Craniotomy vs. Craniectomy: Key Differences Explained

Key points
- Removing brain tumors (both cancerous and benign). The goal is maximal safe resection while preserving surrounding neural tissue. Biopsies may guide targeted radiation or chemotherapy.
- Clipping or repairing brain aneurysms to prevent them from rupturing. A tiny titanium clip is placed across the aneurysm neck to stop blood flow into the weakened vessel wall.
- Removing blood clots or hematomas from a head injury or hemorrhagic stroke. Evacuating the clot reduces mass effect and prevents secondary brain injury.
- Treating an arteriovenous malformation (AVM), an abnormal tangle of blood vessels. Surgical excision is often chosen when the AVM poses a high rupture risk.
- Performing epilepsy surgery to remove brain tissue that causes seizures. This is typically considered only after multiple antiseizure medications have failed.
- Obtaining a brain biopsy to diagnose a condition. A small tissue sample helps pathologists determine tumor grade or identify infectious/inflammatory processes.
Craniotomy and craniectomy are two neurosurgical procedures that sound similar but serve very different purposes. Both involve operating on the skull to access the brain, but the key distinction lies in what happens to the piece of skull bone that is removed. Understanding this difference is crucial for patients and families facing brain surgery. The skull, or cranium, acts as a rigid protective casing for the delicate brain tissue, blood vessels, and cerebrospinal fluid (CSF). When pathology occurs inside this confined space, neurosurgeons must carefully navigate complex anatomical and physiological constraints to achieve treatment goals while minimizing collateral damage to neurological function. The decision to perform one procedure over the other is never arbitrary; it is guided by stringent clinical protocols, imaging findings, intracranial pressure measurements, and the underlying disease process.
A craniotomy is a procedure where a section of the skull, called a bone flap, is temporarily removed to access the brain and then replaced at the end of the operation.
A craniectomy is a procedure where a portion of the skull is removed and not immediately replaced, often to relieve life-threatening pressure from a swelling brain. A second surgery, called a cranioplasty, is usually performed later to restore the skull.
This article will explore the key differences between these procedures, including why they are performed, what the surgery entails, and what to expect during recovery. We will also delve into the physiological rationale behind each approach, pre-surgical preparation, rehabilitation pathways, and long-term quality-of-life considerations.
What is a Craniotomy?
A craniotomy is a surgical procedure where a neurosurgeon cuts an opening into the skull (cranium) to access the brain. After the necessary brain surgery is complete—such as removing a tumor or repairing a blood vessel—the bone flap is secured back in its original position, typically with small titanium plates and screws. The term originates from the Greek words kranion (skull) and tome (cutting). Modern craniotomies are highly precise, often utilizing computer-assisted neuronavigation systems, intraoperative magnetic resonance imaging (MRI), and advanced microsurgical techniques. These technologies allow surgeons to plan the optimal surgical corridor, avoid critical blood vessels, and preserve eloquent brain areas responsible for speech, vision, and motor control.
Before a scheduled craniotomy, patients undergo comprehensive preoperative evaluations. This typically includes high-resolution MRI or CT angiography to map the exact location and vascular supply of the lesion. Blood work, coagulation studies, and cardiac clearance are standard. Patients are instructed to discontinue blood-thinning medications, such as aspirin, ibuprofen, warfarin, or certain supplements, usually 7 to 14 days prior to surgery to minimize bleeding risks. Fasting for 8 to 12 hours before the procedure is also mandatory. In some cases, a multidisciplinary team including neurologists, anesthesiologists, and specialized nurses will meet with the patient to optimize medical conditions like hypertension or diabetes, which can impact surgical outcomes and healing.
Why is a Craniotomy Performed?
Craniotomies are often planned (elective) surgeries performed to treat a variety of conditions within the brain, including:
- Removing brain tumors (both cancerous and benign). The goal is maximal safe resection while preserving surrounding neural tissue. Biopsies may guide targeted radiation or chemotherapy.
- Clipping or repairing brain aneurysms to prevent them from rupturing. A tiny titanium clip is placed across the aneurysm neck to stop blood flow into the weakened vessel wall.
- Removing blood clots or hematomas from a head injury or hemorrhagic stroke. Evacuating the clot reduces mass effect and prevents secondary brain injury.
- Treating an arteriovenous malformation (AVM), an abnormal tangle of blood vessels. Surgical excision is often chosen when the AVM poses a high rupture risk.
- Performing epilepsy surgery to remove brain tissue that causes seizures. This is typically considered only after multiple antiseizure medications have failed.
- Obtaining a brain biopsy to diagnose a condition. A small tissue sample helps pathologists determine tumor grade or identify infectious/inflammatory processes.
- Relieving chronic pain or treating trigeminal neuralgia through microvascular decompression, where a blood vessel pressing on a nerve is gently moved and padded.
The specific type of craniotomy is named after the skull bone removed, such as a pterional (frontotemporal), parietal, occipital, or suboccipital craniotomy. Minimally invasive or "keyhole" approaches are increasingly common, allowing surgeons to work through smaller incisions using endoscopic cameras and specialized tubular retractors, which often translates to less tissue trauma and faster recovery.
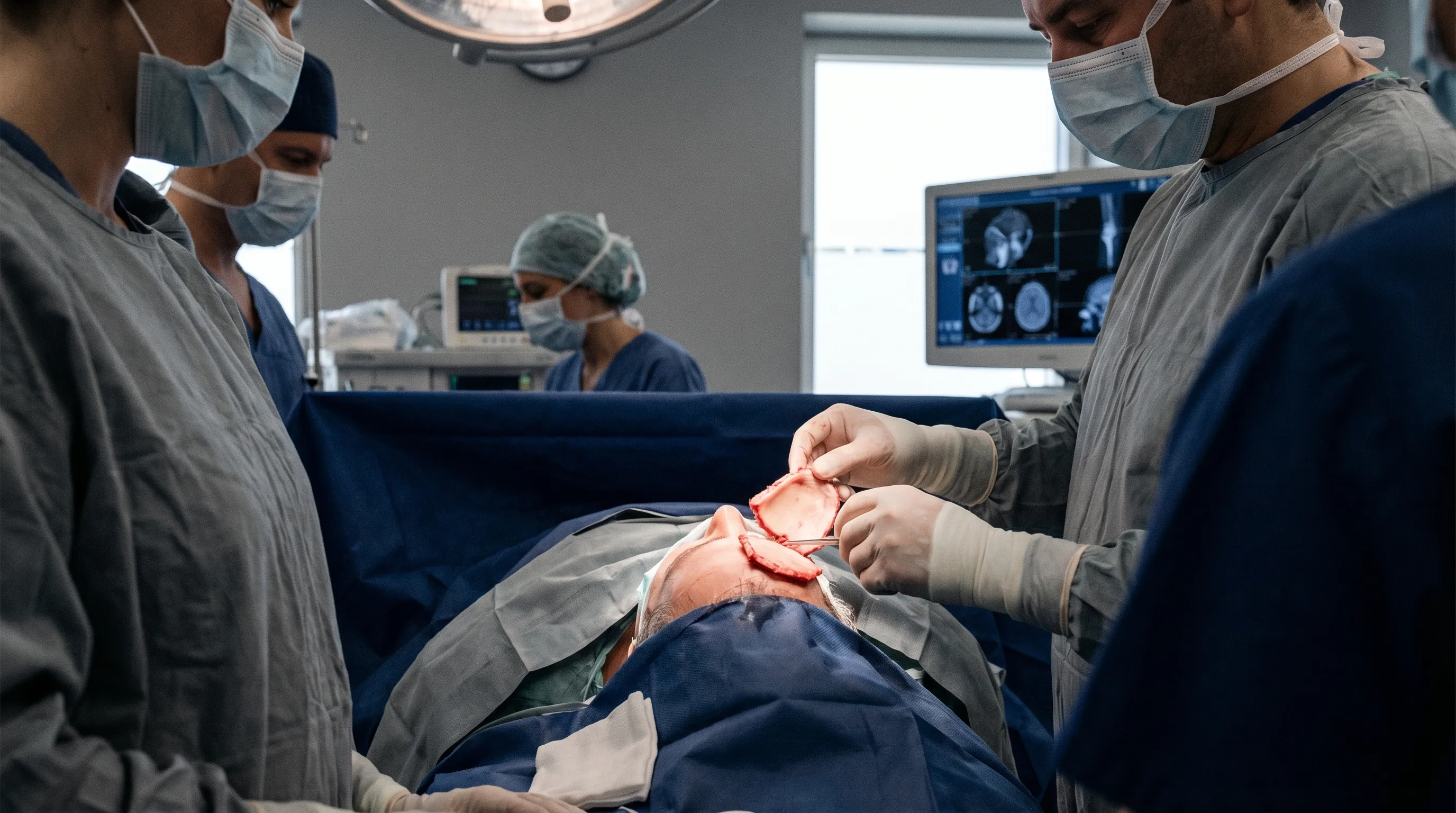
The Craniotomy Procedure
- Anesthesia and Preparation: The patient is placed under general anesthesia. The scalp is shaved or carefully parted, and the surgical site is sterilized with an antiseptic solution. In some cases, an awake craniotomy may be performed, where the patient is conscious during part of the surgery to help surgeons map critical brain functions like speech and movement. During awake mapping, the patient may be asked to read, count, name objects, or move extremities while the surgeon applies mild electrical stimulation to the cortex, ensuring vital pathways remain untouched.
- Incision: The surgeon makes an incision in the scalp, often behind the hairline to minimize visible scarring. The scalp is rich in blood vessels, so meticulous hemostasis is maintained using electrocautery. The skin and muscle layers are reflected back to expose the skull.
- Creating the Bone Flap: A specialized surgical drill is used to create small holes (burr holes) in the skull, and a saw is used to cut between them, creating a removable bone flap. The outer table, diploe (spongy middle layer), and inner table of the bone are carefully separated from the underlying dura mater to prevent cerebrospinal fluid leaks.
- Brain Surgery: The surgeon opens the protective covering of the brain (the dura mater) and performs the necessary procedure. Microscopes, microsurgical instruments, and sometimes intraoperative ultrasound or fluorescent dyes (like 5-ALA for gliomas) are used to enhance visualization and differentiate healthy tissue from pathology. Continuous neurophysiological monitoring (evoked potentials, electroencephalography) tracks real-time brain function.
- Closure: Once finished, the dura mater is stitched closed, often with a synthetic graft or a patch if needed to prevent CSF leakage. The bone flap is put back in place and secured with plates and screws. Titanium is preferred for its biocompatibility, non-corrosive properties, and MRI compatibility. The scalp is then closed with absorbable sutures or surgical staples. A sterile, non-adherent dressing is applied.
Recovery After a Craniotomy
Recovery from a craniotomy typically takes several weeks. The hospital stay is usually 3 to 7 days, with some time spent in the Intensive Care Unit (ICU) for monitoring. During the initial postoperative period, healthcare staff will conduct frequent neurological checks using the Glasgow Coma Scale (GCS) to assess eye opening, verbal response, and motor function. Intravenous lines, urinary catheters, and sometimes temporary surgical drains are used to manage fluid output and reduce the risk of hematoma formation.
Headaches and fatigue are common but improve over time. Steroids (like dexamethasone) may be prescribed temporarily to reduce cerebral edema, while anticonvulsant medications (such as levetiracetam) are often continued for several months to prevent postoperative seizures. Pain is typically managed with acetaminophen or mild opioids, avoiding NSAIDs initially due to bleeding risks. Patients are gradually mobilized by physical therapists, starting with sitting at the edge of the bed and progressing to short hallway walks to prevent blood clots and pneumonia.
Most people can return to light activities within 4-8 weeks, depending on the reason for the surgery and their overall health. Driving is usually restricted until cleared by the surgical team, often requiring a minimum of 3 to 6 months without seizure activity, depending on local regulations. Follow-up imaging is scheduled at 6 weeks, 6 months, and annually to monitor healing and check for any recurrence of the underlying condition. Incision care involves keeping the site clean and dry, avoiding hair dye or harsh chemicals for at least 4 to 6 weeks, and watching for signs of infection such as redness, warmth, drainage, or fever. Cognitive rehabilitation may be recommended if the patient experiences memory lapses, difficulty concentrating, or mood changes, which are often temporary but can benefit from targeted therapy.
What is a Craniectomy?
A craniectomy also involves removing a piece of the skull, but the critical difference is that the bone flap is not immediately replaced. This procedure is most often performed as an emergency, life-saving measure. By leaving a portion of the skull open, a swollen brain has room to expand without being compressed, which can prevent severe brain damage or death. This is often called a decompressive craniectomy. The physiological principle at play is the Monro-Kellie doctrine, which states that the cranial vault contains a fixed volume of brain tissue, blood, and CSF. When one component increases rapidly (such as from hemorrhage or cytotoxic edema), pressure rises exponentially because the rigid skull cannot expand. Removing a large section of bone converts this closed system into an open one, immediately lowering intracranial pressure (ICP) and restoring cerebral perfusion, thereby preventing herniation and irreversible brainstem injury.
Why is a Craniectomy Performed?
Craniectomies are usually performed in urgent situations to manage dangerously high intracranial pressure (pressure inside the skull). Common reasons include:
- Severe Traumatic Brain Injury (TBI): After a major head injury from an accident or fall, the brain may swell significantly. Decompressive craniectomy is considered when ICP remains refractory to maximal medical management (sedation, osmotic agents like mannitol or hypertonic saline, hyperventilation, and barbiturate coma).
- Massive Stroke: A large ischemic or hemorrhagic stroke can cause severe brain swelling (edema). Malignant middle cerebral artery (MCA) infarction is a classic indication, particularly in younger patients, where timely decompression dramatically reduces mortality.
- Brain Hemorrhage: Uncontrolled bleeding in the brain can increase pressure. While hematoma evacuation alone may suffice in smaller bleeds, extensive bleeding with mass effect necessitates bone removal to accommodate post-evacuation swelling.
- Infections: In rare cases, a bone infection (osteomyelitis) may require the removal of the infected skull section. Severe intracranial infections causing refractory edema can also prompt this life-saving step.
- Severe Meningitis or Encephalitis: Inflammatory brain swelling that fails to respond to aggressive medical therapy may occasionally require surgical decompression.
Timing is critical in decompressive craniectomy. Clinical trials, such as the DECRA and RESCUEicp studies, have helped establish guidelines for patient selection, showing that while the procedure saves lives and reduces severe disability in carefully selected populations, functional outcomes can vary widely depending on the extent of the initial brain injury and the speed of intervention.
The Craniectomy Procedure
The initial steps of a craniectomy are similar to a craniotomy. However, after the bone flap is removed and the brain procedure is completed, the bone is not reattached. Instead, it may be cryopreserved in a sterile freezer at a licensed tissue bank or stored in a small pouch in the patient's abdomen to keep it viable for later use. The abdominal subcutaneous pocket method allows the bone to remain in the patient's body, maintaining its sterility and vascular supply, though it carries a small risk of infection or bone resorption. Cryopreservation is highly standardized but requires strict cold-chain logistics.
The dural opening in a craniectomy is typically expanded using a synthetic or bovine pericardial graft to create additional space for brain expansion. This expanded dural sac, or "duroplasty," prevents the brain from herniating through the bone defect. The scalp is then closed over the opening, leaving a soft, sometimes slightly concave or bulging area depending on ICP fluctuations. The surgical site is carefully monitored for wound breakdown, as the tension from brain swelling can compromise scalp healing. Prophylactic antibiotics and meticulous wound care are essential during this phase.
Recovery After a Craniectomy
Recovery after a craniectomy is often long and complex, largely due to the severity of the initial injury or stroke. The immediate focus shifts to neurocritical care, managing cerebral perfusion pressure, preventing complications like ventilator-associated pneumonia, deep vein thrombosis, and stress ulcers. As the patient stabilizes, the rehabilitation phase begins.
- Head Protection: Patients must wear a custom-fitted protective helmet whenever they are out of bed to shield the vulnerable part of the brain from injury. These helmets are custom-molded, lightweight, and designed with adequate ventilation. They are non-negotiable for safety, as even minor bumps can cause catastrophic injury to the unprotected cortex.
- Hospital Stay: The ICU and overall hospital stay are typically longer than for a craniotomy. Transition to acute rehabilitation facilities or specialized neuro-rehab units is common, where therapy is delivered 3 hours daily.
- Rehabilitation: Intensive rehabilitation, including physical, occupational, and speech therapy, is often required to recover functions affected by the brain injury. Neuroplasticity is harnessed through repetitive, task-specific training. Cognitive deficits, fatigue, and emotional lability are common and are addressed through neuropsychological support and counseling for both patients and caregivers.
- Cranioplasty: Once the brain swelling has subsided and the patient is stable (usually after several weeks or months), a second surgery called a cranioplasty is performed. During this procedure, the original bone flap or a custom-made synthetic implant (PEEK, PMMA, or titanium) is used to reconstruct the skull. Modern 3D-printed implants offer exceptional anatomical precision. Cranioplasty not only restores cosmetic appearance but also normalizes cerebrospinal fluid dynamics, improves cerebral blood flow, and often alleviates symptoms associated with the bone defect.
Craniotomy vs. Craniectomy: A Side-by-Side Comparison
| Feature | Craniotomy | Craniectomy |
|---|---|---|
| Bone Flap | Replaced at the end of surgery. | Not replaced immediately; stored for later use. |
| Primary Purpose | To access the brain for planned procedures like tumor removal or aneurysm repair. | To relieve pressure from a swelling brain in emergencies like trauma or stroke. |
| Urgency | Usually a planned (elective) procedure. | Often an emergency, life-saving procedure. |
| Number of Surgeries | Typically one procedure. | Requires at least two procedures: the craniectomy and a later cranioplasty. |
| Post-Op Protection | The skull is intact, providing natural protection. | A protective helmet is required until the skull is repaired. |
| Recovery | Shorter hospital stay; recovery focused on the primary condition. | Longer hospital stay and rehabilitation; recovery focused on the severe brain injury. |
Understanding the Procedure Visually
For a clearer understanding of a craniotomy, this animated video from Nucleus Medical Media demonstrates the surgical steps.

Watch: Craniotomy Surgical Procedure Animation on YouTube
Risks and Complications
Both surgeries carry the general risks associated with any major operation, including infection, bleeding, blood clots, seizures, and adverse reactions to anesthesia. However, a craniectomy carries additional risks due to the missing bone:
- Injury to the brain: The unprotected area is vulnerable to accidental impact. Strict adherence to helmet protocols and caregiver vigilance are paramount.
- Syndrome of the trephined: Some patients experience headaches, dizziness, focal neurological deficits, and cognitive changes due to the missing skull portion. Atmospheric pressure, altered CSF hydrodynamics, and compromised cerebral blood flow contribute to this phenomenon. These symptoms usually resolve after cranioplasty, with many patients reporting noticeable improvement within days of skull reconstruction.
- Fluid buildup or infection at the surgical site. Subgaleal fluid collections or wound dehiscence may require drainage or revision surgery. Deep intracranial infections (meningitis, abscess) are rare but serious.
- CSF Leak: Clear fluid draining from the nose or wound indicates a breach in the dural seal. It often requires bed rest, lumbar drainage, or surgical repair to prevent ascending infection.
- Postoperative Seizures: Irritation to the cerebral cortex during surgery can lower the seizure threshold. Prophylactic antiepileptic drugs are standard, especially for the first 6 to 12 months.
- Deep Vein Thrombosis (DVT) and Pulmonary Embolism (PE): Prolonged immobilization increases clotting risk. Sequential compression devices, early mobilization, and prophylactic anticoagulation (when deemed safe by the surgical team) are routinely employed.
- Cognitive and Emotional Changes: Depending on the surgical site and underlying injury, patients may experience memory impairment, executive dysfunction, depression, or anxiety. A comprehensive neurocognitive assessment and multidisciplinary mental health support are integral to holistic recovery.
Patients should seek immediate medical attention if they experience sudden severe headaches, persistent vomiting, high fever, clear nasal drainage, worsening weakness, speech difficulties, or redness/swelling at the incision site. Early intervention significantly improves outcomes and prevents secondary complications.
Conclusion
The choice between a craniotomy and a craniectomy is not up to the patient but is determined by the specific medical situation. A craniotomy is the standard approach for most planned brain surgeries where the goal is to access and treat a condition without ongoing brain swelling. It offers definitive treatment in a single stage, with the skull's structural integrity immediately restored. A craniectomy is a critical, often life-saving, intervention used in emergencies to give a swelling brain room to expand and prevent further damage. While it necessitates a staged approach and prolonged rehabilitation, it fundamentally shifts the prognosis from fatal or severely disabling to survivable and potentially functional.
While both are serious procedures, advances in neurosurgery have made them safer and more effective. Innovations like image-guided navigation, intraoperative neuromonitoring, minimally invasive corridors, and advanced biomaterials for cranial reconstruction continue to improve patient outcomes and quality of life. Postoperative care has also evolved, with standardized neurocritical care pathways and early rehabilitation protocols maximizing neurological recovery. If you or a loved one is facing brain surgery, it is essential to have an open discussion with your neurosurgeon to understand the recommended procedure, its goals, and what to expect during recovery. Preparing a list of questions, designating a healthcare advocate, and enrolling in caregiver support programs can greatly reduce anxiety and improve postoperative compliance. Trust in the multidisciplinary neurosurgical team is vital, as they combine extensive training with cutting-edge technology to navigate the complexities of the human brain.
Frequently Asked Questions
Can I choose between a craniotomy and a craniectomy for my condition?
Generally, patients do not choose between the two procedures, as the decision is strictly dictated by clinical necessity, imaging findings, and physiological parameters. Craniotomy is the default for elective, non-pressurized conditions like tumor removal or aneurysm clipping, where the brain is expected to heal without significant swelling. Craniectomy is reserved for acute, life-threatening intracranial hypertension where leaving the bone in place would compress brain tissue and lead to herniation. Neurosurgeons make this determination based on established clinical guidelines and real-time intraoperative findings. In rare, borderline cases where swelling is anticipated but not yet severe, a surgeon might discuss a prophylactic craniectomy, but this remains highly situational and carefully weighed against surgical risks.
How long can a bone flap survive in the abdomen before cranioplasty?
When a bone flap is stored in a subcutaneous abdominal pocket, it typically remains viable for cranioplasty for 3 to 6 months, though some cases have successfully utilized flaps after longer intervals. The body's tissue environment helps preserve bone viability by providing a degree of vascularization and protecting against desiccation and contamination. However, extended storage can sometimes lead to minor bone resorption, thinning, or fat infiltration, which might affect the structural integrity needed for a perfect cosmetic and protective fit. Cryopreserved bone stored in specialized tissue banks can often be kept for longer periods (up to several years) under strict sterile, temperature-controlled conditions. Ultimately, the timing of cranioplasty is individualized based on the patient's neurological stability, resolution of edema, infection risk, and overall health status.
What is "syndrome of the trephined" and how is it treated?
Syndrome of the trephined, also known as sinking skin flap syndrome, occurs in patients who have undergone a decompressive craniectomy. The atmospheric pressure acting directly on the unprotected brain, combined with altered cerebrospinal fluid flow dynamics and compromised cerebral perfusion, can cause a constellation of symptoms including chronic headaches, dizziness, cognitive slowing, mood disturbances, and even new focal neurological deficits that mimic a stroke. The skin over the defect often appears visibly sunken. Diagnosis is typically clinical and supported by imaging showing paradoxical herniation or midline shift when the patient sits upright. The definitive treatment is cranioplasty, which restores normal intracranial pressure gradients, improves cerebral blood flow, and typically leads to rapid resolution of symptoms, often within days to weeks following skull reconstruction.
Will I have a visible scar or a permanent dent after a craniotomy or craniectomy?
A craniotomy typically leaves a linear scar hidden within the hairline or natural scalp creases. Over time, the scar usually fades significantly, and the replaced bone flap is secured flush with the surrounding skull, so no dent remains. Hair regrowth is generally unaffected, though temporary thinning near the incision can occur. A craniectomy, before cranioplasty, leaves a noticeable indentation where the bone is missing, which is protected by the overlying skin and subcutaneous tissue. Once a cranioplasty is performed, a synthetic or autologous bone graft is contoured precisely to match the patient's natural cranial curvature, effectively eliminating the dent. The surgical scar from the cranioplasty is often placed in the same location as the original incision. While minor irregularities can occasionally be felt under the skin, modern 3D-printed custom implants have dramatically improved cosmetic outcomes, making the defect virtually undetectable to the casual observer.
How soon after brain surgery can I safely return to work and resume normal activities?
The timeline varies drastically depending on the procedure type, the underlying condition, the patient's age, and the physical/cognitive demands of their occupation. After an uncomplicated elective craniotomy, patients may return to sedentary or desk-based work within 4 to 8 weeks, provided fatigue is managed and neurological recovery is on track. Physically demanding jobs, heavy lifting, or roles requiring high-level concentration may require 3 to 6 months or longer. For craniectomy patients, the timeline is extended due to the severity of the initial injury and the mandatory two-stage surgical process. Most patients do not return to work until after cranioplasty and a comprehensive rehabilitation course, often taking 6 to 12 months or more. Driving is typically restricted until the neurosurgeon clears the patient, which usually requires being off sedating medications, demonstrating adequate visual and motor function, and remaining seizure-free for a legally mandated period. A gradual, phased return-to-work program with occupational therapy support is highly recommended to ensure sustainable reintegration without triggering excessive fatigue or cognitive overload.
Additional Resources
For more detailed information, consult these trusted medical sources:
- American Association of Neurological Surgeons (AANS): Patient Information on Craniotomy
- Mayo Clinic: Craniotomy Overview
- Johns Hopkins Medicine: Craniotomy: What to Expect
- MedlinePlus: Craniotomy - Medical Encyclopedia

About the author
David Chen, DO, is a board-certified neurologist specializing in neuro-oncology and stroke recovery. He is the director of the Comprehensive Stroke Center at a New Jersey medical center and has published numerous articles on brain tumor treatment.