Inner Leg Pimples: Causes, Treatment, and Prevention

Key points
- Poor Hygiene: Not bathing regularly can allow sweat, oil, dead keratinocytes, and environmental pollutants to accumulate. However, over-washing with harsh, alkaline soaps can strip the skin's lipid barrier, triggering rebound oil production and microbiome disruption.
- Diet and Lifestyle: Diets high in sugar, refined carbohydrates, and dairy may worsen acne for some people due to their impact on insulin, IGF-1, and inflammatory cytokines. High glycemic foods cause rapid blood sugar spikes, which can stimulate sebaceous gland activity. Chronic stress elevates cortisol, further dysregulating skin homeostasis. Not changing out of sweaty clothes promptly also increases risk.
- Contact Dermatitis: An allergic reaction to lotions, detergents, fragrances, synthetic fabrics, or laundry softeners can cause red, itchy bumps that may be mistaken for pimples. Type IV delayed hypersensitivity reactions manifest 24-72 hours after exposure, presenting as eczematous patches with small vesicles. Switching to fragrance-free, dye-free laundry detergents and avoiding heavily perfumed body products can help differentiate allergic contact dermatitis from true folliculitis or acne.
Pimples aren't just for your face—they can appear on other parts of your body, including your inner legs and thighs. These uncomfortable bumps are common, but understanding their causes is key to treating and preventing them. This guide covers what inner leg pimples are, why they happen, how to treat them, and how to keep your skin clear and healthy. While facial acne often dominates dermatological discussions and commercial marketing, body breakouts affect millions of individuals across all age groups and demographics. The inner thigh region, in particular, presents a unique dermatological environment due to its proximity to the groin, constant skin-to-skin contact, and susceptibility to moisture buildup. For many, these breakouts are more than a cosmetic concern; they can cause physical discomfort, impact mobility during exercise, and even affect self-confidence when wearing certain clothing. Navigating treatment requires a nuanced approach because the underlying triggers often differ from those of facial acne. Rather than simply applying standard facial acne protocols, effective management involves addressing localized friction, microbiome balance, hair follicle health, and environmental exposures. By integrating clinical insights with practical daily habits, you can develop a sustainable skincare strategy that clears existing blemishes and prevents future flare-ups.
What Are Inner Leg Pimples?
Inner leg pimples are bumps or blemishes that form on the inner thighs, often near the groin or where the thighs rub together. Like facial pimples, they occur when pores or hair follicles become clogged with excess oil (sebum), dead skin cells, and bacteria. However, the skin on the inner thighs differs structurally and functionally from facial skin. The epidermal layer in this region is slightly thinner and more sensitive, making it highly reactive to irritants, moisture, and mechanical stress. When hair follicles become obstructed, the trapped sebum creates an anaerobic environment where Cutibacterium acnes (formerly Propionibacterium acnes) and other skin commensals can proliferate. This triggers an immune response, drawing white blood cells to the area and resulting in localized inflammation, redness, and swelling.
This clogging can lead to inflammation, resulting in bumps that range from small red spots to larger, painful, boil-like lesions. The skin on the inner thighs is often soft and sensitive, and factors like sweat, heat, and friction make it a prime location for breakouts. What looks like a pimple could also be another type of bump, such as an ingrown hair, folliculitis (inflamed hair follicles), or a small boil. Clinically, these lesions manifest across a spectrum. Comedonal breakouts appear as closed (whiteheads) or open (blackheads) clogged pores, though they are less common on the thighs due to larger pore structures. Inflammatory lesions progress to papules (firm, red bumps without pus), pustules (pus-filled with a white or yellow center), nodules (deep, solid, painful lumps), or cysts (fluid-filled pockets that can lead to scarring). The terminology often overlaps in casual conversation, but accurate identification matters because a bacterial folliculitis requires different treatment than a hormonal cyst, and an ingrown hair may need mechanical exfoliation rather than antimicrobial therapy.
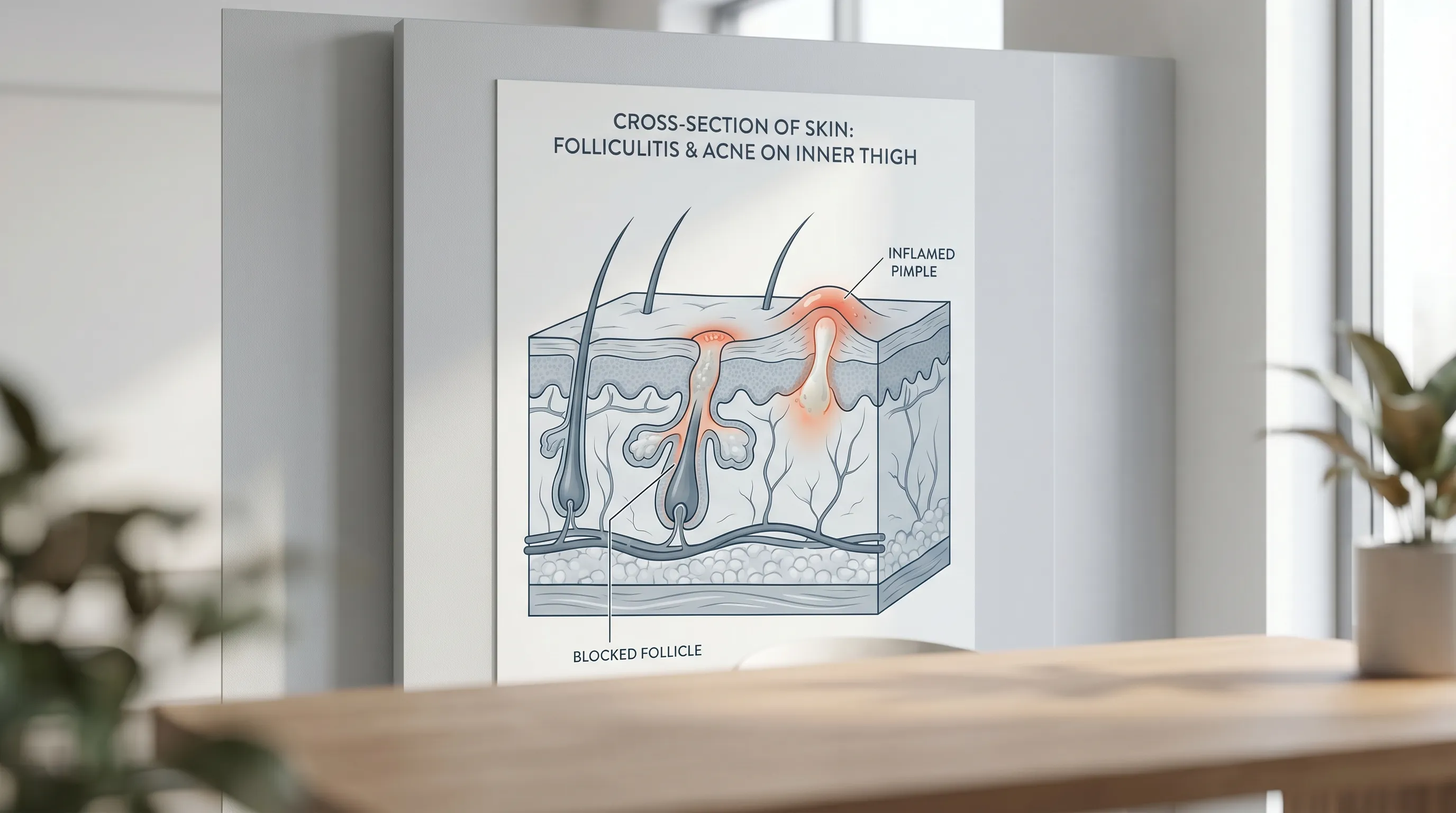
Differentiating between simple body acne and other dermatological conditions is crucial. Fungal folliculitis, often caused by Malassezia yeast, presents as uniform, intensely itchy red bumps that worsen with sweating and antibiotics. Molluscum contagiosum, a viral infection common in children and sexually active adults, appears as pearly, dome-shaped bumps with central dimples. Epidermoid cysts develop when keratin-producing cells move deeper into the skin rather than shedding. Recognizing these distinctions prevents misapplication of treatments that could exacerbate the issue. For instance, using harsh steroid creams on a fungal infection can mask symptoms temporarily while allowing the pathogen to proliferate, while aggressive scrubbing on cystic lesions can rupture the follicular wall and spread inflammation deeper into the dermis. A careful assessment of lesion appearance, symmetry, itch versus pain, and response to previous treatments often guides the correct therapeutic pathway.
Common Causes of Inner Leg Pimples
Inner thigh pimples often result from a combination of environmental and biological factors. Understanding the precise mechanism behind each trigger allows for targeted prevention and more effective treatment strategies.
Friction and Chafing
When your inner thighs rub against each other during activities like walking or running, the friction can irritate the skin and hair follicles. This mechanical stress disrupts the stratum corneum, the skin's outermost protective barrier, leading to micro-abrasions that compromise its integrity. Once the barrier is weakened, it becomes easier for bacteria to penetrate and for transepidermal water loss to increase, paradoxically triggering compensatory oil production. This irritation, combined with heat and moisture from tight clothing, creates an ideal environment for pores to clog and bacteria to grow, leading to pimples. The inflammatory cascade activated by friction releases cytokines like interleukin-1 and tumor necrosis factor-alpha, which recruit immune cells and amplify redness and swelling. Chronic chafing can also lead to post-inflammatory hyperpigmentation, leaving dark marks that linger long after the active bumps resolve. Athletes, dancers, and individuals with a higher body mass index often experience this more severely due to prolonged, repetitive skin contact. Wearing anti-chafing garments or applying barrier creams can mitigate the mechanical stress and protect the follicular architecture.
Sweat and Clogged Pores
The inner thigh area is prone to sweating, especially during exercise or in hot weather. The human body contains two main types of sweat glands: eccrine glands, which produce watery sweat to cool the body, and apocrine glands, concentrated in the groin and armpits, which secrete a thicker fluid that bacteria readily metabolize. When sweat mixes with the skin's natural oils and dead skin cells, it can easily block pores and hair follicles. This buildup can cause inflammation, resulting in what are sometimes called "sweat pimples." Prolonged exposure to moisture also raises the skin's surface pH, disrupting the acidic mantle that normally inhibits pathogenic bacterial growth. In humid climates or during intense physical activity, sweat can remain trapped against the skin by non-breathable fabrics for hours. This maceration effect softens the skin, making follicles more prone to rupture under minor pressure. Furthermore, the salt and urea present in sweat can act as mild irritants when concentrated, triggering contact dermatitis that mimics or compounds acne-like eruptions. Prompt cleansing and moisture management are essential to restore the skin's natural balance and prevent follicular occlusion.
Ingrown Hairs and Folliculitis
Hair removal methods like shaving or waxing can lead to ingrown hairs, which occur when a hair curls back and grows into the skin. This creates a red, pimple-like bump that can become inflamed or infected. When a hair is cut too short or removed against the growth direction, it may retract beneath the skin's surface instead of exiting the follicle. As it continues to grow, the sharp tip penetrates the surrounding dermal tissue, recognized by the body as a foreign invader. This triggers a localized granulomatous reaction, forming a firm, often tender bump.
Folliculitis is a related condition where hair follicles become inflamed or infected, often by bacteria like Staphylococcus aureus or Staphylococcus epidermidis. This results in small, itchy, or tender red bumps or white-headed pimples around the hair follicles. Unlike typical acne, bacterial folliculitis often spreads quickly across a shaved area and can develop into deeper furuncles (boils) if left untreated. Fungal folliculitis, conversely, thrives in warm, occluded environments and responds better to antifungal agents than antibacterial ones. Distinguishing between these subtypes is critical for effective therapy. Overuse of broad-spectrum antibiotics can sometimes worsen fungal variants by eliminating protective skin flora. Preventive measures include proper razor hygiene, avoiding overly aggressive waxing on sensitive skin, and using post-hair-removal soothing agents that reduce inflammation without clogging pores.
"After I started cycling daily, I noticed red bumps on my inner thighs. My dermatologist told me it was due to friction and sweat clogging my hair follicles. Once I switched to looser, breathable shorts and started showering right after my rides, the problem improved significantly." – Personal experience shared on a skincare forum.
This testimonial highlights the direct relationship between mechanical activity, environmental exposure, and follicular health. Cyclists, runners, and gym-goers frequently report similar experiences, underscoring the importance of post-activity skin care. Sweat left to dry on the skin acts as a medium for microbial proliferation, while repetitive leg movement grinds debris into follicular openings. Establishing a consistent post-exercise hygiene routine—rinsing within 30 minutes of finishing activity, changing out of damp gear, and applying a gentle cleanser—can dramatically reduce incidence rates. Additionally, choosing apparel with seamless inner thighs and moisture-wicking properties minimizes both friction and prolonged dampness.
Hormones and Acne
Hormonal fluctuations, such as those during puberty, menstrual cycles, pregnancy, menopause, or due to conditions like polycystic ovary syndrome (PCOS), can increase oil production. Androgens, particularly testosterone and dihydrotestosterone (DHT), bind to receptors in sebaceous glands, stimulating them to produce thicker, more abundant sebum. This can lead to clogged pores and acne breakouts on various parts of the body, including the inner thighs. The inner thigh and groin area contain a high density of androgen receptors, making them particularly responsive to hormonal shifts. If you experience acne on your face, chest, and back as well, hormones may be a contributing factor. Hormonal acne often follows a predictable pattern, flaring cyclically or worsening alongside stress, poor sleep, or dietary changes that influence insulin-like growth factor 1 (IGF-1) levels. Elevated IGF-1 can amplify androgen activity and keratinocyte proliferation, further compounding follicular blockage. Women with PCOS or adrenal hyperplasia may notice more persistent, deep-seated cystic lesions that resist topical treatments. In these cases, addressing the systemic hormonal imbalance through medical intervention, alongside topical care, yields the most sustainable results.
Hidradenitis Suppurativa (Acne Inversa)
If you experience recurrent, painful, boil-like lumps on your inner thighs, groin, or armpits, it could be a chronic skin condition called hidradenitis suppurativa (HS). This condition involves blocked and inflamed hair follicles that lead to painful abscesses, sinus tract formation, and potential scarring. HS is an inflammatory disease, not a hygiene-related condition, and it disproportionately affects individuals with obesity, smokers, and those with a family history of autoimmune disorders. The pathophysiology involves abnormal follicular occlusion, rupture, and a dysregulated immune response that perpetuates chronic inflammation. Unlike typical acne, HS lesions often interconnect beneath the skin, creating tunnels (sinus tracts) that can drain pus and blood. HS requires a medical diagnosis and a specific treatment plan from a dermatologist. Early intervention is critical, as the Hurley staging system classifies disease severity from mild, isolated nodules (Stage I) to extensive, interconnected sinus tracts (Stage III). Treatments range from biologic medications targeting inflammatory pathways (like adalimumab) to surgical excision and laser hair removal in advanced cases. Misdiagnosing HS as recurrent boils or severe acne delays appropriate therapy and increases the risk of permanent skin damage and functional impairment.
Other Factors
- Poor Hygiene: Not bathing regularly can allow sweat, oil, dead keratinocytes, and environmental pollutants to accumulate. However, over-washing with harsh, alkaline soaps can strip the skin's lipid barrier, triggering rebound oil production and microbiome disruption.
- Diet and Lifestyle: Diets high in sugar, refined carbohydrates, and dairy may worsen acne for some people due to their impact on insulin, IGF-1, and inflammatory cytokines. High glycemic foods cause rapid blood sugar spikes, which can stimulate sebaceous gland activity. Chronic stress elevates cortisol, further dysregulating skin homeostasis. Not changing out of sweaty clothes promptly also increases risk.
- Contact Dermatitis: An allergic reaction to lotions, detergents, fragrances, synthetic fabrics, or laundry softeners can cause red, itchy bumps that may be mistaken for pimples. Type IV delayed hypersensitivity reactions manifest 24-72 hours after exposure, presenting as eczematous patches with small vesicles. Switching to fragrance-free, dye-free laundry detergents and avoiding heavily perfumed body products can help differentiate allergic contact dermatitis from true folliculitis or acne.
How to Treat Inner Leg Pimples
Treatment depends on the severity of the pimples and can range from simple at-home care to medical intervention. A strategic approach involves addressing active inflammation, preventing secondary infection, and supporting skin barrier repair. Consistency is key, as most topical treatments require 4 to 8 weeks of continuous use to demonstrate significant improvement due to the natural 28-day epidermal turnover cycle.
At-Home Care and OTC Treatments
For mild cases, start with these steps:
- Gentle Cleansing: Wash the area daily with a mild, non-comedogenic soap. Avoid harsh sulfates or highly alkaline cleansers that compromise the acid mantle. Body washes containing benzoyl peroxide (typically 2.5% to 5%) work by releasing oxygen radicals that destroy acne-causing bacteria, reducing inflammation without promoting antibiotic resistance. Salicylic acid (0.5% to 2%) is a beta-hydroxy acid (BHA) that is lipid-soluble, allowing it to penetrate deep into sebum-filled pores to dissolve the keratin and oil plugs that initiate breakouts. Using these cleansers in a controlled manner—applying to damp skin, massaging gently for 30-60 seconds, and rinsing thoroughly—maximizes efficacy while minimizing irritation.
- Warm Compress: Apply a clean, warm washcloth to the area for 10-15 minutes, several times a day. The gentle heat increases local blood circulation, delivering immune cells and oxygen to the affected follicle. This can reduce pain and help a pimple or boil drain naturally. Always use a fresh cloth each time to avoid reintroducing bacteria, and never apply excessive heat that could cause thermal injury.
- Topical Treatments: Apply an over-the-counter antibiotic ointment like bacitracin or polysporin only if the skin is broken or at high risk of secondary infection from scratching. For acne-like pimples, a spot treatment with benzoyl peroxide or salicylic acid can help. Adapalene gel (0.1%), previously prescription-only and now available OTC, is a third-generation retinoid that normalizes follicular cell turnover, prevents microcomedone formation, and possesses anti-inflammatory properties. Start with application every other night to assess tolerance, and always follow with a fragrance-free moisturizer to counteract potential dryness.
- Avoid Squeezing: Popping pimples can push the infection deeper, worsen inflammation, and lead to scarring. Mechanical extraction disrupts the follicular wall, allowing bacteria and inflammatory mediators to spill into the surrounding dermis. This significantly increases the risk of hyperpigmentation, atrophic (depressed) scars, or hypertrophic (raised) scar tissue. Let them heal on their own or with gentle treatment. If a pimple has naturally come to a head, sterile lancets used by professionals can safely extract contents without damaging surrounding tissue.
- Wear Loose Clothing: Opt for breathable fabrics like cotton to reduce friction and allow air to circulate, keeping the area dry. During treatment, tight waistbands, leggings, or synthetic underwear can trap active ingredients against the skin, causing irritation, or trap heat and moisture, negating treatment progress. Prioritize loose-fitting, moisture-wicking garments until inflammation subsides.
Home Remedies and Natural Options
Some people find relief with natural remedies, though results can vary and scientific evidence is often limited compared to clinically studied actives. These options are best suited for mild irritation or as adjuncts to standard care.
- Tea Tree Oil: Known for its antibacterial properties, dilute it with a carrier oil (like coconut oil or jojoba oil) at a 1-5% concentration before applying to a pimple. Studies have shown 5% tea tree oil to be moderately effective against C. acnes, though it acts slower than benzoyl peroxide. Never apply undiluted essential oils directly to the skin, as they can cause severe contact dermatitis, chemical burns, or photosensitivity. Always perform a patch test 24 hours prior to full application.
- Aloe Vera Gel: Its soothing properties can help reduce redness and inflammation. Pure aloe contains polysaccharides, glycoproteins, and salicylic acid-like compounds that calm irritation and promote wound healing. Opt for products with high aloe content and minimal added alcohols, fragrances, or colorants. Refrigerated aloe gel can provide additional cooling relief for inflamed, chafed skin.
- Oatmeal Baths: A lukewarm bath with colloidal oatmeal can soothe widespread irritation or itching. Colloidal oatmeal is finely ground and suspended in water, forming a protective, anti-inflammatory film on the skin. It contains avenanthramides, which inhibit histamine release and reduce nerve ending sensitivity. Soak for 10-15 minutes, pat dry gently, and apply moisturizer immediately to lock in hydration. Avoid hot water, which strips lipids and exacerbates inflammation.
Medical Treatments and When to See a Doctor
Consult a doctor or dermatologist if your pimples are severe, painful, or recurrent, or if over-the-counter methods fail after 6-8 weeks. Professional evaluation ensures accurate diagnosis and access to targeted therapies.
- Prescription Topicals: A doctor can prescribe stronger treatments like topical antibiotics (e.g., clindamycin, mupirocin, or erythromycin) to eliminate resistant bacterial strains. These are often combined with benzoyl peroxide to prevent resistance development. Topical retinoids like tretinoin or tazarotene regulate keratinization and accelerate cellular turnover, effectively clearing existing blockages and preventing new ones. Clascoterone (a topical androgen receptor inhibitor) is also emerging as a targeted therapy for hormonally driven body acne.
- Oral Medications: For severe infections, widespread acne, or conditions like HS, oral antibiotics (like doxycycline, minocycline, or macrolides) provide systemic anti-inflammatory and antimicrobial effects. Hormonal therapies, such as combined oral contraceptives containing estrogen and progestin, or anti-androgens like spironolactone, can significantly reduce sebum production in women. For severe, treatment-resistant cystic acne, oral isotretinoin remains the gold standard, permanently shrinking sebaceous glands and normalizing follicular differentiation, though it requires strict monitoring due to potential side effects.
- Incision and Drainage: A large, painful boil or abscess may need to be drained by a healthcare professional to relieve pressure, accelerate healing, and clear the infection. The provider will sterilize the area, administer local anesthesia, make a precise incision, evacuate purulent material, and sometimes pack the wound with sterile gauze. Never attempt this at home, as improper technique can introduce deeper pathogens, cause excessive scarring, or lead to life-threatening systemic infections like cellulitis or sepsis.
- Laser Hair Removal: If ingrown hairs and recurrent folliculitis are the primary cause, laser hair removal can be a long-term solution to reduce hair growth and subsequent bumps. By targeting melanin in the hair shaft, lasers destroy the follicular bulb while sparing surrounding tissue. Multiple sessions are required due to hair growth cycles, and it is most effective on individuals with darker hair and lighter skin, though Nd:YAG lasers have expanded safe treatment parameters for diverse skin tones. Diathermy (electrical destruction) of individual follicles is another option for resistant cases.
See a doctor if:
- A pimple is extremely large, painful, or doesn't improve with home care after several weeks.
- You see signs of a spreading infection, such as expanding redness, warmth to the touch, foul-smelling drainage, red streaks, or systemic symptoms like fever and chills.
- You have recurring breakouts in the same area, lesions that interconnect, or persistent scarring, which could signal a condition like HS, cystic disease, or resistant bacterial colonization (e.g., MRSA).
- Over-the-counter products cause severe dryness, peeling, or allergic reactions that disrupt daily life.
How to Treat and Prevent Body Acne A board-certified dermatologist explains common causes of body breakouts and provides tips on choosing the right products and habits to keep skin clear. Source: Dr. Dray on YouTube.
How to Prevent Inner Leg Pimples
Prevention focuses on minimizing the factors that cause breakouts through consistent, sustainable habits that support skin barrier integrity, microbiome balance, and follicular health. Integrating these strategies into your daily routine significantly reduces recurrence rates.
- Practice Good Hygiene: Shower daily, and especially as soon as possible after sweating, exercising, or exposure to high humidity. Use lukewarm water rather than hot, which can deplete natural lipids. Gently cleanse with fingertips rather than rough washcloths or loofahs, which harbor bacteria and cause micro-tears. Pat the area dry with a clean, dedicated towel instead of rubbing, and wash towels and bed linens weekly to prevent bacterial reintroduction. Consider keeping a travel-sized gentle cleanser and clean change of clothes at the gym for immediate post-workout care.
- Wear Breathable Clothing: Choose loose-fitting clothes made of natural fibers like organic cotton or advanced moisture-wicking synthetic blends like nylon-spandex specifically designed for athletic wear. Avoid tight pants, leggings, or synthetic underwear that trap heat, sweat, and friction against the skin. When sitting for prolonged periods, shift positions occasionally to allow air circulation. For sleep, opt for breathable, loose-fitting cotton pajamas or sleep without restrictive bottoms to let the skin recover overnight.
- Reduce Friction: If your thighs rub together, apply an anti-chafe balm, petroleum jelly, or silicone-based lubricant before activities that involve prolonged walking, running, or cycling. Wearing seamless bike shorts, compression liners, or anti-chafing thigh bands under skirts and dresses creates a protective physical barrier. For chronic chafing, barrier repair creams containing ceramides, niacinamide, and panthenol can strengthen the stratum corneum, making it more resilient to mechanical stress. Gradually building skin tolerance through regular moisturization also helps.
- Shave Carefully: To prevent ingrown hairs, always prepare the skin with warm water and a generous application of hypoallergenic shaving gel or cream to soften the hair shaft. Shave in the direction of hair growth using a sharp, single-blade or safety razor, which reduces the likelihood of cutting hair beneath the skin surface. Avoid multiple passes over the same area. Post-shave, rinse with cool water, apply a soothing, alcohol-free toner or aloe gel, and follow with a light, non-comedogenic moisturizer. Consider switching to electric trimmers (which leave a slight stubble above the skin) or depilatory creams formulated for sensitive areas to minimize follicular trauma.
- Exfoliate Gently: Use a mild chemical exfoliant like a body wash containing salicylic acid (BHA) or glycolic/lactic acid (AHA) once or twice a week to remove dead skin cells that can clog pores. Avoid harsh physical scrubs with jagged particles like crushed walnut shells, which cause micro-abrasions and worsen inflammation. Chemical exfoliants work more uniformly and safely dissolve the intercellular cement holding dead cells together. Always apply sunscreen to exposed areas when using AHAs, as they increase photosensitivity. Space exfoliation sessions appropriately to avoid compromising the skin barrier.
- Maintain a Healthy Lifestyle: A balanced diet rich in whole foods, adequate hydration (aiming for at least 64 ounces of water daily), and consistent stress management contribute to overall skin health. Focus on low-glycemic index carbohydrates, omega-3 fatty acids, and antioxidant-rich vegetables to modulate systemic inflammation. Limit high-sugar snacks and excessive dairy if you notice a correlation with flare-ups. Prioritize 7-9 hours of quality sleep nightly, as cellular repair and hormone regulation peak during restorative sleep phases. Regular physical activity improves circulation and metabolic health, but always pair exercise with immediate post-activity hygiene to prevent sweat-related breakouts.
Expert Quote
"The inner thigh is a common area for acne breakouts and pimple-like bumps because of the friction and moisture that builds up. I often tell my patients that simple changes like wearing breathable fabrics and using a benzoyl peroxide wash after workouts can drastically reduce these types of pimples. If a bump is very painful or doesn’t heal, it could be more than just a pimple – so don’t hesitate to see a dermatologist for evaluation." – Board-Certified Dermatologist
This clinical perspective emphasizes the dual importance of mechanical management and targeted active ingredients in daily care. Dermatologists consistently observe that patients who integrate preventative lifestyle adjustments with consistent, gentle topical therapy achieve faster clearance and lower recurrence rates. The quote also serves as an important reminder that while most inner leg pimples are benign and manageable, persistent or atypical lesions warrant professional assessment to rule out underlying inflammatory, infectious, or autoimmune conditions. Early specialist intervention not only resolves current symptoms but also prevents long-term complications like dyspigmentation and scarring, preserving both skin function and patient comfort.
Conclusion
Inner leg pimples are a common and treatable issue that affects individuals across all demographics due to the unique anatomical and environmental conditions of the inner thigh region. By understanding their causes—from mechanical friction and sweat accumulation to folliculitis, hormonal fluctuations, and chronic conditions like hidradenitis suppurativa—you can take informed, effective steps to manage active breakouts and prevent future occurrences. The foundation of successful treatment lies in consistent, gentle skin care: utilizing targeted over-the-counter actives like salicylic acid and benzoyl peroxide, prioritizing barrier-supportive moisturization, avoiding mechanical trauma, and promptly cleansing after perspiration. Good hygiene, proper clothing choices, mindful hair removal techniques, and lifestyle optimization serve as your first and most reliable lines of defense. Remember that skin health is deeply interconnected with overall wellness, and addressing systemic factors like diet, stress, and hormonal balance often amplifies the success of topical interventions. For persistent, deeply painful, or recurrent bumps that resist conservative management, seeking professional medical advice is the best course of action to ensure accurate diagnosis, access to prescription therapies, and long-term skin health. With patience, consistency, and evidence-based strategies, clear, comfortable skin on your inner thighs is entirely achievable.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare provider for any questions you may have regarding a medical condition or treatment. Never disregard professional medical advice or delay seeking it because of something you have read in this content. Individual skin types and medical histories vary, and treatments should be personalized by a licensed physician or dermatologist.
Frequently Asked Questions
Can inner leg pimples be contagious?
Typical inner leg pimples caused by acne, sweat, or friction are not contagious, as they result from blocked follicles, sebum production, and individual microbiome fluctuations rather than transmissible pathogens. However, if the bumps are caused by bacterial folliculitis (particularly Staphylococcus aureus or MRSA), fungal folliculitis, molluscum contagiosum, or scabies, they can potentially spread through direct skin-to-skin contact, sharing contaminated towels, clothing, or gym equipment. Practicing strict hygiene, avoiding sharing personal items, covering open or draining lesions with breathable bandages, and washing hands thoroughly after touching affected areas minimizes transmission risk. If you suspect a contagious skin infection, consult a healthcare provider for accurate diagnosis and isolation guidance.
Do inner leg pimples leave scars, and how can I prevent them?
Yes, inner leg pimples can leave post-inflammatory hyperpigmentation (dark spots), atrophic scars (indentations), or hypertrophic/keloid scars (raised tissue), especially if lesions are picked, squeezed, or become deeply infected. The inner thigh skin heals more slowly due to constant movement and friction, which can disrupt the remodeling phase of wound repair. To minimize scarring, resist the urge to pick or pop bumps, as mechanical trauma extends inflammation deeper into the dermis. Use targeted treatments like adapalene, niacinamide, or vitamin C serums once active inflammation resolves to accelerate cellular turnover and even out pigmentation. Always protect healing skin from sun exposure with clothing or broad-spectrum SPF 30+ if the area is uncovered, as UV radiation darkens post-inflammatory marks. For existing scars, a dermatologist may recommend silicone gel sheets, corticosteroid injections, chemical peels, microneedling, or laser therapy to stimulate collagen remodeling.
How long does it typically take for inner leg pimples to heal?
The healing timeline depends on the lesion type and treatment adherence. Superficial papules and pustules typically resolve within 7 to 10 days with appropriate topical care and friction management. Deep nodules or cysts may take 2 to 4 weeks or longer to fully flatten, as they involve significant dermal inflammation that requires extended cellular clearance. Ingrown hairs often resolve within a few days once the trapped hair is freed, but accompanying inflammation can persist longer. Folliculitis outbreaks usually improve within 7 to 14 days with targeted antimicrobial treatment. Consistent application of active ingredients requires 4 to 8 weeks to show significant reduction in new breakouts due to the skin's natural turnover cycle. Patience and routine consistency are crucial; prematurely switching products can reset progress and prolong irritation.
Is it safe to exercise or swim when I have active inner leg breakouts?
Yes, it is generally safe to exercise or swim, provided you take specific precautions to prevent worsening the breakouts or spreading infection. Physical activity supports circulation and immune function, which aids healing, but sweat and prolonged moisture can aggravate active lesions. Before working out, apply a protective, fragrance-free anti-chafing barrier if friction is a trigger. Wear loose, moisture-wicking, breathable workout attire, and change out of sweaty clothes immediately after finishing. Shower with a gentle cleanser as soon as possible post-activity. If swimming, chlorine in pools has mild antimicrobial properties that may help dry out superficial pimples, but it can also irritate compromised skin barriers; rinsing off pool water promptly and moisturizing afterward is essential. Avoid public hot tubs or saunas if you have open, draining, or actively infected lesions to prevent cross-contamination or deeper bacterial penetration.
What are the early warning signs that an inner thigh bump might be something more serious than a pimple?
Several clinical indicators suggest a bump may require professional medical evaluation rather than home acne care. These include: lesions that rapidly enlarge, become extremely painful to light touch, or feel hot and firm; systemic symptoms like fever, chills, fatigue, or swollen lymph nodes in the groin; red streaks radiating from the bump, which may indicate lymphangitis or spreading cellulitis; recurrent clusters of interconnected, draining tunnels that heal and reopen in the same area (classic signs of hidradenitis suppurativa); lesions that fail to improve after 6-8 weeks of consistent OTC treatment; or bumps accompanied by unusual discharge (foul-smelling, bloody, or persistently green/yellow pus). Additionally, if you have a compromised immune system, diabetes, or a history of recurrent staph infections, any new or persistent bump should be evaluated promptly to rule out abscesses, atypical mycobacterial infections, or other dermatological conditions requiring prescription intervention.

About the author
Elena Vance, MD, is a double board-certified dermatologist and pediatric dermatologist. She is an assistant professor of dermatology at a leading medical university in California and is renowned for her research in autoimmune skin disorders.