Little Bumps on Lips: Causes, Treatments, and When to See a Doctor

Key points
- Appearance: A cluster of tiny, fluid-filled blisters, typically on the border of the lip. These blisters eventually break, ooze, and form a yellow crust or scab.
- Symptoms: Tingling or burning prodrome, pain, tenderness. May be accompanied by fever or swollen lymph nodes on the first outbreak.
- Contagious: Yes, highly contagious through direct contact like kissing or sharing utensils.
- Treatment: Cold sores usually heal on their own in 1-2 weeks. Over-the-counter creams (like docosanol) or prescription antiviral medications (like valacyclovir) can speed up healing, especially if used at the first sign of tingling.
Finding a small bump on your lip can be alarming, but most causes are harmless and easily managed. From a tingling cold sore to painless white spots, understanding the cause is the first step to proper care and peace of mind. The lips are composed of highly specialized tissue, with a thin outer layer (stratum corneum) and an underlying zone of transition that lacks the protective oil glands found on the rest of your face. This unique anatomy makes the vermilion border and surrounding perioral skin particularly susceptible to environmental triggers, infections, inflammatory responses, and minor trauma. When a bump appears, it’s rarely a cause for panic, but recognizing its characteristics helps you avoid unnecessary interventions and choose the most effective treatment pathway.
This guide explores the most common causes of little bumps on lips, how to identify them, what your treatment options are, and when it's time to consult a healthcare professional.
Common Causes of Little Bumps on Lips
Not all lip bumps are the same. Their location, appearance, and symptoms can help you identify the cause. Understanding the underlying pathophysiology and clinical progression of each condition is essential for accurate self-assessment and appropriate care.
Cold Sores (Fever Blisters)
Cold sores are small, painful blisters caused by the highly contagious herpes simplex virus (HSV-1). Before the blisters appear, you may feel a characteristic tingling, itching, or burning sensation on your lip.
- Appearance: A cluster of tiny, fluid-filled blisters, typically on the border of the lip. These blisters eventually break, ooze, and form a yellow crust or scab.
- Symptoms: Tingling or burning prodrome, pain, tenderness. May be accompanied by fever or swollen lymph nodes on the first outbreak.
- Contagious: Yes, highly contagious through direct contact like kissing or sharing utensils.
- Treatment: Cold sores usually heal on their own in 1-2 weeks. Over-the-counter creams (like docosanol) or prescription antiviral medications (like valacyclovir) can speed up healing, especially if used at the first sign of tingling.
A dermatologist explains the causes, symptoms, and treatment of cold sores.](https://www.youtube.com/watch?v=aL3gI68_464 "Dermatologist Explains Cold Sores | Dr. Sam Ellis")
After initial exposure, HSV-1 travels along sensory nerve pathways and establishes latency in the trigeminal ganglion. The virus can reactivate periodically due to specific triggers such as ultraviolet radiation from sun exposure, psychological or physical stress, hormonal fluctuations (like menstruation), immune suppression, or dental procedures. During reactivation, the virus travels back down the nerve to the lip surface, initiating the classic prodromal phase. The viral shedding period typically begins during the tingling stage and continues until the scab has completely fallen off and fresh skin has formed. It’s important to note that asymptomatic viral shedding can also occur, meaning the virus can spread even when no visible lesion is present. For individuals experiencing frequent recurrences (more than six per year), suppressive antiviral therapy may be recommended by a physician to significantly reduce outbreak frequency and transmission risk.
Canker Sores (Aphthous Ulcers)
Unlike cold sores, canker sores are not contagious and appear inside the mouth, such as on the inner lip or cheek. Their exact cause is unknown but can be triggered by stress, minor mouth injuries, or certain foods.
- Appearance: A small, round, or oval ulcer with a white or yellow center and a red, inflamed border.
- Symptoms: Localized pain, especially when eating or talking. No tingling sensation beforehand.
- Contagious: No.
- Treatment: Most heal on their own in 1-2 weeks. To ease discomfort, you can use over-the-counter numbing gels, rinse with warm salt water, and avoid spicy or acidic foods.

Canker sores, medically termed aphthous stomatitis, are broadly categorized into three clinical types: minor, major, and herpetiform. Minor aphthae, the most common variety, are typically smaller than one centimeter in diameter and heal without scarring. Major aphthae are larger, deeper, and more painful, often taking several weeks to resolve and sometimes leaving behind tissue scarring. Herpetiform canker sores present as dozens of pinpoint ulcers that cluster together, mimicking a viral outbreak but lacking an actual viral etiology. While the precise pathogenesis remains multifactorial, research strongly implicates localized immune dysregulation, where T-cells mistakenly attack the oral mucosal epithelium. Common precipitating factors include nutritional deficiencies (particularly vitamin B12, iron, folate, and zinc), mechanical trauma from dental appliances or accidental biting, and chemical irritants like sodium lauryl sulfate (SLS) found in many commercial toothpastes. Certain systemic conditions, such as celiac disease, inflammatory bowel disease, or Behçet's disease, can also manifest with recurrent aphthous ulcers. If you experience unusually large, persistent, or exceptionally frequent canker sores, a clinical workup to rule out underlying nutritional or gastrointestinal issues may be warranted.
Fordyce Spots
Fordyce spots are visible sebaceous (oil) glands. They are a normal anatomical variation and are completely harmless. They are not an infection and are not contagious.
- Appearance: Clusters of tiny (1–3 mm) pale yellow, white, or skin-colored bumps, often on the border of the lips. They may be more noticeable when the skin is stretched.
- Symptoms: None. They are painless and not itchy.
- Contagious: No.
- Treatment: None is needed. Since they are harmless, dermatologists advise against trying to treat them at home. Cosmetic removal options like laser therapy exist but are rarely necessary.

Embryologically, Fordyce spots represent ectopic sebaceous glands that develop outside of hair follicles. They are incredibly prevalent, appearing in an estimated 70% to 80% of the adult population, though they are often more noticeable during puberty and young adulthood due to androgen-driven glandular hypertrophy. Because the lip vermilion lacks terminal hair follicles, these glands have nowhere to release their sebum, resulting in their characteristic pale, raised appearance. They frequently become more prominent during periods of heightened skin tension, such as when stretching the lips wide, or during pregnancy when hormonal shifts further stimulate glandular activity. It is crucial to distinguish Fordyce spots from sexually transmitted infections or inflammatory conditions. Many patients mistakenly squeeze or attempt to extract them, which can cause localized trauma, post-inflammatory hyperpigmentation, or bacterial superinfection. While purely cosmetic interventions such as carbon dioxide laser ablation, pulsed dye laser therapy, or electrodessication are available, the risk of scarring or altered lip texture generally outweighs the aesthetic benefit. Maintaining a consistent lip care routine with gentle, non-comedogenic moisturizers can help the surrounding skin appear uniform, minimizing visual contrast.
Pimples or Acne
The skin around the lips has pores that can become clogged with oil and dead skin cells, leading to a pimple. This is often caused by comedogenic lip balms, makeup, or hormonal fluctuations.
- Appearance: A single red, inflamed bump, sometimes with a white or yellow pus-filled center (a whitehead). Usually forms on the skin bordering the lip, not on the lip tissue itself.
- Symptoms: May be tender or sore, but lacks the specific tingling of a cold sore.
- Contagious: No.
- Treatment: Keep the area clean and apply a warm compress to help it drain naturally. A spot treatment with salicylic acid or benzoyl peroxide can be carefully applied to the skin next to the lip, but avoid the lip itself. Do not pop it.
Perioral acne or isolated comedones develop when the pilosebaceous units surrounding the mouth become occluded. The buildup of sebum, keratin, and Cutibacterium acnes bacteria creates an anaerobic environment conducive to inflammation. Heavy, oil-based lip balms, petroleum-based cosmetics, and frequent use of face masks ("maskne") can exacerbate pore blockage in this delicate area. Additionally, hormonal fluctuations during the menstrual cycle, periods of high cortisol, or discontinuation of certain contraceptives can stimulate excess sebum production. It's important to differentiate true acne from perioral dermatitis, a distinct inflammatory condition characterized by clusters of small red bumps and pustules that often spare a narrow band of skin immediately adjacent to the vermilion border. Perioral dermatitis is frequently triggered by topical corticosteroid use, heavy occlusive skincare products, or fluorinated toothpaste, and requires a completely different treatment approach than standard acne. For isolated pimples, gentle cleansing and targeted, well-formulated topical treatments are effective, but aggressive scrubbing or high-concentration acids should be avoided due to the risk of barrier disruption and chemical burns on the thin lip margin.
Allergic Reactions (Contact Dermatitis)
Small bumps, redness, and swelling on the lips can be an allergic reaction to a substance that touched them. Common triggers include ingredients in lipstick, lip balm, toothpaste, or certain foods.
- Appearance: Redness, swelling, and multiple tiny red bumps or a rash-like texture. The lips may also become dry, scaly, or cracked.
- Symptoms: Itching, burning, or a tingling sensation.
- Contagious: No.
- Treatment: Identify and avoid the trigger. A cold compress can soothe irritation. Over-the-counter antihistamines may help with itching, and a mild hydrocortisone cream can be used on the skin around the lips for inflammation.
Contact dermatitis affecting the lips is categorized into two primary mechanisms: irritant contact dermatitis (ICD) and allergic contact dermatitis (ACD). ICD results from direct chemical damage to the skin barrier by harsh substances, such as alcohol-based sanitizers, strong exfoliants, or repeated exposure to saliva. ACD, on the other hand, involves a delayed-type (Type IV) hypersensitivity reaction mediated by T-cells, occurring 24 to 72 hours after exposure to a specific allergen. The lip mucosa and vermilion border are highly permeable, making them exceptionally vulnerable to allergens. Common culprits include fragrance mixes, cinnamal (found in cinnamon-flavored products), lanolin, propolis (bee glue), essential oils like peppermint or tea tree, and certain sunscreens such as oxybenzone. Chronic exposure can lead to cheilitis, characterized by persistent dryness, fissuring, scaling, and lichenification. Diagnosis often requires a thorough product audit and, in persistent cases, patch testing administered by a dermatologist. Management hinges on strict allergen avoidance, barrier restoration using plain occlusive agents like medical-grade petrolatum, and short-term use of topical anti-inflammatory agents under medical supervision to prevent steroid-induced atrophy.
Mucoceles (Mucous Cysts)
A mucocele is a harmless, fluid-filled swelling that forms when a minor salivary gland duct on the inside of the lip is blocked or injured, often from accidentally biting your lip.
- Appearance: A soft, smooth, round bump on the inside of the lip (usually the lower lip). It can appear clear, bluish, or pinkish.
- Symptoms: Usually painless, but can be bothersome when eating or talking.
- Contagious: No.
- Treatment: Many mucoceles rupture and heal on their own. If one is persistent or large, a dentist or doctor can drain or remove it with a simple procedure.
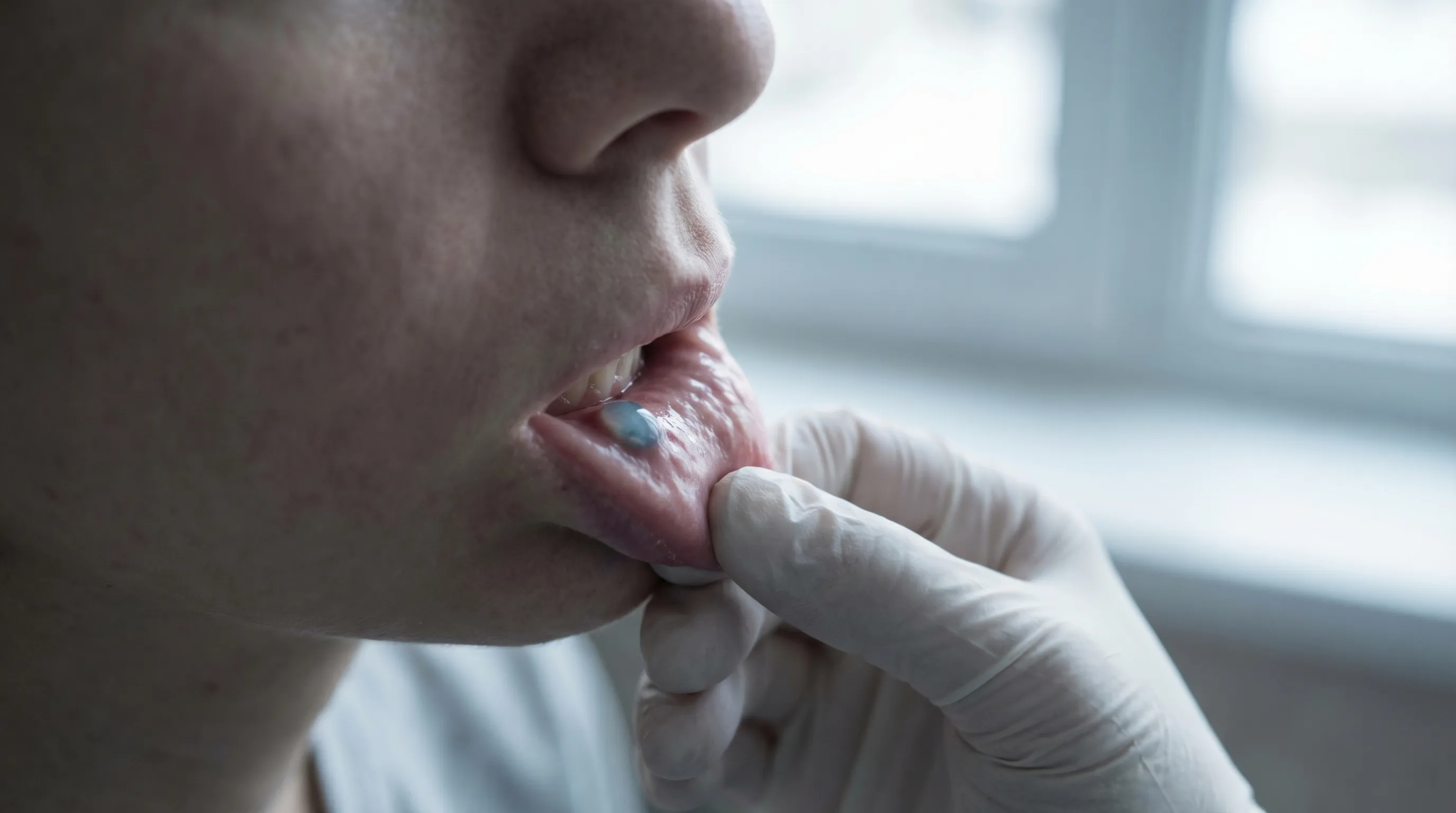
The minor salivary glands are distributed throughout the oral mucosa, with a high concentration in the lower lip. These microscopic glands continuously produce serous and mucinous secretions that lubricate the mouth and aid in digestion. A mucocele typically develops when physical trauma—such as lip biting, impact from sports, or accidental piercing—severs or obstructs the delicate ductal system. This results in two main types: an extravasation mucocele, where saliva leaks into the surrounding connective tissue and becomes encapsulated, and a retention mucocele, which involves duct blockage without rupture. Mucoceles can fluctuate in size, sometimes appearing to vanish only to recur weeks later as saliva continues to accumulate. They are benign and carry no malignant potential. However, if left untreated, they can interfere with speech, mastication, or cause localized discomfort. Professional management typically involves conservative monitoring for small, asymptomatic lesions. For recurrent or large cysts, an oral surgeon or dentist may perform surgical excision of the cyst along with the associated minor salivary gland to prevent recurrence, or employ marsupialization or laser ablation techniques for minimally invasive removal.
Other Possible Causes
While less common, other conditions can cause lip bumps:
- Milia: Tiny white cysts caused by trapped keratin. Harmless and often resolve on their own.
- Oral Warts: Caused by the human papillomavirus (HPV), these can appear as small, cauliflower-like bumps. They are treatable by a doctor.
- Oral Thrush: A yeast infection that can cause white patches or bumps. It requires antifungal medication.
- Oral Cancer: In rare cases, a persistent sore or lump on the lip that doesn't heal could be a sign of oral cancer. This is more common in those with high sun exposure or who use tobacco.
Milia form when dead keratinocytes become trapped beneath the surface of the skin, creating firm, pearl-like papules. They are particularly common in newborns but frequently appear in adults following skin trauma or heavy, occlusive product use around the mouth. Unlike whiteheads, milia lack an opening and cannot be extracted through standard popping, requiring professional extraction if cosmetic removal is desired. Oral warts, typically caused by HPV types 6 and 11, are transmitted through skin-to-skin contact or autoinoculation. They present as exophytic, verrucous growths that can be treated with cryotherapy, topical agents, or surgical excision. Oral thrush (candidiasis) is a fungal overgrowth often seen in infants, denture wearers, asthmatics using inhaled corticosteroids, or immunocompromised individuals. It presents as creamy white lesions that may bleed when scraped and responds well to topical or systemic antifungals. Oral squamous cell carcinoma, though rare in younger populations without risk factors, demands immediate clinical evaluation. Key warning signs include an ulcer or lump that fails to heal after three weeks, induration (hardening), unexplained bleeding, numbness, or leukoplakia/erythroplakia (persistent white or red patches). Risk stratification involves cumulative UV exposure, tobacco and alcohol use, high-risk HPV strains, and chronic immunosuppression.
How to Identify Your Lip Bump
Consider these factors to help determine the cause:
| Feature | Cold Sore | Canker Sore | Fordyce Spots | Pimple | Allergic Reaction | Mucocele |
|---|---|---|---|---|---|---|
| Location | Outer lip border | Inside mouth/lip | Lip border | Skin near lip | On the lips | Inside lip |
| Appearance | Cluster of blisters | Single white ulcer | Tiny yellow/white dots | Single red bump | Red rash, tiny bumps | Single soft bubble |
| Feeling | Tingling, pain | Painful | Painless | Tender | Itchy, burning | Painless |
| Contagious? | Yes | No | No | No | No | No |
Accurate self-identification begins with careful observation of onset, progression, and associated symptoms. Keep a symptom diary to track patterns, such as recurring bumps before menstruation, after trying a new cosmetic product, or following periods of intense stress. High-resolution photographs taken in consistent lighting can be incredibly useful for healthcare providers, especially if the lesion has changed appearance or resolved by the time of your appointment. When performing a self-exam, gently stretch the lip and note whether the bump is mobile, fixed, soft, firm, fluid-filled, or solid. Assess your recent lifestyle factors: Have you been outdoors without sun protection? Started a new medication or supplement? Experienced a recent viral illness or dental work? While this table and observational guide provide a strong foundation for initial assessment, visual overlap between conditions is common. Conditions like herpetic whitlow, granulomatous cheilitis, or early-stage malignancies can mimic benign bumps. Never rely solely on internet diagnostics when a lesion behaves atypically, persists beyond expected healing timelines, or is accompanied by systemic symptoms.
When to See a Doctor
Most lip bumps are not a cause for alarm, but you should see a doctor or dentist if a bump:
- Doesn't heal within two to three weeks.
- Is extremely painful or makes it difficult to eat or drink.
- Grows rapidly or bleeds easily.
- Is a firm, painless lump that persists.
- Is accompanied by other symptoms like high fever or widespread swelling.
"If you have a lip lesion that hasn't healed in about two weeks, especially if you use tobacco or spend a lot of time in the sun, get it checked. Early evaluation is key to address any serious issues." — American Dental Association
Professional evaluation ensures accurate diagnosis and rules out complications or underlying systemic conditions. During a clinical visit, your provider will conduct a thorough extraoral and intraoral examination, palpating the lesion for texture, depth, and fixation to underlying tissues. Diagnostic procedures may include a viral PCR swab for suspected herpes infections, bacterial or fungal cultures if infection is suspected, or a punch biopsy for persistent or suspicious growths. In cases of suspected allergic contact dermatitis, referral to a dermatologist for patch testing can identify specific culprits. Depending on the diagnosis, you may be directed to a primary care physician, dermatologist, oral medicine specialist, otolaryngologist (ENT), or oral surgeon. Delaying evaluation of atypical lesions can complicate treatment and, in rare cases, allow precancerous or malignant conditions to progress. If you experience difficulty breathing, severe facial swelling, or anaphylactic symptoms alongside a lip reaction, seek emergency medical attention immediately, as this may indicate a severe systemic allergic response requiring epinephrine and airway management.
Treatment and Home Care
Treatment depends entirely on the cause.
Medical Treatments
- Cold Sores: Prescription oral or topical antiviral medications.
- Canker Sores: Prescription topical steroids or medicated mouthwashes for severe cases.
- Allergies: Topical steroids or antihistamines.
- Infections: Antifungals for thrush or antibiotics for bacterial infections.
- Mucoceles/Warts: Simple removal procedures by a doctor or dentist.
When prescribed, antiviral therapy for HSV is most effective when initiated during the prodromal phase, typically reducing healing time by one to two days. Medications like acyclovir, valacyclovir, or famciclovir work by inhibiting viral DNA polymerase, halting replication. For aphthous ulcers, clinicians may prescribe amlexanox paste, dexamethasone elixir swishes, or lidocaine-based protective barriers to accelerate epithelialization and manage pain. Allergic or inflammatory conditions often respond to short courses of low-potency topical corticosteroids or calcineurin inhibitors (like tacrolimus ointment), which suppress localized immune activation without the thinning risks associated with prolonged steroid use. Bacterial superinfections secondary to picked-at lesions may require targeted oral or topical antibiotics like mupirocin. It's critical to follow prescribed regimens exactly as directed, even if symptoms improve quickly, to prevent recurrence, resistance, or incomplete resolution.
Home Remedies and Self-Care
- Cold Compress: Use for painful or swollen bumps like cold sores or allergic reactions to reduce inflammation.
- Warm Compress: Apply to a pimple to encourage natural drainage.
- Saltwater Rinse: Swishing with warm salt water can clean and soothe sores inside the mouth, like canker sores.
- Avoid Irritants: Steer clear of spicy, acidic, or salty foods that can irritate a sore.
- Don't Pick or Pop: Squeezing or picking at any lip bump can cause infection, scarring, and delay healing.
Evidence-supported home management focuses on symptom relief, infection prevention, and barrier optimization. A clean, damp cloth applied to a cold sore or allergic swelling for 10–15 minutes several times daily reduces vasodilation and numbs nerve endings. For canker sores, rinsing with a mixture of half a teaspoon of baking soda dissolved in a glass of warm water helps neutralize oral acidity and promote a healing environment. Medical-grade honey (like Manuka) has demonstrated antimicrobial and wound-healing properties in clinical studies and can be applied sparingly to external sores. L-lysine supplementation is widely discussed, though clinical evidence remains mixed; it may help some individuals by competitively inhibiting arginine uptake, which HSV requires for replication. Always avoid unverified internet remedies such as applying undiluted essential oils, alcohol, hydrogen peroxide, or crushed aspirin directly to lesions, as these cause chemical burns, delay epithelial migration, and worsen scarring. Maintain strict hand hygiene, use separate towels, and replace toothbrushes after a cold sore or bacterial infection clears to prevent reinoculation.
Prevention Tips
- Use Lip Balm with SPF: Protect your lips from sun exposure, a common trigger for cold sores and a risk factor for lip cancer.
- Don't Share Personal Items: Avoid sharing lip balm, drinks, or utensils to prevent the spread of viruses like HSV-1.
- Manage Stress: Stress can trigger outbreaks of both cold sores and canker sores.
- Know Your Allergens: If you have sensitive skin, use hypoallergenic or fragrance-free lip products to prevent contact dermatitis.
- Stay Hydrated: Drinking enough water and using a plain moisturizer can prevent chapped lips and associated irritation.
Preventive strategies revolve around barrier maintenance, trigger avoidance, and systemic wellness. Incorporate a broad-spectrum SPF 30+ lip balm into your daily routine, reapplying every two hours during outdoor activities, and choose formulations free of synthetic fragrances and irritating preservatives. When selecting cosmetics and skincare, opt for "non-comedogenic" and "dermatologist-tested" labels, especially if you are prone to perioral acne or milia. Implement a consistent sleep schedule and integrate stress-reduction techniques such as mindfulness meditation, moderate aerobic exercise, or deep breathing protocols, as cortisol directly modulates immune surveillance and mucosal integrity. Maintain optimal nutritional status by consuming a balanced diet rich in B-complex vitamins, zinc, and omega-3 fatty acids, which support epithelial turnover and anti-inflammatory pathways. If you wear dentures or orthodontic appliances, ensure proper fit and clean them daily to prevent mechanical trauma and microbial colonization. For individuals with a history of recurrent HSV outbreaks, sun-blocking lip protection, adequate hydration, and proactive antiviral prophylaxis before known stressors (like travel or surgery) can dramatically reduce flare frequency. Finally, schedule routine dental checkups every six months, as dental professionals perform vital oral cancer screenings and can identify early mucosal changes long before they become symptomatic.
Frequently Asked Questions
Can I safely pop a little bump on my lip if it looks like a pimple?
No, you should never attempt to pop or squeeze a bump on or around your lip. The perioral region lies within the "danger triangle" of the face, an area where blood vessels drain directly into the cavernous sinus near the brain. Popping can force bacteria deeper into tissue, leading to severe cellulitis or systemic infection. Additionally, rupturing a bump prematurely disrupts the natural healing cascade, increases the risk of permanent scarring or post-inflammatory hyperpigmentation, and can transform a minor localized issue into a widespread inflammatory response. If a bump contains visible pus or becomes increasingly painful, a healthcare professional can safely incise and drain it under sterile conditions.
Are little bumps on my lips a sign of a sexually transmitted infection?
While certain STIs like herpes simplex virus (HSV-1 or HSV-2) or syphilis can cause oral lesions, the vast majority of lip bumps are completely unrelated to sexual activity. Cold sores are primarily transmitted through non-sexual close contact during childhood, and Fordyce spots, mucoceles, canker sores, acne, and allergic reactions have zero connection to sexual health. HPV-related oral warts can be transmitted through intimate contact but are also commonly acquired via non-sexual routes. If you are concerned about STI exposure or notice lesions alongside genital symptoms, discuss testing and screening options with a healthcare provider. However, isolated lip bumps should not automatically be assumed to be sexually transmitted.
How long does it usually take for a random lip bump to heal on its own?
Healing timelines vary significantly based on the underlying etiology. A typical pimple or minor mucocele may resolve within 7 to 14 days with proper care. Cold sores generally progress through their full cycle in 10 to 14 days, while canker sores take about 1 to 2 weeks to completely epithelialize. Allergic contact dermatitis can persist for several weeks if the triggering allergen is continuously applied or ingested. Fordyce spots, being a permanent anatomical feature, do not "heal" as they are not pathological. If any bump persists beyond three weeks, changes in texture or color, or recurs in the exact same location, professional evaluation is necessary to rule out chronic conditions or atypical growths.
What ingredients should I avoid in lip products if I’m prone to bumps?
Individuals with reactive lip skin should exercise caution with products containing common sensitizers and irritants. Avoid formulations with artificial fragrances, flavoring agents like cinnamal or menthol, essential oils (tea tree, peppermint, eucalyptus), and preservatives such as formaldehyde-releasers (e.g., DMDM hydantoin) or high concentrations of phenoxyethanol. Sodium lauryl sulfate (SLS), a foaming agent in some toothpastes, can also exacerbate perioral inflammation and aphthous ulcers. Opt for minimalist formulations featuring ceramides, squalane, shea butter, or plain petrolatum, which reinforce the skin barrier without triggering immune responses. Always perform a patch test on a small area of skin or the corner of the mouth for 24 to 48 hours before applying a new product to the entire lip area.
Can stress really cause bumps on my lips, and how can I manage it?
Yes, psychological and physiological stress is a well-documented trigger for multiple lip conditions. Stress elevates cortisol levels, which suppresses localized immune function, allowing latent viruses like HSV to reactivate. It also alters skin barrier recovery, increases sebum production, and heightens neurogenic inflammation, making canker sores, acne, and contact dermatitis flare-ups more likely. Effective stress management involves both lifestyle modification and practical routine adjustments. Prioritize consistent sleep hygiene, engage in regular moderate exercise, and practice proven relaxation techniques such as diaphragmatic breathing, progressive muscle relaxation, or cognitive behavioral therapy (CBT) strategies. During periods of unavoidable high stress, maintaining strict lip hygiene, using prophylactic sun protection, and avoiding known dietary triggers can serve as a protective buffer against stress-induced cutaneous reactions.
Conclusion
Little bumps on the lips are a common occurrence with a wide spectrum of benign and manageable causes. From the highly contagious but self-limiting cold sore to the harmless anatomical presence of Fordyce spots, the vast majority of these lesions pose no serious health threat. Accurate identification hinges on observing location, texture, symptom progression, and potential triggers. Implementing gentle, evidence-based home care while avoiding aggressive picking or unverified chemical treatments significantly supports natural healing and prevents complications. However, the mouth and lip tissue serve as a visible window into overall systemic health, making it essential to recognize warning signs that warrant professional intervention. Persistent, painful, bleeding, or rapidly changing lesions should never be ignored, as timely medical evaluation is crucial for ruling out underlying infections, allergic disorders, or rare but serious conditions. By prioritizing consistent lip protection, mindful product selection, stress management, and routine clinical screenings, you can maintain optimal oral mucosal health and navigate future lip concerns with confidence and clarity.

About the author
Elena Vance, MD, is a double board-certified dermatologist and pediatric dermatologist. She is an assistant professor of dermatology at a leading medical university in California and is renowned for her research in autoimmune skin disorders.