Is Osteoarthritis a Disability? Understanding Your Rights and Options

Key points
- Commonly Affected Joints: It most often affects the knees, hips, hands, and spine.
- Symptoms: Key symptoms are joint pain, stiffness (especially in the morning or after inactivity), a grinding sensation (crepitus), and a decreased range of motion.
- Gradual Onset: OA typically develops slowly and becomes more common with age, though joint injuries or repetitive stress can cause it in younger people.
- High Prevalence: According to the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), millions of adults worldwide have osteoarthritis, making it a leading cause of joint problems.
Osteoarthritis (OA) is the most common form of arthritis, known for causing joint pain and stiffness. But is it considered a disability? The answer depends on the severity of your condition and the specific context—whether medical, legal, or social. This article explores what osteoarthritis is, how it can impact daily life, and the circumstances under which it is legally recognized as a disability.
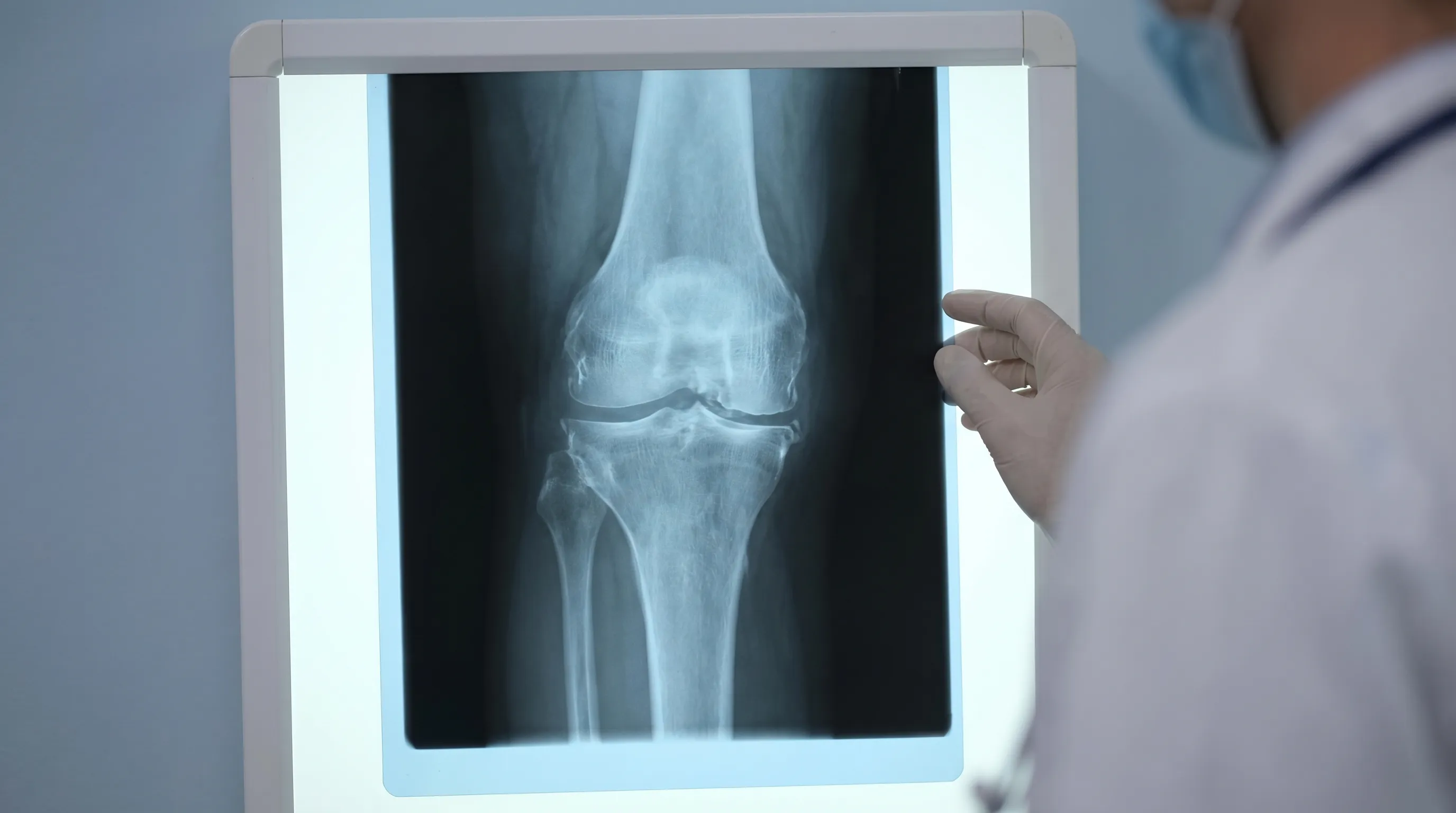 An X-ray image of a knee with advanced osteoarthritis reveals reduced space between the bones due to cartilage loss.
An X-ray image of a knee with advanced osteoarthritis reveals reduced space between the bones due to cartilage loss.
Understanding Osteoarthritis
Osteoarthritis is a degenerative joint disease often called "wear-and-tear" arthritis. It develops when the protective cartilage cushioning the ends of your bones wears down over time. As cartilage deteriorates, bones can rub directly against each other, causing pain, swelling, and reduced mobility.
Key characteristics of osteoarthritis include:
- Commonly Affected Joints: It most often affects the knees, hips, hands, and spine.
- Symptoms: Key symptoms are joint pain, stiffness (especially in the morning or after inactivity), a grinding sensation (crepitus), and a decreased range of motion.
- Gradual Onset: OA typically develops slowly and becomes more common with age, though joint injuries or repetitive stress can cause it in younger people.
- High Prevalence: According to the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), millions of adults worldwide have osteoarthritis, making it a leading cause of joint problems.
While many manage OA with mild symptoms, for others, the condition can lead to severe pain and mobility issues. Historically viewed as an inevitable consequence of aging, modern rheumatology and orthopedics now classify OA as a complex, multifactorial disease involving not just mechanical degradation but also low-grade inflammatory processes, metabolic changes, and genetic predispositions. The disease does not affect all joints equally, and its progression varies significantly between individuals based on a combination of biomechanical and biological factors.
The Pathophysiology of Osteoarthritis At a cellular level, osteoarthritis involves much more than simple friction. The breakdown of articular cartilage is driven by an imbalance between cartilage matrix synthesis and degradation. Chondrocytes, the cells responsible for maintaining cartilage health, begin to produce abnormal matrix proteins while releasing inflammatory cytokines like interleukin-1 (IL-1) and tumor necrosis factor-alpha (TNF-α). These molecules accelerate the breakdown of collagen and proteoglycans, leading to the characteristic thinning and fraying of the cartilage surface. As the disease progresses, the underlying bone responds by becoming denser (subchondral sclerosis) and forming bony outgrowths at the joint margins (osteophytes). The synovial membrane may also become inflamed (synovitis), and excess fluid can accumulate in the joint space (effusion), further contributing to pain, swelling, and restricted movement.
Risk Factors and Contributors Several modifiable and non-modifiable factors influence the development and progression of OA:
- Age: The incidence of OA rises sharply after age 50 due to cumulative joint use, decreased regenerative capacity of cartilage, and age-related muscle mass loss.
- Genetics: Family history plays a significant role, particularly in nodal OA of the hands and certain hip deformities. Specific gene variants affect collagen structure, cartilage metabolism, and inflammatory responses.
- Obesity and Metabolic Health: Excess body weight places disproportionate mechanical stress on weight-bearing joints. Beyond biomechanics, adipose tissue acts as an active endocrine organ, releasing pro-inflammatory adipokines that systemically exacerbate joint degradation.
- Previous Joint Injury: Traumatic injuries like anterior cruciate ligament (ACL) tears, meniscus damage, or fractures dramatically increase the risk of post-traumatic OA, sometimes manifesting just a decade after the initial injury.
- Joint Misalignment and Muscle Weakness: Abnormal biomechanics (e.g., bowlegs or knock-knees) and weakness in surrounding muscles, such as the quadriceps in knee OA, fail to adequately absorb impact forces, accelerating cartilage breakdown.
- Occupational and Repetitive Stress: Jobs requiring heavy lifting, frequent kneeling, squatting, or repetitive fine motor movements (e.g., in manufacturing, construction, or agriculture) are strongly correlated with higher OA rates.
Diagnostic Approach Diagnosing osteoarthritis typically involves a thorough clinical evaluation rather than a single definitive lab test. Rheumatologists and orthopedic specialists rely on patient-reported symptoms, physical examination findings (joint tenderness, crepitus, limited range of motion, bony enlargement), and imaging. Standard weight-bearing X-rays remain the gold standard for confirming OA, as they clearly demonstrate joint space narrowing, osteophyte formation, and subchondral bone changes. In complex or early-stage cases, magnetic resonance imaging (MRI) may be used to assess soft tissue structures, meniscal tears, ligament integrity, and bone marrow lesions (also known as bone bruises), which are increasingly recognized as strong predictors of pain and disease progression. Blood tests are generally not used to diagnose OA but may be ordered to rule out inflammatory arthritides like rheumatoid arthritis, lupus, or gout.
"Arthritis is the leading cause of disability among adults in the U.S."
— Arthritis Foundation
This statement underscores the profound impact arthritis, including OA, can have on a person's life. But to understand when it crosses the line, we must first define "disability."
What Does "Disability" Mean?
The term disability refers to a physical or mental condition that significantly limits a person’s movements, senses, or activities. It’s not just about a diagnosis; it’s about the functional impact on your life.
- Medical Perspective: A doctor might consider someone disabled if their OA is so severe that they can barely walk, even with a cane.
- Legal Perspective: In the United States, the Americans with Disabilities Act (ADA) defines a person with a disability as someone with a physical or mental impairment that substantially limits one or more major life activities (e.g., walking, standing, lifting, working). Severe OA can meet this definition.
- Functional Perspective: The World Health Organization (WHO) views disability as an interaction between a health condition and environmental barriers. For example, severe knee OA combined with a workplace that only has stairs can become a disabling situation.
Evolving Models of Disability The understanding of disability has shifted significantly over the past several decades. The traditional medical model views disability strictly as a deficit within the individual that requires treatment or cure to normalize functioning. In contrast, the social model argues that while the impairment (like joint degeneration) is a biological reality, the disability itself is often created by societal and environmental barriers—such as inaccessible buildings, lack of ergonomic tools, or inflexible work policies. Modern disability frameworks, including those used by the WHO's International Classification of Functioning, Disability and Health (ICF), integrate both perspectives, recognizing that disability is a dynamic interaction between health conditions, personal factors (like age, coping skills, and comorbidities), and environmental contexts.
Invisible Disability and Episodic Symptoms Osteoarthritis is frequently categorized as an invisible disability. Unlike a visible limb difference or mobility aid, many individuals with severe OA may appear completely able-bodied when walking short distances on flat ground. However, their pain, fatigue, and joint instability can flare unpredictably. This episodic nature complicates the disability experience. A person might manage daily routines effectively for weeks, only to experience a debilitating "flare" triggered by weather changes, overexertion, or stress. These invisible and fluctuating symptoms often lead to misunderstandings from employers, family members, or insurers who expect disability to be a constant, static state. Recognizing OA's variable presentation is crucial for both accurate self-assessment and fair legal or workplace evaluation.
Crucially, not everyone with osteoarthritis is disabled. The condition exists on a spectrum, from minor aches to chronic pain that severely impairs daily functioning.
When Does Osteoarthritis Become a Disability?
Osteoarthritis becomes a disability when it significantly limits your daily life or ability to work. Here are signs that your OA may be considered disabling:
- Severe Pain and Stiffness: The pain is persistent and intense, even at rest, and stiffness severely restricts your joint's range of motion.
- Limited Mobility: You struggle to walk, climb stairs, or stand for more than a few minutes and may require a cane, walker, or other assistive device.
- Difficulty with Daily Activities: Severe OA in the hands can make it hard to grip objects, write, or type. OA in the knees or spine can interfere with bathing, dressing, or household chores.
- Inability to Work: Your condition prevents you from performing the essential duties of your job. For instance, a person with severe knee OA may have to quit a job that requires standing or lifting.
Functional Assessment Tools Healthcare professionals and disability adjudicators often use standardized questionnaires and performance tests to objectively measure how OA impacts function. The Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) evaluates pain, stiffness, and physical function in hip and knee OA. The Health Assessment Questionnaire Disability Index (HAQ-DI) measures difficulty performing daily activities like dressing, eating, and hygiene. Clinically, gait analysis, grip strength dynamometry, and timed up-and-go (TUG) tests provide quantifiable data on mobility deficits. These tools help translate subjective pain reports into actionable metrics for disability determination.
The Impact on Sleep, Mental Health, and Fatigue Severe osteoarthritis rarely exists in isolation. Chronic, unrelenting joint pain frequently disrupts sleep architecture, leading to insomnia and non-restorative sleep. This sleep deprivation exacerbates pain perception through central sensitization—a neurological phenomenon where the central nervous system becomes hyper-reactive to pain signals, making even minor joint movements feel intensely painful. The resulting cycle of pain, fatigue, and sleep loss significantly increases the risk of developing secondary conditions like major depressive disorder and generalized anxiety. Mental health struggles can further diminish functional capacity, as reduced motivation, cognitive fatigue, and emotional distress make self-care, employment, and social engagement increasingly difficult. Therefore, when evaluating disability, clinicians increasingly consider the biopsychosocial burden of OA, not just radiographic findings.
Work Capacity and Vocational Impact Determining whether OA crosses into work-related disability involves analyzing specific physical demands against individual capacity. Sedentary work may become impossible if lumbar spine or cervical OA causes severe radicular pain or if hand involvement prevents sustained typing or document manipulation. Light-duty or physical labor becomes untenable when hip, knee, or foot OA limits walking distances below six hours per day, restricts bending or climbing, or requires frequent postural changes that cannot be accommodated. The unpredictable nature of flare-ups means some individuals can only maintain employment on a strictly modified or part-time basis, which may fall below the substantial gainful activity (SGA) threshold used by disability programs.
In short, osteoarthritis is considered a disability when it functionally impairs you to the point where you cannot perform routine daily tasks or job duties that an average person could.
Legal Recognition: Osteoarthritis and Disability Benefits
From a legal standpoint, whether your osteoarthritis is recognized as a disability depends on specific criteria used by government agencies and insurance programs.
Employment and Anti-Discrimination Laws (e.g., ADA)
In the U.S., the Americans with Disabilities Act (ADA) protects individuals with disabilities from workplace discrimination.
- Under the ADA, osteoarthritis is considered a disability if it “substantially limits one or more major life activities.”
- If you are qualified for your job, your employer must provide reasonable accommodations, unless it causes undue hardship. Accommodations for OA might include:
- An ergonomic chair or sit-stand desk.
- More frequent breaks.
- Flexible work hours or remote work options.
- Reassignment of strenuous tasks.
- An accessible workspace (e.g., a closer parking spot).
The Interactive Accommodation Process Securing workplace accommodations requires a collaborative approach known as the interactive process. Employees must formally request accommodations, typically through human resources or a designated ADA coordinator, and provide medical documentation outlining the specific functional limitations and how the requested adjustments will enable them to perform essential job functions. Employers are legally obligated to engage in good-faith dialogue to identify effective solutions. It's important to note that the ADA Amendments Act (ADAAA) of 2008 broadened the definition of disability, making it easier for chronic conditions like OA to qualify. Employers cannot retaliate against employees for requesting accommodations, nor can they penalize staff for utilizing legally protected sick leave or intermittent Family and Medical Leave Act (FMLA) benefits, which often run parallel to ADA protections. The Job Accommodation Network (JAN) offers extensive guidance on workplace accommodations for arthritis.
Social Security Disability (U.S.)
If OA prevents you from working entirely, you may qualify for Social Security Disability benefits (SSDI or SSI).
The Social Security Administration (SSA) evaluates OA under its listing for "Major dysfunction of a joint(s)" in its medical guide, the "Blue Book." To qualify, you generally need:
- Medical evidence of joint damage (e.g., X-rays showing joint space narrowing).
- Chronic pain and stiffness.
- Significant functional loss, such as an inability to walk effectively or perform fine and gross movements with your hands.
The Five-Step Sequential Evaluation Process The SSA uses a rigorous, five-step framework to determine disability:
- Step 1: Substantial Gainful Activity (SGA) – If you are currently earning above a specific monthly threshold (adjusted annually), you will generally be denied benefits regardless of your medical condition.
- Step 2: Severity of Impairment – The SSA assesses whether your OA significantly limits your ability to perform basic work activities for at least 12 continuous months. Mild or moderate OA often does not meet this threshold.
- Step 3: Meeting or Equaling a Listed Impairment – The examiner checks if your medical records satisfy Listing 1.18 (Major Dysfunction of a Joint). This requires objective imaging evidence of joint destruction combined with severe functional limitation, such as requiring a walker, inability to walk effectively, or severe hand impairment preventing manipulation.
- Step 4: Past Relevant Work – If you don't meet the listing, the SSA evaluates your Residual Functional Capacity (RFC) to see if you can still perform your previous jobs. An RFC details exactly what you can physically do despite your limitations (e.g., lifting limits, standing/walking duration, need to avoid climbing or kneeling).
- Step 5: Other Work – Finally, considering your RFC, age, education, and transferable skills, the SSA determines if you can adjust to any other type of work in the national economy. Advanced age (over 55) and limited education significantly improve approval odds under the "medical-vocational grid rules."
Even if you don't meet the exact listing, you may still be approved if the SSA determines your "residual functional capacity" (RFC) is too limited to perform any job. Strong medical documentation from your doctor is crucial for a successful claim. Treatment history, physical exam notes, therapy reports, and consistent follow-ups carry far more weight than symptom descriptions alone. Gaps in treatment, noncompliance with prescribed therapies, or reliance solely on emergency room visits can negatively impact your case. If denied initially, applicants should utilize the appeals process, which includes reconsideration, a hearing before an Administrative Law Judge (ALJ), and potential federal court review. ALJ hearings are statistically where the highest approval rates occur, as vocational experts are cross-examined about hypothetical workers with your exact limitations. For more information, you can review the SSA's guidelines on musculoskeletal disorders.
Life with Osteoarthritis: Challenges and Coping Strategies
Living with severe osteoarthritis requires adaptation and a proactive approach to management. The journey often involves navigating chronic pain, adjusting expectations, and building a sustainable self-care routine that preserves joint function while protecting mental well-being.
Treatment Options to Improve Function
While there is no cure for OA, many treatments can manage symptoms and improve quality of life, potentially preventing or delaying severe disability.
- Exercise & Weight Management: Low-impact exercises like swimming, cycling, and walking strengthen the muscles that support your joints. If you are overweight, losing weight can significantly reduce stress on your knees and hips.
- Medications: Over-the-counter pain relievers (acetaminophen) and nonsteroidal anti-inflammatory drugs (NSAIDs) can help manage pain. Corticosteroid injections may provide temporary relief from severe inflammation.
- Physical and Occupational Therapy: A physical therapist can design a personalized exercise program, while an occupational therapist can recommend assistive devices and modifications to your home to make daily tasks easier.
- Braces and Supports: A knee brace or shoe orthotics can provide stability and help align joints properly.
- Surgery: For advanced cases, joint replacement surgery (hip or knee) can be life-changing. It often dramatically reduces pain and restores mobility, allowing many to resume activities they once thought impossible.
Beyond Basics: Multidisciplinary Pain Management and Lifestyle Adaptations Comprehensive OA care extends far beyond medication and surgery. Multidisciplinary pain clinics integrate physicians, physiatrists, psychologists, and specialized therapists to address the complex nature of chronic joint pain. Cognitive Behavioral Therapy (CBT) has strong evidence supporting its efficacy in chronic pain management, helping patients reframe pain-related catastrophizing, develop coping strategies for flare-ups, and improve sleep hygiene. Mindfulness-based stress reduction (MBSR) and paced breathing exercises can also downregulate the sympathetic nervous system, reducing muscle tension and pain perception.
Nutritional interventions are increasingly recognized as adjunctive therapies. While no specific "OA diet" exists, consuming an anti-inflammatory dietary pattern rich in omega-3 fatty acids (found in fatty fish, flaxseeds, and walnuts), colorful vegetables, whole grains, and healthy fats (like olive oil) may help modulate systemic inflammation. Emerging research on gut microbiome health suggests that dietary fiber and fermented foods might indirectly influence joint inflammation. Regarding supplements, glucosamine and chondroitin show mixed clinical evidence, with some patients reporting modest relief and others experiencing no benefit. Turmeric/curcumin and SAM-e have demonstrated anti-inflammatory and analgesic properties in several trials, but patients should always consult their physicians before starting supplements due to potential drug interactions.
Energy conservation and joint protection principles are essential for daily living. These include pacing activities to avoid post-exertional malaise, using larger or stronger joints to bear loads (e.g., pushing doors with your arm rather than your hand), utilizing adaptive equipment like jar openers, long-handled reachers, and raised toilet seats, and incorporating scheduled rest periods into daily routines. Proper footwear with cushioned soles, rocker-bottom designs, or custom orthotics can dramatically reduce impact forces transmitted through the knees and hips. Heat therapy helps relax stiff muscles and improve circulation, while cryotherapy (cold packs) effectively reduces acute swelling and inflammation during flare-ups.
Frequently Asked Questions about Osteoarthritis and Disability
Q1: Can osteoarthritis qualify for disability benefits?
A: Yes, if your osteoarthritis is severe enough to significantly limit your ability to work or perform daily activities, it can qualify you for disability benefits like Social Security Disability (SSDI) in the U.S. Qualification requires documented medical evidence of advanced joint damage and functional limitations, such as an inability to walk effectively or use your hands for work-related tasks. Consistency in medical care, comprehensive documentation from treating physicians, and a clear demonstration that symptoms persist despite adherence to prescribed treatments are critical. Private disability insurance through employers follows different contractual definitions (often "own occupation" vs. "any occupation"), so reviewing your specific policy language and meeting stated deadlines is essential.
Q2: Is osteoarthritis considered a disability under the ADA (Americans with Disabilities Act)?
A: Yes, osteoarthritis can be considered a disability under the ADA if it substantially limits one or more major life activities, such as walking, standing, lifting, or performing manual tasks. This protection means qualified employees with OA have the right to request reasonable accommodations from their employers to help them perform their job duties. The ADA covers employers with 15 or more employees and applies to state and local governments as well. Remember that the ADA does not require employers to eliminate essential job functions, hire unqualified applicants, or create accommodations that cause significant difficulty or expense. However, the threshold for "undue hardship" is relatively high and assessed on a case-by-case basis.
Q3: What are some reasonable accommodations for osteoarthritis in the workplace?
A: Reasonable accommodations vary based on the job and affected joints. Examples include an ergonomic chair or sit-stand desk for back or hip OA, voice-to-text software for hand OA, more frequent breaks, a modified work schedule, a closer parking space, or the reassignment of physically strenuous tasks. Other effective accommodations may include anti-fatigue floor mats for employees who must stand, temperature-controlled environments to prevent cold-induced stiffness, job restructuring to alternate between sitting and standing tasks, telework options to eliminate painful commuting, and permission to use assistive devices discreetly in the office. The most successful accommodations are those tailored to the specific functional deficits identified by a healthcare provider.
Q4: If I get a knee or hip replacement, will I lose my disability benefits?
A: Potentially. A successful joint replacement that restores significant function can lead to a loss of disability benefits. Agencies like the Social Security Administration typically consider you disabled for a recovery period (often up to one year) and then will review your case. If the surgery allows you to return to work, your benefits may cease. However, if complications arise or your function remains limited, benefits could continue. It is legally required that you report changes in your medical condition or work activity to the SSA. Attempting to work a "trial work period" is permitted under specific SSA guidelines and can help you transition back to employment without immediately losing benefits. Always consult with a disability attorney or advocate before returning to work to understand how it impacts your specific claim status.
Q5: How can I prevent my osteoarthritis from becoming disabling?
A: While not always preventable, you can minimize the impact of OA by staying active with low-impact exercises, maintaining a healthy weight to reduce stress on joints, using assistive devices like canes or braces to offload pressure, and following a treatment plan from your healthcare provider. Early and consistent management can significantly slow the progression of the disease and help maintain function. Additional preventive strategies include avoiding high-impact activities that exacerbate joint wear, incorporating cross-training to prevent repetitive stress on specific joints, addressing biomechanical imbalances with targeted physical therapy, prioritizing high-quality sleep to support tissue repair, and managing systemic conditions like diabetes and hypertension that can worsen inflammatory processes. Proactive symptom tracking and early intervention during minor flare-ups can prevent them from escalating into prolonged functional declines.
Conclusion
So, is osteoarthritis a disability? It certainly can be. When severe, OA is recognized by medical, legal, and social systems as a condition that can cause significant disability.
However, a diagnosis of OA does not automatically mean a life of limitation. Many people manage their condition effectively and lead active, fulfilling lives. If your OA is progressing, know that you have options—from medical treatments and assistive devices to legal protections and disability benefits.
Advocate for yourself by talking to your doctor about a comprehensive treatment plan, discussing accommodations with your employer, and exploring your eligibility for benefits if you can no longer work. By staying informed and proactive, you can navigate the challenges of osteoarthritis and maintain the best possible quality of life. Keep detailed records of your symptoms, treatments, and functional limitations; seek out patient support communities to share coping strategies and reduce isolation; and work with a multidisciplinary healthcare team that views your care holistically. Disability labels, while sometimes necessary for legal and financial support, do not define your worth or your capacity for adaptation and fulfillment. With the right resources, adjustments, and mindset, individuals with osteoarthritis can continue to engage meaningfully with work, family, and community.
Disclaimer: This article is for informational purposes only and does not constitute medical or legal advice. Consult with a qualified healthcare professional for medical concerns and a disability advisor or attorney for legal matters.

About the author
Isabelle Laurent, MD, is board-certified in both internal medicine and rheumatology. She is in private practice in New Orleans, Louisiana, where she has a special interest in treating systemic lupus erythematosus and rheumatoid arthritis in underserved communities.