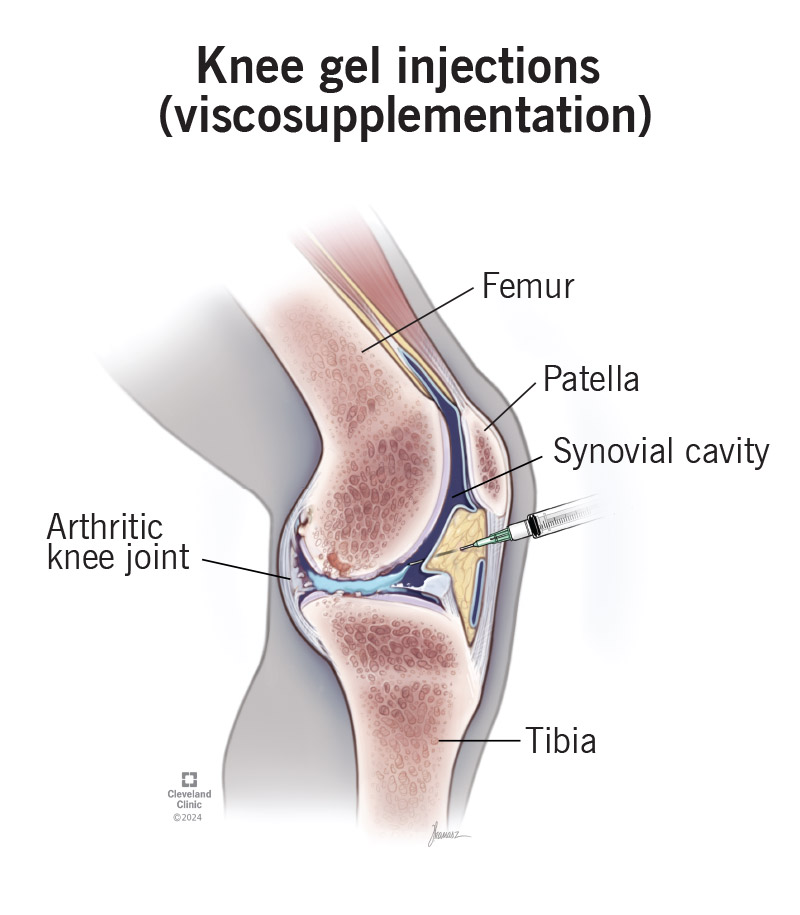
How Much Do Knee Gel Injections Really Cost? A 2025 Guide

Key points
- Per Injection: A single hyaluronic acid injection typically costs between $500 and $1,300 when paying out-of-pocket. This base rate usually encompasses the pharmaceutical product itself, physician administration, and standard facility overhead. However, prices can fluctuate based on the specific molecular weight and cross-linking technology of the HA formulation used. High-viscosity, highly cross-linked formulations generally command premium pricing due to extended manufacturing processes and longer proposed durations of clinical effect.
- Full Treatment Series: Most treatment protocols involve a series of 3 to 5 weekly injections. The total cost for a complete series can range from $1,200 to over $3,000. When multiplied across multiple visits, the financial burden compounds quickly, making it crucial for patients to understand the full economic commitment before initiating therapy. Additionally, each visit often incurs separate professional service charges, co-pays, or facility fees depending on your insurance structure or cash-pay agreement.
Knee gel injections, clinically known as viscosupplementation, are a common treatment for the pain and stiffness caused by knee osteoarthritis. By injecting a gel-like substance called hyaluronic acid (HA) into the knee, this procedure aims to restore the natural lubrication and cushioning of the joint. Hyaluronic acid is a glycosaminoglycan naturally present in synovial fluid and cartilage, responsible for maintaining joint homeostasis, absorbing mechanical shocks, and providing lubricating properties during weight-bearing activities. In osteoarthritis, the degradation and depletion of endogenous hyaluronic acid lead to increased friction, cartilage breakdown, and inflammatory cascades that manifest as chronic pain, swelling, and reduced mobility. Viscosupplementation attempts to reverse these biomechanical deficiencies by supplementing the joint with exogenous HA, theoretically improving synovial viscosity, reducing nociceptive signaling, and creating a temporary therapeutic window for patients to engage in rehabilitative exercises and daily activities.
However, navigating the cost of this treatment can be complex. The price you are quoted is often just the starting point. This comprehensive guide breaks down the real cost of knee gel injections, uncovering the various factors that influence the final bill, from insurance coverage and hidden fees to the ongoing debate about their true value. Understanding the financial landscape is essential for patients weighing their treatment options, particularly given the chronic nature of osteoarthritis and the potential need for repeated therapeutic cycles over many years. By examining the economic, clinical, and administrative dimensions of this procedure, individuals can make informed, cost-conscious healthcare decisions aligned with their medical needs and financial realities.
What is the Average Cost of Knee Gel Injections?
The out-of-pocket cost for knee gel injections varies widely. Based on data from multiple healthcare providers and cost analyses, you can expect the following price ranges:
- Per Injection: A single hyaluronic acid injection typically costs between $500 and $1,300 when paying out-of-pocket. This base rate usually encompasses the pharmaceutical product itself, physician administration, and standard facility overhead. However, prices can fluctuate based on the specific molecular weight and cross-linking technology of the HA formulation used. High-viscosity, highly cross-linked formulations generally command premium pricing due to extended manufacturing processes and longer proposed durations of clinical effect.
- Full Treatment Series: Most treatment protocols involve a series of 3 to 5 weekly injections. The total cost for a complete series can range from $1,200 to over $3,000. When multiplied across multiple visits, the financial burden compounds quickly, making it crucial for patients to understand the full economic commitment before initiating therapy. Additionally, each visit often incurs separate professional service charges, co-pays, or facility fees depending on your insurance structure or cash-pay agreement.
A 2022 study on nonsurgical treatments for knee osteoarthritis, cited by Medical News Today, found the average cost per session to be approximately $1,019. These figures highlight the substantial financial outlay required for viscosupplementation, particularly for uninsured patients or those with high-deductible health plans. It is also important to note that these baseline figures rarely include ancillary expenses such as diagnostic imaging, physical therapy referrals, or follow-up consultations, which are frequently recommended to optimize clinical outcomes.
Factors That Influence the Final Price: The 'All-In' Cost
The sticker price of the injection itself is only one piece of the puzzle. Several other factors contribute to your final bill, often referred to as the "all-in" cost. Healthcare pricing in the United States operates on a highly fragmented model, where identical clinical services can carry vastly different charges depending on administrative classifications, contractual agreements between payers and providers, and geographical market dynamics. Understanding these variables empowers patients to anticipate financial obligations accurately and avoid unexpected billing surprises.
Provider and Facility Fees
The same procedure can have a different price tag depending on where it's performed. A specialized orthopedic clinic may have different rates than a hospital's outpatient department, which often includes separate facility fees. In a hospital outpatient setting, you will typically be billed for the professional component (the physician's expertise and administration) and the technical/facility component (room use, nursing staff, equipment sterilization, and overhead). Ambulatory Surgery Centers (ASCs) and private practice clinics usually offer more streamlined pricing models, often resulting in lower facility fees or bundled cash-pay packages. Additionally, physician specialty matters; sports medicine specialists, physiatrists, and orthopedic surgeons may utilize different billing structures based on their overhead costs, credentialing, and regional market positioning.
Geographic Location
Healthcare costs can differ significantly based on your location. Urban centers with a higher cost of living generally have higher prices for medical procedures compared to rural areas. Metropolitan regions with dense healthcare networks and elevated real estate and labor costs typically reflect those expenses in procedural pricing. Conversely, suburban or rural clinics may offer more competitive rates due to lower operational overhead. State-specific regulations, Medicaid/Medicare reimbursement baselines, and regional insurance market competition also heavily influence baseline pricing. Patients considering medical tourism or traveling to lower-cost states for elective injections should carefully weigh transportation and accommodation expenses against potential procedural savings.
Brand of the Injection
Several brands of hyaluronic acid injections are available, and their costs and treatment protocols differ. Common brands include:
- Synvisc-One® (often a single-injection formula)
- Hyalgan®
- Orthovisc®
- Monovisc®
- Supartz FX™
The specific brand your doctor recommends can impact the total number of required visits and the overall price. These formulations vary significantly in molecular weight, source material (avian rooster comb vs. bacterial fermentation), cross-linking degree, and rheological properties. Higher molecular weight and heavily cross-linked products are engineered for slower degradation within the joint space, theoretically extending therapeutic duration and reducing the frequency of repeat injections. While premium brands may carry higher per-unit costs, they may ultimately prove more economical when accounting for fewer clinical visits, reduced time off work, and lower transportation costs. Insurance formularies also dictate brand availability; many plans maintain preferred product tiers, requiring step therapy or prior authorization before covering newer or more expensive alternatives.
Use of Ultrasound Guidance
To ensure the injection is placed accurately within the joint capsule, some doctors use ultrasound guidance. While this can improve the effectiveness of the shot, it typically adds a separate fee to the procedure cost. Ultrasound-guided injections allow real-time visualization of needle trajectory, ensuring precise intra-articular placement and minimizing the risk of extra-articular deposition, which can reduce efficacy and increase post-injection discomfort. This image-guided approach is particularly beneficial for patients with anatomical variations, severe osteophyte formation, obesity, or joint deformities that obscure surface landmarks. However, the additional equipment utilization, technician assistance, and billing codes (CPT 76942 for ultrasonic guidance) can add $75 to $250+ to the total visit charge, depending on regional fee schedules.
Additional Medical Services
The total cost should also account for related services, such as the initial consultation fee, follow-up appointments, and any recommended physical therapy to complement the treatment. Comprehensive osteoarthritis management rarely relies on injections alone. Physicians typically prescribe structured rehabilitation programs to strengthen quadriceps and hamstring musculature, improve joint proprioception, and optimize biomechanics. Physical therapy sessions, orthotic devices, unloader knee braces, and over-the-counter or prescription analgesics all contribute to the comprehensive financial footprint of conservative knee osteoarthritis care. Patients should request an itemized cost estimate that includes these ancillary services to gain a realistic understanding of their financial commitment.
Does Insurance Cover Knee Gel Injections?
Insurance coverage is the most significant factor determining your out-of-pocket expense. Most plans, including Medicare, cover the procedure, but only if specific criteria are met. The transition from theoretical eligibility to actual coverage involves navigating complex administrative pathways designed to control healthcare spending while ensuring medical necessity. Understanding these pathways can prevent claim denials, appeal delays, and unexpected financial burdens.
Medicare Coverage Explained
Medicare Part B typically covers 80% of the Medicare-approved amount for knee gel injections once you have met your annual deductible. This leaves you responsible for the remaining 20% coinsurance.
However, Medicare enforces strict requirements for coverage, which are detailed by the Centers for Medicare & Medicaid Services (CMS). You must:
- Have a confirmed diagnosis of symptomatic knee osteoarthritis.
- Provide medical imaging (like an X-ray) that confirms the diagnosis. Radiographic evidence typically demonstrates joint space narrowing, osteophyte formation, subchondral sclerosis, or bone cysts consistent with Kellgren-Lawrence grade II or III osteoarthritis.
- Have tried and failed at least three months of conservative treatments (e.g., physical therapy, exercise, pain relievers like NSAIDs). Documentation of these interventions must be thoroughly recorded in your medical record.
- Have unsuccessfully tried corticosteroid injections or be unable to receive them due to another medical condition.
Medicare also stipulates that a repeat series of injections will only be covered if at least six months have passed since the previous treatment. This time-based restriction is designed to prevent overutilization and encourage long-term disease management rather than continuous pharmacological intervention. Patients with Medicare Advantage (Part C) plans should verify that their specific network and benefit design align with traditional Part B guidelines, as Advantage plans often implement additional utilization management strategies, preferred provider networks, and tiered copay structures.
Private Insurance Coverage
Coverage from private insurance companies varies widely by plan. Most insurers follow similar medical necessity guidelines as Medicare. Before starting treatment, it is crucial to:
- Contact your insurer: Confirm the specifics of your coverage for viscosupplementation. Request a benefits verification letter outlining your exact financial responsibility.
- Ask about prior authorization: Many plans require your doctor to get approval before administering the injections. This process can take 7 to 14 days and requires detailed clinical notes, imaging reports, and documentation of failed conservative therapies.
- Understand your costs: Clarify your deductible, copayment, and coinsurance responsibilities. High-deductible health plans (HDHPs) may require patients to pay the full negotiated rate until their deductible is satisfied, making upfront cost transparency essential.
- Verify step therapy requirements: Some insurers mandate that patients attempt lower-cost alternatives, such as oral medications, physical therapy, or corticosteroid injections, before approving viscosupplementation. Failure to document these steps often results in automatic claim denial.
- Check formulary tier placements: Even when covered, HA injections may be placed on higher formulary tiers, triggering elevated copays. If your prescribed brand is non-preferred, ask your physician if a therapeutic alternative on a preferred tier would yield comparable clinical results at a lower out-of-pocket cost.
The Cost-Effectiveness Debate: Are Gel Injections Worth It?
While many patients report substantial pain relief from gel injections, the medical community is divided on their effectiveness, leading to a debate about their value. This divergence stems from the gap between real-world patient-reported outcomes and rigorous clinical trial data evaluating statistically significant structural or symptomatic improvements.
Clinical Evidence vs. Patient Experience
Many patients find that gel injections provide enough relief to improve their quality of life and delay the need for a knee replacement surgery. They experience reduced pain, less stiffness, and better mobility for daily activities. Patient satisfaction surveys consistently show favorable responses, with many individuals citing improved sleep quality, increased participation in low-impact exercise, and enhanced psychological well-being as direct benefits of treatment. These subjective improvements are clinically meaningful, particularly for older adults seeking non-operative pain management strategies.
However, the clinical evidence is less convincing. A large-scale 2022 review of 50 years of data published in The BMJ concluded that hyaluronic acid injections offer a "clinically irrelevant" benefit over placebo injections. This has led major medical bodies, including the American Academy of Orthopaedic Surgeons (AAOS) and the American College of Rheumatology (ACR), to issue conditional recommendations against their use for knee osteoarthritis. The AAOS guidelines emphasize the high risk of bias in older industry-sponsored trials and note that modern, rigorously designed studies fail to demonstrate meaningful differences in pain reduction or functional improvement compared to saline placebo. The conditional nature of these recommendations allows clinicians to exercise individualized judgment, recognizing that certain patient subgroups may still derive symptomatic benefit despite broader statistical trends.
Cost Comparison: HA vs. Other Treatments
When considering value, it's helpful to compare gel injections to alternatives.
- Corticosteroids: These anti-inflammatory injections are less expensive than HA and often recommended for short-term relief of acute flare-ups. Corticosteroid injections typically cost $50 to $150 per administration and provide rapid, albeit temporary, anti-inflammatory effects lasting 4 to 12 weeks. However, repeated corticosteroid use has been associated with cartilage thinning, tendon weakening, and potential metabolic disruptions in diabetic patients.
- No Injections: A 2022 study found that patients who received either HA or corticosteroid injections had higher long-term healthcare costs and a greater likelihood of eventually needing a total knee replacement compared to those who received no injections. The pathway involving HA injections was the most expensive. This finding suggests that while injections may mask symptoms temporarily, they do not alter the underlying pathophysiology of osteoarthritis progression. The study highlights the importance of comprehensive, multimodal management focusing on weight optimization, neuromuscular strengthening, and activity modification as foundational, cost-effective interventions.
Beyond direct medical costs, patients should consider indirect economic factors such as productivity loss, caregiver burden, and long-term joint preservation strategies. While gel injections offer a non-surgical intervention with minimal systemic side effects, their role should be viewed as part of a broader, patient-centered care continuum rather than a standalone curative solution.
Single-Dose vs. Multi-Dose Series: A Cost Comparison
Traditionally, viscosupplementation was administered as a series of three to five injections, spaced one week apart. Today, single-injection formulations are available, which offer a full course of treatment in one visit. This shift in administration protocols has significant financial and logistical implications for both patients and healthcare systems.
A growing body of research suggests that single-injection treatments are more cost-effective. A 2017 study found that a single-injection option was cheaper and led to better outcomes at 24 weeks than a five-injection series. Beyond the direct medical savings, a single visit reduces indirect costs for patients, such as transportation, parking, and time away from work. While some conflicting data exists, efficacy is generally considered comparable between the two methods, making the single-injection regimen an attractive and convenient alternative. The pharmacological advancement lies in increased molecular weight and advanced cross-linking technologies that create a viscoelastic scaffold capable of prolonged joint residence time. From a health economics perspective, consolidating multiple visits into one encounter reduces administrative overhead, streamlines insurance billing, and minimizes cumulative facility fees.
Patients considering the multi-dose approach should verify whether their insurance plan covers all visits in the series without gaps in authorization. Some insurers approve initial doses but require re-authorization for subsequent injections if early clinical improvement is not documented, creating potential financial exposure. Conversely, single-dose protocols typically secure full course approval upfront, providing predictable pricing and eliminating mid-series financial uncertainty.
Who Should Not Get Knee Gel Injections?
According to the Mayo Clinic, viscosupplementation is not recommended for everyone. You should avoid this treatment if you have:
- An allergy to hyaluronic acid products or to gram-positive bacterial proteins (some HA is derived from rooster combs). Patients with severe avian or protein allergies should specifically request fermentation-derived, synthetic HA alternatives.
- An active infection in or around the knee joint. Introducing a foreign substance into an infected space can exacerbate bacterial proliferation, lead to septic arthritis, and complicate systemic antimicrobial therapy.
- A skin disease or infection at the injection site. Compromised skin integrity increases the risk of introducing cutaneous flora into the sterile joint environment.
Additional relative contraindications include uncontrolled coagulopathies, active venous thromboembolism in the affected limb, severe joint instability requiring surgical stabilization, and end-stage bone-on-bone osteoarthritis where structural deformity precludes accurate intra-articular delivery. Discuss your full medical history with your doctor to ensure this treatment is safe for you. A thorough musculoskeletal examination, coupled with a review of current medications (particularly anticoagulants and immunosuppressants), helps mitigate procedural risks and optimize therapeutic safety.
Pre-Procedure Requirements & Diagnostic Costs
Before receiving your first knee gel injection, your physician will typically require a comprehensive diagnostic workup to establish medical necessity and baseline joint status. This preparatory phase directly impacts your overall treatment cost but is essential for ensuring clinical appropriateness. Weight-bearing radiographs are standard, costing $100 to $400 out-of-pocket depending on imaging center pricing and insurance coverage. Advanced imaging such as MRI is rarely required unless meniscal pathology or occult fractures are suspected, but if ordered, MRIs can add $400 to $1,500+ to your expenses.
Blood tests are occasionally ordered to rule out inflammatory arthropathies like rheumatoid arthritis or gout, which require entirely different treatment algorithms and are not eligible for HA therapy under most insurance protocols. Additionally, many insurers mandate documented proof of conservative management failure, meaning you will need to show medical records reflecting completed physical therapy courses, consistent NSAID use, and activity modifications. Failing to meet these documentation thresholds before initiating injections almost guarantees prior authorization denial, leaving patients responsible for the full procedural cost. Proactively compiling these records with your primary care provider or physical therapist can streamline insurance approval and prevent costly administrative delays.
Post-Injection Care and Hidden Recovery Expenses
The financial impact of knee gel injections extends beyond the procedural day. Post-procedural care is critical for maximizing therapeutic benefit and minimizing complications, yet these ancillary costs are frequently overlooked during treatment planning. For the first 48 hours following injection, patients are typically advised to avoid strenuous weight-bearing activities, prolonged standing, and high-impact exercise. This temporary activity modification may require arranging alternative transportation, hiring household help, or taking unpaid leave from physically demanding occupations.
Mild post-injection soreness, joint effusion, and localized warmth are common and typically resolve within 2 to 3 days. Over-the-counter analgesics like acetaminophen or topical NSAIDs are recommended, adding $10 to $40 to your immediate post-care expenses. Some patients experience transient synovial irritation or pseudogout-like inflammatory reactions, which may necessitate an unscheduled follow-up visit, diagnostic arthrocentesis to rule out infection, or a short course of prescription anti-inflammatory medication. Budgeting for one or two follow-up appointments within your insurance's visit allowance is advisable to monitor treatment response and address any adverse reactions promptly.
To optimize long-term outcomes, physicians often pair viscosupplementation with targeted physical therapy focusing on quadriceps strengthening, hamstring flexibility, hip abductor conditioning, and proprioceptive training. A standard 6 to 8-week PT protocol can cost $25 to $65 per session, with insurance typically covering 8 to 12 visits annually. Integrating rehabilitation into your treatment plan not only enhances injection efficacy but also builds sustainable musculoskeletal resilience, potentially reducing the need for future pharmacological interventions.
Financial Assistance and Payment Navigation Strategies
Given the substantial out-of-pocket potential of knee gel injections, exploring financial assistance options can significantly reduce economic burden. Health Savings Accounts (HSAs) and Flexible Spending Accounts (FSAs) are excellent tools for tax-advantaged payment, as viscosupplementation qualifies as a reimbursable medical expense under IRS Publication 502. Utilizing these pre-tax dollars effectively lowers your true cost by your marginal tax bracket percentage.
For patients without insurance coverage or with high-deductible plans, many orthopedic clinics offer transparent cash-pay packages that bundle physician fees, facility costs, and the HA product into a single, predictable price. Negotiating payment plans, requesting sliding-scale fees based on income, or inquiring about manufacturer-sponsored patient assistance programs can yield substantial savings. Several HA manufacturers maintain copay assistance cards or savings programs that reduce eligible commercial insurance patients' out-of-pocket expenses to as low as $0 to $50 per injection, though these programs typically exclude government-funded insurance recipients due to federal anti-kickback statutes.
Hospital financial counselors and non-profit medical billing advocates can also review your itemized statement for coding errors, duplicate charges, or incorrectly applied facility fees. Ensuring that CPT codes (20610 for major joint injection, 76942 for ultrasound guidance if applicable) and diagnosis codes align precisely with your clinical documentation prevents unjustified claim rejections. Persistent, organized financial advocacy is often the difference between an unmanageable bill and a successfully navigated healthcare expense.
References
- Arthritis Knee Pain Centers. (n.d.). Knee Gel Injections Cost. Retrieved from https://arthritiskneepain.com/knee-gel-injections-cost/
- Bahou, C. (2024). Medicare and rooster comb injections: What to know. Medical News Today. Retrieved from https://www.medicalnewstoday.com/articles/does-medicare-pay-for-rooster-comb-injections
- Cleveland Clinic. (n.d.). Knee Gel Injections (Viscosupplementation). Retrieved from https://my.clevelandclinic.org/health/procedures/knee-gel-injections-viscosupplementation
- Cueto, I. (2022). Common injections don’t help knee osteoarthritis more than placebo, large data review finds. STAT News. Retrieved from https://www.statnews.com/2022/07/06/hyaluronic-acid-injections-dont-help-knee-osteoarthritis-review-finds/
- Hobbs, H. (2024). Knee Gel Injections and Medicare: Coverage Details. Healthline. Retrieved from https://www.healthline.com/health/medicare/does-medicare-pay-for-rooster-comb-injections
- Mayo Clinic. (2025). Hyaluronic Acid (Injection Route). Retrieved from https://www.mayoclinic.org/drugs-supplements/hyaluronic-acid-injection-route/description/drg-20074557
- Rath, L. (2024). Hyaluronic Acid Injections. Arthritis Foundation. Retrieved from https://www.arthritis.org/health-wellness/treatment/treatment-plan/disease-management/hyaluronic-acid-injections-for-knee-pain
Frequently Asked Questions
How long does the pain relief from knee gel injections typically last?
The duration of therapeutic effect varies significantly among patients and depends on factors such as disease severity, injection brand, and individual metabolic response. Clinical trials and real-world data generally report symptom relief lasting between 6 to 12 months. Single-injection formulations utilizing advanced cross-linking technology may provide extended duration toward the upper end of this range, while multi-dose traditional series often show peak efficacy around 3 to 6 months post-completion. Because hyaluronic acid gradually metabolizes within the synovial environment, patients frequently notice a gradual decline in symptom control rather than an abrupt cessation. If pain returns prematurely, it may indicate inadequate initial response, advanced structural degeneration, or the need for alternative interventional strategies.
Can I receive knee gel injections if I am currently taking blood thinners?
Patients on anticoagulant or antiplatelet therapy (such as warfarin, apixaban, clopidogrel, or daily aspirin) require careful clinical evaluation before proceeding with knee gel injections. Joint aspiration and intra-articular administration carry a baseline risk of hemarthrosis, which is amplified in individuals with impaired coagulation. Most orthopedic specialists consider HA injections relatively safe for patients on stable, therapeutic-dose blood thinners, provided no active bleeding disorders exist and the procedure is performed with meticulous aseptic technique. Your physician may recommend continuing your medication regimen while utilizing a smaller-gauge needle, applying prolonged post-procedure compression, and monitoring closely for joint swelling. Never discontinue anticoagulants without explicit guidance from your prescribing cardiologist or primary care provider, as the risk of thromboembolic events far outweighs the procedural bleeding risk.
What happens if my insurance denies coverage for knee gel injections?
An insurance denial is not necessarily the end of your treatment pathway. The first step is to obtain the exact denial reason from your insurer's Explanation of Benefits (EOB) document. Common reasons include missing documentation of failed conservative therapy, lack of prior authorization, or step therapy non-compliance. You and your physician can submit a formal appeal, typically including a peer-to-peer review where your doctor directly discusses clinical necessity with the insurance medical director. Including detailed physical therapy progress notes, radiographic reports, medication history logs, and a letter of medical necessity significantly strengthens appeal success rates. If the appeal is unsuccessful, you can explore cash-pay options, inquire about manufacturer copay programs (if commercially insured), or consider clinically comparable lower-cost alternatives like corticosteroid injections or structured physical therapy intensification.
Are there any long-term risks or side effects associated with repeated hyaluronic acid treatments?
Hyaluronic acid injections are generally well-tolerated with a favorable safety profile over decades of clinical use. The most common adverse effects are localized and transient, including injection-site pain, mild swelling, warmth, and occasional joint effusion, which typically resolve within 48 to 72 hours. Rare complications include pseudo-septic inflammatory reactions, hypersensitivity responses, and localized calcification. Long-term studies have not demonstrated significant systemic toxicity or accelerated cartilage degradation attributable to exogenous HA administration. However, repeated injections into a progressively degenerating joint may delay definitive surgical intervention, potentially allowing further functional decline if relied upon as a standalone therapy. Maintaining a multidisciplinary approach that emphasizes weight management, biomechanical optimization, and activity pacing mitigates long-term risks and preserves treatment efficacy across multiple cycles.
Is it safe to combine knee gel injections with corticosteroid injections?
Clinicians generally advise against administering hyaluronic acid and corticosteroids into the same knee joint during the same clinical encounter, primarily due to conflicting pharmacological mechanisms and potential interference with therapeutic outcomes. Corticosteroids rapidly suppress synovial inflammation but possess catabolic properties that may theoretically degrade hyaluronic acid structure if mixed directly. Most specialists recommend spacing these interventions by at least two to four weeks, with many preferring to complete the full HA series before considering subsequent corticosteroid administration, or vice versa. Sequential use allows each therapy to exert its intended effect without pharmacological antagonism. Your physician will determine the optimal sequencing based on your current inflammatory status, pain profile, and radiographic findings. If a severe acute flare occurs mid-series, clinical discretion may permit adjusted protocols, but this should only be managed by a qualified musculoskeletal specialist.
Conclusion
Navigating the financial landscape of knee gel injections requires a thorough understanding of both clinical variables and administrative intricacies. While the baseline out-of-pocket costs typically range from $500 to $1,300 per injection, the true "all-in" expense encompasses provider fees, facility overhead, imaging prerequisites, ultrasound guidance, and essential adjunctive therapies like physical therapy. Insurance coverage, particularly through Medicare and private plans, can substantially offset these expenses, but only when stringent medical necessity criteria, step therapy requirements, and prior authorization protocols are meticulously documented and satisfied. The ongoing clinical debate surrounding viscosupplementation's efficacy underscores the importance of aligning treatment expectations with evidence-based outcomes, recognizing that while many patients experience meaningful symptomatic relief, the broader data suggests modest benefits over placebo. Ultimately, deciding whether to pursue knee gel injections should involve a collaborative discussion with your orthopedic specialist or rheumatologist, weighing individual disease severity, functional goals, financial capacity, and long-term joint preservation strategies. By leveraging available financial assistance tools, optimizing conservative management, and maintaining realistic expectations, patients can make informed, sustainable decisions that prioritize both physical comfort and economic responsibility in their osteoarthritis care journey.

About the author
Samuel Jones, MD, is a board-certified orthopedic surgeon specializing in joint replacement and orthopedic trauma. He is a team physician for a professional sports team and practices at a renowned orthopedic institute in Georgia.