Non-Blanchable Erythema: A Warning Sign for Pressure Ulcers

Key points
- What It Is: Reddened skin that does not turn white when you press on it. Healthy red skin will momentarily turn pale (blanch) when pressed.
- Key Sign of Pressure Ulcers: It is the earliest visible sign of a Stage 1 Pressure Injury, indicating that damage is starting beneath the intact skin surface.
- Importance of Early Detection: This persistent redness signals underlying tissue damage from prolonged pressure. If caught early and pressure is relieved, the damage can be reversed. If ignored, it can progress to open wounds (deeper pressure ulcers).
- Who’s at Risk: Individuals with limited mobility, such as those confined to a bed or wheelchair, elderly individuals, and people with conditions like diabetes or spinal cord injuries are particularly vulnerable.
- Prevention is Key: Regular repositioning, keeping skin clean and dry, using supportive cushions or mattresses, and maintaining good nutrition are essential for prevention.
Non-blanchable erythema is a medical term for a red or discolored area on the skin that does not turn white (or “blanch”) when pressed. This finding is a key early warning sign of skin damage, and it is the defining characteristic of a Stage 1 pressure ulcer (also known as a pressure injury or bedsore).
Recognizing non-blanchable erythema is crucial for individuals at risk, such as those who are bedridden or use a wheelchair. Early detection allows for prompt intervention, which can prevent the development of more serious open wounds and complications.
Quick Facts
- What It Is: Reddened skin that does not turn white when you press on it. Healthy red skin will momentarily turn pale (blanch) when pressed.
- Key Sign of Pressure Ulcers: It is the earliest visible sign of a Stage 1 Pressure Injury, indicating that damage is starting beneath the intact skin surface.
- Importance of Early Detection: This persistent redness signals underlying tissue damage from prolonged pressure. If caught early and pressure is relieved, the damage can be reversed. If ignored, it can progress to open wounds (deeper pressure ulcers).
- Who’s at Risk: Individuals with limited mobility, such as those confined to a bed or wheelchair, elderly individuals, and people with conditions like diabetes or spinal cord injuries are particularly vulnerable.
- Prevention is Key: Regular repositioning, keeping skin clean and dry, using supportive cushions or mattresses, and maintaining good nutrition are essential for prevention.
What Is Non-Blanchable Erythema?
Erythema is the medical term for skin redness, which occurs when small blood vessels (capillaries) widen, bringing more blood to the surface. This happens in response to irritation, pressure, or injury.
When you press on a typical red patch of skin, you temporarily push blood out of the vessels. If the area blanches (turns white) and then quickly reddens again when you release, it's called blanchable erythema. This is generally a sign of temporary irritation.
However, if you press on a red area and it does not turn white, this is non-blanchable erythema. It suggests that blood flow is impaired or blood has leaked into the tissue due to damage in the small vessels. The redness is "fixed" and won't disappear with pressure.
In healthcare, non-blanchable erythema on intact skin is the defining feature of a Stage 1 pressure ulcer, the mildest category of pressure-related skin injury.
According to the National Pressure Injury Advisory Panel (NPIAP), a "Stage 1 Pressure Injury is characterized by non-blanchable erythema of intact skin." This means that although the skin has not broken open, the tissue underneath is already injured.
How to Perform a Blanching Test
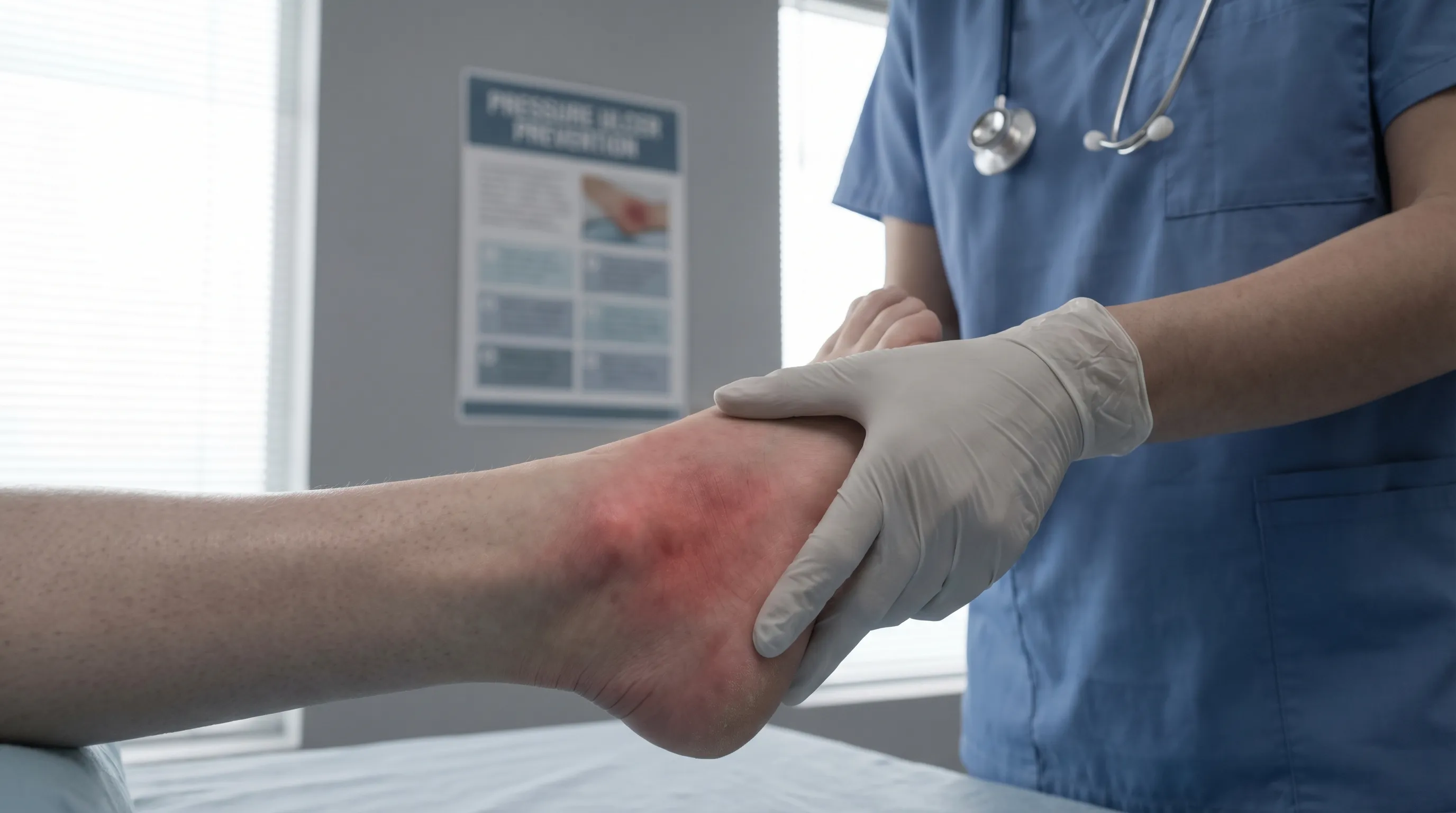
The simplest way to check for non-blanchable erythema is with a blanch test (also called a capillary refill or "press test").
Steps to Perform a Blanch Test:
- Locate the Red Area: Identify a patch of red or discolored skin, typically over a bony area like a heel, hip, or the lower back.
- Apply Gentle Pressure: Using a fingertip, gently press down on the center of the red area. A clear drinking glass can also be used (the "glass test").
- Hold and Observe: Hold the pressure for about 3 seconds, then release.
- Watch for Color Change:
- If the area turns white or pale and then quickly returns to red, the erythema is blanchable (a good sign).
- If the area stays red or discolored and does not fade, it is non-blanchable, indicating potential tissue damage.
On darker skin tones, redness may not be as obvious. The area might appear darker, purple, or bluish. Look for changes in skin texture (firmer or softer) or temperature (warmer or cooler) compared to the surrounding skin.
What Causes Non-Blanchable Erythema?
The most common cause of non-blanchable erythema in a pressure injury context is prolonged pressure on the skin.
- Pressure and Reduced Blood Flow: When a part of the body is pressed against a surface for too long, the pressure squeezes blood vessels, reducing blood flow and depriving tissues of oxygen and nutrients.
- Ischemia and Redness: Initially, when pressure is relieved, blood rushes back, causing temporary, blanchable redness (reactive hyperemia).
- Blood Vessel Damage: If pressure continues, the lack of blood flow damages the tissues and capillaries. Damaged vessels may leak blood into the surrounding tissue or clot. At this point, the redness becomes fixed and non-blanching.
Other contributing factors include:
- Shear and Friction: Sliding down in a bed or chair can stretch and damage deeper tissue and blood vessels.
- Moisture: Skin softened by sweat or incontinence is more prone to injury.
- Bony Prominences: Areas where bones are close to the skin surface are common sites for pressure injuries, including the tailbone, hips, heels, ankles, elbows, and back of the head.
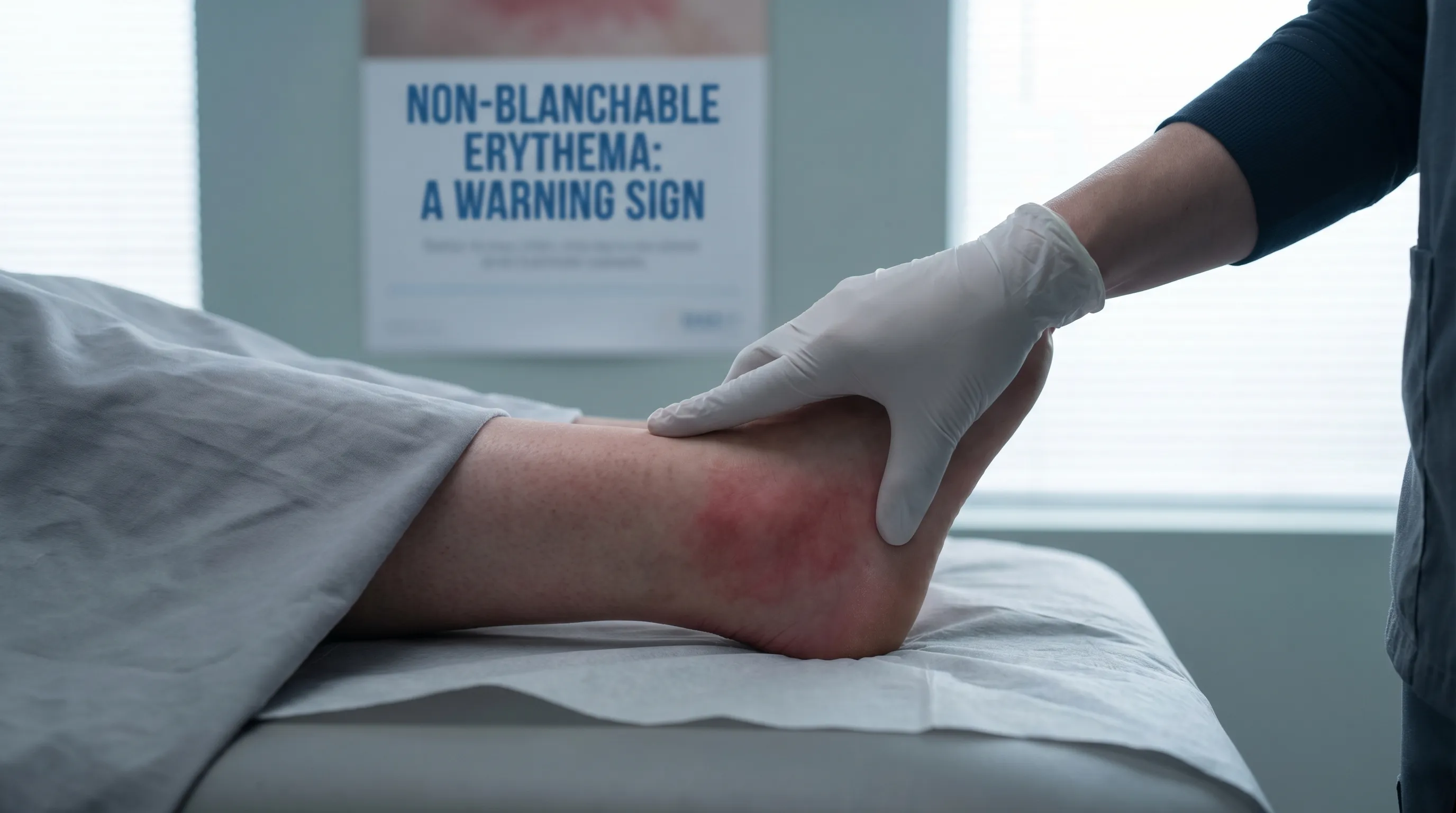
Non-Blanchable Erythema as a Stage 1 Pressure Injury
Non-blanchable erythema of intact skin is the clinical definition of a Stage 1 pressure injury. This is the first and mildest stage in a classification system that ranges up to Stage 4 (most severe).
- Stage 1 (Non-Blanchable Erythema): The skin is intact but has a persistent red or discolored area that does not blanch. It may be painful, firm, soft, warmer, or cooler than surrounding skin. This is a critical warning sign that damage is starting.
- Stage 2 (Partial-Thickness Skin Loss): The skin breaks open, wears away, or forms a blister. The wound is shallow with a pink or red base.
- Stage 3 (Full-Thickness Skin Loss): The damage extends deeper into the tissue, affecting the fat layer beneath the skin, creating a deeper, crater-like wound.
- Stage 4 (Full-Thickness Tissue Loss): The damage is severe, extending down to muscle, bone, or other deep structures.
- Deep Tissue Pressure Injury (DTPI): A severe injury where the skin may be intact but appears deep red, purple, or maroon. It can progress rapidly to a deep wound.
- Unstageable: The depth of the wound cannot be determined because it is covered by dead tissue (slough or eschar).
Catching a pressure injury at Stage 1 is crucial because the damage is often reversible if pressure is promptly and completely removed.
*This video from a certified wound care expert explains how to identify and manage Stage 1 pressure injuries, including a demonstration of the blanch test.*Symptoms and Identification
A person with non-blanchable erythema may exhibit the following signs and symptoms:
- Persistent Redness or Discoloration: Red in lighter skin; purplish, bluish, or darker in darker skin. The color does not fade with pressure.
- Temperature Changes: The area may feel warmer (due to inflammation) or cooler (due to poor circulation) than surrounding skin.
- Texture Changes: The skin may feel firmer or softer than the surrounding tissue.
- Sensation: The area might be tender, painful, or itchy. However, individuals with nerve damage may not feel any pain.
- Intact Skin: In a Stage 1 injury, the skin surface is not broken.
A blanchable red mark typically fades within 30 minutes of pressure relief. Non-blanchable erythema persists for longer, signaling an underlying injury.
Who Is at Risk?
Certain individuals are at a much higher risk of developing pressure-related non-blanchable erythema:
- People Who Are Immobile: Including those who are bedridden, use a wheelchair, or are recovering from surgery.
- Elderly People: Aging skin is thinner, more fragile, and has less natural cushioning.
- People with Diabetes or Neuropathy: Nerve damage can prevent a person from feeling the discomfort that signals them to move. Poor circulation also makes skin more vulnerable.
- Those with Limited Sensation or Cognition: Conditions like spinal cord injuries, dementia, or sedation increase risk.
- Poor Nutrition and Dehydration: Skin health depends on adequate protein, vitamins, and hydration.
- Incontinence: Moisture from urine or feces weakens the skin, making it susceptible to breakdown.
Why Non-Blanchable Erythema Matters: Potential Complications
Ignoring a non-blanching red spot can lead to serious complications:
- Progression to Open Wounds: A Stage 1 injury can quickly worsen to a painful, open sore (Stages 2, 3, and 4).
- Infection Risk: Broken skin allows bacteria to enter, leading to skin infections (cellulitis), bone infections (osteomyelitis), or a life-threatening body-wide infection (sepsis).
- Pain and Suffering: Advanced pressure ulcers are often extremely painful and significantly reduce quality of life.
- Longer Hospital Stays & Healthcare Costs: Treating severe pressure ulcers is difficult, expensive, and can complicate recovery from other illnesses.
Preventing Non-Blanchable Erythema and Pressure Ulcers
Most pressure ulcers are preventable. A helpful mnemonic for prevention is SSKIN:
- S – Surface: Use pressure-redistributing mattresses or cushions (foam, gel, or air).
- S – Skin Inspection: Check the skin daily for any signs of redness or discoloration, especially over bony areas.
- K – Keep Moving: Reposition bed-bound individuals at least every 2 hours and wheelchair users every hour. Encourage weight shifts every 15 minutes if possible.
- I – Incontinence Management: Keep skin clean and dry. Use gentle cleansers and apply barrier creams to protect skin from moisture.
- N – Nutrition and Hydration: Ensure a balanced diet rich in protein, vitamins, and adequate fluid intake.
Additional prevention strategies include:
- Cushioning Bony Areas: Use pillows or foam wedges to "float" heels and prevent knees and ankles from pressing together.
- Avoiding Shear and Friction: Lift, rather than drag, a person when repositioning them in bed.
Managing Non-Blanchable Erythema (Treatment of Stage 1)
If you identify non-blanchable erythema, act quickly:
- Relieve Pressure Immediately: Reposition the person to completely offload the affected area.
- Do Not Massage the Area: Rubbing can cause further damage to the fragile underlying tissue.
- Keep Skin Clean and Dry: Gently cleanse the area with a mild cleanser, pat it dry, and apply a barrier cream if moisture is a concern.
- Monitor Closely: Check the area frequently to see if the redness is improving or worsening. Document any changes.
- Seek Medical Evaluation: If the redness does not improve within 24-48 hours, or if it worsens (gets darker, blisters, or opens), contact a healthcare professional.
With prompt and proper care, a Stage 1 pressure injury can heal completely without progressing.
Other Conditions Causing Non-Blanchable Redness
While most commonly associated with pressure injuries, non-blanchable redness can occur in other conditions:
- Bruises (Contusions): A bruise is bleeding under the skin from trauma and will not blanch.
- Petechiae and Purpura: These are tiny red or purple spots caused by bleeding under the skin from infections or clotting issues. They do not blanch. A non-blanching rash with a fever can be a sign of a medical emergency like meningitis.
- Severe Skin Infections (Cellulitis): While early cellulitis is often blanchable, severe inflammation can damage vessels and cause it to become non-blanchable.
- Birthmarks (Port-Wine Stains): These birthmarks are caused by malformed blood vessels and do not blanch, but they are a chronic condition present from birth.
When to Seek Medical Advice
Consult a healthcare provider if:
- A non-blanchable red area does not improve or worsens after 24-48 hours of pressure relief.
- The area becomes bigger, darker, blistered, or develops into an open sore.
- Signs of infection appear, such as increased pain, warmth, swelling, pus, or fever.
- You see a non-blanching rash accompanied by other serious symptoms like fever, severe headache, or confusion.
Frequently Asked Questions
Can non-blanchable erythema heal completely?
Yes. When identified early as a Stage 1 pressure injury, the tissue damage is typically reversible. Immediate and consistent offloading of pressure, combined with proper skin protection and adequate nutrition, usually allows the area to return to normal within a few days to a week.
How quickly can non-blanchable erythema develop?
Pressure-related tissue damage can develop surprisingly fast. In vulnerable individuals, significant capillary damage can occur after as little as two to four hours of continuous, unrelieved pressure. This highlights why strict repositioning schedules and frequent skin checks are critical.
Is non-blanchable erythema only visible on lighter skin tones?
No. While classic redness is more apparent on lighter skin, non-blanchable erythema presents differently on melanin-rich skin. It often appears as a persistent darker, purplish, or bluish patch. Clinicians must also rely on tactile and temperature assessments, looking for localized warmth, firmness, swelling, or pain, since color alone may be misleading.
Should I massage a non-blanchable red spot to improve circulation?
Absolutely not. Massaging the affected area is contraindicated. Rubbing or deep tissue massage can cause shearing forces that further rupture fragile capillaries and damage already ischemic tissue, potentially accelerating the progression to a deeper, open wound.
Does non-blanchable redness always mean a pressure ulcer is forming?
While it is the primary clinical indicator of a Stage 1 pressure injury, non-blanchable discoloration can also result from trauma (bruising), petechiae, certain vascular birthmarks, or severe localized infections. A healthcare professional will evaluate the patient's mobility status, medical history, and the exact location and texture of the mark to confirm the diagnosis.
Conclusion
Non-blanchable erythema is a critical warning sign that the skin is under stress and at risk of breaking down. Early recognition and immediate intervention—primarily relieving all pressure from the area—can prevent the development of painful and dangerous pressure ulcers. By staying vigilant with skin checks, proper positioning, and good overall care, you can protect the skin and prevent serious complications.
Additional Resources & References
- Mayo Clinic – Bedsores (Pressure ulcers) Overview: A comprehensive guide on causes, symptoms, and treatments. Mayo Clinic: Bedsores (Pressure ulcers)
- National Pressure Injury Advisory Panel (NPIAP) – Staging Illustrations: Official definitions and images for each pressure injury stage. NPIAP – Pressure Injury Stages
- NHS UK – Pressure Sores (Pressure Ulcers): Information from the UK’s National Health Service on prevention and treatment. NHS – Pressure Sores
- AHRQ – Preventing Pressure Ulcers in Hospitals: A toolkit from the Agency for Healthcare Research and Quality with best practices for prevention. AHRQ Pressure Ulcer Prevention Toolkit
Disclaimer: This article is for informational purposes only. Always consult a healthcare professional for diagnosis and treatment of any medical condition.

About the author
Elena Vance, MD, is a double board-certified dermatologist and pediatric dermatologist. She is an assistant professor of dermatology at a leading medical university in California and is renowned for her research in autoimmune skin disorders.