Tibialis Anterior Tendonitis: A Guide to Causes, Symptoms, and Treatment

Key points
- Tibialis Anterior Muscle: This long, thick muscle is located on the front of your lower leg, running alongside the shinbone (tibia). You can feel it tense when you flex your foot upward.
- Tibialis Anterior Tendon: This tough, fibrous cord connects the muscle to your foot. It crosses the front of the ankle and attaches to the medial cuneiform and first metatarsal bones near your foot's arch.
- Function: Together, the muscle and tendon lift your foot so your toes don’t drag when you walk or run. They also control the foot's motion as your heel strikes the ground, acting as a shock absorber. This explains why activities like running uphill (active lifting) or downhill (controlling descent) can trigger pain.
- Tendon Sheath: The tendon is surrounded by a protective sheath that produces fluid, allowing it to glide smoothly. When overused, both the tendon and its sheath can become inflamed, a condition known as tenosynovitis.
If you’ve ever felt a persistent ache or sharp pain along the front of your ankle or shin, especially after running downhill or long periods of walking, you might be experiencing tibialis anterior tendonitis. This condition involves irritation or inflammation of the tibialis anterior tendon, a key structure that helps you lift your foot and control your stride.
Tibialis anterior tendonitis is a common overuse injury, particularly among runners, hikers, and athletes. It can cause pain and swelling that makes everyday activities uncomfortable. Fortunately, with proper care, most people can recover fully and return to their activities.
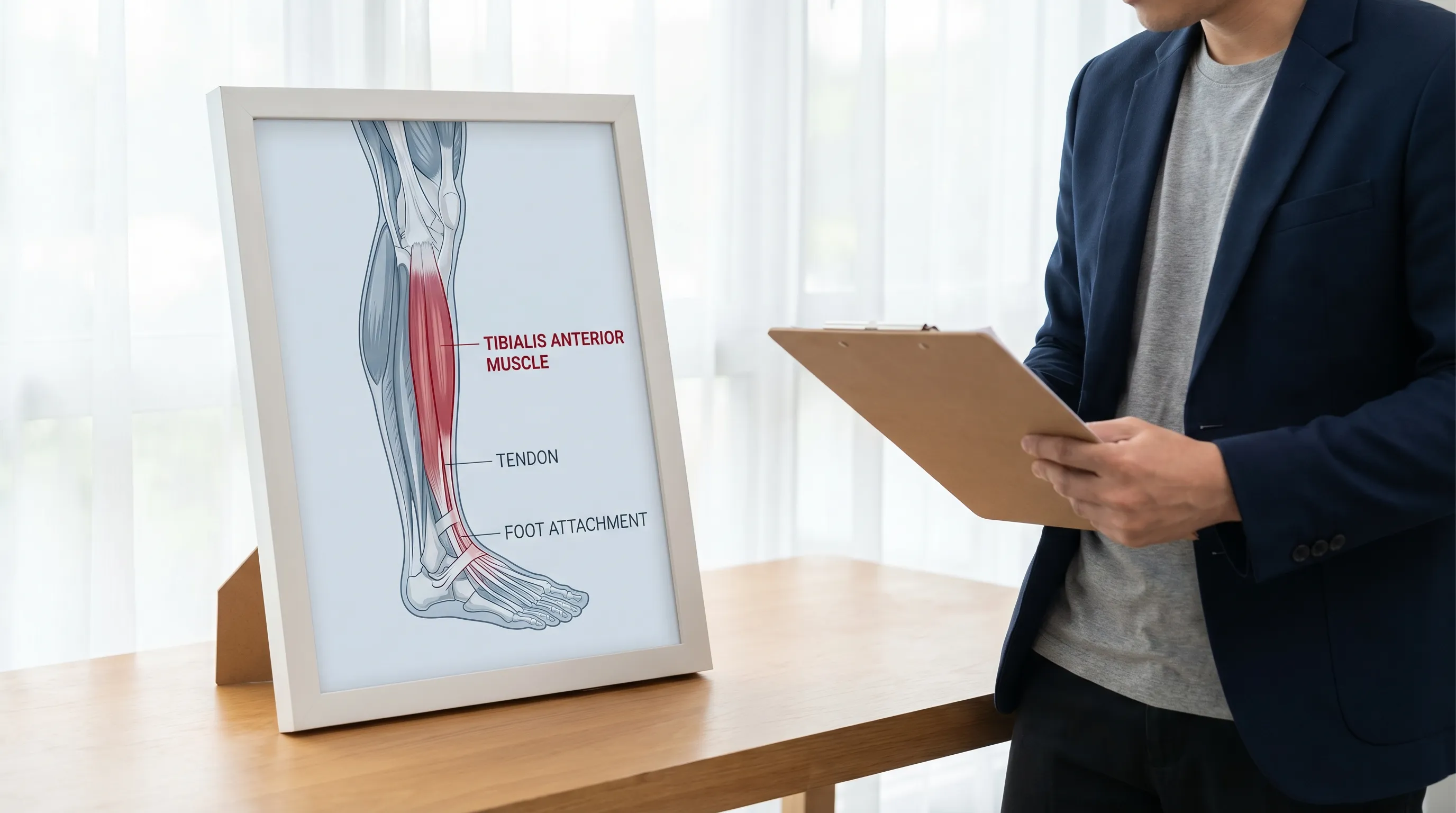 , a crucial movement for walking and running.")
, a crucial movement for walking and running.")
What is Tibialis Anterior Tendonitis?
Tibialis anterior tendonitis is an overuse injury characterized by inflammation or degeneration of the tibialis anterior tendon. This tendon connects the large tibialis anterior muscle on the front of your shin to the bones on the inner side of your foot. This muscle is primarily responsible for dorsiflexion (lifting the front of your foot upward) and also assists with inversion (turning the sole of your foot inward).
When this muscle and tendon are overused or strained—for example, by running long distances downhill or suddenly increasing physical activity—tiny tears and inflammation can develop. The term "tendonitis" means inflammation of a tendon. Over time, acute tendonitis can become a chronic condition known as tendinopathy or tendinosis, where the tendon's collagen fibers begin to degenerate, potentially causing thickening and persistent pain.
Anatomy of the Tibialis Anterior Muscle and Tendon
Understanding the anatomy of your lower leg helps clarify why this condition occurs:
- Tibialis Anterior Muscle: This long, thick muscle is located on the front of your lower leg, running alongside the shinbone (tibia). You can feel it tense when you flex your foot upward.
- Tibialis Anterior Tendon: This tough, fibrous cord connects the muscle to your foot. It crosses the front of the ankle and attaches to the medial cuneiform and first metatarsal bones near your foot's arch.
- Function: Together, the muscle and tendon lift your foot so your toes don’t drag when you walk or run. They also control the foot's motion as your heel strikes the ground, acting as a shock absorber. This explains why activities like running uphill (active lifting) or downhill (controlling descent) can trigger pain.
- Tendon Sheath: The tendon is surrounded by a protective sheath that produces fluid, allowing it to glide smoothly. When overused, both the tendon and its sheath can become inflamed, a condition known as tenosynovitis.
Causes and Risk Factors
Tibialis anterior tendonitis is almost always an overuse injury that develops gradually. Common causes and risk factors include:
- Increased or Repetitive Activity: Suddenly increasing the intensity, duration, or frequency of high-impact activities like running can overload the tendon. Running on hilly terrain, especially downhill, is a frequent culprit.
- Running on Hard or Uneven Surfaces: Concrete and uneven trails increase the stress on the muscles and tendons of the lower leg.
- Poor Footwear: Unsupportive or improperly fitting shoes can contribute to the problem. Stiff soles or tightly laced shoes that press on the front of the ankle (sometimes called "lace bite") can irritate the tendon.
- Lack of Proper Warm-up: Jumping into intense activity without warming up leaves muscles and tendons less flexible and more susceptible to injury.
- Biomechanical Factors: Foot structure and gait can play a significant role. Individuals with flat feet or high arches may place extra stress on the tendon. Overpronation (foot rolling inward) or tight calf muscles can also increase the workload on the tibialis anterior.
- Overuse in Daily Activities: Jobs or hobbies that involve extensive walking on slopes or climbing stairs can trigger the condition.
- Age and Degeneration: In middle-aged or older adults, tendons can degenerate over time (tendinosis), making them more prone to injury or rupture from even minor activity.
Symptoms
Symptoms of tibialis anterior tendonitis typically develop gradually and may include:
- Pain and Tenderness: An ache or sharp pain along the front of the ankle or lower shin, often tender to the touch.
- Pain with Foot Movement: Pain is especially noticeable when lifting your foot upward (dorsiflexion). Walking or running, particularly downhill or on stairs, can be painful.
- Swelling or Redness: Mild swelling, and occasionally redness or warmth, may appear on the front of the ankle along the tendon's path.
- Stiffness: The ankle and foot may feel stiff, especially in the morning or after periods of rest. The pain might decrease with light activity but return after prolonged use.
- Weakness: In more severe cases, you might find it difficult to lift your foot. A "foot drop," where the foot slaps the ground while walking, can occur with a significant injury or rupture but is not typical in mild tendonitis.
- Pain During Specific Activities: Driving (using pedals), hiking on declines, or running downhill often aggravates the pain.
Diagnosis
A healthcare professional like an orthopedic doctor or physical therapist can diagnose this condition. The process usually involves:
- Medical History: Discussing your symptoms, activity levels, and any recent changes in your exercise routine.
- Physical Examination: The clinician will press along the tendon to check for tenderness and ask you to move your foot against resistance to assess pain and strength.
- Gait Analysis: They may watch you walk to observe any abnormalities, such as difficulty lifting your foot.
- Imaging Tests: While often not necessary for a diagnosis, imaging can rule out other conditions.
- X-ray: To check for bone-related issues like stress fractures or bone spurs.
- Ultrasound: To visualize the tendon and detect inflammation, thickening, or tears.
- MRI: Provides a detailed view of soft tissues and is used if a tendon rupture is suspected or the diagnosis is unclear.
Your doctor will also differentiate your symptoms from other conditions like shin splints, extensor tendonitis, or chronic exertional compartment syndrome.
Treatment Options
Most cases of tibialis anterior tendonitis respond well to conservative, non-surgical treatments.
1. Rest and Activity Modification (R.I.C.E.)
The first step is often the R.I.C.E. method:
- Rest: Avoid activities that cause pain. Switch to low-impact exercises like swimming or cycling.
- Ice: Apply an ice pack (wrapped in a cloth) to the front of your ankle for 15-20 minutes several times a day to reduce inflammation.
- Compression: Use an elastic bandage or compression sleeve to minimize swelling and provide support.
- Elevation: Prop your leg up above heart level when resting to help drain excess fluid.
2. Medication
Over-the-counter medications can help manage symptoms:
- NSAIDs (Non-Steroidal Anti-Inflammatory Drugs): Ibuprofen (Advil) or naproxen (Aleve) can reduce pain and inflammation in the short term.
- Topical Anti-inflammatories: Gels or creams like diclofenac can be applied directly to the painful area.
3. Physical Therapy: Stretching and Strengthening
Once the initial pain subsides, rehabilitation exercises are crucial for recovery and prevention.
Stretching Exercises
- Seated Toe Point Stretch: Sit with your legs extended. Gently point your toes away from you and slightly inward to feel a stretch along your shin. Hold for 20-30 seconds and repeat 3-4 times.
- Calf Stretch: Tight calf muscles can contribute to the problem. Stand facing a wall and step one foot back, keeping the heel on the ground. Lean forward to feel a stretch in your calf. Hold for 30 seconds on each side.
For visual guides, you can search YouTube for "How to Stretch Tibialis Anterior".
Strengthening Exercises
- Heel Walks: Stand and lift your toes off the ground, balancing on your heels. Walk forward for 30 seconds. This directly strengthens the tibialis anterior muscle.
- Resistance Band Dorsiflexion: Sit with your legs extended. Loop a resistance band around the top of your foot and secure the other end. Pull your foot toward your shin against the band's resistance. Perform 2-3 sets of 10-15 reps, focusing on a slow, controlled return motion (eccentric strengthening).
- Balance Exercises: Standing on one foot or using a wobble board can strengthen the stabilizing muscles around your ankle.

For exercise demonstrations, search YouTube for "Tibialis Anterior Strengthening Exercises".
4. Footwear and Orthotics
- Proper Footwear: Choose shoes with good arch support and cushioning. If you have flat feet or overpronation, orthotic inserts may help align your foot and reduce strain on the tendon.
- Lacing Techniques: Avoid lacing shoes too tightly over the front of the ankle to prevent direct pressure on the tendon.
5. Progressive Return to Activity
When you start feeling better, reintroduce activity gradually. Follow the 10% rule: increase your workout intensity or duration by no more than 10% per week. Start on flat surfaces before reintroducing hills.
6. Medical Treatments
For persistent cases, a doctor may recommend:
- Corticosteroid Injections: Used cautiously to reduce severe inflammation, as they can weaken the tendon if overused.
- Platelet-Rich Plasma (PRP) Injections: This therapy uses your own blood platelets to promote healing in chronic tendon injuries.
- Immobilization: A walking boot or brace may be used for severe cases to allow the tendon to rest completely.
- Surgery: Rarely needed, surgery is typically reserved for cases involving a significant tendon tear or rupture.
Prevention
Preventing tibialis anterior tendonitis involves managing activity levels and taking care of your lower legs:
- Increase Training Gradually: Follow the 10% rule to allow your body to adapt.
- Wear Proper Footwear: Replace worn-out shoes and choose footwear appropriate for your activity and foot type.
- Warm Up and Stretch: Always warm up before exercise and stretch your shins and calves afterward.
- Strengthen Lower Legs: Regularly perform exercises like heel walks and calf raises.
- Cross-Train: Mix in low-impact activities like swimming or cycling to reduce repetitive stress.
- Listen to Your Body: Address minor aches and pains early with rest and ice to prevent them from becoming serious injuries.
Frequently Asked Questions (FAQs)
What’s the difference between tibialis anterior tendonitis and shin splints?
Shin splints (medial tibial stress syndrome) typically cause diffuse pain along the inner edge of the shinbone (tibia) due to overworked muscles and bone tissue. Tibialis anterior tendonitis involves inflammation of a specific tendon, causing pain at the front of the ankle or top of the foot, which is often aggravated by lifting the foot upwards.
How long does it take to recover from tibialis anterior tendonitis?
Recovery time varies. Mild cases may improve in 2 to 4 weeks with home care. More moderate or chronic cases can take 6 to 8 weeks or longer. Recovery depends on the injury's severity and adherence to rest and rehabilitation.
Can I continue running or exercising with tibialis anterior tendonitis?
It is not recommended to continue high-impact activities like running through the pain, as this can worsen the injury. Switch to low-impact cross-training like swimming or cycling. A gradual return to activity is crucial once you are pain-free during daily activities.
Should I use ice or heat for tibialis anterior tendonitis?
In the acute phase (the first few days), use ice to reduce inflammation and pain. After the initial inflammation subsides, heat can be used before stretching to increase blood flow and promote healing. Some people benefit from contrast therapy (alternating ice and heat).
Do I need to see a doctor for tibialis anterior tendonitis?
You should see a doctor if the pain is severe or worsening, if you have significant swelling, if you have difficulty lifting your foot (foot drop), or if the pain persists for several weeks despite home care. A proper diagnosis is important to rule out other conditions.
Can tibialis anterior tendonitis become a chronic problem?
Yes, if not treated properly, it can become chronic tendinopathy, which involves tendon degeneration. This can lead to persistent pain and an increased risk of a tendon tear. Early intervention and a complete rehabilitation program are key to preventing this.
What kind of stretches or exercises help tibialis anterior tendonitis?
Helpful exercises include gentle stretches for the shin (like the seated toe point stretch) and strengthening exercises such as toe raises (heel walks) and resistance band dorsiflexion. It is also beneficial to stretch the calf muscles and perform balance exercises.
Are there any specific shoes or orthotics recommended for tibialis anterior tendonitis?
The right footwear depends on your foot type. Shoes with good arch support and cushioning are beneficial. If you have flat feet or overpronation, orthotic inserts may help align your foot and reduce strain on the tendon. A podiatrist can provide specific recommendations.
Can tibialis anterior tendonitis lead to a tear in the tendon?
While uncommon, severe or untreated chronic tendonitis can increase the risk of a tendon tear or rupture, especially in older adults or those who continue strenuous activity despite pain. A rupture often causes 'foot drop' and typically requires medical intervention.
Conclusion
Tibialis anterior tendonitis can be a painful setback, but it is highly treatable. The key to recovery lies in early intervention—including rest, ice, and activity modification—followed by a dedicated rehabilitation program of stretching and strengthening. By understanding the causes, you can also take effective steps to prevent it from happening again. Listen to your body, progress gradually, and don't hesitate to seek professional guidance if your symptoms persist. With patience and proper care, you can get back to the activities you love, pain-free.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.

About the author
Samuel Jones, MD, is a board-certified orthopedic surgeon specializing in joint replacement and orthopedic trauma. He is a team physician for a professional sports team and practices at a renowned orthopedic institute in Georgia.