist
For immediate relief from large, painful cysts and to prevent scarring, a dermatologist may perform:
- Corticosteroid Injections: Injected directly into a large cyst, this can dramatically reduce inflammation and size within 24-48 hours. Intralesional triamcinolone acetonide delivers a targeted anti-inflammatory burst, preventing tissue destruction and subsequent atrophic scarring. Overuse or high concentrations can cause localized hypopigmentation or dermal thinning, so practitioners use highly diluted doses judiciously.
- Chemical Peels: Use acids to exfoliate the skin, unclog pores, and improve skin texture. Medium-depth peels utilizing glycolic, salicylic, or Jessner’s solutions can accelerate desquamation, reduce comedone counts, and improve post-inflammatory erythema. Multiple sessions spaced 3-4 weeks apart are typically recommended for optimal results.
- Light and Laser Therapy: Can help reduce bacteria and inflammation. Blue light (415 nm) targets porphyrins produced by C. acnes, destroying the bacteria via photodynamic action, while red light (630-660 nm) penetrates deeper to modulate inflammatory pathways and promote tissue repair. Fractional non-ablative lasers and microneedling with radiofrequency are increasingly utilized later in the treatment journey to remodel collagen and address existing acne scars.
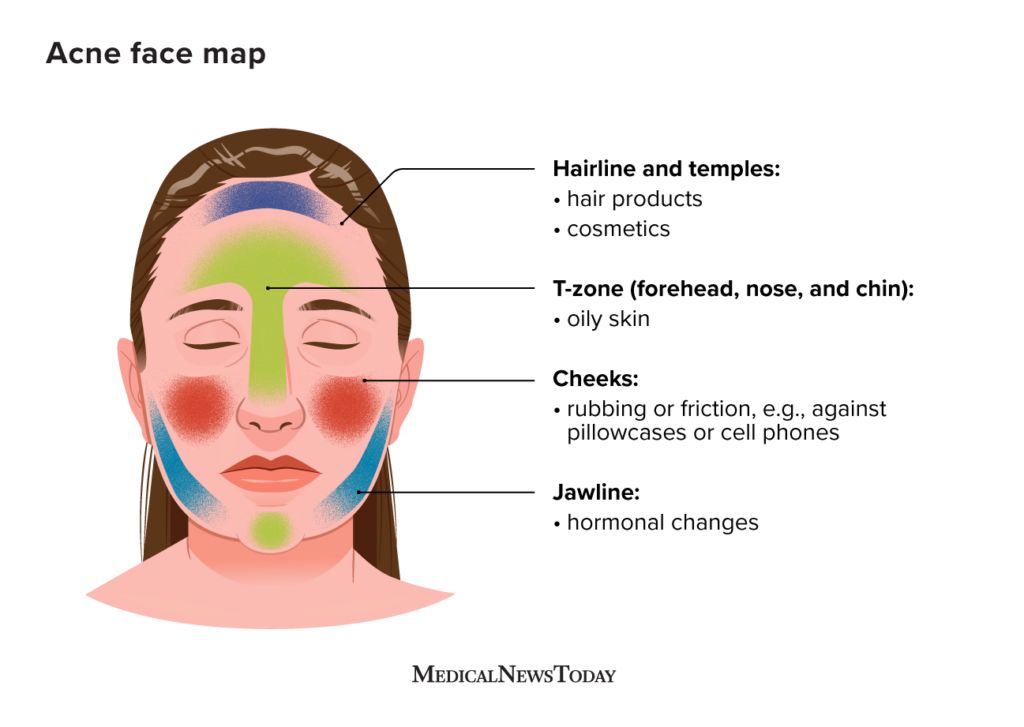 Image Source: Medical News Today
Image Source: Medical News Today
Prevention: How to Keep Your Jawline Clear
Once your acne is under control, consistency is key to preventing its return. Acne management is fundamentally a long-term skin health strategy rather than a short-term spot-treatment endeavor. Maintaining a clear jawline requires a disciplined approach that balances active treatment with barrier preservation. Over-cleansing or aggressive scrubbing strips essential lipids, triggering compensatory sebum overproduction and worsening congestion. Instead, focus on gentle, evidence-based practices that support the skin's natural acid mantle and microbiome equilibrium.
Skincare Routine Essentials
- Cleanse Gently: Wash your face twice a day with a mild, non-abrasive cleanser. Scrubbing too hard can irritate the skin and make acne worse. Opt for pH-balanced, soap-free formulations (pH 4.5-5.5) that remove excess sebum without disrupting the stratum corneum. If you wear heavy makeup or water-resistant sunscreen, consider the double-cleansing method in the evening: first use a balm or micellar water to dissolve lipophilic impurities, followed by your regular gentle cleanser to remove residual sweat and water-soluble debris.
- Use Non-Comedogenic Products: Ensure your moisturizer, sunscreen, and makeup won't clog your pores. Even oily skin requires hydration; look for lightweight, oil-free gels or fluid emulsions containing humectants like glycerin, hyaluronic acid, and squalane, alongside barrier-repairing ingredients like ceramides and panthenol. Daily broad-spectrum SPF 30+ sunscreen is non-negotiable, as UV exposure thickens the skin, promotes post-inflammatory hyperpigmentation (PIH), and degrades active ingredients like retinoids. Mineral sunscreens with zinc oxide offer additional anti-inflammatory benefits.
- Don't Pick: Squeezing pimples can push bacteria deeper into the skin, leading to more inflammation and potential scarring. Manipulating lesions ruptures the follicular wall, spilling inflammatory mediators into the dermis and often transforming a superficial papule into a deep, painful nodule. If extraction is necessary, it should only be performed by a licensed professional using sterile instruments in a controlled clinical setting.
Lifestyle Habits
- Hands Off: Avoid resting your chin in your hands or touching your face unnecessarily. Hands harbor thousands of bacteria, fungi, and environmental pollutants that are directly transferred to facial pores upon contact. Developing a habit of keeping hands away from the jawline significantly reduces mechanical irritation and cross-contamination.
- Keep It Clean: Regularly wipe down your cell phone and wash pillowcases and any gear (like helmet straps) that touches your jaw. Cell phones are notorious vectors for bacterial transmission; disinfect screens daily with 70% isopropyl alcohol wipes and use hands-free or speakerphone functions during calls. Change pillowcases every 2-3 days, opting for breathable, moisture-wicking fabrics like silk or bamboo that generate less friction and harbor fewer microbes compared to traditional cotton.
- Manage Stress: Incorporate stress-reducing activities like exercise, meditation, or getting enough sleep to help keep your hormones in balance. Physical activity improves circulation and insulin sensitivity, while quality sleep (7-9 hours) allows for optimal cortisol regulation and overnight epidermal repair. Mindfulness practices, journaling, or cognitive behavioral therapy (CBT) can also help mitigate the psychological feedback loop where acne causes stress, and stress exacerbates acne.
When to See a Dermatologist
It's time to consult a board-certified dermatologist if:
- Your acne doesn't improve after 6-8 weeks of consistent OTC treatment.
- You have deep, painful cysts or nodules.
- Your acne is leaving scars or dark spots.
- It is causing you significant emotional distress.
- You have other symptoms of a hormonal imbalance, such as irregular periods or excessive hair growth.
A dermatologist can provide an accurate diagnosis and create a personalized treatment plan to help you achieve clear, healthy skin. Professional evaluation is particularly important because many conditions mimic jawline acne, including perioral dermatitis, rosacea, keratosis pilaris, cutaneous lupus, and even rare malignancies like basal cell carcinoma in atypical presentations. A thorough dermatological exam involves assessing lesion morphology, mapping distribution, evaluating skin barrier function, and reviewing complete medical, family, and medication histories.
If hormonal etiology is strongly suspected, your dermatologist may collaborate with an endocrinologist or gynecologist to order targeted laboratory panels. These typically include total and free testosterone, dehydroepiandrosterone sulfate (DHEAS), sex hormone-binding globulin (SHBG), luteinizing hormone (LH), follicle-stimulating hormone (FSH), prolactin, and thyroid function tests (TSH, T3, T4). Identifying conditions like hyperandrogenism, adrenal hyperplasia, or thyroid dysfunction is crucial, as treating the underlying endocrine disorder often resolves the cutaneous manifestations more effectively than topical monotherapy. Early intervention also prevents permanent textural changes such as icepick, rolling, or boxcar scars, which require more invasive and costly resurfacing procedures like fractional laser therapy, subcision, or TCA CROSS once formed.
References
- Medical News Today. (2025). Jawline acne: Causes, treatment and prevention. https://www.medicalnewstoday.com/articles/321218
- Verywell Health. (2025). Why You Have Jawline Acne and What to Do About It. Cleveland Clinic
- Tufts Medicine. (n.d.). Adult Acne at Age 30. https://www.tuftsmedicine.org/about-us/news/adult-acne-age-30
- American Academy of Dermatology Association. (n.d.). Can the right diet get rid of acne? https://www.aad.org/public/diseases/acne/causes/diet
- Gallo, R. L., et al. (2016). Hormonal treatment of acne vulgaris: an update. Clinical, Cosmetic and Investigational Dermatology. https://pmc.ncbi.nlm.nih.gov/articles/PMC5015761/
Frequently Asked Questions
Can jawline acne be permanently cured?
While acne is a chronic condition for many adults rather than an acute illness with a one-time "cure," jawline acne can be effectively controlled to the point of long-term remission with the right combination of treatments. Consistent use of prescription retinoids, hormonal modulators (like spironolactone or specific oral contraceptives), and proper skincare maintenance can keep breakouts at bay for years. Many patients eventually reach a maintenance phase where OTC products and lifestyle adjustments alone are sufficient, though hormonal shifts like pregnancy, menopause, or stopping birth control may require temporary treatment adjustments.
How long does it take for hormonal acne treatments to work?
Hormonal therapies require patience because they work by gradually altering systemic endocrine signaling rather than providing immediate topical effects. Spironolactone typically begins reducing oil production within 2 to 3 weeks, but visible clearing of deep nodules and cysts usually takes 8 to 12 weeks, with maximal improvement occurring around 6 months. Oral contraceptives may initially cause a temporary flare during the first 1-2 months as the body adapts to exogenous hormones, followed by steady improvement by month 4 to 6. Topical retinoids show comedonal improvement in 4-8 weeks but require 3-4 months for significant inflammatory reduction. Stopping treatments prematurely is the most common reason for perceived "treatment failure."
Should I pop deep, painful jawline cysts at home?
Absolutely not. Attempting to pop deep, subcutaneous cysts or nodules is highly likely to rupture the follicular wall beneath the skin's surface. When this occurs, the inflammatory contents—including keratin, sebum, and bacteria—are forced into the deeper dermal tissue, triggering a severe immune response that dramatically increases the risk of permanent atrophic scarring and post-inflammatory hyperpigmentation. Furthermore, home extraction introduces additional bacteria from fingernails and unsterilized tools, potentially causing secondary infections like cellulitis. If a cyst is exceptionally painful or persistent, a dermatologist can safely administer an intralesional corticosteroid injection or perform a sterile incision and drainage in a clinical setting.
Does stress really cause breakouts specifically on the jawline?
Stress does not cause acne in isolation, but it acts as a powerful catalyst and exacerbating factor, particularly in hormonally sensitive areas like the jawline. Psychological stress activates the hypothalamic-pituitary-adrenal (HPA) axis, releasing cortisol and corticotropin-releasing hormone (CRH). CRH receptors are densely concentrated in sebaceous glands; when stimulated, they increase lipid synthesis and promote inflammation. Additionally, stress impairs wound healing and compromises the skin barrier, making it more vulnerable to bacterial colonization and environmental irritants. While stress-induced breakouts can appear anywhere, individuals with pre-existing androgen sensitivity will typically notice them clustering along the jaw, chin, and neck where those hormonal receptors dominate.
Are natural or DIY remedies effective for jawline acne?
Most DIY kitchen remedies (like lemon juice, baking soda scrubs, or undiluted essential oils) lack clinical evidence and can actually damage the skin barrier, worsen inflammation, and trigger contact dermatitis. The skin's natural pH is slightly acidic (~4.5-5.5), and highly alkaline or caustic substances disrupt the acid mantle, stripping protective lipids and allowing harmful microbes to proliferate. However, certain naturally derived, clinically formulated ingredients do show promise in peer-reviewed studies. Tea tree oil (5% concentration) demonstrates mild antimicrobial properties comparable to low-strength benzoyl peroxide, while niacinamide (2-5%) and green tea extract offer anti-inflammatory and sebum-regulating benefits. If you prefer "clean" or botanical-focused products, choose those that are dermatologically tested, properly formulated, and non-comedogenic rather than attempting unsafe home concoctions.
Conclusion
Acne along the jawline is rarely just a superficial skin issue; it is frequently a visible manifestation of internal hormonal fluctuations, genetic predispositions, and environmental influences working in tandem. The cyclical, deep, and often painful nature of lower facial breakouts underscores the importance of looking beyond basic cleansers and understanding the underlying physiological drivers, particularly androgen activity, follicular hyperkeratinization, and systemic inflammation. Effective management requires a multifaceted approach that combines targeted topical actives like benzoyl peroxide, salicylic acid, and retinoids with lifestyle modifications, barrier-supportive skincare, and, when necessary, prescription hormonal therapies or systemic medications.
Patience and consistency remain the cornerstones of successful acne treatment. Because skin cell turnover and hormonal recalibration take time, expecting immediate results often leads to premature discontinuation of effective therapies. By establishing a gentle, non-irritating daily routine, avoiding physical manipulation of lesions, and seeking professional guidance when breakouts persist or scar, you can successfully bring jawline acne under control. Remember that achieving clear skin is a gradual journey rather than an overnight fix, and working collaboratively with a board-certified dermatologist ensures you receive a safe, personalized, and scientifically backed treatment plan tailored to your unique dermatological and hormonal profile.

About the author
Elena Vance, MD, is a double board-certified dermatologist and pediatric dermatologist. She is an assistant professor of dermatology at a leading medical university in California and is renowned for her research in autoimmune skin disorders.