Black Dot on Eyeball White: Causes, Risks, Diagnosis, and Treatment
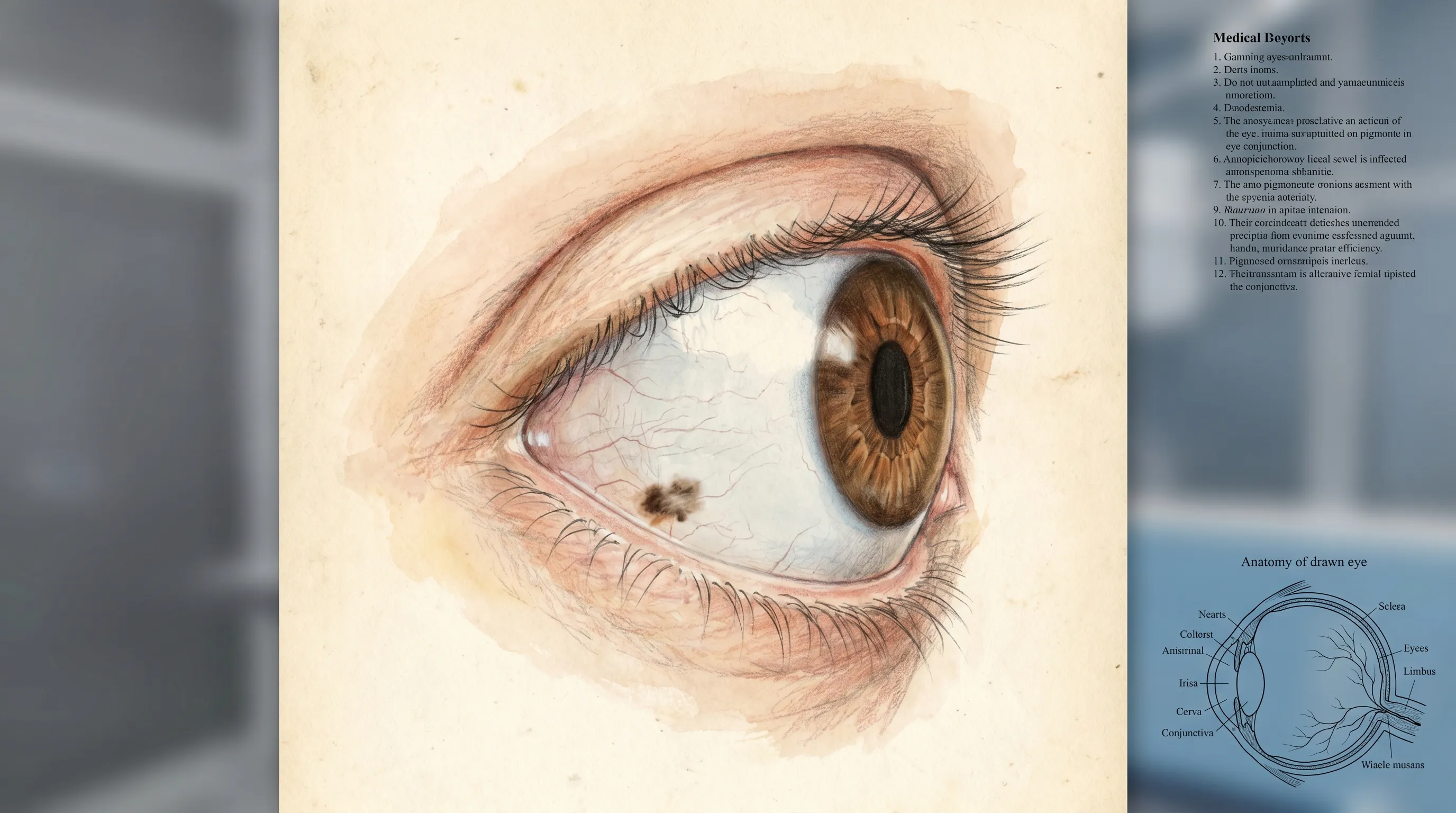
Noticing a black dot on eyeball white can be an alarming experience, especially since the eyes are highly visible and essential to daily functioning. Whether you spot it in the mirror or during a routine self-check, your immediate concern is likely whether it signals a serious medical condition or a harmless anatomical variation. In clinical practice, this presentation is remarkably common, and the overwhelming majority of cases are completely benign. A dark or black spot on the sclera—the white, outer protective layer of the eye—is typically the result of localized melanin deposition within the conjunctival tissue. Understanding the underlying anatomy, the range of possible causes, and the clinical pathways for evaluation is crucial for maintaining ocular health and preventing unnecessary anxiety. While most pigmented lesions are merely 'eye freckles' that require nothing more than periodic observation, a small fraction can represent precancerous changes or early-stage malignancies. Therefore, professional assessment, combined with patient education on warning signs and preventative strategies, forms the cornerstone of modern ophthalmic care. By familiarizing yourself with the diagnostic process, risk factors, and evidence-based management options, you can take a proactive approach to preserving your vision and overall eye wellness. This comprehensive guide breaks down exactly what these spots are, how medical professionals evaluate them, and what steps you should take to ensure optimal long-term outcomes.
Understanding the Anatomy and Prevalence of Scleral Pigmentation
The human eye is a complex organ protected by multiple layers of tissue, and the white area visible to the naked eye is actually a combination of the sclera and the overlying conjunctiva. The sclera itself is a tough, fibrous, opaque structure that maintains the eye's shape and provides attachment points for the extraocular muscles. Covering the anterior portion of the sclera is a thin, transparent mucous membrane called the bulbar conjunctiva. This membrane contains a rich network of blood vessels and immune cells, but it also harbors melanocytes—specialized cells responsible for producing melanin, the pigment that gives color to skin, hair, and eyes. When melanocytes cluster or proliferate in a localized area, they can create a visible dark spot on the eye's surface. Research from the Bascom Palmer Eye Institute at the University of Miami indicates that conjunctival nevi account for approximately 17.2% to 42% of all conjunctival tumors, highlighting just how frequently these pigmented lesions appear in the general population.
Demographic trends reveal distinct patterns in how and when these spots develop. They most frequently present in individuals with lighter skin tones during the first to early third decades of life, though they can be congenital or appear later. Gender distribution remains relatively equal, but certain genetic predispositions and environmental exposures play a significant role in their formation and evolution. Importantly, melanocytic activity in the conjunctiva is highly sensitive to both ultraviolet radiation and systemic hormonal shifts. Studies tracking over 400 patients with documented conjunctival nevi found that color changes occurred in 13% of cases, while size changes were noted in 8%. These alterations are rarely sudden and are often linked to life stages characterized by intense endocrine activity. Recognizing that a black dot on eyeball white is fundamentally a biological variation rather than an automatic disease marker helps patients approach evaluation with clarity and calm. The conjunctival tissue also possesses remarkable healing capacity, which influences how benign lesions are managed compared to malignant transformations.
Primary Causes and Differential Diagnosis of Dark Ocular Spots
Identifying the exact nature of a pigmented lesion requires a systematic differential diagnosis, as several distinct conditions can manifest as a dark mark on the eye's surface. While they may appear similar to an untrained observer, their cellular origins, growth patterns, and clinical implications vary dramatically. Eye care professionals categorize these findings into benign melanocytic lesions, precancerous conditions, rare malignancies, and non-melanocytic mimics. Each category demands a different management strategy, ranging from simple observation to urgent surgical intervention.
Conjunctival Nevus (The Most Common Cause)
A conjunctival nevus is essentially an ocular mole, formed by a localized proliferation of benign melanocytes within the epithelial or subepithelial layers of the conjunctiva. These lesions are typically well-demarcated, round or oval, and can range in color from pale tan to deep brown or nearly black. Approximately half of all conjunctival nevi contain characteristic intralesional epithelial inclusion cysts, which appear as tiny translucent bubbles under magnification and serve as a strong clinical indicator of benignity. They are most commonly found in the interpalpebral bulbar conjunctiva—the area of the white eye visible when the eyelids are open—particularly near the limbus (the border between the cornea and sclera). Because they are stable and asymptomatic, they rarely require treatment unless they grow rapidly, cause mechanical irritation, or raise cosmetic concerns.
Scleral Melanocytosis and Racial Melanosis
Scleral melanocytosis is a rare, typically unilateral condition characterized by diffuse or patchy blue-gray to brownish-black pigmentation that extends deep into the episcleral tissue. Unlike superficial conjunctival freckles, this condition results from dermal melanocytes that fail to migrate properly during embryonic development. It is usually congenital, asymptomatic, and does not compromise visual acuity. However, it does carry a slightly elevated lifetime risk of uveal melanoma, warranting periodic fundoscopic monitoring. Racial melanosis, on the other hand, presents as bilateral, irregularly shaped brown-tan patches on the conjunctiva, predominantly affecting individuals with darker skin pigmentation. This condition represents a physiological variation in baseline melanocyte distribution and is entirely benign. It typically appears symmetrically and remains stable throughout adulthood without requiring any intervention.
Primary Acquired Melanosis (PAM)
Primary acquired melanosis is a flat, unilateral, brownish patch that appears on the conjunctival surface in middle-aged to older adults. Unlike congenital nevi, PAM develops later in life and carries significant clinical weight because approximately half of the cases lack cytologic atypia (PAM without atypia), while the other half exhibit dysplastic cellular changes (PAM with atypia). The latter category is considered a direct precursor to conjunctival melanoma. PAM lesions tend to spread horizontally rather than vertically, often covering a larger surface area than discrete nevi. Clinical evaluation must distinguish between stable melanosis and actively proliferating dysplasia. When PAM with atypia is suspected, ophthalmologists recommend close surveillance, photographic documentation, and sometimes map biopsies to rule out early malignant transformation.
Ocular and Conjunctival Melanoma
Conjunctival melanoma accounts for roughly 5% of all ocular melanocytic tumors. It is an aggressive malignancy that can arise de novo, from pre-existing PAM, or, rarely, from a malignant transformation of a nevus. Clinically, it often presents as a nodular, highly vascularized lesion with feeder blood vessels, irregular borders, and potential ulceration. Patients may report localized thickening, a foreign body sensation, or unexplained irritation. Prompt diagnosis is critical, as conjunctival melanoma can invade adjacent structures, metastasize to regional lymph nodes, or spread systemically. Management involves wide local excision, cryotherapy to the surgical margins, adjuvant topical chemotherapy, and sometimes radiotherapy depending on staging.
Non-Melanocytic Mimics
Not every dark spot on the sclera originates from melanin. Axenfeld nerve loops are normal anatomical variations where long posterior ciliary nerves pierce the sclera near the limbus. They appear as small, grayish-blue dots with an overlying thin blood vessel and are completely harmless. Subconjunctival hemorrhages, caused by ruptured tiny blood vessels, can initially present as bright red patches that gradually darken to deep brown or black as the blood breaks down. These typically resolve within two to three weeks without treatment and are often triggered by coughing, heavy lifting, or minor ocular trauma.
Clinical Evaluation and Diagnostic Pathways
When a patient presents with a black dot on eyeball white, the diagnostic process relies on advanced optical instrumentation, imaging technology, and systematic clinical documentation. Eye specialists do not diagnose based on visual inspection alone; instead, they follow a standardized protocol designed to differentiate benign nevi from suspicious or malignant lesions. Accurate identification prevents unnecessary procedures for harmless freckles while ensuring that potentially dangerous growths are intercepted early.
The Slit Lamp Examination
The slit lamp biomicroscope remains the gold standard for evaluating anterior segment lesions. By projecting a high-intensity, narrow beam of light into the eye, the ophthalmologist can achieve magnifications up to 40x. This reveals critical morphological details such as lesion borders, surface topography, vascular patterns, cystic inclusions, and depth of pigmentation. During this examination, clinicians assess for the presence of intrinsic cysts, which strongly favor a diagnosis of a benign nevus. They also evaluate the surrounding conjunctiva for satellite lesions, feeder vessels, or signs of epithelial disruption. The dynamic nature of the slit lamp allows practitioners to observe how light interacts with the tissue, differentiating superficial pigment from deeper scleral involvement.
Advanced Imaging and Documentation Protocols
Anterior Segment Optical Coherence Tomography (AS-OCT) has revolutionized non-invasive evaluation of pigmented lesions. This cross-sectional imaging modality provides micrometer-resolution scans of the conjunctiva and underlying episcleral tissue. It can highlight sub-clinical cysts, measure lesion thickness, and detect early subepithelial invasion that might be invisible during standard examination. Furthermore, high-resolution digital photography is routinely employed to establish a baseline. Many clinics utilize specialized anterior segment cameras with standardized lighting and magnification settings to capture precise color and topographical details. These images are stored in the patient's medical record and compared during subsequent visits to detect even millimeter-scale growth or subtle pigment shifts.
Histopathological Analysis and Excisional Biopsy
When clinical and imaging findings raise suspicion for malignancy, surgical intervention becomes necessary. Excisional biopsy with clear margins remains the definitive diagnostic procedure. The lesion is carefully removed, oriented, and sent to a specialized ocular pathology laboratory. Histopathologists examine the tissue under a microscope, evaluating cellular architecture, nuclear atypia, mitotic figures, and stromal invasion. Immunohistochemical staining for markers such as HMB-45, Melan-A, and S100 helps confirm melanocytic origin and differentiate melanoma from benign hyperplasia. This pathological correlation directly guides subsequent treatment planning and follow-up intervals.
| Feature | Conjunctival Nevus | Primary Acquired Melanosis (PAM) | Conjunctival Melanoma |
|---|---|---|---|
| Onset | Childhood to young adulthood | Middle age or older | Middle age or older |
| Appearance | Discrete, well-circumscribed nodule or patch | Flat, diffuse, patchy pigmentation | Nodular, elevated, highly vascular |
| Cystic Inclusions | Present in ~50% of cases | Absent | Typically absent |
| Growth Pattern | Slow, stable, or hormonally influenced | Horizontal spread, may progress slowly | Rapid, vertical and invasive growth |
| Malignant Potential | Very low (rarely transforms) | Moderate to high (if atypia is present) | High (requires aggressive management) |
Cancer Risk Assessment and Warning Signs
Understanding the malignancy potential of pigmented conjunctival lesions is essential for patient safety, even though the statistical likelihood of transformation remains low. Most black spots on the eye's white are benign, but vigilance ensures early detection if cellular changes occur. The risk stratification process considers demographic factors, lesion characteristics, and environmental exposures to determine the appropriate level of clinical surveillance.
Key Risk Factors for Malignant Transformation
According to the Mayo Clinic, several demographic and clinical factors elevate the baseline risk for conjunctival and uveal melanoma. Light eye color, particularly blue or green irises, correlates with reduced ocular melanin and higher susceptibility to ultraviolet-induced DNA damage. Being White or of Caucasian descent is another significant epidemiological risk factor, though conjunctival melanoma can affect all ethnicities. Increasing age correlates with cumulative environmental exposure and cellular aging. Additionally, individuals with dysplastic nevus syndrome (atypical mole syndrome), pre-existing ocular melanocytosis, or chronic UV exposure require heightened monitoring. Hormonal therapies and immunosuppressive conditions may also modulate melanocyte behavior, though research in this area continues to evolve.
Red Flags That Demand Immediate Ophthalmic Evaluation
Not all changes in ocular pigmentation are benign, and recognizing early warning signs can be vision-saving or life-saving. Patients should schedule an urgent eye examination if they notice a black dot on eyeball white that undergoes rapid growth, becomes irregularly shaped, or darkens significantly within weeks to months. Visual disturbances such as sudden onset of floaters, flashing lights, peripheral vision loss, or persistent blurriness warrant immediate investigation. Physical symptoms including unexplained eye pain, persistent foreign body sensation, localized thickening, bleeding from the spot, or redness that fails to resolve with standard care are also critical indicators. Delaying evaluation in the presence of these symptoms can allow malignant cells to invade deeper tissues or metastasize. As noted by clinical experts, early-stage melanoma confined to the conjunctiva has a dramatically higher survival rate than advanced disease.
Treatment Pathways and Clinical Management Strategies
Once a diagnosis is established, the treatment plan aligns with the lesion's biological behavior, symptomatic impact, and patient preferences. Management ranges from conservative observation to multi-modal surgical therapy, with the primary goal of preserving ocular function, preventing malignant spread, and maintaining cosmetic integrity when feasible.
Active Surveillance for Benign Nevi
For confirmed conjunctival nevi without atypical features, observation is the standard of care. Patients undergo comprehensive dilated eye exams annually or biennially, during which clinicians document lesion dimensions, color, and vascularity. Many eye care providers utilize digital mapping software to overlay sequential photographs, enabling precise measurement of microscopic changes over time. Patients are educated on self-monitoring techniques and instructed to report any sudden alterations between scheduled visits. This approach minimizes unnecessary surgical trauma while ensuring that slow progression does not go unnoticed.
Surgical Excision and Cryotherapy
When a lesion exhibits suspicious characteristics or demonstrates documented growth, surgical excision is performed under local or general anesthesia. The surgeon removes the entire nevus along with a narrow margin of healthy conjunctival tissue to ensure complete clearance. To eliminate residual microscopic cells and reduce recurrence risk, double freeze-thaw cryotherapy is applied to the surgical bed. The resulting defect is typically closed with fine absorbable sutures or secured using medical-grade tissue adhesive. Postoperative care involves antibiotic and steroid eye drops to prevent infection and control inflammation. Pathological analysis of the excised tissue confirms the diagnosis and guides long-term follow-up scheduling.
Laser Ablation and Cosmetic Considerations
For patients with stable, biopsy-confirmed benign nevi that cause cosmetic distress, laser treatment offers a minimally invasive alternative. Q-switched Nd:YAG or diode lasers target melanin selectively, fragmenting pigment particles that are subsequently cleared by macrophages. Multiple sessions spaced several months apart are often necessary to achieve uniform lightening without causing conjunctival scarring or symblepharon formation. While laser therapy improves appearance, it does not eliminate the underlying melanocytes, meaning recurrence is possible. Patients must understand that cosmetic intervention carries inherent risks and should only be pursued after thorough counseling and confirmation of benign status.
The Dangers of DIY and Over-the-Counter Eye Spot Removal
The eye is an exquisitely sensitive organ with zero tolerance for unregulated chemical or physical interventions. There are absolutely no FDA-approved drops, serums, or at-home kits that can safely remove a black dot on eyeball white. Attempting self-treatment with unverified substances risks chemical conjunctivitis, corneal epithelial defects, permanent scarring, secondary infections, and irreversible vision impairment. Furthermore, masking the appearance of a pigmented lesion without professional evaluation could delay the diagnosis of early melanoma. Always consult a board-certified ophthalmologist before considering any intervention.
Evidence-Based Prevention and Long-Term Eye Health
While genetic predisposition and developmental factors cannot be altered, modifiable environmental and lifestyle elements play a substantial role in melanocyte regulation and conjunctival health. Implementing proactive ocular protection strategies significantly reduces the cumulative burden of ultraviolet damage and supports long-term visual wellness.
Ultraviolet Radiation and Melanocyte Activation
Chronic exposure to ultraviolet A (UVA) and ultraviolet B (UVB) radiation stimulates melanocyte proliferation and increases oxidative stress within ocular tissues. UV rays penetrate the cornea and conjunctiva, triggering DNA mutations that may contribute to nevi formation, PAM development, or malignant transformation over decades. Wearing 100% UV-protective sunglasses that block both UVA and UVB wavelengths is the most effective preventive measure. Wraparound frames provide additional lateral shielding, reducing peripheral light exposure. Patients should also utilize wide-brimmed hats during peak sunlight hours and avoid tanning beds, which emit concentrated UV radiation.
Scheduling Regular Comprehensive Eye Examinations
Routine eye care extends far beyond vision prescription updates. Annual comprehensive examinations include tonometry, slit lamp biomicroscopy, dilated retinal evaluation, and conjunctival screening. Early detection of pigmented abnormalities allows clinicians to establish baselines, monitor subtle changes, and intervene before malignancy develops. Patients with multiple nevi, family histories of ocular cancer, or diagnosed PAM should adhere to stricter surveillance intervals as directed by their specialist. Building a long-term relationship with a licensed optometrist or ophthalmologist ensures continuity of care and personalized risk management.
Practical Self-Monitoring Techniques at Home
While professional evaluation remains essential, informed patients can participate actively in their ocular health maintenance. Using a clean mirror in bright, natural lighting, individuals should inspect both eyes monthly, noting the location, size, and color of any pigmented spots. Smartphone cameras with macro capabilities or ring-light attachments can document lesions for comparison, though they cannot replace clinical imaging. Any new appearance of a black dot on eyeball white should be logged with the date and brought to the next appointment. Consistency in documentation empowers both patients and providers to track evolutionary patterns accurately. Additionally, maintaining systemic health through balanced nutrition, hydration, and avoiding tobacco use supports overall tissue integrity and immune surveillance.
Frequently Asked Questions
Is a black dot on the white of my eye dangerous?
In the vast majority of cases, a black dot on the white of the eye is a benign conjunctival nevus and poses no threat to vision or overall health. However, because a small percentage can develop into conjunctival melanoma, regular monitoring by an eye care professional is essential to track any changes in size, shape, or color.
What is the difference between a conjunctival nevus and eye melanoma?
A conjunctival nevus is a benign cluster of pigment-producing cells that typically remains stable or changes slowly over decades. Conjunctival melanoma is a rare malignant tumor that grows rapidly, often presents with prominent feeding blood vessels and irregular borders, and requires immediate surgical and oncological management. Definitive diagnosis relies on clinical evaluation and histopathology.
Can hormonal changes cause an eye freckle to change appearance?
Yes. Clinical research demonstrates that conjunctival nevi can undergo pigment and size alterations due to endocrine fluctuations. Puberty, pregnancy, and oral contraceptive use have been documented to trigger melanocyte activity, making periodic professional evaluation particularly important during these physiological transitions.
How do eye doctors safely remove a dark spot on the sclera?
Removal typically involves surgical excision under local anesthesia, followed by microscopic tissue analysis to confirm benign status. For confirmed benign lesions removed for cosmetic reasons, targeted laser therapy may be offered. Both procedures are performed by trained ophthalmic surgeons to preserve ocular surface integrity and minimize scarring.
Can I use over-the-counter eye drops or home remedies to fade the spot?
No. There are no safe, FDA-approved topical agents or home remedies for removing a black dot on eyeball white. DIY treatments risk severe chemical injury, infection, corneal scarring, and permanent vision loss. Professional evaluation is the only medically sound approach to diagnosis and management.
Conclusion
Discovering a black dot on eyeball white is a surprisingly common experience that, while initially concerning, is most often traced to a harmless conjunctival nevus or a benign physiological variation in melanocyte distribution. The key to optimal outcomes lies in understanding that ocular pigmentation exists on a spectrum—from completely normal freckles to rare, clinically significant lesions requiring intervention. Relying on evidence-based evaluation, including slit lamp examination, anterior segment imaging, and professional documentation, ensures accurate classification and appropriate management. Patients should embrace regular comprehensive eye exams as a foundational pillar of preventive healthcare, utilize high-quality UV protection daily, and practice mindful self-observation without succumbing to unverified DIY treatments. By staying informed, recognizing early warning signs, and maintaining open communication with qualified eye care specialists, individuals can confidently navigate the management of conjunctival pigmentation while safeguarding their long-term visual health. The eye's remarkable resilience, combined with modern diagnostic technology, makes it entirely possible to monitor, treat, and preserve ocular wellness across a lifetime.


About the author
Elena Vance, MD, is a double board-certified dermatologist and pediatric dermatologist. She is an assistant professor of dermatology at a leading medical university in California and is renowned for her research in autoimmune skin disorders.