Dry Skin on Penis: Causes, Treatments, and When to Worry

Key points
- Harsh Soaps and Chemicals: Soaps with strong fragrances, dyes, or harsh chemicals can strip the skin of its natural oils, leading to dryness. Many conventional body washes contain sulfates (like SLS or SLES) that act as powerful surfactants, effectively degreasing the skin but also disrupting its protective acid mantle. The same applies to laundry detergents and fabric softeners used on your underwear. Residue from these products remains trapped in fabric fibers and transfers directly to the penile shaft and glans throughout the day, triggering cumulative irritation.
- Friction and Chafing: Prolonged sexual activity or masturbation without adequate lubrication can cause friction that results in dry, irritated skin. Similarly, wearing tight-fitting clothing or underwear can lead to constant chafing. Synthetic fabrics like polyester or nylon trap heat and sweat, creating a microclimate that exacerbates friction while simultaneously drawing moisture away from the skin's surface through rapid evaporation when the clothing is eventually removed.
- Allergies: Your skin may be reacting to an allergen. This is a form of contact dermatitis. Common culprits include:
- Latex in condoms
- Spermicides
- Fragrances in lotions, soaps, or personal deodorants
Dry, flaky, or itchy skin on the penis can be uncomfortable and concerning. While it's a common issue that many men experience, it's natural to worry about the cause. The good news is that in most cases, dry penile skin is not a sign of a serious condition and can be managed with simple lifestyle changes or over-the-counter treatments. The penile skin is anatomically distinct from the skin found on most other parts of the body. It is notably thinner, lacks thick sebaceous (oil) glands, and contains a high concentration of nerve endings, making it exceptionally permeable to irritants and highly sensitive to moisture fluctuations. This unique physiology means that factors which might cause minor dryness elsewhere can lead to pronounced irritation, redness, and discomfort in the genital region. Understanding these anatomical nuances is crucial for implementing effective care and avoiding further damage.
This comprehensive guide will walk you through the potential causes, effective home remedies, and crucial signs that indicate it's time to see a doctor. By understanding the root triggers and adopting a gentle, evidence-based skincare routine, you can restore comfort, maintain tissue integrity, and alleviate anxiety surrounding this highly sensitive area.
Common Causes of Dry Penile Skin
The skin on the penis is thin and sensitive, making it susceptible to various irritants and conditions. Causes can generally be grouped into two categories: lifestyle factors and underlying medical conditions. Identifying whether your symptoms stem from daily habits or a physiological imbalance is the first step toward targeted relief.
Lifestyle and Environmental Factors
These are often the easiest issues to identify and correct. Modern grooming habits and environmental exposures play a massive role in maintaining or compromising the genital skin barrier.
- Harsh Soaps and Chemicals: Soaps with strong fragrances, dyes, or harsh chemicals can strip the skin of its natural oils, leading to dryness. Many conventional body washes contain sulfates (like SLS or SLES) that act as powerful surfactants, effectively degreasing the skin but also disrupting its protective acid mantle. The same applies to laundry detergents and fabric softeners used on your underwear. Residue from these products remains trapped in fabric fibers and transfers directly to the penile shaft and glans throughout the day, triggering cumulative irritation.
- Friction and Chafing: Prolonged sexual activity or masturbation without adequate lubrication can cause friction that results in dry, irritated skin. Similarly, wearing tight-fitting clothing or underwear can lead to constant chafing. Synthetic fabrics like polyester or nylon trap heat and sweat, creating a microclimate that exacerbates friction while simultaneously drawing moisture away from the skin's surface through rapid evaporation when the clothing is eventually removed.
- Allergies: Your skin may be reacting to an allergen. This is a form of contact dermatitis. Common culprits include:
- Latex in condoms
- Spermicides
- Fragrances in lotions, soaps, or personal deodorants
- Parabens, formaldehyde releasers, and botanical extracts in "natural" or "organic" grooming products
- Lubricant ingredients like glycerin or propylene glycol, which can cause osmotic dehydration in some individuals Contact dermatitis typically presents as delayed hypersensitivity, meaning the reaction may appear 24 to 48 hours after exposure, making it difficult to pinpoint the exact trigger without careful tracking or patch testing.
Medical Skin Conditions
If lifestyle changes don't resolve the issue, an underlying skin condition may be the cause. Genital dermatoses require precise diagnosis, as treatments vary significantly.
- Eczema (Dermatitis): This common inflammatory skin condition can cause intense itching, redness, bumps, and dry, cracked skin on the penis. It can be triggered by irritants or allergens. Atopic dermatitis often follows a cyclical pattern of flare-ups and remission, frequently worsening during periods of stress, temperature changes, or illness. Scratching eczematous lesions can lead to secondary bacterial infections, further compromising skin integrity.
- Psoriasis: An autoimmune disease, psoriasis can cause red patches of skin, sometimes with a silvery, scaly appearance. When it affects the genitals, the patches may look smooth and red rather than scaly. This phenomenon, known as inverse psoriasis, occurs because the warm, moist, and occluded environment of the groin prevents typical scale formation. Genital psoriasis can be particularly painful and is frequently associated with similar lesions on the elbows, knees, or scalp.
- Fungal Infections: A warm, moist environment can encourage fungal growth.
- Penile Yeast Infection (Candidiasis): This can cause a red rash, white patches, swelling, itching, and sometimes a thick, white discharge under the foreskin. Candida albicans thrives on elevated glucose levels and altered skin pH, making it more common in individuals with poorly controlled diabetes or those who have recently completed a broad-spectrum antibiotic course.
- Balanitis: This is an inflammation of the head of the penis (glans), often caused by poor hygiene or a fungal infection. It results in redness, swelling, soreness, and can cause the skin to appear dry and cracked. Balanitis is significantly more prevalent in uncircumcised men due to the potential for moisture, dead skin cells, and smegma to accumulate beneath the foreskin, creating an ideal breeding ground for irritants and microorganisms.
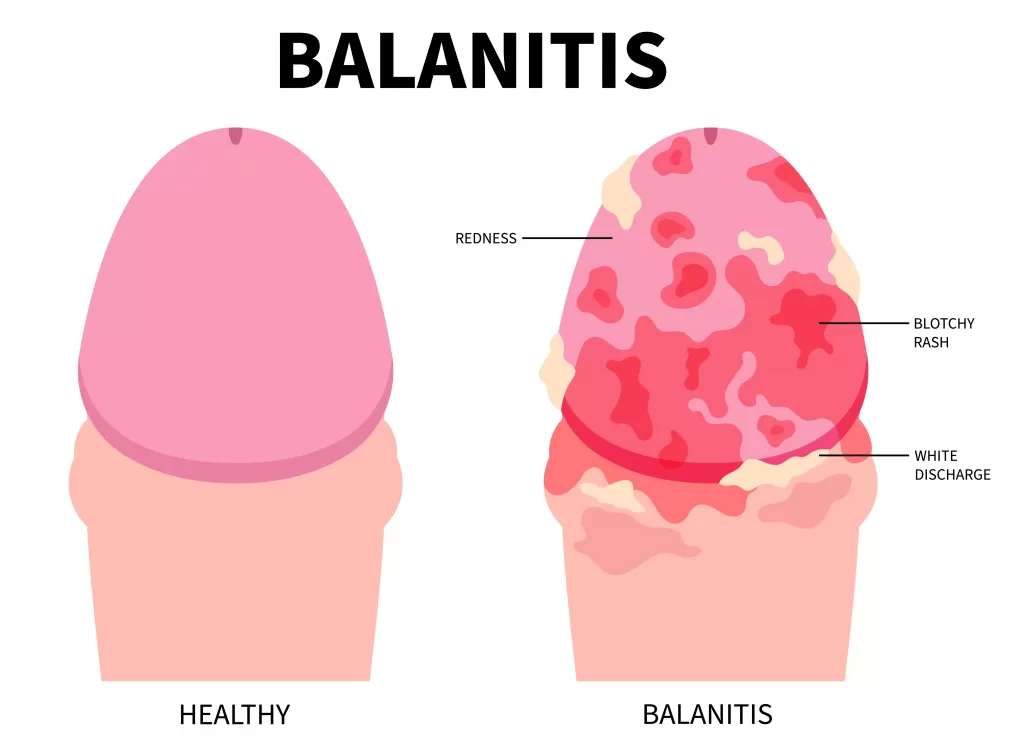 Image Source: qoctor.com.au
Image Source: qoctor.com.au
The Impact of Over-Washing and Poor Hygiene
Paradoxically, both excessive and insufficient cleansing can lead to dry penile skin. Over-washing disrupts the natural lipid barrier, causing transepidermal water loss. Conversely, infrequent washing allows dead skin cells, sweat, and bodily secretions to accumulate, altering the local microbiome and triggering irritation that manifests as dryness, tightness, and mild desquamation. Striking a balance is essential for maintaining optimal genital skin health.
How to Treat Dry Skin on the Penis
Treatment depends entirely on the cause. You can start with simple at-home care, but don't hesitate to seek medical advice if the problem persists. A systematic approach that prioritizes barrier repair, irritation removal, and targeted therapy will yield the best outcomes.
At-Home Remedies and Lifestyle Adjustments
For dryness caused by irritation or friction, these steps can provide significant relief:
- Switch to Gentle Products: Wash your penis with warm water and a small amount of mild, soap-free, and fragrance-free cleanser. Consider using a hypoallergenic laundry detergent. Look for cleansers labeled "syndet" (synthetic detergent) with a pH balanced between 5.0 and 7.0, which closely matches the skin's natural acidity and prevents disruption of the microbiome.
- Wear Breathable Clothing: Opt for loose-fitting underwear made of 100% cotton to minimize friction and moisture buildup. Bamboo-derived viscose and moisture-wicking modal fabrics are also excellent alternatives for individuals who sweat heavily or live in humid climates, as they maintain better temperature regulation while remaining soft against sensitive tissue.
- Use Lubrication: During sex or masturbation, always use a high-quality lubricant. Water-based lubricants are generally the least irritating and are safe to use with condoms. If you experience recurring dryness despite lubricant use, consider switching to silicone-based options for longer-lasting glide, or explore hybrid formulas. Avoid warming, tingling, or numbing lubricants until the skin has fully healed, as these often contain chemical irritants.
- Moisturize Carefully: Apply a bland, thick moisturizer or emollient ointment like Aquaphor or CeraVe Healing Ointment after showering to lock in moisture. As Dr. Rhys Young, a General Practitioner, notes for Healthy Male, it's important to use products that are safe for sensitive skin. For optimal results, apply moisturizers to slightly damp skin within three minutes of washing. This technique traps water molecules in the stratum corneum, dramatically enhancing hydration compared to applying products to completely dry skin.
- Stay Hydrated: Drinking plenty of water helps keep your skin hydrated from the inside out. Systemic hydration supports keratinocyte function and dermal elasticity. Incorporate omega-3 fatty acids from sources like fatty fish, flaxseeds, or walnuts into your diet, as these nutrients contribute to a healthy lipid barrier and possess natural anti-inflammatory properties.
- Gentle Drying Technique: Pat the area dry with a soft, clean towel instead of rubbing. Vigorous rubbing can cause micro-tears in already compromised skin. If uncircumcised, always gently retract the foreskin to clean and dry beneath it before pulling it back into place, preventing moisture entrapment and subsequent irritation.
Over-the-Counter (OTC) Treatments
If you suspect a specific condition, some OTC options may help:
- Antifungal Creams: For a suspected yeast infection or jock itch, an over-the-counter antifungal cream (containing clotrimazole or miconazole) can be effective. Apply as directed to the affected area. Continue application for at least 1-2 weeks, even if symptoms resolve sooner, to ensure complete eradication of the fungal colony and prevent rapid recurrence.
- Low-Strength Hydrocortisone Cream: For mild eczema or an allergic reaction, a 1% hydrocortisone cream can reduce itching and inflammation. However, do not use a steroid cream if you suspect a fungal infection, as it can make the infection worse. Additionally, avoid prolonged use of topical steroids on genital skin, as this thin area readily absorbs the medication, increasing the risk of local skin thinning, striae (stretch marks), and telangiectasia (visible blood vessels). Limit OTC steroid application to a maximum of 7-10 days unless specifically instructed otherwise by a physician.
Differentiating Benign Dryness from a Serious Concern
While most cases are harmless, it's crucial to recognize symptoms that point to a more serious issue. Self-diagnosis has limitations, and understanding clinical red flags helps you make informed decisions about when professional evaluation is necessary.
| Symptom | Likely Benign Dryness | May Indicate a Medical Condition |
|---|---|---|
| Appearance | Mild redness, flaking, fine lines | Intense red rash, white patches, silvery scales, bumps, sores |
| Sensation | Tightness, mild itching | Severe, persistent itching, burning, pain |
| Other Symptoms | None | Thick discharge, swelling, bleeding, foul odor |
| Response to Home Remedies | Improves within a few days | Persists or worsens despite home care |
!A close-up image showing peeling skin, which could be a sign of a male yeast infection.:max_bytes(150000):strip_icc()/male-yeast-infection-skin-peeling-5192706_final1-2e93a95276bf4b2eb8bc96a7b5c37b1c.jpg) Image Source: WebMD
Chronic Dermatological Conditions to Consider
If standard dryness treatments consistently fail, consider less common but clinically significant conditions. Lichen sclerosus presents as thin, white, parchment-like patches that can cause tightness, tearing, and severe discomfort, particularly around the foreskin and glans. It requires prompt medical management to prevent scarring and phimosis. Lichen planus often manifests as purplish, flat-topped bumps or lacy white lines (Wickham striae) that can affect the penile shaft, causing significant itching and potential mucosal erosion. Zoon's balanitis (plasma cell balanitis) typically appears as shiny, orange-red plaques on the glans of uncircumcised men, often accompanied by pinpoint red spots resembling "cayenne pepper." Unlike infectious or irritant causes, these chronic inflammatory dermatoses require targeted immunomodulatory therapy.
Could it be an STI?
Dry skin alone is not a typical symptom of a sexually transmitted infection (STI). However, some STIs like genital herpes or syphilis can cause sores, blisters, or rashes that could be confused with severe dry skin. If there is any possibility you have been exposed to an STI, it is essential to get tested. Human papillomavirus (HPV) may present initially as dry, scaly patches or flat warts that feel rough to the touch, while secondary syphilis can cause a non-itchy rash on the palms, soles, and genital area that mimics dry dermatitis. Comprehensive STI screening, including blood work and swab testing, is the only definitive way to rule out infectious etiologies, particularly if symptoms are accompanied by systemic signs like swollen lymph nodes in the groin, unexplained fatigue, or flu-like symptoms.
When to See a Doctor
Consult a doctor or dermatologist if you experience any of the following:
- Your symptoms do not improve after a week of home care.
- The dry skin is getting worse.
- You experience severe pain, itching, or swelling.
- You notice any lumps, sores, blisters, or a rash.
- There is a thick or foul-smelling discharge from under your foreskin or the tip of your penis.
- You also have a fever or feel generally unwell.
- You notice difficulty retracting or replacing your foreskin (phimosis or paraphimosis), which constitutes a medical emergency.
- You experience painful urination, blood in the urine, or pain during ejaculation.
A healthcare professional can provide an accurate diagnosis and prescribe stronger treatments like prescription-strength steroid creams, oral antifungal medications, or specific therapies for conditions like psoriasis. Diagnosis typically involves a thorough clinical examination, review of sexual and medical history, and potentially a skin scraping, swab culture, or biopsy to rule out malignancies or atypical dermatoses. Urologists and dermatologists specializing in male genital health are particularly well-equipped to manage complex or refractory cases.
The Role of Underlying Systemic Health Conditions
Local skin symptoms rarely exist in isolation. Systemic metabolic and hormonal shifts significantly influence genital tissue health and resilience.
Diabetes and Blood Sugar Regulation Uncontrolled diabetes is one of the most overlooked contributors to recurrent penile dryness and fungal overgrowth. Elevated blood glucose levels lead to increased glucose in sweat and urine. When this sugary fluid contacts genital skin, it creates a highly favorable environment for yeast proliferation. Furthermore, chronic hyperglycemia impairs peripheral circulation and compromises neutrophil function, slowing wound healing and increasing susceptibility to micro-tears and secondary infections. If you experience recurrent balanitis or persistent dryness alongside increased thirst, frequent urination, or unexplained weight loss, a fasting blood glucose or HbA1c test is highly recommended.
Hormonal Fluctuations Testosterone plays a vital role in maintaining skin thickness, collagen production, and sebum regulation. Age-related andropause (late-onset hypogonadism) or other endocrine disruptions can lead to generalized skin thinning, decreased moisture retention, and heightened sensitivity. Similarly, thyroid dysfunction—particularly hypothyroidism—can cause widespread xerosis (abnormally dry skin), which frequently affects thinner, more delicate areas like the genital region before progressing to the extremities or torso.
Medication Side Effects Several prescription medications list dry skin and mucosal irritation as common adverse effects. Isotretinoin (used for severe acne), diuretics, antihistamines, beta-blockers, and certain psychiatric medications can systemically reduce skin hydration by altering sweat gland activity, sebum production, or peripheral blood flow. If dry penile skin coincided with starting a new medication, discussing dosage adjustments or supportive skincare strategies with your prescribing physician may be necessary.
Advanced Medical Treatments and Procedures
When conservative measures and standard OTC therapies prove insufficient, clinicians have several advanced interventions at their disposal.
Prescription Topicals and Immunomodulators For chronic inflammatory conditions like psoriasis or eczema, dermatologists may prescribe topical calcineurin inhibitors (tacrolimus or pimecrolimus). Unlike corticosteroids, these medications do not cause skin thinning, making them safer for long-term use on delicate genital tissue. They work by selectively modulating local immune responses, effectively reducing inflammation and itching without compromising epidermal structure.
Targeted Antifungal and Antibacterial Regimens Severe or recurrent fungal infections may require oral antifungal medications like fluconazole or itraconazole, which achieve therapeutic concentrations in skin and mucous membranes from the inside out. If bacterial balanitis (often caused by Group A Streptococcus or Staphylococcus species) is diagnosed via culture, a targeted course of oral or topical antibiotics will be prescribed. Mixed infections require sequential or combination therapy to address both pathogen types effectively.
Circumcision for Refractory Cases In cases of chronic, treatment-resistant balanoposthitis or severe lichen sclerosus where the foreskin is heavily involved and causing recurrent scarring or functional impairment, circumcision may be recommended as a definitive therapeutic option. Removing the moist, occluded environment beneath the foreskin often resolves the underlying inflammatory trigger and prevents future episodes. This decision is always made collaboratively after exhausting conservative and medical management strategies.
Long-Term Prevention and Skin Barrier Maintenance
Sustaining healthy penile skin requires consistent, mindful habits that protect the epidermal barrier and support tissue resilience over time.
Establishing a Minimalist Grooming Routine Less is often more when it comes to genital skincare. Stick to a simple regimen: rinse with lukewarm water daily, use a fragrance-free, pH-balanced cleanser 2-3 times per week, and apply a basic moisturizer like plain petroleum jelly or a ceramide-rich cream post-shower. Avoid exfoliating scrubs, loofahs, or rough washcloths on the genital area, as physical abrasion rapidly compromises thin skin.
Smart Sexual Health Practices Always urinate after intercourse to flush potential irritants or pathogens from the urethral opening. Cleanse the area gently within 15-30 minutes after sexual activity, but avoid aggressive washing. If you or your partner use vaginal antifungal treatments, spermicides, or flavored/warming products, be aware that residual chemicals can easily transfer and trigger contact dermatitis on penile skin. Using non-latex condoms (polyurethane or polyisoprene) is advisable if latex sensitivity is suspected or confirmed.
Environmental Control and Stress Management Chronic psychological stress elevates cortisol levels, which directly impairs skin barrier function, delays wound healing, and exacerbates inflammatory conditions like eczema and psoriasis. Incorporating stress-reduction techniques such as mindfulness, adequate sleep (7-9 hours nightly), and regular moderate exercise supports systemic hormone balance and, by extension, skin health. Additionally, managing indoor humidity levels between 40-60% using a humidifier during winter or dry seasons prevents environmental moisture stripping.
References:
- Gillespie, C. (2018). What Causes Dry Skin on the Penis?. Healthline. https://www.healthline.com/health/mens-health/dry-skin-on-penis
- Burgess, L. (2019). Dry skin on the penis: Causes and home remedies. Medical News Today. https://www.medicalnewstoday.com/articles/325286
- Young, R. Ask the Doc: Why do I have dry skin on my penis?. Healthy Male. https://healthymale.org.au/ask-the-doc/why-do-i-have-dry-skin-my-penis/
- Letorney, A. (2024). 8 Reasons the Skin on Your Penis is Dry. Hone Health. https://honehealth.com/edge/dry-skin-on-penis/
- Cleveland Clinic. (2023). Eczema on Penis. https://my.clevelandclinic.org/health/diseases/24314-eczema-on-penis
Frequently Asked Questions
How long does it typically take for dry penile skin to heal?
The healing timeline depends entirely on the underlying cause and the consistency of your care routine. Simple dryness caused by harsh soaps, friction, or mild environmental factors usually resolves within 3 to 7 days once the irritant is removed and a consistent moisturizing regimen is established. However, if the dryness stems from a fungal infection, eczema, psoriasis, or lichen sclerosus, healing may take several weeks of targeted treatment. Chronic conditions often require long-term maintenance therapy rather than a one-time cure. Patience is key, and pushing through symptoms with continued exposure to irritants will only prolong the healing process.
Can I use regular body lotion or coconut oil on my penis?
While some men tolerate coconut oil and lightweight body lotions without issue, dermatologists generally advise against them for the genital area. Many commercial body lotions contain alcohols, fragrances, preservatives, or high concentrations of glycerin that can cause stinging or allergic contact dermatitis on thin mucosal skin. Coconut oil is highly comedogenic and can sometimes disrupt the natural microbiome, potentially worsening underlying yeast overgrowth. It is safer to opt for medically formulated, hypoallergenic barrier creams, plain petroleum jelly, or zinc oxide ointments, which are occlusive, non-irritating, and specifically tested for sensitive tissue.
Does circumcision prevent dry skin and fungal infections on the penis?
Circumcision significantly reduces the moisture-trapping environment beneath the foreskin, which directly lowers the risk of recurrent candidiasis, bacterial balanitis, and irritant dermatitis caused by smegma accumulation. Many circumcised men report fewer episodes of genital fungal infections and easier hygiene maintenance. However, circumcision is not a guaranteed preventative measure for all types of dry skin. The glans remains exposed to friction, environmental factors, and systemic dermatological conditions like psoriasis or eczema, which can still manifest as dryness. Good hygiene and appropriate moisturization remain essential regardless of circumcision status.
Should I stop all sexual activity if I have dry, flaky skin?
It is generally advisable to temporarily abstain from penetrative sex, oral sex, and masturbation until the skin barrier has fully healed and the underlying cause has been addressed. Friction during sexual activity can exacerbate micro-tears, increase inflammation, and delay recovery. Additionally, if the cause is infectious (such as a yeast infection, bacterial balanitis, or an undiagnosed STI), sexual contact poses a transmission risk to your partner. If abstinence is difficult, ensure any sexual activity is extremely gentle, thoroughly lubricated with a hypoallergenic product, and accompanied by barrier protection like condoms to minimize direct skin-to-skin irritation.
When is a biopsy necessary for dry penile skin?
A skin biopsy is typically reserved for cases where the diagnosis remains unclear after standard treatments, when lesions appear atypical, or when chronic inflammatory conditions fail to respond to appropriate therapy. It is particularly important if you notice persistent, non-healing ulcers, rapidly changing pigmentation, firm nodules, or lesions suspicious for premalignant or malignant conditions like penile intraepithelial neoplasia (PeIN) or squamous cell carcinoma. The procedure is minimally invasive, performed under local anesthesia, and provides definitive histopathological analysis, ensuring that rare but serious conditions are not overlooked or mismanaged.
Conclusion
Dry skin on the penis is a highly prevalent, usually benign condition that rarely indicates a serious medical emergency. Because penile tissue is uniquely thin and highly sensitive, it responds rapidly to irritants, environmental changes, friction, and microbial imbalances. By identifying trigger factors—whether they stem from harsh grooming products, sexual habits, allergic reactions, or underlying dermatological conditions—you can implement a targeted, evidence-based care routine that restores skin integrity and eliminates discomfort. Consistent use of gentle cleansers, appropriate moisturizers, breathable clothing, and cautious application of OTC treatments resolves the vast majority of cases within a short timeframe.
However, vigilance is crucial. Recognizing when symptoms deviate from typical dryness and escalate into persistent inflammation, unusual lesions, pain, or systemic signs empowers you to seek timely professional intervention. Underlying metabolic conditions like diabetes, chronic dermatoses like psoriasis or lichen sclerosus, and sexually transmitted infections all require precise medical diagnosis and tailored treatment plans that cannot be self-managed. Prioritizing long-term skin barrier maintenance, practicing mindful sexual health habits, and avoiding the overuse of chemical irritants will safeguard genital skin resilience for years to come. If you ever feel uncertain, overwhelmed by symptoms, or if simple remedies fail to provide relief, consulting a primary care physician, dermatologist, or urologist is always the safest and most effective path forward. Your comfort, health, and confidence are entirely achievable with the right knowledge and care.

About the author
Elena Vance, MD, is a double board-certified dermatologist and pediatric dermatologist. She is an assistant professor of dermatology at a leading medical university in California and is renowned for her research in autoimmune skin disorders.