Understanding the Cost of Hip Replacement Surgery

Key points
- Osteoarthritis: "Wear-and-tear" arthritis where cartilage breaks down over time.
- Rheumatoid Arthritis: An autoimmune disease causing chronic inflammation that damages joints.
- Post-Traumatic Arthritis: Arthritis that develops after a serious hip injury or fracture.
- Avascular Necrosis: The death of bone tissue due to a lack of blood supply, causing the joint to collapse.
- Childhood Hip Disease: Certain conditions from childhood can lead to arthritis and the need for a replacement later in life.
Hip replacement surgery is a life-changing procedure that can significantly reduce pain and restore mobility for people with severe hip damage or arthritis. However, one of the most common questions patients have is: “How much does a hip replacement surgery cost?” The answer isn’t straightforward, as the cost can vary widely depending on factors like location, type of procedure, and insurance coverage. Navigating the financial landscape of major orthopedic surgery requires careful planning, a clear understanding of medical billing, and proactive communication with healthcare providers. Many patients experience anxiety not just about the surgery itself, but about the unexpected financial burdens that can accompany it, from pre-operative clearance to long-term rehabilitation.
This guide explores the cost of hip replacement surgery in detail, breaking down the components, discussing influencing factors, and providing tips on managing expenses. Whether you are uninsured, navigating Medicare, or utilizing private insurance, understanding the true scope of these costs will empower you to make informed decisions about your care and financial future.
What is Hip Replacement Surgery?
Hip replacement surgery, or total hip arthroplasty, is a procedure where a damaged hip joint is removed and replaced with an artificial implant. The hip is a ball-and-socket joint. When damage from conditions like osteoarthritis, rheumatoid arthritis, or fractures causes severe pain and stiffness, this surgery can provide relief.
during the procedure, an orthopedic surgeon replaces the damaged femoral head (the "ball") with a metal or ceramic ball. The socket in the pelvis is resurfaced and fitted with a durable cup. These prosthetic parts replicate the function of a healthy hip, allowing for smooth, pain-free movement. Modern surgical techniques have evolved significantly over the past two decades. Surgeons now frequently utilize either a traditional posterior approach or an anterior (front-side) approach, which often results in less muscle disruption and faster initial recovery. Additionally, the integration of computer-navigated and robotic-assisted surgery has improved implant placement precision, which directly correlates with longer-lasting joint function and potentially fewer revision surgeries down the road. The materials used in the implants are also highly engineered, typically combining titanium or cobalt-chromium alloy stems with cross-linked polyethylene, ceramic, or metal bearing surfaces to minimize wear and reduce the risk of particle-induced inflammation over time.
An X-ray of a total hip replacement. The metal stem and ball replace the top of the thigh bone, fitting into an artificial socket. Image source: Wikimedia Commons.
According to the American Academy of Orthopaedic Surgeons (AAOS), over 450,000 total hip replacements are performed in the United States each year. It is considered one of the most successful operations in all of medicine, with patients often experiencing a dramatic reduction in pain and improved mobility. Success rates consistently exceed 95% at the 10-year mark, making it a cornerstone intervention for restoring independence in aging populations and younger individuals with degenerative joint disease.
Why Do People Need Hip Replacement Surgery?
The need for a hip replacement arises when the hip joint is severely damaged and non-surgical treatments no longer provide relief. Common reasons include:
- Osteoarthritis: "Wear-and-tear" arthritis where cartilage breaks down over time.
- Rheumatoid Arthritis: An autoimmune disease causing chronic inflammation that damages joints.
- Post-Traumatic Arthritis: Arthritis that develops after a serious hip injury or fracture.
- Avascular Necrosis: The death of bone tissue due to a lack of blood supply, causing the joint to collapse.
- Childhood Hip Disease: Certain conditions from childhood can lead to arthritis and the need for a replacement later in life.
Before surgeons recommend joint replacement, they typically exhaust conservative management strategies. Patients are usually guided through months of targeted physical therapy, non-steroidal anti-inflammatory drugs (NSAIDs), corticosteroid or hyaluronic acid joint injections, weight management programs, and lifestyle modifications like switching to low-impact exercises. When pain begins to interfere with basic activities of daily living—such as dressing, walking short distances, sleeping through the night, or maintaining employment—the clinical threshold for surgical intervention is met. Diagnostic imaging, primarily weight-bearing X-rays, MRI, or CT scans, confirms joint space narrowing, bone spurs, and subchondral sclerosis, providing objective evidence that supports the medical necessity of the procedure for insurance purposes.
Types of Hip Replacement Surgeries
The type of procedure performed can also influence the final cost:
- Total Hip Replacement (THR): The most common type, where both the ball and socket are replaced.
- Partial Hip Replacement (Hemiarthroplasty): Only the ball (femoral head) is replaced. This is often performed for specific types of hip fractures.
- Hip Resurfacing: The femoral head is trimmed and capped with a metal covering instead of being fully removed. This is an alternative for some younger, more active patients.
In recent years, bilateral hip replacement (replacing both hips in a single operative session or staged within a short timeframe) has become more common among highly selected patients, though it carries different risk profiles and cost structures. Additionally, minimally invasive surgical techniques and robotic-assisted arthroplasty are gaining traction. While these advanced approaches may carry a slightly higher upfront facility or technology fee, they often reduce hospital stay duration, lower post-operative complication rates, and accelerate return-to-work timelines, which can offset initial expenses in the long run.
How Much Does a Hip Replacement Surgery Cost?
The cost of a hip replacement varies dramatically. For patients without insurance in the United States, a total hip replacement can range from $20,000 to over $50,000. In some high-cost regions or at specialized academic centers, the price can exceed $100,000.
Most patients do not pay this full "sticker price." Insurance companies, Medicare, and Medicaid negotiate lower rates with hospitals. These negotiated discounts are a critical component of healthcare economics, as the chargemaster rates are rarely reflective of what is actually paid. Cash-paying patients who negotiate upfront can sometimes secure discounted bundled pricing that bypasses traditional billing complexities, though this requires diligent research and direct communication with hospital financial counseling departments.
Breakdown of Typical Uninsured Costs in the U.S.
| Cost Component | Estimated Cost (USD) |
|---|---|
| Hospital or Surgical Facility | $15,000 – $30,000 |
| Surgeon’s Fees | $2,000 – $5,000 |
| Anesthesiologist’s Fees | $1,000 – $3,000 |
| Artificial Hip Implant (Prosthesis) | $5,000 – $10,000 |
| Pre-operative Tests (X-rays, labs) | $500 – $1,500 |
| Post-operative Care (Physical therapy, etc.) | $1,000 – $5,000+ |
| TOTAL Estimated Cost | $20,000 – $50,000+ |
A partial hip replacement may cost slightly less, while a revision hip replacement (a second surgery to replace a failed implant) is often more complex and can cost 20-30% more. The implant component alone is highly regulated and represents one of the most technologically expensive aspects of modern orthopedics. Surgical centers must purchase these devices from major manufacturers, and the cost is passed through the facility's billing system. Additionally, anesthesia billing depends heavily on duration and complexity; longer operative times or patients with significant comorbidities requiring invasive monitoring will see higher anesthesiology charges. Post-operative care costs are highly variable, as they depend on the patient's adherence to home exercise programs, the number of required outpatient physical therapy sessions, and whether a skilled nursing facility stay is medically necessary after discharge.
Cost Variation by Location
Where you have your surgery has a major impact on cost. A study by the Blue Cross Blue Shield Association found that costs for the same procedure can vary by tens of thousands of dollars between different cities. This is due to differences in labor costs, hospital overhead, regional market competition, and state-level healthcare regulations. Metropolitan areas with higher costs of living and dense concentrations of academic medical centers typically charge premium rates. Conversely, rural community hospitals or facilities in regions with lower overhead may offer significantly reduced pricing. Many states and organizations like FAIR Health Consumer offer tools to help you compare the average costs of procedures at different facilities in your area. Utilizing these transparency databases can save patients thousands of dollars and help them negotiate fair rates before committing to a specific provider.
Hip Replacement Cost Around the World
- United Kingdom: The National Health Service (NHS) provides medically necessary hip replacements free of charge to residents, though wait times can be long. Privately, the procedure can cost £10,000 to £15,000.
- Canada: The public healthcare system covers the cost of medically necessary hip replacements, but like in the UK, patients may face significant wait times for elective surgery.
- Medical Tourism (India, Thailand, Mexico): Costs in these countries can be significantly lower. A total hip replacement in India might cost between $7,000 and $15,000. While this offers substantial savings, patients must also factor in travel, accommodation, and the logistics of follow-up care.
When considering international options, it is crucial to verify surgeon credentials, hospital accreditation (such as Joint Commission International), and implant quality standards. Complications managed abroad can become exponentially expensive if emergency repatriation or stateside revision surgery is required. Furthermore, continuity of care is vital; physical therapists and orthopedic specialists in your home community need clear surgical notes, implant identifiers, and post-operative protocols to ensure a safe rehabilitation trajectory.
For a clearer understanding of the costs involved specifically for Medicare patients, this video breaks down the differences between traditional Medicare and Medicare Advantage.
Factors That Influence Hip Replacement Surgery Cost
- Geographic Location: Costs vary between countries, states, and even between urban and rural areas. Regional wage scales for healthcare workers, real estate costs for facilities, and state-mandated insurance requirements all contribute to baseline pricing differences.
- Type of Hospital or Facility: Large academic medical centers or specialized orthopedic hospitals may charge more than community hospitals or outpatient surgery centers. Academic centers often bill for advanced technology, teaching staff, and complex case management capabilities.
- Surgeon’s Experience: Highly sought-after surgeons may have higher fees. Surgeon expertise directly impacts surgical efficiency, complication rates, and long-term implant survival, which justifies premium pricing for many patients.
- Type of Hip Implant: Advanced materials like ceramic or highly cross-linked polyethylene can be more expensive than traditional metal-on-plastic implants. The choice of bearing surface is customized based on patient age, activity level, and bone quality.
- Inpatient vs. Outpatient Surgery: With modern techniques, some healthy patients can go home the same day. An outpatient procedure avoids the costs associated with a multi-day hospital stay, reducing room-and-board fees and ancillary service charges.
- Pre- and Post-Operative Care: Costs include initial consultations, imaging, physical therapy, medications, and any necessary assistive devices. Comprehensive care pathways that bundle these services often provide more predictable pricing.
- Length of Hospital Stay: A typical stay is 1 to 3 days. Longer stays due to complications will increase the total bill. Each additional inpatient night incurs nursing, monitoring, and facility overhead costs.
- Complications: Unexpected issues like infections, deep vein thrombosis, dislocations, or blood clots require additional treatment and significantly raise costs. Complications can trigger readmissions, extended antibiotic courses, and unplanned return-to-the-OR expenses, which dramatically inflate the financial burden.
Insurance Coverage and Medicare
For most patients, insurance is the single biggest factor determining their out-of-pocket cost.
- Private Health Insurance: Most plans cover medically necessary hip replacements. However, patients are typically responsible for their deductible, copayments, and coinsurance until they reach their annual out-of-pocket maximum. Using in-network providers is essential to minimize costs. Understanding the difference between a flat copay and a percentage-based coinsurance is critical, as a 20% coinsurance on a $40,000 procedure can still result in significant personal expense.
- Medicare: Medicare covers hip replacement surgery for eligible individuals.
- Part A (Hospital Insurance) covers inpatient hospital costs. You must first pay the Part A deductible.
- Part B (Medical Insurance) covers surgeon's fees and outpatient services. You pay 20% of the Medicare-approved amount after meeting the annual Part B deductible.
- Medigap (Medicare Supplement) or Medicare Advantage plans can help cover these out-of-pocket expenses. Medicare Advantage plans often offer $0 copays for hospital stays but require network adherence and prior authorization, while Medigap plans typically cover most or all deductibles and coinsurance in exchange for a monthly premium.
- Medicaid: For eligible low-income individuals, Medicaid typically covers hip replacement with minimal out-of-pocket costs, though provider choice may be limited. Eligibility thresholds and covered services vary significantly by state, and prior authorization is almost universally required.
Always contact your insurance provider before scheduling surgery to get a pre-authorization and an estimate of your costs. Request a detailed "good faith estimate" or pre-service cost prediction from your insurer, which outlines expected patient responsibility based on your specific benefit design. If a claim is denied initially, patients have the right to an internal appeal and, if necessary, an external independent review.
How to Manage and Reduce Hip Replacement Surgery Costs
- Choose In-Network Providers: Ensure your surgeon, anesthesiologist, and hospital are all in your insurance network. Out-of-network billing can trigger surprise costs, especially from ancillary staff like surgical assistants or pathologists.
- Get a Cost Estimate in Advance: Under the Hospital Price Transparency Rule, hospitals must provide clear pricing information. Ask for an itemized estimate. Compare these figures against your insurance plan's cost-sharing structure to avoid billing surprises.
- Consider an Outpatient Surgery Center: If you are a candidate, an ambulatory surgical center (ASC) often has lower facility fees than a hospital. ASCs specialize in efficiency and frequently negotiate lower implant procurement costs, passing savings to patients.
- Inquire About Financial Assistance: Many non-profit hospitals have charity care programs for uninsured or underinsured patients based on income. These programs can reduce bills by 50% to 100%, depending on household size and federal poverty guidelines.
- Ask About Payment Plans: Most hospitals offer interest-free or low-interest payment plans to help you manage your portion of the bill. Structuring payments before surgery is financially safer than negotiating high-interest credit card debt after receiving a final statement.
- Use Tax-Advantaged Accounts: Use funds from a Health Savings Account (HSA) or Flexible Spending Account (FSA) to pay for medical expenses with pre-tax dollars. This effectively provides an immediate 20-30% discount depending on your marginal tax bracket.
- Review All Bills Carefully: Check every bill for errors and question any charges you don't understand. Common errors include duplicate charges, unbundled services, incorrect procedure coding, or charges for services you didn't receive. You have the legal right to request an itemized billing ledger and challenge discrepancies.
If you are wondering about the specifics of coverage, this short video explains whether Medicare covers total hip replacement surgery.
Hidden Costs and Financial Preparation for Recovery
Beyond the direct medical bills, patients must budget for the indirect costs of recovery. Preparing your home environment is a critical financial consideration. You may need to purchase or rent equipment such as a walker, raised toilet seat, shower chair, reaching aid, or ice therapy machine. These items are rarely covered by standard insurance but are essential for preventing falls and promoting safe mobility in the early weeks.
Additionally, patients often need to arrange for caregiver support. While some rely on family, hiring a professional home health aide for assistance with bathing, meal preparation, and transportation to follow-up appointments can add $20 to $30 per hour. Time off work represents another substantial financial impact. Depending on your occupation, recovery before returning to light desk work may take 4 to 6 weeks, while physically demanding jobs may require 3 to 6 months of disability leave. Exploring short-term disability insurance, state-mandated paid family leave programs, or employer-sponsored leave policies well in advance can protect your household income during this critical healing window.
Long-Term Value of Hip Replacement
When evaluating the cost, it's vital to consider the long-term benefits.
- Improved Quality of Life: The primary benefit is a dramatic reduction in pain, allowing a return to daily activities. Patients frequently report restored independence, better sleep, and renewed social engagement.
- Long-Lasting Results: Modern hip implants are durable, with most lasting 15 to 20 years or longer. Technological advancements in metallurgy, surface treatments, and manufacturing precision continue to extend implant lifespans, delaying the need for costly revision surgeries.
- Potential Cost Savings Over Time: A successful surgery can reduce or eliminate ongoing expenses for pain medication, frequent doctor visits, and other treatments related to chronic hip pain. Studies have consistently shown that hip replacement is a highly cost-effective procedure for improving quality of life. Economic analyses frequently demonstrate that when factoring in lost productivity, prescription costs, and reduced healthcare utilization, the procedure pays for itself within 1 to 3 years post-operation.
- Mental and Physical Health Synergy: Chronic joint pain is strongly linked to depression, social isolation, and sedentary lifestyles. By restoring mobility, patients are more likely to engage in cardiovascular exercise, maintain healthy weight, and manage metabolic conditions like diabetes and hypertension, creating compounding health and financial benefits.
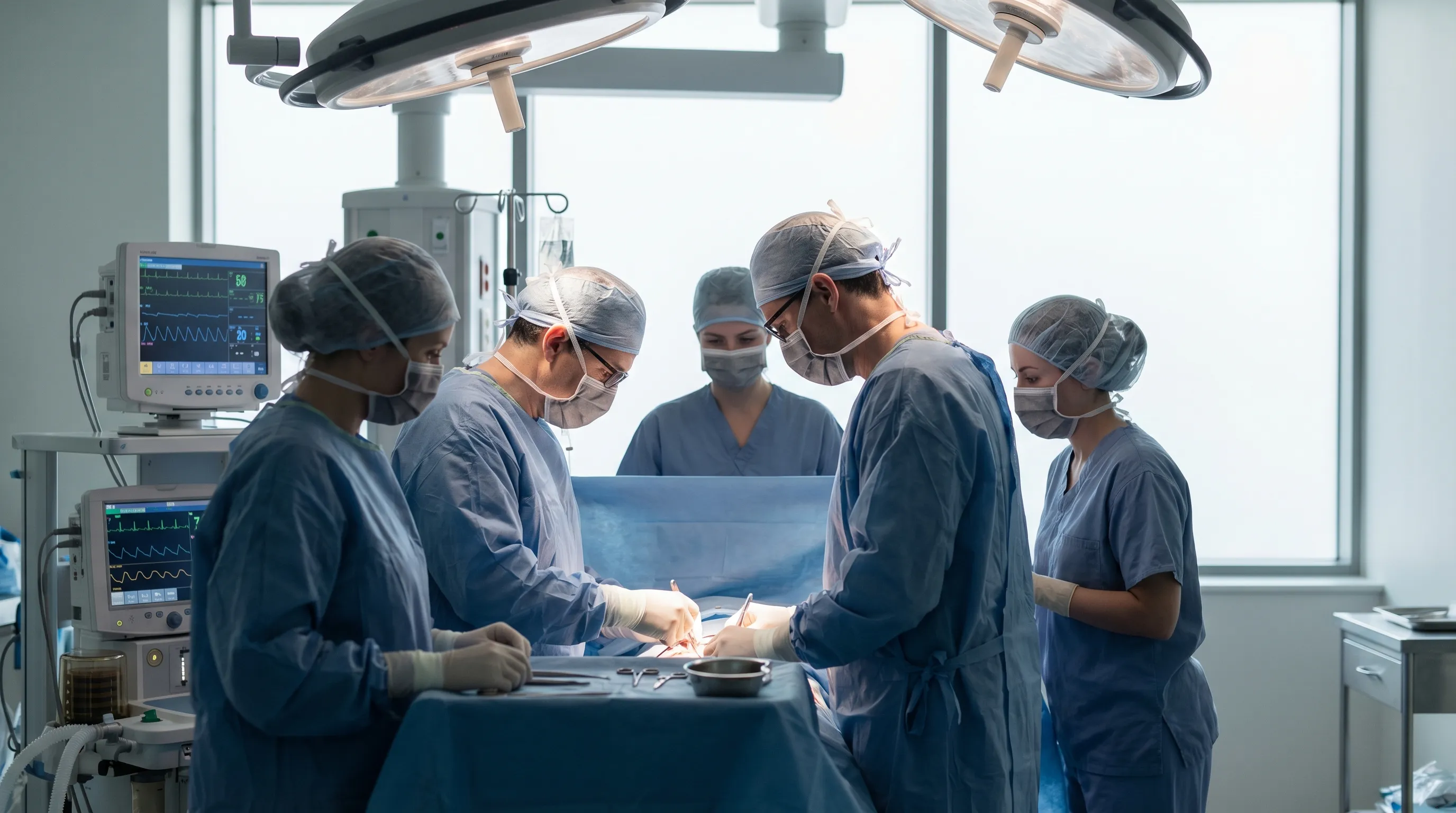 Surgeons performing a hip replacement operation. The sterile environment and specialized team ensure patient safety. Image source: Wikimedia Commons.
Surgeons performing a hip replacement operation. The sterile environment and specialized team ensure patient safety. Image source: Wikimedia Commons.
Conclusion
Hip replacement surgery is a major investment in your health and well-being. While the total costs can be substantial, insurance and Medicare cover a large portion for most patients. By proactively researching options, communicating with your healthcare providers and insurer, and understanding all the factors involved, you can navigate the financial aspects of the procedure and focus on what matters most: a successful recovery and a return to a pain-free, active life. Financial planning should be treated with the same diligence as medical preparation. Gather documentation, understand your benefits, ask questions, and build a support system. With careful navigation, the path to restored mobility can be both clinically successful and financially manageable.
For More Information and Resources:
- American Academy of Orthopaedic Surgeons (AAOS): Total Hip Replacement Overview
- American Association of Hip and Knee Surgeons (AAHKS): Patient Education Resources
- Medicare.gov: Official U.S. Government Site for Medicare
- Arthritis Foundation: Resources for surgery and financial assistance
Frequently Asked Questions
How long does a hip replacement implant typically last before it needs to be replaced?
Modern total hip implants are engineered to last 15 to 25 years, with many patients experiencing excellent function for two decades or more. Implant longevity depends on several factors, including patient age at surgery, activity level, body weight, bone quality, and the specific bearing surfaces used. Highly cross-linked polyethylene, ceramic-on-ceramic, and advanced metal alloys have significantly reduced wear debris, which historically triggered inflammation and loosening. Younger, more active patients may place greater stress on the joint, potentially necessitating a revision surgery later in life. Regular follow-up imaging and adherence to low-impact exercise guidelines can help maximize implant lifespan and delay or avoid the higher costs associated with revision procedures.
Does health insurance require prior authorization for hip replacement surgery?
Yes, the vast majority of private insurance plans and all Medicare Advantage plans require prior authorization before a hip replacement can be performed. Prior authorization is a utilization management process where your insurer reviews medical records, imaging results, and documentation of failed conservative treatments to confirm medical necessity. The process typically takes 1 to 3 weeks. If you undergo surgery without obtaining this authorization, your claim may be denied entirely, leaving you responsible for the full cost. It is highly recommended that your surgeon's billing coordinator initiates this process early, while you verify coverage details and network requirements directly with your insurance carrier.
Can I use my Health Savings Account (HSA) or Flexible Spending Account (FSA) for pre- and post-surgery expenses?
Absolutely. HSAs and FSAs are specifically designed to cover qualified medical expenses with tax-advantaged dollars, and hip replacement surgery-related costs are fully eligible. You can use these funds to pay for your deductible, coinsurance, copayments, and out-of-pocket expenses for the surgery itself, anesthesia, and physical therapy. Additionally, they cover necessary durable medical equipment like walkers, raised toilet seats, ice machines, and even transportation costs to and from medical appointments if primarily for medical care. Since HSA funds roll over year-to-year while FSA funds typically expire, planning your elective surgery timing around your account balance and employer plan year can yield significant tax savings.
What happens if complications arise after I'm discharged from the hospital?
If complications such as surgical site infections, blood clots, joint dislocation, or excessive swelling occur after discharge, you should contact your orthopedic surgeon immediately. Many hospitals include a global surgical period (typically 90 days post-operation) in their initial billing, which covers routine follow-up visits and treatment of standard complications directly related to the procedure. However, readmissions, emergency room visits for severe issues, or complications requiring separate surgical intervention may generate additional charges. Understanding your insurance policy's readmission coverage, coordinating closely with your care team during the first three months, and following all post-operative protocols rigorously are the most effective ways to mitigate unexpected medical and financial burdens.
Are there grants or charitable programs available to help cover the cost of a hip replacement for uninsured patients?
Yes, several resources exist to assist uninsured or underinsured individuals. Non-profit hospitals are legally required to offer charity care and financial assistance programs based on household income, often covering 100% of costs for patients earning below 200-300% of the federal poverty level. Additionally, national and state-based organizations such as the HealthWell Foundation, Patient Advocate Foundation, and local community health charities may offer grants or copay assistance for qualifying surgical procedures. Patients can also explore clinical trials or teaching hospital programs where surgical costs may be partially subsidized in exchange for participation in approved orthopedic research studies. Contacting a hospital financial counselor before scheduling surgery is the most reliable first step to identifying eligible assistance programs.

About the author
Samuel Jones, MD, is a board-certified orthopedic surgeon specializing in joint replacement and orthopedic trauma. He is a team physician for a professional sports team and practices at a renowned orthopedic institute in Georgia.