How to Sleep with Calcific Tendonitis: A Complete Guide for Pain-Free Nights

Key points
- Increased Pressure: When you lie down, especially on your side, you place direct and sustained pressure on your shoulder joint. This compresses the inflamed tendon and bursa, significantly amplifying pain signals. Furthermore, the redistribution of bodily fluids when horizontal increases venous congestion in the extremities and upper torso. This fluid shift can cause subtle swelling in the already compromised shoulder capsule, increasing intra-articular pressure and stimulating pain receptors.
- Reduced Anti-inflammatory Hormones: Your body operates on a circadian rhythm. At night, the production of cortisol—a powerful natural anti-inflammatory hormone—dips to its lowest levels to allow melatonin production. This lowers your body's ability to manage inflammation, making you more sensitive to pain. Simultaneously, the drop in cortisol unmasks underlying chemical irritation caused by the resorptive calcium crystals.
- Immobility and Stiffness: While you sleep, your shoulder remains relatively still for long periods. This lack of movement can cause the joint capsule and surrounding muscles to stiffen, leading to a dull, aching pain that intensifies throughout the night. Synovial fluid, which lubricates the joint, becomes thicker and less mobile during prolonged rest, creating a sensation of grinding or catching upon subtle micro-movements.
- Cellular Changes: Research has shown that the affected tendons in calcific tendonitis have a significant increase in new nerve endings and blood vessels (neoinnervation and neovascularization). This makes the area hypersensitive to pain and contributes to chronic inflammation, which doesn't simply turn off at night. These newly formed nociceptors are highly sensitive to mechanical compression, temperature changes, and inflammatory cytokines, meaning even minor shifts during sleep can trigger sharp pain responses.
- Central Sensitization and Sleep Architecture Disruption: Chronic shoulder pain often leads to central sensitization, where the spinal cord and brain amplify pain signals even in the absence of additional tissue damage. When sleep is fragmented, the brain's descending inhibitory pathways—which normally dampen pain perception—become less effective. This creates a vicious cycle: pain disrupts slow-wave and REM sleep, and sleep deprivation lowers your pain threshold, making the next night even more difficult. Understanding these mechanisms validates your experience and highlights why passive rest alone isn't enough. You must actively counteract these physiological shifts through strategic positioning, environmental control, and targeted pre-sleep routines.
If you're battling calcific tendonitis, you know the agonizing reality: the pain doesn't clock out when the sun goes down. In fact, for many, the night brings a new level of throbbing, aching discomfort that makes finding a restful position feel impossible. As one person on a Reddit forum described, it can lead to sitting up in bed all night "with tears in my eyes staring into space."
This severe nocturnal pain isn't just in your head; it's a physiological response to the condition. But there is hope. By understanding why the pain intensifies at night and implementing targeted strategies—from sleeping positions and pre-bed routines to specialized aids and long-term treatments—you can reclaim your nights and get the restorative sleep your body needs to heal.
This guide provides a comprehensive roadmap to sleeping better with calcific tendonitis, blending medical insights with practical, real-world advice. We will walk through the exact mechanisms that cause nighttime flare-ups, step-by-step positioning guides, evidence-based pain management techniques, and long-term clinical interventions designed to eradicate the calcium deposits permanently. Whether you are in the early stages of diagnosis or navigating a stubborn resorptive phase, this article equips you with everything necessary to sleep through the night while actively supporting your shoulder's recovery.
Understanding Calcific Tendonitis and Why It Worsens at Night
Before we can tackle the solution, it's crucial to understand the problem. What exactly is happening in your shoulder, and why does it seem to conspire against you when you're trying to sleep? Calcific tendonitis is not simply a wear-and-tear condition; it is a complex metabolic and inflammatory process that directly impacts how your nervous system perceives pain during periods of rest.
What is Calcific Tendonitis?
Calcific tendonitis is a condition where calcium hydroxyapatite deposits build up in your tendons, most commonly in the supraspinatus or infraspinatus tendons of the rotator cuff. It predominantly affects adults between the ages of 30 and 60, with women experiencing it at a slightly higher rate than men. Interestingly, it is not strictly correlated with repetitive overhead activity or athletic trauma, which sets it apart from many other rotator cuff pathologies. According to the Cleveland Clinic, this process typically occurs in three distinct stages:
- Pre-calcific Stage: Cellular changes occur in the tendon, setting the stage for calcium formation. Fibrocartilaginous metaplasia transforms normal tendon cells into cells that begin depositing calcium. You might begin to feel mild pain with movement, or in many cases, experience zero symptoms during this silent buildup phase.
- Calcific Stage: Calcium crystals are actively deposited in the tendon, forming a paste-like or chalky mass. This stage includes a formative phase and a later resorptive phase, where the body recognizes the foreign material and sends inflammatory cells to reabsorb the deposit. This resorptive phase triggers intense chemical inflammation and is almost universally the most excruciatingly painful part of the condition. The sudden pressure increase within the rigid tendon sheath causes severe nociceptive signaling to the brain.
- Post-calcific Stage: The calcium deposit is fully cleared, and the tendon begins to remodel with healthy, aligned collagen fibers. Pain subsides gradually as inflammation resolves and tissue integrity is restored.
The pain is primarily caused by the inflammation and pressure the calcium deposits create within the tendon, which can lead to a condition known as shoulder impingement. As the tendon swells, it has less room to glide beneath the acromion (the bony roof of the shoulder), resulting in pinching, catching, and severe pain when reaching, lifting, or lying down. Understanding this timeline is critical because the resorptive phase, while agonizing, actually signals the beginning of your body's natural healing process.
The Physiology of Nocturnal Pain
The spike in pain at night is due to a perfect storm of physiological factors that interact to amplify your discomfort precisely when you need rest:
- Increased Pressure: When you lie down, especially on your side, you place direct and sustained pressure on your shoulder joint. This compresses the inflamed tendon and bursa, significantly amplifying pain signals. Furthermore, the redistribution of bodily fluids when horizontal increases venous congestion in the extremities and upper torso. This fluid shift can cause subtle swelling in the already compromised shoulder capsule, increasing intra-articular pressure and stimulating pain receptors.
- Reduced Anti-inflammatory Hormones: Your body operates on a circadian rhythm. At night, the production of cortisol—a powerful natural anti-inflammatory hormone—dips to its lowest levels to allow melatonin production. This lowers your body's ability to manage inflammation, making you more sensitive to pain. Simultaneously, the drop in cortisol unmasks underlying chemical irritation caused by the resorptive calcium crystals.
- Immobility and Stiffness: While you sleep, your shoulder remains relatively still for long periods. This lack of movement can cause the joint capsule and surrounding muscles to stiffen, leading to a dull, aching pain that intensifies throughout the night. Synovial fluid, which lubricates the joint, becomes thicker and less mobile during prolonged rest, creating a sensation of grinding or catching upon subtle micro-movements.
- Cellular Changes: Research has shown that the affected tendons in calcific tendonitis have a significant increase in new nerve endings and blood vessels (neoinnervation and neovascularization). This makes the area hypersensitive to pain and contributes to chronic inflammation, which doesn't simply turn off at night. These newly formed nociceptors are highly sensitive to mechanical compression, temperature changes, and inflammatory cytokines, meaning even minor shifts during sleep can trigger sharp pain responses.
- Central Sensitization and Sleep Architecture Disruption: Chronic shoulder pain often leads to central sensitization, where the spinal cord and brain amplify pain signals even in the absence of additional tissue damage. When sleep is fragmented, the brain's descending inhibitory pathways—which normally dampen pain perception—become less effective. This creates a vicious cycle: pain disrupts slow-wave and REM sleep, and sleep deprivation lowers your pain threshold, making the next night even more difficult. Understanding these mechanisms validates your experience and highlights why passive rest alone isn't enough. You must actively counteract these physiological shifts through strategic positioning, environmental control, and targeted pre-sleep routines.
Immediate Strategies for a Better Night's Sleep
While long-term treatment is key, you need relief tonight. These immediate strategies focus on positioning and pre-bed routines to minimize pain and help you fall asleep. Implementing these techniques requires consistency, as your neuromuscular system needs time to adapt to new sleep habits.
Finding the Right Sleeping Position
Your sleeping posture is the single most important factor you can control. The goal is to keep the shoulder in a neutral, supported, and pressure-free position. Maintaining this alignment throughout the night reduces strain on the rotator cuff, prevents impingement, and minimizes nocturnal fluid accumulation in the joint.
The Best Position: On Your Back
Sleeping on your back is widely recommended by orthopedic specialists as it places the least amount of stress on the shoulder joint. It allows for optimal spinal alignment and evenly distributes weight across the largest surface area of the body.
- How to do it: Lie flat on your back. To enhance comfort and support, place a small, thin pillow or rolled-up towel under your affected arm or elbow. This slight elevation prevents the shoulder from rotating inward or dropping back, which can strain the inflamed tendon. Keep your hand resting comfortably on your abdomen or by your side with the palm facing down to promote external rotation relief.
- Pro-Tip: Placing another pillow under your knees can help flatten your lower back, reducing lumbar strain and making the back-sleeping position more comfortable if you're not used to it. Additionally, if your affected arm tends to roll backward, tuck a second folded towel along your side to act as a physical barrier, training your body to stay aligned.
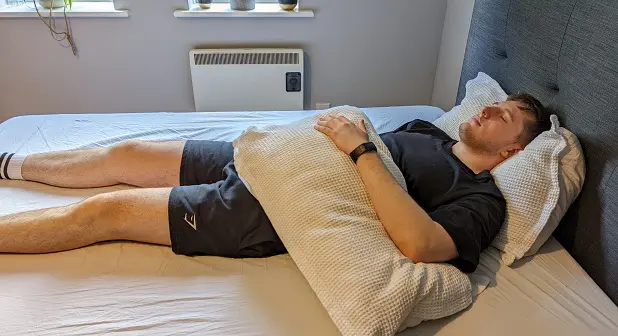 Image Source: Resilience Orthopedics
Image Source: Resilience Orthopedics
The Second-Best Position: On Your Unaffected Side
If you are a dedicated side-sleeper, you can still find a comfortable position by sleeping on your non-painful side. Many patients find this the most sustainable compromise during the acute resorptive phase.
- How to do it: Lie on your unaffected side. Hug a large pillow (a body pillow works exceptionally well) in front of your chest. Rest your affected arm entirely on top of this pillow, ensuring the entire length from hand to elbow is supported. This "pillow wall" supports the weight of your arm and keeps the shoulder in a neutral, open position, preventing it from slumping forward and compressing the subacromial space.
- Pro-Tip: Place a firm pillow between your knees to help keep your spine and pelvis aligned. This prevents your upper body from twisting forward during the night, which is a common subconscious habit that often rolls the affected shoulder into an impinged position. Choose a pillow with adequate loft so that your head and neck remain in a straight line with your spine, avoiding compensatory strain.
Positions to Avoid
- On your affected shoulder: This is the most important rule. Lying directly on the painful shoulder will compress the calcium deposits and inflamed tissues, restricting local blood flow and triggering severe nociceptive feedback. It also prevents the natural drainage of inflammatory exudate, prolonging morning stiffness.
- On your stomach: Stomach sleeping often forces one arm up and under the pillow, placing the shoulder in extreme internal rotation and forward flexion for hours. This position maximizes subacromial impingement and places tremendous shear stress on the anterior capsule. It also strains the cervical spine, potentially referring tension into the trapezius and shoulder girdle.
- The "Halo" Position: Avoid sleeping with your hands tucked behind or above your head. While this feels relieving for some conditions, it narrows the subacromial space and can aggravate tendon compression in calcific tendonitis.
Pre-Bed Pain Management Routine
Creating a simple 30-minute routine before you try to sleep can dramatically reduce your pain levels and lower sympathetic nervous system arousal, making it easier to transition into restorative sleep stages. Sleep hygiene fundamentals should also be integrated: maintain a consistent bedtime, limit blue light exposure 60 minutes before sleep, and keep bedroom temperature between 60-67°F (15-19°C) to naturally facilitate the onset of deep sleep cycles.
The Great Debate: Heat vs. Ice Before Bed
Conflicting advice abounds, but the best choice depends on your specific symptoms that day and the stage of your condition.
- Use Ice (Cryotherapy): Apply an ice pack wrapped in a thin towel for 15-20 minutes if you're experiencing a sharp, acute flare-up or if your shoulder feels hot and inflamed after an active day. As recommended by Medical News Today, ice helps constrict blood vessels, numbing the pain, reducing swelling, and slowing nerve conduction velocity, which temporarily decreases pain signaling to the brain. For optimal results, use ice packs that contour to the shoulder anatomy rather than rigid rectangular packs that leave pressure gaps.
- Use Heat (Thermotherapy): Apply a heating pad or warm compress for 15-20 minutes if your primary symptom is chronic stiffness, muscle guarding, and a dull, muscular ache. Heat increases local blood flow, delivers oxygen and nutrients to the healing tendon, and helps relax tight muscles surrounding the joint like the levator scapulae and upper trapezius. Heat also stimulates mechanoreceptors, which can override pain signals via the gate control theory. Never fall asleep with a heating pad on to avoid thermal burns.
- Contrast Therapy: For some patients, alternating 3 minutes of warm compress with 1 minute of cold, repeated three times, ending on cold, can effectively pump inflammatory fluids out of the tissue while soothing nerve endings.
Over-the-Counter Pain Relief
Taking a non-steroidal anti-inflammatory drug (NSAID) like ibuprofen or naproxen about 30-60 minutes before bed can help reduce inflammation and pain, giving you a crucial window to fall asleep. Timing is essential: taking the medication too early means peak blood concentration will occur before you're in bed, while taking it too late delays its onset. Acetaminophen can also be used as an adjunct for pain relief, though it lacks anti-inflammatory properties. Always consult with your doctor before starting any new medication, especially if you have gastrointestinal, renal, or cardiovascular considerations. Additionally, consider topical NSAID gels (like diclofenac 1%) applied directly over the anterior and lateral shoulder. Topical formulations achieve high local tissue concentrations with minimal systemic absorption, significantly reducing the risk of gastric irritation while providing targeted overnight relief.
Gentle Stretches and Exercises
Gentle, pain-free range-of-motion exercises can help combat stiffness before bed by maintaining joint capsule elasticity and preventing nocturnal adhesive capsulitis. Avoid any movements that cause sharp pain. A physical therapist can provide a safe and effective stretching routine tailored to you, but generally, the following are beneficial:
- Pendulum swings: Lean forward slightly, let your affected arm hang loosely, and gently swing it in small circles using your body's momentum.
- Scapular retractions: Gently squeeze your shoulder blades together and down to improve posture and relieve anterior shoulder tension.
- Cross-body stretch: Use your unaffected arm to gently pull the affected arm across your chest until you feel a mild stretch in the posterior shoulder.
- Sleeper stretch (modified): Lie on your unaffected side with the affected arm bent at 90 degrees. Gently use your good hand to guide the affected forearm toward the mattress. Stop immediately if sharp pain occurs. Hold each gentle movement for 15-20 seconds, repeating 2-3 times. The goal is lubrication, not stretching to the end range. Avoid aggressive overhead reaching before bed, as it can compress the subacromial bursa and trigger rebound inflammation.
Mindfulness and Relaxation Techniques
Pain and anxiety about sleep create a vicious cycle known as psychophysiological insomnia. The anticipation of pain heightens muscle tension and keeps the central nervous system in a hyper-aroused state, making sleep onset nearly impossible. Mindfulness techniques can help break this cycle. A 2018 study found that daily meditation practice increased pain tolerance in injured athletes by altering pain perception in the anterior cingulate cortex and insula. Try a guided meditation app, diaphragmatic breathing exercises (4-7-8 technique), or a progressive muscle relaxation body scan to calm your nervous system and promote parasympathetic dominance. Cognitive Behavioral Therapy for Insomnia (CBT-I) has also demonstrated high efficacy in patients with chronic musculoskeletal pain, helping to reframe maladaptive sleep beliefs and establish sustainable sleep routines.
Optimizing Your Sleep Environment with Specific Aids
Sometimes, your regular pillows aren't enough. Investing in specialized sleep aids can provide the targeted support your shoulder needs, turning your bed into a therapeutic recovery space. The right environment doesn't just mask pain; it actively prevents the micro-traumas that occur during unconscious position changes.
Choosing the Right Pillows for Support
The goal is to fill anatomical gaps and maintain skeletal alignment throughout all sleep cycles.
- Pillow Material: Memory foam and latex pillows are often best as they contour to your body and provide consistent support without collapsing like softer down or fiberfill pillows. High-density memory foam specifically responds to body heat and weight, cradling the joint without bottoming out. Buckwheat hull pillows are another excellent option, offering firm, adjustable support that doesn't compress overnight.
- Wedge Pillows: A wedge pillow elevates your entire torso, creating a semi-upright sleeping position similar to a recliner. This uses gravity to help reduce pressure and inflammation in the shoulder joint by decreasing venous return pressure to the upper extremity and minimizing acid reflux, which can sometimes mimic or exacerbate shoulder and chest discomfort.
- Body Pillows: As mentioned for side-sleepers, a long body pillow is excellent for supporting the top arm and preventing the shoulder from collapsing forward. Look for one at least 48 inches long with a firm yet compressible fill to provide structural support all night.
- Pillow Placement Strategy: When lying on your back, place a flat, medium-loft pillow under the elbow of the affected arm so the entire upper arm is elevated to roughly a 45-degree angle from your torso. This takes tension off the supraspinatus tendon and opens the subacromial space. For side sleepers, use a pillow with 4-6 inches of loft under the head to keep the cervical spine parallel to the mattress, preventing lateral neck strain that can refer pain into the trapezius and upper shoulder.
 Video Source: Tone and Tighten on YouTube
Video Source: Tone and Tighten on YouTube
Using a Shoulder Brace for Stability
A shoulder brace worn at night can offer significant benefits, particularly during the severe resorptive phase or immediately post-procedure:
- Stabilization: It gently holds the shoulder in a stable, supported position, preventing you from moving into a painful position during REM sleep when natural muscle paralysis (sleep atonia) occurs but micro-movements still happen.
- Pain Reduction: By reducing strain on the injured tissues and limiting unnecessary joint excursion, a brace can help alleviate inflammation and discomfort, allowing the inflammatory cascade to settle.
- Types: Options range from simple compression sleeves that provide light proprioceptive feedback to more structured immobilizing slings or abduction braces, which keep the arm slightly away from the body. The latter is often recommended post-lavage or post-surgery to maintain optimal tendon healing tension.
- Important Considerations: Prolonged use of rigid braces can lead to muscle atrophy and joint stiffness. Always follow your physician's or physical therapist's guidelines on duration and weaning. Ensure the brace is snug but not restrictive, checking for signs of impaired circulation like tingling, cold fingers, or bluish discoloration before settling in for the night. Keep the skin underneath clean and dry to prevent fungal or bacterial overgrowth in warm, occluded environments. If your skin becomes irritated, apply a barrier cream like zinc oxide or switch to a moisture-wicking, seamless cotton liner beneath the brace.
When to Consider a Recliner
For nights with unbearable pain or during recovery from an invasive procedure, sleeping in a recliner can be a lifesaver. The elevated position naturally mimics a modified Trendelenburg posture that minimizes fluid pooling and mechanical compression.
- Benefits: The semi-upright position minimizes direct pressure on the shoulder, naturally restricts harmful rotational movement, and keeps the thoracic cavity expanded for deeper diaphragmatic breathing.
- How to Optimize:
- Neck Support: Use a contoured travel pillow or U-shaped memory foam pillow to keep your head and cervical spine neutrally aligned, preventing lateral strain that refers pain to the trapezius and shoulder girdle.
- Lumbar Support: Place a small lumbar cushion or rolled towel behind your lower back to maintain the natural lumbar lordosis, preventing sacral pressure and mid-back fatigue.
- Arm Support: Use pillows or a lap desk to support both arms at heart level, ensuring your affected shoulder is in a relaxed, slightly abducted and externally rotated neutral position. Keep a lightweight blanket over the torso to maintain core temperature, as reclining in a cool room can cause muscle guarding.
- Ergonomic Transition: Recliners are excellent for short-term acute phases but are not ideal for long-term sleep due to reduced deep sleep time. Transition back to a horizontal bed as pain allows, gradually decreasing the incline over several nights.
Mattress Selection and Firmness Considerations
While often overlooked, your mattress foundation plays a critical role in nocturnal shoulder pain. A mattress that is too soft allows your torso to sink excessively, forcing your spine out of alignment and compressing the shoulder joint against the bed surface. Conversely, an overly firm mattress creates high pressure points on the hips and shoulders. A medium-firm mattress with a responsive comfort layer typically offers the best compromise, providing adequate support while contouring enough to distribute weight evenly. If replacing your mattress isn't feasible, consider adding a 2-inch gel-infused memory foam or latex topper to improve pressure relief and micro-climate temperature regulation. Mattress toppers should be rotated regularly to prevent material breakdown and maintain consistent support.
Long-Term Solutions for Lasting Relief (and Better Sleep)
While the strategies above provide immediate relief, the ultimate path to consistently pain-free sleep is to treat the underlying condition. Nighttime positioning is a bridge, not a permanent fix. Addressing the calcium deposit itself breaks the inflammatory cycle and restores normal sleep architecture.
- Extracorporeal Shockwave Therapy (ESWT): This non-invasive treatment uses high-energy sound waves to break down the calcium deposits into smaller fragments, which the body then naturally reabsorbs. The acoustic waves also stimulate angiogenesis and tissue regeneration, effectively jumpstarting the healing process in chronic, stagnant deposits. Clinical success rates often range from 60-80%, typically requiring 3 to 5 weekly sessions. Some patients experience temporary soreness post-treatment, so scheduling sessions earlier in the week can prevent weekend sleep disruption. Low-energy radial shockwave therapy is generally well-tolerated, while focused high-energy variants may require local anesthesia but offer faster deposit breakdown.
- Ultrasound-Guided Needling (Lavage/Barbotage): A minimally invasive in-office procedure where a clinician uses real-time ultrasound imaging to precisely guide a needle into the deposit. Sterile saline solution is then repeatedly aspirated and injected to mechanically flush out the calcium paste. This provides rapid decompression and dramatic pain relief, often within 48 hours. A small amount of corticosteroid may be injected afterward to control post-procedural inflammation, significantly improving sleep quality in the immediate recovery period. Post-lavage, patients are advised to avoid heavy lifting for 1-2 weeks while the needle tract heals and to perform prescribed pendulum exercises to prevent capsular tightening.
- Physical Therapy: Crucial for restoring full range of motion, strengthening the dynamic stabilizers of the shoulder (rotator cuff and scapular stabilizers), and improving thoracic mobility and posture to prevent recurrence. A structured PT program progresses from pain management and gentle mobilization to eccentric strengthening and eventual functional retraining. Addressing postural imbalances like rounded shoulders or forward head posture reduces anterior capsule tension and prevents future impingement. Therapists often integrate dry needling, manual soft tissue mobilization, and neuromuscular re-education to restore proper scapulohumeral rhythm, which is frequently disrupted in patients guarding against calcific pain.
- Surgery: In persistent, calcification cases that fail conservative management, an orthopedic surgeon may recommend an arthroscopic procedure to manually visualize and remove the calcium deposit. The surgeon will also perform a subacromial decompression if bone spurs are present, creating more space for tendon gliding. Post-operative recovery requires strict adherence to a rehabilitation protocol, with sleep positioning playing a vital role in graft and tendon healing over the following 6-12 weeks. Arthroscopic removal boasts high success rates (90-95%) for eliminating pain, though postoperative stiffness requires diligent rehabilitation to restore overhead mobility.
- Metabolic and Nutritional Considerations: Emerging research suggests that calcific tendonitis may have a metabolic component, with associations to thyroid dysfunction, diabetes, and vitamin D metabolism irregularities. Maintaining optimal vitamin D and calcium levels (under medical guidance), managing blood sugar, and incorporating an anti-inflammatory diet rich in omega-3 fatty acids, leafy greens, and antioxidants can support overall tissue health and modulate systemic inflammatory markers. Supplementation with high-quality fish oil (EPA/DHA), curcumin, and bromelain has shown promise in reducing tendon inflammation and improving pain scores in clinical trials. Hydration also plays an underappreciated role; well-hydrated connective tissues are more resilient and less prone to micro-trauma. Limiting processed foods, refined sugars, and excessive alcohol intake can further dampen systemic inflammatory pathways that exacerbate nocturnal pain flares.
Discuss these options with your doctor or orthopedic specialist to create a tiered treatment plan that addresses the root cause of your pain. Combining procedural intervention with consistent rehabilitation and sleep hygiene offers the highest probability of returning to uninterrupted rest.
When to See a Doctor
While home care and conservative management can be highly effective for symptom relief, it's important to seek professional medical advice when the pain interferes with daily function or sleep quality for an extended period. Calcific tendonitis can closely mimic other serious shoulder pathologies, and an accurate diagnosis is essential for targeted treatment. According to the UK's National Health Service (NHS), you should schedule an appointment if:
- The pain does not improve within two to four weeks of consistent self-care and modified activity.
- The pain is severe, sudden, or the result of a significant traumatic injury.
- You are having difficulty with basic daily activities like dressing, reaching, or carrying light objects.
- You experience night sweats, unexplained weight loss, fever, or redness and warmth over the joint, which could indicate an infectious process rather than calcific deposition.
- You notice visible deformity, profound weakness (inability to lift the arm at all), or persistent numbness/tingling radiating down the arm, which may suggest nerve compression or a concurrent rotator cuff tear.
A doctor will typically begin with a thorough physical examination assessing range of motion, strength, and specific impingement signs. Imaging is the gold standard for confirmation. Standard X-rays clearly reveal calcium density and exact location within the tendon. Ultrasound provides dynamic assessment, allowing the clinician to observe tendon gliding in real-time and identify coexisting bursitis. MRI may be ordered if there is suspicion of a full-thickness tendon tear or complex soft tissue involvement. Differential diagnoses often include adhesive capsulitis (frozen shoulder), glenohumeral osteoarthritis, biceps tendinopathy, and cervical radiculopathy (C5-C6 nerve root compression), which can present with remarkably similar shoulder and nocturnal pain patterns.
Once diagnosed, your healthcare provider can recommend the most appropriate course of action, whether that involves supervised physical therapy, pharmacological intervention, minimally invasive lavage, or surgical consultation. Early professional involvement often shortens the duration of the painful resorptive phase and prevents secondary complications like adhesive capsulitis (frozen shoulder) or compensatory cervical strain. A multidisciplinary approach involving orthopedists, physical therapists, and sleep medicine specialists yields the best long-term outcomes for chronic tendon pathology.
References
- Calcific Tendonitis: Symptoms, Causes, & Treatment. (2021, August 12). Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/21638-calcific-tendonitis
- Martin, L. (2024, March 13). How to sleep with calcific tendonitis: Tips and more. Medical News Today. https://www.medicalnewstoday.com/articles/how-to-sleep-with-calcific-tendonitis
- Mehta, P. (2025, July 4). How To Sleep With Shoulder Pain, With Examples & Pictures. Resilience Orthopedics. https://www.resilienceorthopedics.com/shoulder/sleep-with-shoulder-pain/
- Calcific tendonitis of the shoulder. (n.d.). NHS. https://www.nhs.uk/conditions/shoulder-pain/
- Calcific tendinitis pain and phases - Please share your experience. (2022). Reddit. https://www.reddit.com/r/RotatorCuff/comments/16mqpbc/calcific_tendinitis_pain_and_phases_please_share/
Frequently Asked Questions
How long does calcific tendonitis pain typically last at night?
The duration of severe nocturnal pain varies depending on the stage of the condition. The intense resorptive phase, which causes the worst nighttime flare-ups, typically lasts anywhere from 2 to 6 weeks. However, the entire lifecycle of the calcium deposit, from initial formation to complete reabsorption, can take several months to over a year. During the resorptive window, nighttime pain is common but will gradually decrease in frequency and intensity as the inflammatory process subsides. Consistent use of nighttime positioning, anti-inflammatory strategies, and medical interventions can significantly shorten this uncomfortable period.
Can I use a heating pad on my shoulder all night?
No, you should never leave a heating pad on your shoulder unattended or fall asleep with it turned on. Doing so poses a significant risk of thermal burns, especially since the numbing effect of prolonged heat can prevent you from feeling when your skin is overheating. Instead, apply dry or moist heat for 15-20 minutes before bedtime to relax the muscles and increase circulation, then remove it completely. If you find that heat is the only thing that helps you stay comfortable through the night, consider using a microwavable wheat bag or a self-heating therapeutic wrap designed to cool down gradually and maintain a safe temperature without an electrical cord.
Is it better to immobilize my shoulder completely at night with a sling?
Complete immobilization with a rigid sling is generally not recommended for long-term nighttime use unless specifically prescribed by your surgeon post-procedure. While a sling can provide short-term relief during acute, unbearable flare-ups by taking the weight of the arm off the joint, prolonged immobilization can lead to adhesive capsulitis (frozen shoulder), muscle atrophy, and increased morning stiffness. Instead, opt for soft supportive pillows, a mild compression sleeve, or an adjustable abduction pillow that maintains a neutral, functional position while still allowing gentle, safe movement and healthy blood flow to the tissues.
Should I change my mattress to help with shoulder pain?
If your mattress is over 8-10 years old, visibly sagging, or causing you to wake up with aches, replacing it or adding a high-quality mattress topper can significantly improve sleep quality for shoulder pain. A medium-firm surface with adequate pressure-relieving properties prevents your shoulder from sinking too deeply or bearing excessive localized weight. If a full mattress replacement isn't feasible, a 2 to 3-inch memory foam or latex topper can redistribute weight more evenly and reduce pressure points on the acromion and surrounding musculature. Pair this with a supportive pillow system to ensure your spine remains in a straight, neutral line.
Will exercising my shoulder during the day make nighttime pain worse?
It depends entirely on the type, intensity, and timing of the exercise. Gentle, controlled range-of-motion exercises and light stretching during the day actually improve nocturnal symptoms by promoting synovial fluid circulation, preventing stiffness, and strengthening the dynamic stabilizers. However, aggressive strengthening, heavy lifting, repetitive overhead motions, or exercising too close to bedtime can trigger inflammatory flare-ups and worsen night pain. Follow the 24-hour pain rule: if your pain increases significantly during sleep after daytime activity, you may have overexerted the tendon. Scale back the intensity, focus on pain-free movements, and ensure you are allowing at least 48 hours of recovery between targeted strengthening sessions.
Conclusion
Navigating the sleepless nights caused by calcific tendonitis is undeniably challenging, but it is also highly manageable with a systematic, multi-faceted approach. The severe nocturnal pain you experience is not a permanent state; it is a direct result of physiological changes, inflammatory cascades, and positional pressure that can be effectively countered. By prioritizing strategic sleeping positions—favoring your back or unaffected side with proper pillow support—you immediately reduce mechanical stress on the inflamed tendon. Complementing this with a targeted pre-bed routine of appropriate thermal therapy, carefully timed medication, gentle mobility work, and nervous system regulation creates a physiological environment conducive to rest.
Furthermore, understanding that these sleep modifications are a temporary bridge while you address the root cause through medical intervention is crucial. Whether your path forward involves extracorporeal shockwave therapy, ultrasound-guided lavage, structured physical therapy, or surgical removal of the calcium deposits, consistent collaboration with your healthcare provider will accelerate your recovery. Do not endure chronic sleep deprivation, as it impairs tissue healing, lowers pain tolerance, and disrupts overall metabolic health. Implement the positioning techniques tonight, optimize your sleep environment, and take the proactive steps toward professional treatment. With patience, precise management, and targeted therapy, pain-free nights and full shoulder function are well within your reach.

About the author
Samuel Jones, MD, is a board-certified orthopedic surgeon specializing in joint replacement and orthopedic trauma. He is a team physician for a professional sports team and practices at a renowned orthopedic institute in Georgia.