Permanent Retainers: The Complete Guide to Pros, Cons, Cost, and Care

Key points
- Constant Retention: It's always working, providing the best defense against tooth relapse.
- Invisible: Since it's bonded to the back of your teeth, no one will know it's there.
- No Compliance Needed: Ideal for individuals who might forget to wear a removable retainer consistently.
- Durable: Unlike removable retainers, it can't be lost, accidentally thrown away, or warped by heat.
After completing orthodontic treatment with braces or clear aligners, the next crucial phase begins: retention. To prevent your teeth from shifting back to their original positions—a process known as relapse—orthodontists recommend retainers. One popular option is the permanent retainer, also known as a bonded or fixed retainer.
While it offers a "set it and forget it" advantage, the reality of a permanent retainer is more complex. This guide covers everything you need to know, from its benefits and drawbacks to cost, care, and potential long-term issues. Understanding the biological, mechanical, and clinical aspects of fixed retention will empower you to make informed decisions about your orthodontic aftercare and long-term oral health. The retention phase is not merely a follow-up to treatment; it is an essential, lifelong component of maintaining a healthy, functional, and aesthetically pleasing smile. Orthodontic relapse occurs because the periodontal ligaments and surrounding bone require significant time to fully remodel and stabilize around the newly positioned teeth. Even after braces are removed, natural aging processes, habitual tongue thrusting, nocturnal bruxism, and subtle shifts in dental arches can exert forces that gradually undo months or years of careful alignment. This physiological reality underscores why retention is non-negotiable, and why choosing the right retention modality is one of the most important post-treatment decisions you will make alongside your dental care team.
What Is a Permanent Retainer?
A permanent retainer is a thin, custom-fitted wire, typically made of metal, that is bonded to the back (lingual side) of your teeth. It is most commonly placed on the lower front four to six teeth, as this area is highly prone to shifting. While they can be placed on the upper teeth, it's less common because the bite can put more pressure on the upper wire, increasing the risk of breakage.
Its primary purpose is to provide continuous retention, holding your teeth in their newly straightened positions 24/7 without requiring you to remember to put it in or take it out.
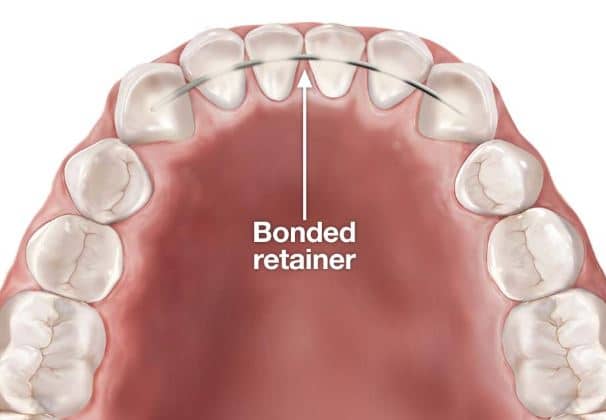 Image source: Orthodontic Specialists of White Plains
Image source: Orthodontic Specialists of White Plains
The fabrication and placement of a fixed retainer involve precise clinical techniques. Orthodontists typically use a multi-strand, braided stainless steel wire because its flexible nature allows it to adapt to minor physiological tooth movements without causing undue stress on the periodontium. In some modern practices, fiber-reinforced composite wires are utilized for patients with metal allergies or those seeking a tooth-colored aesthetic, though these materials generally have a shorter lifespan and lower fracture resistance compared to metallic options. The bonding process begins with meticulous cleaning and etching of the lingual enamel surfaces to create micro-retentive pores. A dental adhesive is then applied, followed by precise placement of the retainer wire. Orthodontists often use dental floss as a spacer to maintain proper interproximal contact while curing a light-polymerized composite resin. This step-by-step protocol ensures optimal bond strength while preserving the natural occlusal relationships. Ideal candidates for fixed retention are typically patients with a high risk of relapse, such as those who previously had severe crowding, midline diastemas (gaps), or rotated canines. Additionally, individuals who travel frequently, lead active lifestyles, or struggle with routine adherence to removable appliance wear often benefit greatly from the continuous protection a bonded wire provides.
The Great Debate: Permanent vs. Removable Retainers
Choosing a retainer is a significant decision. While your orthodontist will provide a recommendation based on your specific needs, it's helpful to understand the differences between permanent and removable options.
| Feature | Permanent (Bonded) Retainer | Removable Retainer (Essix/Hawley) |
|---|---|---|
| Effectiveness | Highly effective, as it works continuously without relying on patient compliance. | Effectiveness depends entirely on the patient consistently wearing it as directed. |
| Appearance | Invisible from the front. | Clear (Essix) retainers are discreet but can be noticeable. Hawley retainers have a visible wire. |
| Oral Hygiene | Challenging. Requires special tools like floss threaders to clean properly. | Easy. The retainer is removed for normal brushing and flossing. |
| Convenience | No need to remember to wear, remove, or store it. | Must be removed for eating and drinking (anything other than water) and stored safely. |
| Risk | Can break or debond. May lead to plaque/tartar buildup if not cleaned well. | Can be easily lost, misplaced, or damaged if not stored correctly. |
Many orthodontists recommend a combination approach: a permanent retainer on the lower teeth and a removable one for the upper teeth. This hybrid retention strategy is increasingly favored in contemporary orthodontics because it leverages the biomechanical strengths of both modalities. The lower anterior segment is historically the most unpredictable area following orthodontic treatment due to natural mesial drift and the powerful influence of the lower lip musculature. By securing this region with a fixed retainer, patients eliminate the most common site of relapse. Meanwhile, the upper arch, which generally exhibits greater stability post-treatment, can often be effectively maintained with a removable appliance that allows for thorough nocturnal and part-time daytime wear. Clinically, removable retainers offer additional diagnostic benefits; they allow dentists to visually inspect the lingual surfaces during routine exams, assess gingival health without obstruction, and make incremental adjustments to the retention protocol if minor shifting occurs. Ultimately, the decision should be guided by a comprehensive evaluation of your occlusion, periodontal status, manual dexterity for hygiene, and lifestyle factors.
Pros and Cons of Permanent Retainers
Advantages
- Constant Retention: It's always working, providing the best defense against tooth relapse.
- Invisible: Since it's bonded to the back of your teeth, no one will know it's there.
- No Compliance Needed: Ideal for individuals who might forget to wear a removable retainer consistently.
- Durable: Unlike removable retainers, it can't be lost, accidentally thrown away, or warped by heat.
Disadvantages
- Oral Hygiene Challenges: This is the most significant drawback. Flossing is difficult and requires tools like a floss threader or water flosser.
- Plaque and Tartar Buildup: Inadequate cleaning can lead to significant tartar buildup, increasing the risk for cavities and gum disease.
- Dietary Restrictions: You must be cautious with hard, sticky, or crunchy foods that can bend or break the wire.
- Potential for Breakage: The wire can break or the bonding agent can fail, requiring an urgent trip to the orthodontist for repair.
- Tongue Irritation: Some people experience initial discomfort or irritation where their tongue touches the wire.
Beyond these foundational points, the biomechanical and psychological benefits of fixed retainers are substantial. Because the wire is bonded to multiple teeth, it creates a rigid unit that distributes occlusal and functional forces across the entire segment rather than concentrating them on individual teeth. This splinting effect can be particularly advantageous for patients with mild periodontal concerns, as it provides gentle stabilization against pathological mobility. Psychologically, the elimination of retention-related anxiety is a major advantage. Patients with removable appliances often report stress about misplacing them in restaurants, damaging them during travel, or the social embarrassment of being reminded to wear them. Fixed retainers remove this cognitive load, allowing patients to integrate their orthodontic aftercare seamlessly into their daily routines without disruption. However, the disadvantages warrant careful consideration. The oral hygiene challenges are not merely inconvenient; they represent a genuine clinical risk. Plaque accumulation around bonding pads and wire contours can rapidly mineralize into subgingival calculus, creating an environment conducive to gingival inflammation and interproximal caries. Patients must also recognize that dietary modifications are lifelong. Biting directly into whole apples, crusty breads, or hard candies places excessive tensile and shear forces on the composite bonds, significantly increasing the likelihood of debonding. Furthermore, while initial tongue adaptation usually occurs within two to three weeks, a subset of patients with highly sensitive lingual mucosa or specific speech patterns may experience persistent lisping or tactile discomfort, which sometimes necessitates transition to an alternative retention method.
The "Permanence" Paradox: How Long Do They Really Last?
Despite the name, a "permanent" retainer is not guaranteed to last a lifetime. While a well-maintained retainer can last for up to 20 years, the "permanence paradox" lies in its notable failure rate. Research indicates that over a third of bonded retainers may experience failure over the long term.
Factors that influence longevity include:
- Oral Hygiene: Proper cleaning prevents issues that could weaken the bonding.
- Diet and Habits: Avoiding hard foods and not using your teeth as tools prevents damage.
- Biting Forces: A person's individual bite can put stress on the retainer.
- Practitioner Skill: The experience of the orthodontist in placing the retainer is a crucial factor in its survival rate.
Failure typically involves either the wire fracturing or, more commonly, the bonding material detaching from one or more teeth.
Clinical literature reveals fascinating insights into the longevity dynamics of fixed retainers. Studies utilizing Kaplan-Meier survival analysis demonstrate that the highest risk of failure occurs within the first five years of placement, after which the survival curve typically stabilizes if the retainer remains intact. This early vulnerability period is primarily attributed to inadequate initial curing of the adhesive, improper isolation during placement leading to moisture contamination, or premature occlusal contact that places repetitive micro-trauma on the bonds. The adhesive interface itself undergoes continuous stress from thermal expansion and contraction, mastication cycles, and subtle arch form changes. When a partial debond occurs—where one composite pad detaches while others remain secure—the wire effectively becomes a long, unsupported lever. This altered mechanical environment concentrates stress on the remaining bonded teeth, dramatically increasing the likelihood of cascading failure. Regular monitoring is therefore essential. Patients should perform a simple tactile check monthly by gently running their tongue along the wire to feel for any rough edges, gaps, or mobility. Any deviation from the original smooth contour should prompt an immediate clinical evaluation. Advances in adhesive dentistry, including the use of silane coupling agents and hydrophobic composite resins, have improved bond durability, but they cannot overcome the fundamental challenges of the moist, dynamic oral environment. Consequently, viewing a permanent retainer as a long-term but finite device, rather than a truly permanent fixture, aligns expectations with clinical reality and encourages proactive maintenance.
The Cost of a Permanent Retainer
The cost for the initial placement or a full replacement of a permanent retainer generally ranges from $150 to $500 per arch. However, some advanced, custom-designed wires (like CAD/CAM retainers) can cost up to $850 per arch.
Often, the cost of your first set of retainers is included in the overall price of your orthodontic treatment. It's important to remember that repairs often cost just as much as a new placement. Be sure to check with your dental insurance provider to see what, if any, of the cost is covered.
Understanding the financial landscape of orthodontic retention helps prevent unexpected expenses. The initial placement fee typically encompasses the clinical appointment time, materials (wire, etching gel, bonding adhesive, curing equipment), and digital or physical impressions required for fabrication. Geographic location and practice overhead significantly influence pricing; metropolitan areas with higher operational costs generally charge at the upper end of the spectrum. Insurance coverage for retainers varies dramatically. Many dental plans classify orthodontic retainers as part of the comprehensive treatment benefit rather than a standalone prosthetic or preventive service. If your plan includes an orthodontic lifetime maximum (often $1,000 to $3,000), retainer fees are frequently deducted from that pool. Once the maximum is exhausted, out-of-pocket payment becomes necessary. Some insurers cover only the initial set, leaving replacements or repairs entirely to the patient, while others provide annual or periodic allowances for orthodontic appliances. It is highly advisable to request a pre-treatment authorization and a detailed breakdown of benefits from your provider. Additionally, many orthodontic offices offer retention warranty programs or discounted maintenance plans for patients who commit to biannual check-ups. Investing in a robust hygiene kit upfront—including high-quality floss threaders, interdental brushes, and a reliable water flosser—pays long-term dividends by reducing the likelihood of costly complications such as interproximal restorations or periodontal therapy. When evaluating cost, consider the long-term value proposition: a well-maintained fixed retainer can prevent hundreds or thousands of dollars in future alignment correction or restorative dental work caused by untreated relapse or decay.
Caring for Your Permanent Retainer: A Guide to Oral Hygiene
Diligent oral hygiene is non-negotiable with a permanent retainer. Here’s how to keep your teeth and gums healthy:
- Brushing: Use a soft-bristled toothbrush and be sure to angle the bristles to clean thoroughly above and below the wire.
- Flossing: This is the most critical and challenging step. You cannot floss normally. Instead, use one of these tools:
- Floss Threader: A stiff-tipped loop that helps you thread floss under the retainer wire, allowing you to clean between each tooth.
- Water Flosser: A device that shoots a high-pressure stream of water to dislodge food particles and plaque from around the wire and between teeth.
- Interdental Brushes: Tiny brushes designed to clean in small spaces.
- Regular Dental Check-ups: Schedule professional cleanings every six months. A dental hygienist has the tools to remove tartar that you can't get at home.
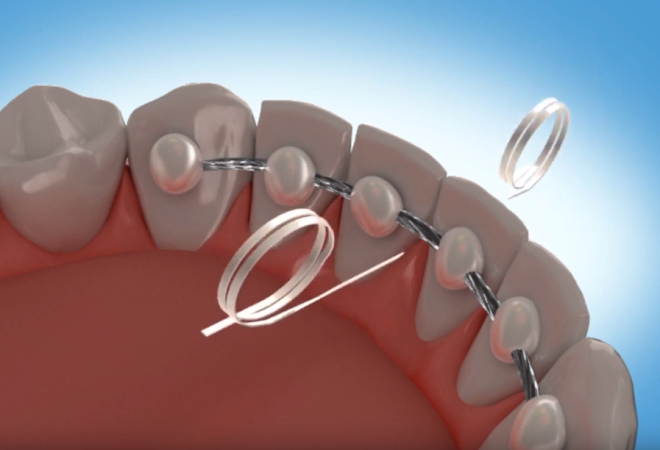 Image source: Premier Orthodontics
Image source: Premier Orthodontics
Mastering hygiene around a bonded retainer requires adapting standard techniques to accommodate the physical barrier. For optimal plaque disruption, modify the Bass brushing technique: place your toothbrush at a 45-degree angle toward the gumline and use gentle, circular vibrations, paying extra attention to the gingival margin beneath the wire. Electric toothbrushes with oscillating-rotating heads are highly effective, but ensure the brush head is compact enough to maneuver around bonding pads without snagging. When flossing, adopt a systematic approach. Use waxed or PTFE floss, which glides more easily through tight contacts and around composite contours. Guide the floss through the threader, position it beneath the wire, and carefully pull it upward to wrap around the mesial and distal surfaces of each tooth in a "C-shape" motion. Gently slide it below the gumline to disrupt subgingival plaque, then lift it out without snapping to avoid traumatizing delicate papillae. Water flossers should be used on a medium pressure setting (approximately 50-70 PSI) to prevent gingival recession while effectively flushing out debris. Aim the tip perpendicular to the tooth surface and trace the wire's length systematically. Interdental brushes are excellent supplemental tools but must be selected carefully; choose the largest size that fits comfortably without forcing it through, as excessive friction can wear down composite bonds over time. Incorporating an antimicrobial mouthwash containing cetylpyridinium chloride or essential oils can help reduce bacterial load in hard-to-reach areas, but it should never replace mechanical cleaning. Initially, mild gingival bleeding and temporary sensitivity are common as inflamed tissue heals. Consistent, gentle hygiene will resolve these symptoms within two to four weeks. If bleeding persists beyond this window or if you notice localized swelling, it may indicate early periodontal involvement requiring professional intervention.
Potential Problems and Long-Term Health Implications
If not properly maintained, a permanent retainer can lead to several issues.
Health Risks
- Cavities and Gum Disease: The difficulty in cleaning makes the area a prime spot for plaque to harden into tartar, leading to tooth decay and gum inflammation (gingivitis), which can progress to more severe periodontitis.
- Bad Breath (Halitosis): The accumulation of bacteria can cause persistent bad breath.
Mechanical Failures
- Shifting Teeth: If a bond fails on even one tooth or the wire breaks, your teeth can start to shift. It's vital to contact your orthodontist immediately if you feel something is loose or broken.
- The "Twist Effect": In rare cases, a bonded retainer can cause unwanted tooth movement even while fully attached. This phenomenon may involve the canines twisting in opposite directions, potentially leading to bone loss or gum recession. Regular orthodontic check-ups can help catch this early.
The clinical management of complications surrounding fixed retainers requires vigilance and prompt intervention. When debonding occurs, the timeline for professional repair is critical. Teeth can begin migrating within days, particularly in younger patients with higher cellular turnover in the periodontal ligament. Waiting weeks or months to address a broken retainer often results in irreversible space loss, occlusal discrepancies, or the need for comprehensive retreatment. Beyond obvious breakage, micro-mobility of composite pads can create plaque-retentive ledges that escape visual detection but are readily apparent on tactile examination or diagnostic imaging. Halitosis in retainer wearers is frequently multifactorial, stemming from volatile sulfur compound production by anaerobic bacteria thriving in the microenvironment between the wire and enamel. Targeted tongue cleaning, chlorhexidine rinses (used short-term to avoid staining), and professional air-polishing can effectively mitigate this. The so-called "twist effect" or paradoxical tooth movement warrants particular attention. Biomechanical studies suggest that rigid splinting of teeth with inherently different root morphologies and centers of resistance can create torsional stresses during functional loading. Over years, these asymmetric forces may cause canines to rotate axially or incisors to intrude slightly, potentially compromising interproximal bone levels. This underscores why routine orthodontic evaluations every 12 to 24 months are recommended even during the retention phase. Radiographic monitoring, periodontal probing, and occlusal analysis allow clinicians to detect subtle shifts before they manifest as visible misalignment. In cases where the retainer actively contributes to periodontal compromise or malposition, conservative debonding and transition to a passive removable appliance is often the safest therapeutic pathway. Patient education remains the cornerstone of prevention: recognizing warning signs, maintaining impeccable hygiene, and honoring scheduled follow-ups dramatically reduce long-term morbidity associated with fixed retention.
The Removal Process: Is It Really Permanent?
A permanent retainer can be removed by a dentist or orthodontist at any time. The process is straightforward and involves:
- Carefully breaking the bonding material.
- Removing the wire.
- Polishing the back of the teeth to remove any remaining adhesive.
It is critical to have a new retention plan in place immediately after removal. Without a retainer, your teeth will begin to shift. This usually means getting fitted for a removable retainer that you will need to wear as directed by your orthodontist.
Professional removal is a controlled, non-invasive procedure typically completed in a single appointment. Clinicians utilize specialized dental instruments, such as high-speed burs with safety tips or ultrasonic scalers, to gently fracture the composite resin without damaging the underlying enamel structure. Once the bonds are compromised, the wire lifts away cleanly. The subsequent polishing phase is critical; residual adhesive not only feels rough to the tongue but also serves as a potent plaque magnet. Dental hygienists employ fine-grit polishing paste and prophylaxis cups to restore the natural enamel surface texture and luster. Patients often report temporary tooth sensitivity or a sensation of "space" immediately following removal, which is entirely normal as the periodontal ligament adjusts to the sudden absence of rigid stabilization. The transition to a removable retainer must be seamless to prevent orthodontic relapse. Clinicians typically take new impressions or digital scans on the day of removal to fabricate a precision-fitted Essix or Hawley appliance. Initial wear protocols usually mandate full-time use (22+ hours daily) for a minimum of three to six months, followed by a gradual transition to nocturnal wear. Attempting to remove a permanent retainer at home using fingernails, floss, or sharp objects is strongly discouraged and potentially dangerous. DIY extraction can fracture enamel, lacerate gingival tissues, introduce bacterial infections, or leave substantial adhesive remnants that complicate future dental care. Furthermore, uncoordinated removal without a concurrent retention strategy guarantees rapid tooth movement, potentially necessitating expensive corrective orthodontics. Open communication with your dental provider ensures that removal is strategically timed with life transitions, occlusal changes, or hygiene challenges, safeguarding your investment in a straight, healthy smile.
References
- Medical News Today. (2025). Permanent retainer: Pros and cons, cost, and removal. https://www.medicalnewstatoday.com/articles/permanent-retainer
- WebMD. (2025). What to Know About Permanent Retainers. https://www.webmd.com/oral-health/what-to-know-about-permanent-retainers
- Invisalign. (n.d.). Permanent Retainers. https://www.invisalign.com/resources/retainers/permanent-retainers
- Allure. (2022). What I Wish I'd Known Before Getting a "Permanent" Retainer. https://www.allure.com/story/permanent-retainer-photos-risks-cost
Frequently Asked Questions
Can I get a permanent retainer on my upper teeth?
Yes, permanent retainers can be bonded to the upper arch, but it is less common than lower placement due to biomechanical and anatomical considerations. The upper anterior teeth typically experience greater occlusal forces during biting and chewing, particularly when the lower incisors contact them. This increased stress concentration elevates the risk of wire fracture or composite debonding. Additionally, the upper arch generally exhibits better post-orthodontic stability compared to the lower arch, which is more susceptible to crowding and mesial drift over time. Many orthodontists prefer prescribing a removable retainer for the upper teeth, allowing patients to maintain superior hygiene and enabling clinicians to monitor periodontal health more effectively. However, fixed retention on the upper anterior segment may be recommended for patients with a history of significant diastema closure, severe rotations, or demonstrated non-compliance with removable appliance wear. Your orthodontist will evaluate your bite dynamics, gingival architecture, and relapse risk factors before determining the optimal configuration.
How do I know if my permanent retainer has broken or debonded?
Early detection of retainer failure is essential to prevent unwanted tooth movement. Clinical signs include feeling a sharp or rough edge with your tongue, noticing that the wire moves or clicks when touched, or observing visible gaps between the composite bonding pads and the tooth surface. You may also detect food impaction in areas that were previously easy to clean, or experience a subtle change in how your teeth meet when biting. Sometimes, debonding is asymptomatic, which is why regular professional examinations are crucial. If you suspect failure, avoid poking the area with sharp objects or attempting to adjust the wire yourself. Contact your orthodontist promptly; they can assess the integrity of the bonds, determine whether localized rebonding or complete replacement is necessary, and provide interim guidance to minimize shifting while awaiting your appointment.
Are permanent retainers safe for people with metal allergies or sensitivities?
The vast majority of permanent retainers are fabricated from medical-grade stainless steel or nickel-titanium alloys, which are highly biocompatible and safe for most patients. However, individuals with confirmed nickel hypersensitivity may experience localized gingival inflammation, burning sensations, or mucosal irritation. In such cases, alternative materials are available, including titanium wires, fiber-reinforced polymer composites, or tooth-colored zirconia-reinforced splints. These hypoallergenic options eliminate metal exposure while maintaining adequate retention properties. Before placement, discuss any known allergies, dermatological sensitivities, or previous adverse reactions to dental materials with your orthodontist. Patch testing or reviewing manufacturer specifications can help confirm material safety. If you develop unexplained gum redness, swelling, or persistent discomfort months after placement, an allergy-related reaction should be considered alongside standard periodontal evaluations.
What happens if I delay getting a broken permanent retainer repaired?
Delaying repair significantly increases the risk of orthodontic relapse. Teeth are dynamic structures suspended in elastic periodontal ligaments that constantly adapt to functional forces. Once the continuous retention provided by the bonded wire is interrupted, even partially, teeth can begin migrating within days to weeks. This movement is often irreversible without active intervention, potentially requiring new braces, clear aligners, or complex restorative adjustments to correct spacing or bite misalignment. Prolonged exposure of the underlying tooth surfaces without bonding protection can also lead to increased susceptibility to caries and gingival inflammation around the remaining composite pads. Furthermore, a broken wire with loose ends can traumatize the tongue, cheeks, or gingival tissues, causing ulceration and infection. Prompt clinical evaluation and timely intervention are the most effective strategies for preserving your orthodontic results and avoiding costly, extensive retreatment.
Can I whiten my teeth while wearing a permanent retainer?
Yes, professional and over-the-counter whitening treatments can be safely used while a permanent retainer is in place, but with important considerations. The retainer itself does not change color, but because it covers specific areas of enamel, those sections will remain the shade they were at the time of placement. If you undergo whitening treatment, the exposed enamel will lighten while the covered portions remain unchanged, potentially creating subtle shade discrepancies once the retainer is eventually removed. To minimize this effect, maintain excellent oral hygiene to prevent extrinsic staining, and consider using whitening toothpaste with mild abrasives that clean without damaging composite bonds. If you desire uniform whitening results, some patients opt for temporary professional bleaching after retainer removal, or coordinate with their orthodontist to plan elective whitening during a phase when a removable appliance is temporarily substituted. Always consult your dentist before initiating any bleaching protocol to ensure your gingival tissues and enamel are healthy enough to tolerate the treatment.
Conclusion
Navigating the decision to get a permanent retainer requires a balanced understanding of its clinical benefits, maintenance demands, and long-term implications. Fixed bonded retainers offer unparalleled convenience and continuous protection against orthodontic relapse, making them an excellent choice for many patients, particularly in the lower anterior segment. However, their "permanence" is a relative term; they are highly durable yet finite appliances that demand diligent oral hygiene, mindful dietary habits, and proactive professional monitoring. The success of a permanent retainer ultimately depends on a collaborative partnership between patient and dental provider. Meticulous cleaning protocols, prompt attention to mechanical failures, and regular retention evaluations are essential to mitigate risks such as periodontal inflammation, interproximal decay, and paradoxical tooth movement. By adhering to evidence-based hygiene practices, honoring scheduled check-ups, and communicating openly with your orthodontist, you can maximize the longevity and effectiveness of your retention system. Whether you ultimately choose a fixed, removable, or hybrid approach, committing to lifelong retention is the definitive investment in preserving the alignment, function, and aesthetics of your smile for decades to come.

About the author
Benjamin Carter, MD, is a board-certified otolaryngologist specializing in head and neck surgery, with an expertise in treating throat cancer. He is an associate professor and the residency program director at a medical school in North Carolina.