Why Are My Inner Thighs Dark? A Dermatologist-Approved Guide

Key points
- Wearing tight clothing or non-breathing fabrics.
- Having a body shape where thighs naturally touch.
- Being overweight, which can increase the surface area of skin-on-skin contact.
Dark skin on the inner thighs is an incredibly common experience, yet it often becomes a source of self-consciousness and concern. If you've found yourself wondering why this area is a different shade, you're not alone. The discoloration is usually harmless, but understanding its root causes is the first step toward effective management and feeling confident in your skin.
From a biological standpoint, skin pigmentation is not uniform across the human body. Evolutionarily, areas that experience frequent folding, bending, or friction naturally develop higher concentrations of melanocytes, the cells responsible for producing melanin. The groin and inner thigh region is also subject to fluctuating moisture levels, temperature changes, and unique hormonal receptor distributions, all of which contribute to a baseline pigmentation that is typically darker than sun-exposed areas like the face or arms. This natural variation is entirely physiological and should be distinguished from pathological hyperpigmentation that arises from disease or injury. Recognizing the difference between inherent anatomical pigmentation and acquired darkening is essential for setting realistic treatment goals and avoiding unnecessary stress.
This comprehensive guide, synthesized from dermatological advice, clinical studies, and real-user experiences, will explore the science behind dark inner thighs, differentiate between normal pigmentation and medical concerns, and outline the most effective strategies for treatment and prevention.
What Causes Dark Inner Thighs? Understanding Hyperpigmentation
The darker appearance of the skin on your inner thighs is a form of hyperpigmentation, which simply means the skin is producing an excess amount of melanin, the pigment that gives skin its color. This overproduction isn't random; it's a response to a trigger. Let's break down the most common culprits.
At the cellular level, melanogenesis is regulated by a complex interplay of genetic factors, inflammatory cytokines, and hormonal signals. When the epidermis experiences stress, it releases signaling molecules like prostaglandins, interleukins, and melanocyte-stimulating hormone (MSH). These compounds bind to receptors on melanocytes, upregulating tyrosinase activity—the key enzyme in melanin synthesis. The resulting pigment is then transferred to surrounding keratinocytes, creating the visible dark patches. Understanding this pathway is crucial because effective treatment strategies specifically target one or more steps in this cascade, from inhibiting tyrosinase to accelerating the shedding of pigment-laden keratinocytes.
Friction and Chafing (The Most Common Culprit)
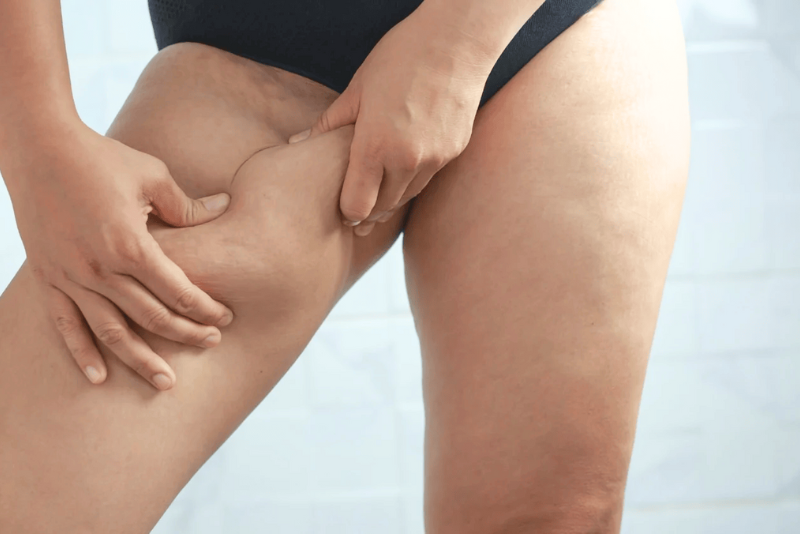
The primary cause for most people is chronic friction. When your thighs rub against each other while walking, running, or exercising, the skin becomes irritated and inflamed. To protect itself from this constant trauma, the skin thickens and produces more melanin, resulting in a darker appearance. This is known as post-inflammatory hyperpigmentation (PIH).
The biomechanics of chafing involve more than just simple rubbing. Sweat plays a compounding role by softening the stratum corneum (the outermost protective layer of skin) and increasing the coefficient of friction between surfaces. This combination of moisture, mechanical stress, and elevated skin temperature can trigger a localized inflammatory response. In response to micro-tears and repetitive shear forces, fibroblasts deposit thicker collagen, leading to epidermal hyperplasia, while melanocytes ramp up pigment production as a biological shield against further damage. Over time, this chronic cycle results in both textural changes and pronounced darkening.
Factors that increase friction include:
- Wearing tight clothing or non-breathing fabrics.
- Having a body shape where thighs naturally touch.
- Being overweight, which can increase the surface area of skin-on-skin contact.
To combat friction-induced PIH, dermatologists often recommend moisture-wicking synthetic blends over cotton for physical activity, as they draw sweat away from the skin and reduce maceration. Anti-chafing balms containing dimethicone or zinc oxide can create a protective barrier, while properly fitted compression shorts redistribute pressure and prevent direct skin-to-skin contact. Addressing the mechanical trigger is always the foundational step in resolving friction-related darkening.
Hormonal Fluctuations
Hormones play a significant role in regulating melanin production. Imbalances or shifts can lead to darkened skin in various areas, including the inner thighs.
Estrogen and progesterone receptors are highly expressed in cutaneous tissue, particularly in genital and inguinal regions. Fluctuations in these sex hormones can directly stimulate melanocyte activity by increasing tyrosinase synthesis and altering melanosome transfer. Additionally, systemic stress hormones like cortisol can indirectly affect pigmentation by modulating inflammatory pathways and altering insulin sensitivity. This hormonal cascade is why many individuals notice darkening during puberty, pregnancy, or perimenopause, times when endocrine shifts are most pronounced.
- Polycystic Ovary Syndrome (PCOS): This hormonal condition is often linked to insulin resistance, which can cause dark, velvety patches of skin known as acanthosis nigricans. In PCOS, elevated androgen levels combined with compensatory hyperinsulinemia lead to increased production of insulin-like growth factor 1 (IGF-1). IGF-1 binds to receptors on keratinocytes and fibroblasts, causing them to proliferate rapidly and create the characteristic thickened, hyperpigmented plaques.
- Pregnancy and Menstruation: Fluctuations in estrogen and other hormones during these times can stimulate excess melanin production. The placenta produces high levels of estrogen, progesterone, and melanocyte-stimulating hormone (MSH), which collectively drive the hyperpigmentation seen in melasma, linea nigra, and darker inguinal folds. While pregnancy-related darkening often fades postpartum, it can persist in some individuals, particularly those with naturally darker Fitzpatrick skin types.
- Hormonal Contraceptives: Some people may experience hyperpigmentation as a side effect of birth control pills. Combined oral contraceptives containing both estrogen and progestin mimic the high-hormone state of pregnancy, triggering similar melanogenic pathways in susceptible individuals.
Underlying Medical Conditions
While usually benign, dark inner thighs can sometimes signal an underlying health issue that needs attention.
Systemic metabolic and dermatological conditions frequently manifest in skin folds due to the unique microenvironment of these areas. Warmth, humidity, and occlusion make the groin particularly susceptible to conditions that thrive in intertriginous zones. Moreover, the skin's high concentration of insulin receptors and androgen receptors means it often serves as an early warning system for endocrine or autoimmune dysfunction.
- Acanthosis Nigricans: This is a key condition to be aware of. It causes dark, thick, velvety skin in body folds like the groin, armpits, and neck. It's strongly associated with insulin resistance, pre-diabetes, and type 2 diabetes. Treating the underlying cause is crucial for improving the skin's appearance. Weight management, dietary modifications focusing on low-glycemic index foods, and medications like metformin can significantly reduce insulin levels and, consequently, the skin changes. In rare cases, acanthosis nigricans can be associated with internal malignancies or certain endocrine tumors, making prompt evaluation essential if it appears suddenly.
- Fungal Infections: Infections like Tinea cruris (jock itch) can cause inflammation and lead to post-inflammatory hyperpigmentation even after the infection has cleared. Dermatophytes thrive in warm, moist environments and invade the stratum corneum, releasing enzymes that damage skin cells and provoke an immune response. The resulting erythema, scaling, and intense itching lead to scratching, which exacerbates PIH. Even after successful antifungal therapy, the residual melanin deposition can take months to fade.
- Genetic Disorders: In rare cases, conditions like Darier's disease can cause hyperpigmentation. Other inherited conditions such as incontinentia pigmenti or Laugier-Hunziker syndrome may also present with mucocutaneous pigmentation in flexural areas, typically accompanied by other dermatological or systemic findings.
Other Contributing Factors
- Skin Irritation: Eczema, psoriasis, or irritation from hair removal methods like shaving or waxing can inflame the skin and lead to darkening. Contact dermatitis from scented body washes, harsh detergents, or synthetic fragrances in underwear disrupts the skin barrier, allowing allergens to penetrate and trigger T-cell mediated inflammation that culminates in melanocyte activation.
- Dry Skin: A buildup of dead, dry skin cells can make the area appear darker. Xerosis impairs desquamation, the natural process by which the epidermis sheds pigmented corneocytes. This retention hyperpigmentation is often reversible with consistent hydration and gentle exfoliation.
- Medications: Certain drugs, including some chemotherapy agents and antibiotics, can cause hyperpigmentation as a side effect. Minocycline, amiodarone, and antimalarial drugs are notorious for depositing pigment complexes in the dermis or directly stimulating melanogenesis. This type of hyperpigmentation is often deeper and more resistant to topical treatments.
- Sun Exposure: UV radiation stimulates melanin production. If your inner thighs are exposed to the sun, they can become darker. While the groin is typically shielded from ultraviolet light, activities like swimming, wearing high-cut athletic shorts, or sunbathing in certain positions can lead to localized UV exposure. Consistent use of broad-spectrum SPF 30+ on exposed thigh areas is necessary for comprehensive pigment management.
 Source: Isya Aesthetics
Source: Isya Aesthetics
When to See a Doctor
It's important to distinguish between common hyperpigmentation and something that requires medical attention. You should consult a doctor or board-certified dermatologist if:
- The darkening appears suddenly and without an obvious cause.
- The skin's texture changes, becoming thick, velvety, or leathery.
- The area is painful, itchy, or has an odor.
- The discoloration is spreading rapidly.
- You have other symptoms that could indicate a condition like diabetes or PCOS.
A thorough dermatological evaluation often begins with a detailed history and physical examination, potentially aided by a Wood's lamp to differentiate epidermal from dermal pigmentation. If acanthosis nigricans is suspected, your provider may order fasting insulin, glucose tolerance tests, or hemoglobin A1c panels to assess metabolic health. For suspected fungal or bacterial etiologies, a simple skin scraping or KOH preparation can confirm the diagnosis. In ambiguous cases, a punch biopsy may be performed to rule out atypical cellular changes or rare genodermatoses. Establishing a precise diagnosis ensures that treatment targets the root cause rather than merely masking symptoms, which is especially important when systemic conditions are driving cutaneous changes.
How to Lighten Dark Inner Thighs: A Comprehensive Treatment Guide
Managing dark inner thighs requires a two-pronged approach: treating the existing discoloration and preventing it from recurring. Patience is key, as visible results can take several weeks or months.
The skin's epidermal turnover cycle averages 28 days in young adults but slows significantly with age, hormonal fluctuations, or metabolic stress. Because hyperpigmentation resides in the basal or suprabasal layers of the epidermis, or occasionally deeper in the dermis, topical agents and procedural interventions must work consistently over multiple turnover cycles to gradually fade excess melanin. Rapid lightening is neither physiologically possible nor dermatologically advisable, as aggressive approaches frequently trigger rebound inflammation and worsen PIH, particularly in Fitzpatrick skin types IV through VI.
At-Home Remedies and Lifestyle Adjustments
Prevention and gentle care are the foundation of any treatment plan.
- Minimize Friction:
- Wear loose-fitting, breathable clothing like cotton.
- Consider wearing anti-chafing shorts or bands under dresses and skirts.
- Keep the area dry, as moisture can worsen irritation. Incorporating moisture-wicking technical fabrics during exercise, applying talc-free barrier powders, and using silicone-based anti-friction sticks before prolonged walking or workouts can dramatically reduce mechanical stress on the skin. Additionally, maintaining a healthy weight through balanced nutrition and regular physical activity reduces the biomechanical load on the inner thighs, though it's important to remember that thigh-to-thigh contact is anatomically normal and does not inherently require weight modification unless accompanied by metabolic concerns.
- Gentle Exfoliation: Regularly sloughing off dead skin cells can help lighten the area. Use a mild chemical exfoliant (with acids like glycolic or lactic) or a gentle physical scrub (like sugar or oatmeal) 1-2 times a week. Avoid scrubbing irritated or broken skin. Chemical exfoliants work by disrupting the desmosomal bonds between corneocytes, allowing pigmented dead cells to shed more efficiently. Lactic acid and polyhydroxy acids (PHAs) like gluconolactone are particularly well-suited for the sensitive groin area, as they are humectants that exfoliate while simultaneously drawing moisture into the barrier, minimizing irritation compared to harsher alpha hydroxy acids (AHAs). Physical scrubs should be used sparingly; abrasive particles can cause micro-tears that trigger inflammation and subsequent melanogenesis, counteracting the desired lightening effect.
- Moisturize Daily: Keeping the skin hydrated and supple improves its barrier function and can reduce irritation from friction. Look for formulations containing ceramides, cholesterol, and fatty acids to replenish the lipid matrix, alongside humectants like hyaluronic acid, glycerin, or panthenol. A robust skin barrier resists environmental stressors, heals micro-abrasions more quickly, and maintains optimal desquamation rates, all of which contribute to a more even complexion over time. Apply moisturizer immediately after showering while the skin is still damp to lock in hydration, and consider incorporating a lightweight, non-comedogenic body oil or occlusive balm for nighttime barrier repair.
Avoid harmful DIY trends such as applying raw lemon juice, baking soda, or undiluted essential oils to the groin. These substances have extreme pH levels that disrupt the acid mantle, cause chemical burns, and dramatically increase the risk of severe PIH, contact dermatitis, or photosensitivity reactions. Evidence-based skincare prioritizes barrier integrity and gradual, controlled cellular renewal over aggressive, untested home mixtures.
Over-the-Counter (OTC) Topical Treatments
Look for products containing ingredients proven to target hyperpigmentation. These are often found in serums and creams.
- Niacinamide (Vitamin B3): A superstar ingredient that helps reduce the transfer of pigment within the skin, effectively lightening dark spots. At concentrations of 4-5%, niacinamide inhibits melanosome transfer from melanocytes to keratinocytes while simultaneously boosting ceramide synthesis and reducing transepidermal water loss. Its anti-inflammatory properties make it exceptionally well-tolerated, even in sensitive intertriginous zones.
- Kojic Acid: Derived from fungi, it inhibits an enzyme needed to produce melanin. Specifically, kojic acid chelates copper at the active site of tyrosinase, rendering the enzyme inactive. It is highly effective but can be sensitizing at high concentrations or in unstable formulations. Look for products that pair kojic acid with antioxidants like vitamin E to prevent oxidation and maintain efficacy.
- Azelaic Acid: Naturally found in grains, it reduces inflammation and decreases melanin production. At OTC strengths of 10%, azelaic acid selectively targets hyperactive melanocytes without affecting normally pigmented cells. It also possesses mild antibacterial and comedolytic properties, making it a versatile option if folliculitis or acneiform eruptions accompany the hyperpigmentation.
- Vitamin C (Ascorbic Acid): A powerful antioxidant that brightens skin and inhibits melanin production. Stable derivatives like magnesium ascorbyl phosphate, sodium ascorbyl phosphate, or ethyl ascorbic acid penetrate the skin and interrupt oxidative stress pathways that trigger melanogenesis. Vitamin C also enhances the efficacy of sunscreens and promotes collagen synthesis, improving overall skin resilience.
- Licorice Root Extract & Arbutin: These plant-derived ingredients are known for their skin-lightening properties. Glabridin, the active compound in licorice root, suppresses UV-induced pigmentation and exhibits potent anti-inflammatory activity. Alpha-arbutin acts as a competitive tyrosinase inhibitor, gradually fading pigmented lesions with minimal irritation risk.
One popular product, Topicals Faded Serum, combines several of these ingredients, including tranexamic acid, niacinamide, and azelaic acid, to tackle stubborn discoloration.
When layering multiple active ingredients, introduce them gradually to assess tolerance. A safe routine might involve alternating nights between a niacinamide-containing product and an AHA exfoliant, while using vitamin C in the morning. Always perform a patch test behind the ear or on the inner arm before applying new actives to larger or more sensitive areas. If stinging, redness, or peeling occurs beyond mild transient dryness, reduce frequency or discontinue use.
 Source: Sublime Life
Source: Sublime Life
Professional and Prescription-Strength Treatments
If OTC products aren't delivering the desired results, a dermatologist can offer more powerful solutions.
Dermatological interventions operate at deeper epidermal or dermal levels, utilizing controlled injury or targeted photothermolysis to accelerate pigment clearance. These treatments are particularly beneficial for stubborn PIH, acanthosis nigricans, or pigmentary disorders resistant to months of consistent topical therapy.
- Prescription Creams:
- Hydroquinone: Long considered a gold standard for lightening skin, it works by decreasing the number of melanocytes (pigment-producing cells). It should only be used under a doctor's supervision due to potential side effects like irritation or, rarely, a paradoxical darkening called ochronosis. Typically prescribed at 2-4% concentrations, hydroquinone competitively inhibits tyrosinase and induces melanocyte cytotoxicity. Treatment courses are generally limited to 3-4 months, followed by maintenance with alternative brightening agents to prevent rebound hyperpigmentation.
- Retinoids (Tretinoin): These Vitamin A derivatives speed up skin cell turnover, helping to shed pigmented cells and reveal lighter skin underneath. Tretinoin also enhances the penetration of other topical lightening agents and stimulates dermal remodeling. Starting with low concentrations (0.025%) and applying a pea-sized amount 2-3 times weekly, gradually increasing frequency as tolerated, minimizes retinoid dermatitis. Combining retinoids with a moisturizer in a "sandwich method" can buffer irritation without compromising efficacy.
- In-Office Procedures:
- Chemical Peels: A dermatologist applies a chemical solution (like high-concentration glycolic or salicylic acid) to exfoliate the top layers of skin. Medium-depth peels (TCA 15-25%) penetrate the papillary dermis to address deeper pigment deposits. Pre-peel conditioning with hydroquinone or retinoids for 2-4 weeks improves outcomes and reduces the risk of post-procedure hyperpigmentation, especially in darker skin tones. Multiple sessions spaced 4-6 weeks apart are typically required for optimal fading.
- Laser Therapy: Treatments like Intense Pulsed Light (IPL) or fractional lasers target melanin in the skin, breaking it up so the body can eliminate it. This is a highly effective but more expensive option. For patients with higher melanin content, Q-switched Nd:YAG lasers (1064 nm wavelength) are preferred because they penetrate deeply while minimizing epidermal melanin absorption, drastically reducing burn risk and PIH complications. Non-ablative fractional lasers create microthermal zones that stimulate collagen production and accelerate pigment dispersion. Strict sun avoidance and diligent post-procedure barrier repair are mandatory to prevent complications.
Watch this video to see how a DIY treatment using licorice root can be prepared at home:
Source: [YouTube - Farah Dhukai](https://www.youtube.com/watch?v=RqMu2VI-ozw)While DIY preparations can offer mild brightening, they lack standardized concentrations and stability testing. Clinical-grade formulations undergo rigorous stability, penetration, and safety evaluations, ensuring predictable results and minimizing the risk of adverse reactions in delicate anatomical regions.
The Psychological Impact and Normalization
It's crucial to acknowledge the emotional toll that concerns about dark inner thighs can take. In a society saturated with filtered images, it's easy to feel that any deviation from a uniform skin tone is a flaw. Many people, as shared in online forums like Reddit, feel self-conscious to the point that it affects their intimacy and confidence.
Body image distress related to intimate area hyperpigmentation often stems from culturally reinforced beauty standards that equate pale, uniform skin with cleanliness, youth, and attractiveness. These narratives frequently ignore biological reality and disproportionately impact individuals with darker constitutive skin tones, who naturally produce more baseline melanin. Clinicians increasingly recognize that addressing the psychological burden is as important as treating the physical manifestation. Cognitive behavioral strategies, media literacy education, and open conversations about anatomical diversity can significantly alleviate distress. For those experiencing severe body dysmorphia or avoidance behaviors, referral to a mental health professional specializing in body image issues can be profoundly beneficial.
However, there is a strong and growing conversation around normalization. As dermatologist Dr. Priyanka Reddy explained to Vogue, skin in areas of friction is supposed to be different. "That pigmentation is the skin protecting itself... It’s a functional response, not a flaw."
Dermatological science consistently affirms that flexural hyperpigmentation is a physiological adaptation, not a pathology. Melanocytes in skin folds are naturally more active, and the cumulative effect of friction, hormonal fluctuations, and natural aging makes this darkening virtually universal across all ethnicities. Recognizing this biological baseline empowers individuals to make informed choices: pursuing treatment for personal comfort is entirely valid, but doing so out of shame or unrealistic expectations is unnecessary and potentially harmful. True skin health prioritizes barrier function, comfort, and informed care over arbitrary aesthetic ideals.
Dark inner thighs are a normal variation of the human body, especially in people with more melanin-rich skin tones. Pursuing treatment should be a personal choice for your own comfort, not a response to societal pressure.
Key Takeaways
- Dark inner thighs are common and usually harmless, caused primarily by friction, hormones, or underlying medical conditions.
- A multi-step approach involving minimizing friction, gentle exfoliation, and using targeted topical ingredients can significantly improve their appearance.
- Consult a dermatologist for a proper diagnosis, especially if the discoloration is sudden, changes in texture, or is accompanied by other symptoms.
- Remember that this is a normal skin variation. Treatment is a personal choice, not a necessity.
By understanding the causes and available solutions, you can take control of your skin's health and, most importantly, feel comfortable and confident in your own body. Consistency, patience, and a barrier-supportive routine will yield the most sustainable and health-focused results.
Frequently Asked Questions
Can dark inner thighs be a sign of insulin resistance or diabetes?
Yes, dark inner thighs can sometimes indicate insulin resistance, particularly when accompanied by acanthosis nigricans. This condition presents as velvety, hyperpigmented plaques in skin folds like the groin, armpits, and neck. Insulin resistance causes elevated circulating insulin levels, which cross-react with insulin-like growth factor 1 (IGF-1) receptors on skin cells, stimulating rapid keratinocyte and fibroblast proliferation alongside increased melanin deposition. If your darkened skin has a noticeably thickened or rough texture, or if you experience other metabolic symptoms like unexplained weight changes, fatigue, or increased thirst, consult a healthcare provider for fasting glucose, HbA1c, and fasting insulin testing. Addressing underlying metabolic dysfunction through dietary changes, regular physical activity, and medical management when indicated often leads to significant improvement in the skin's appearance over several months.
How long does it take to see results from topical lightening treatments?
Visible improvements from topical lightening agents typically require 8 to 12 weeks of consistent, daily application, though some individuals may notice subtle brightening as early as 4 weeks. The epidermal turnover cycle averages 28 days in healthy adults, and hyperpigmentation resides in the deeper basal or spinous layers, meaning it takes multiple cellular renewal cycles to gradually transport melanin-loaded cells to the surface and shed them. Factors like the depth of pigment, skin type, adherence to the regimen, and concurrent friction management all influence the timeline. Deeper dermal pigmentation, medication-induced discoloration, or untreated underlying conditions may require 3 to 6 months or professional intervention. Consistency, proper moisturization, and avoiding irritants are far more critical than aggressively applying multiple products at once, which can compromise the barrier and trigger rebound darkening.
Are there any safe home remedies that actually work for dark inner thighs?
The safest and most evidence-supported home approaches focus on gentle chemical exfoliation, barrier repair, and friction reduction rather than aggressive bleaching. Regular application of body lotions containing 5-10% lactic acid, glycolic acid, or urea can safely accelerate the shedding of pigmented dead skin cells while maintaining hydration. Natural ingredients like niacinamide (found in some stabilized OTC formulations) and licorice root extract have documented tyrosinase-inhibiting and anti-inflammatory properties when properly formulated. However, avoid harsh DIY mixtures containing undiluted lemon juice, baking soda, apple cider vinegar, or hydrogen peroxide, as their extreme pH disrupts the acid mantle, causes micro-burns, and frequently worsens post-inflammatory hyperpigmentation. If you prefer natural approaches, focus on gentle cleansing, daily moisturization with ceramides and panthenol, wearing breathable fabrics, and maintaining a healthy weight to minimize mechanical friction.
Does shaving or waxing cause permanent darkening of the inner thighs?
Shaving and waxing do not cause permanent darkening, but they can trigger temporary post-inflammatory hyperpigmentation if they lead to irritation, micro-cuts, ingrown hairs, or folliculitis. Repeated trauma to the epidermis during hair removal stimulates melanocytes to produce excess pigment as a protective response. Additionally, chronic ingrown hairs can cause localized inflammation and scarring, leaving behind residual brown spots long after the active inflammation resolves. To minimize this risk, consider alternative hair removal methods like electric trimmers (which leave a slight stubble without cutting skin-level), laser hair removal (which reduces follicular inflammation long-term), or depilatory creams formulated for sensitive skin. Always use a sharp, clean razor, shave in the direction of hair growth, apply a soothing, fragrance-free moisturizer or aloe vera post-shave, and never exfoliate immediately before or after hair removal to avoid compounding skin stress.
Should I be concerned if my inner thighs are naturally darker than the rest of my legs?
In most cases, no. It is entirely normal for the skin on the inner thighs, groin, elbows, knees, and axillae to be darker than sun-exposed areas. These regions naturally contain a higher density of melanocytes, experience constant folding and friction, and have greater exposure to fluctuating hormones and moisture levels. From a dermatological and evolutionary perspective, this baseline pigmentation serves as a protective mechanism against mechanical stress and maintains barrier integrity. Concern is only warranted if the darkening develops suddenly, spreads rapidly, changes in texture (becoming raised, velvety, scaly, or cracked), or is accompanied by itching, pain, odor, or systemic symptoms. If the pigmentation has been stable since adolescence or has gradually developed over years without accompanying symptoms, it is almost certainly a benign anatomical variation that requires no medical intervention.
References:
- Healthgrades Health Library. (2022). Treating Dark Inner Thighs: Causes, Remedies, and More. Link
- Medical News Today. (2019). Dark inner thighs: Treatments and home remedies. Link
- Tua Saúde. (2025). Dark Inner Thighs: 6 Causes (& How to Lighten). Link
- SkyMD. (n.d.). 3 Dermatologist approved ways for treating dark inner thighs. Link
- Vogue India. (2025). Head, shoulders, knees and toes—now with their own skincare routines. Link

About the author
Elena Vance, MD, is a double board-certified dermatologist and pediatric dermatologist. She is an assistant professor of dermatology at a leading medical university in California and is renowned for her research in autoimmune skin disorders.