What Do External Hemorrhoids (Piles) Look Like? A Visual Guide

Key points
- Location: They appear as lumps or bumps just outside the anal opening. Because they form in the perianal region, they are often most noticeable when standing or during gentle palpation.
- Size: Their size can vary significantly, from as small as a pea to as large as a grape. In severe or chronic cases, multiple external hemorrhoids may cluster together, creating a more extensive swollen region.
- Texture: They generally feel like soft, fleshy, or rubbery lumps. However, they can become firm or hard if a blood clot forms inside. The transition from soft to firm is a key clinical indicator of disease progression and often signals the onset of thrombosis.
- Color: The color can be similar to your skin tone, or it may appear pinkish or reddish. Erythema (redness) typically indicates active inflammation, while normal skin-colored protrusions may represent chronic, non-inflamed hemorrhoidal tissue or resolved skin tags.
Searching for "pictures of external piles hemorrhoids" is a common first step for many people experiencing discomfort and uncertainty about their anal health. Understanding what external hemorrhoids look like can help you identify potential symptoms, but it is crucial to remember that a professional medical diagnosis is essential for proper treatment and to rule out more serious conditions. In today's digital age, the immediate urge to self-assess via visual references is highly understandable, particularly when dealing with a condition located in a private and often embarrassing area of the body. However, reliance on photographs alone can sometimes lead to unnecessary anxiety or, conversely, delayed medical intervention when symptoms are actually indicative of more serious pathology. Hemorrhoids, whether internal or external, are among the most prevalent anorectal conditions worldwide, affecting an estimated 75% of adults at some point in their lives. Their high incidence is directly tied to modern lifestyle factors, including prolonged sitting, low-fiber diets, and chronic straining. Recognizing the visual hallmarks of this condition is valuable for early detection, but it should always be paired with an awareness of accompanying symptoms and clinical guidance.
This comprehensive guide synthesizes information from medical experts and patient experiences to provide a clear visual and descriptive breakdown of external hemorrhoids, from mild cases to more severe complications. By combining anatomical insights, clinical staging, differential diagnosis, and evidence-based management strategies, this resource aims to empower you with accurate information while emphasizing the irreplaceable value of professional medical evaluation.
What Do External Hemorrhoids Look Like? A Visual Breakdown
External hemorrhoids, also known as piles, are swollen veins that form under the sensitive skin around the anus. Unlike internal hemorrhoids, which are located inside the rectum and are covered by mucosal tissue, external ones develop distal to the dentate line and are covered by stratified squamous epithelium. This anatomical distinction is highly significant because the tissue surrounding external hemorrhoids is richly innervated with somatic pain receptors, meaning external hemorrhoids are typically much more painful when inflamed or thrombosed compared to their internal counterparts. Because they are visible and palpable, patients often notice them first as unusual lumps, swelling, or irritation during routine hygiene practices or bowel movements.
To accurately interpret pictures of external piles hemorrhoids, it helps to understand the underlying vascular anatomy. The anal canal contains two main venous plexuses: the internal hemorrhoidal plexus (drained by the superior rectal vein) and the external hemorrhoidal plexus (drained by the inferior rectal vein). When pressure within these venous channels increases—due to straining, prolonged sitting, pregnancy, or chronic constipation—the vessel walls stretch, become engorged, and may eventually protrude. Over time, the supporting connective tissue weakens, allowing the vascular cushions to descend and become more prominent. This pathophysiological process directly influences how the condition presents visually and symptomatically.
General Appearance and Characteristics
According to medical sources like MedicalNewsToday and Verywell Health, the visual characteristics of a typical external hemorrhoid include:
- Location: They appear as lumps or bumps just outside the anal opening. Because they form in the perianal region, they are often most noticeable when standing or during gentle palpation.
- Size: Their size can vary significantly, from as small as a pea to as large as a grape. In severe or chronic cases, multiple external hemorrhoids may cluster together, creating a more extensive swollen region.
- Texture: They generally feel like soft, fleshy, or rubbery lumps. However, they can become firm or hard if a blood clot forms inside. The transition from soft to firm is a key clinical indicator of disease progression and often signals the onset of thrombosis.
- Color: The color can be similar to your skin tone, or it may appear pinkish or reddish. Erythema (redness) typically indicates active inflammation, while normal skin-colored protrusions may represent chronic, non-inflamed hemorrhoidal tissue or resolved skin tags.
Beyond these baseline characteristics, the visual presentation can shift throughout the day based on venous congestion, bowel habits, and physical activity. For instance, hemorrhoids often appear more engorged after prolonged standing, heavy lifting, or immediately following a bowel movement. Conversely, they may temporarily flatten when lying down due to reduced hydrostatic pressure in the pelvic veins. Patients frequently describe a sensation of fullness, heaviness, or a "foreign object" feeling, even when the visual protrusion is relatively small.
The Visual Spectrum of Severity: Mild vs. Thrombosed Hemorrhoids
The appearance of an external hemorrhoid changes dramatically based on its severity, particularly if it becomes thrombosed. Thrombosis represents a distinct clinical event within the spectrum of hemorrhoidal disease and requires different management considerations. Understanding the visual and symptomatic progression helps patients gauge urgency and select appropriate care pathways.
Pictures of Mild External Hemorrhoids
Mild external hemorrhoids often present as small, soft bumps. They may not cause significant pain but can lead to:
- Itching and irritation around the anus (pruritus ani), often exacerbated by moisture retention, residual stool, or sweat.
- A feeling of discomfort, especially when sitting for long periods or during certain physical activities like cycling or rowing.
- Small amounts of bright red blood on toilet paper after a bowel movement. Unlike internal hemorrhoids, external ones bleed less frequently because they are covered by tougher, less vascularized skin. Bleeding usually occurs if the overlying skin is eroded by wiping friction or minor trauma.
These hemorrhoids can often be managed with home remedies and typically resolve on their own within a few days to a week. The natural healing process involves gradual reduction of venous engorgement, subsidence of inflammation, and eventual contraction of the stretched perianal skin. In some cases, the skin does not fully retract, leaving behind a painless skin tag. You can find more visual examples and clinical descriptions through Healthline's guide on hemorrhoid appearance.
Pictures of Thrombosed External Hemorrhoids
A thrombosed hemorrhoid occurs when a blood clot forms inside the swollen vein, blocking blood flow and causing localized tissue ischemia and inflammation. This is an acute condition that causes a distinct and more severe appearance, often developing suddenly within hours rather than gradually.
- Appearance: A thrombosed hemorrhoid presents as a hard, swollen, and tender lump. The surface often appears shiny and taut due to rapid expansion and increased internal pressure.
- Color: Due to the trapped blood, its color changes dramatically to a dark purple, blue, grey, or black. The hue reflects the oxidation of hemoglobin and the degree of venous congestion. Over several days, as the body begins to resorb the clot, the color gradually shifts toward green or yellow, similar to a resolving bruise.
- Symptoms: The primary symptom is a sudden onset of severe and constant pain, which can be incapacitating. Patients often report difficulty sitting, walking, or sleeping. The pain typically peaks within 48 hours before gradually improving as inflammation subsides.
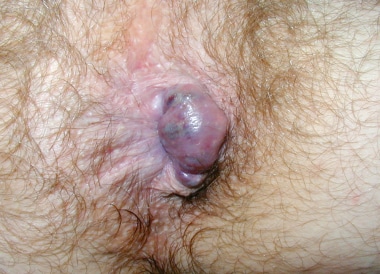 Image Source: Dr. Jonathan Adler via Medscape
Image Source: Dr. Jonathan Adler via Medscape
This condition often requires medical attention for pain relief. While the body will eventually break down and reabsorb the clot over several weeks, the associated discomfort during this period can be substantial. Prompt clinical evaluation can provide rapid relief and reduce the risk of complications such as skin necrosis, secondary infection, or excessive scar tissue formation.
Visual Clues: Distinguishing Hemorrhoids from Other Anal Conditions
Several other anal conditions can be mistaken for hemorrhoids, which is why a professional diagnosis is vital. Misidentification is particularly common because the perianal region is prone to a variety of dermatological, infectious, and structural disorders that share overlapping visual characteristics. Here’s how they visually differ:
| Condition | Key Visual and Symptomatic Differences |
|---|---|
| External Hemorrhoid | Soft, grape-like lump around the anus. Itchy or painful. Becomes hard and dark-colored if thrombosed. Symptoms fluctuate with bowel habits and venous pressure. |
| Anal Fissure | A small, linear tear in the anal lining. Not typically a visible lump. Causes severe, sharp pain during and after bowel movements. Often accompanied by sentinel piles (skin tags at the tear's edge). |
| Anal Abscess | A firm, red, warm, and swollen lump caused by infection. Associated with constant, throbbing pain and may be accompanied by fever and pus drainage. Rapidly progressive and requires urgent drainage. |
| Anal Skin Tag | A painless, soft flap of excess skin. Often a remnant of a previous hemorrhoid. Does not bleed or cause significant discomfort unless irritated by hygiene practices. |
| Anal Warts | Caused by HPV, these growths can be single or multiple and often have a cauliflower-like texture. They may itch or bleed but are distinct from swollen veins. Spread through contact. |
| Anal or Colorectal Cancer | A lump in the anal area could potentially be a tumor. Symptoms like persistent bleeding and change in bowel habits warrant immediate evaluation. For more on differentiation, see the American Cancer Society's guide on anal cancer. |
Understanding these distinctions requires careful attention to symptom chronology, pain quality, systemic signs, and visual morphology. For example, hemorrhoidal pain is typically described as dull, aching, or pressure-like unless thrombosed, whereas fissure pain is characteristically sharp and tearing, often described by patients as "passing ground glass." Abscesses, by contrast, present with systemic inflammatory markers such as fever, malaise, and localized warmth, which are entirely absent in uncomplicated hemorrhoidal disease. Additionally, anal skin tags are purely dermatological remnants and lack the vascular engorgement seen in active piles. Patients should also be aware that conditions like condyloma acuminata (genital warts) require completely different management pathways and are not related to venous congestion. Any lesion that ulcerates, bleeds persistently, grows asymmetrically, or fails to respond to conservative hemorrhoid care warrants prompt specialist evaluation to exclude malignancy or chronic inflammatory conditions.
Visual Indicators and Corresponding Treatment Paths
The appearance of an external hemorrhoid can help indicate the most appropriate course of action. Clinical decision-making in hemorrhoid management is heavily guided by symptom severity, thrombosis status, patient comorbidities, and response to prior interventions. Treatment algorithms typically progress from conservative lifestyle modifications to minimally invasive office procedures, and finally to surgical excision when conservative and office-based therapies fail.
When Home Remedies Are Appropriate (Mild Hemorrhoids)
For soft, skin-colored, or reddish lumps with mild itching or discomfort, home treatment is often effective. According to Harvard Health and other medical sources, these remedies include:
- Sitz Baths: Soaking the anal area in a few inches of warm water for 15 minutes, several times a day. The warmth increases local blood circulation, relaxes the internal anal sphincter, and promotes drainage of edema. Using a dedicated basin that fits over your toilet is highly recommended for consistency.
- OTC Creams: Applying over-the-counter creams containing witch hazel or hydrocortisone to reduce itching and swelling. Hydrocortisone should be used for limited periods (typically no more than 7-10 days) to avoid perianal skin thinning, which can paradoxically increase irritation.
- Cold Compresses: Using a cloth-covered ice pack to soothe the area and reduce inflammation. Limit application to 10-15 minutes at a time to prevent frostbite or reactive vasodilation.
- Dietary Changes: Increasing fiber and water intake to soften stools and prevent straining. Target 25-35 grams of fiber daily from sources like oats, legumes, fruits, and vegetables. Gradually increase intake to avoid bloating. Hydration is equally critical; aim for at least 2-3 liters of water daily to ensure fiber functions optimally. Detailed dietary tips can be found on the NIDDK website.
Beyond these foundational strategies, optimizing bowel habits plays a crucial role in preventing progression. Experts recommend establishing a consistent toilet routine, ideally 15-30 minutes after meals to leverage the gastrocolic reflex. Avoid prolonged sitting on the toilet (keep sessions under 5 minutes), as this posture increases rectal venous pressure significantly. Using a small footstool to elevate the knees can also straighten the anorectal angle, facilitating easier evacuation without excessive straining. Additionally, switch to unscented, alcohol-free, dye-free wipes or rinse with water instead of dry toilet paper to minimize mechanical irritation.
When to See a Doctor (Thrombosed or Persistent Hemorrhoids)
Medical intervention is recommended if you see:
- A hard, severely painful, dark blue or purple lump.
- Bleeding that is heavy or doesn't stop.
- Symptoms that persist for more than a week despite home care.
- Any anal lump accompanied by a fever.
- Recurrent episodes that interfere with daily activities or sleep quality.
- Signs of anemia, such as unusual fatigue, pallor, shortness of breath, or dizziness, particularly if bleeding is frequent.
A doctor may recommend a procedure called an external thrombectomy, where a small incision is made to drain the clot, providing immediate pain relief. This is most effective if done within 48-72 hours of the clot's formation. The procedure is typically performed under local anesthesia in an outpatient setting and takes only a few minutes. After incision, the clot is gently expressed, and the site may be left open to drain or closed with a single absorbable suture, depending on surgeon preference. Post-procedure care involves sitz baths, analgesics, and wound hygiene instructions.
For recurrent or refractory external hemorrhoids, other medical options include rubber band ligation (more commonly used for internal components), sclerotherapy, infrared coagulation, or surgical hemorrhoidectomy. Modern surgical techniques, such as stapled hemorrhoidopexy or Doppler-guided hemorrhoidal artery ligation, aim to reduce recovery time and postoperative pain while effectively addressing prolapsing tissue. Detailed clinical guidelines can be found via the Mayo Clinic's hemorrhoid diagnosis page.
Frequently Asked Questions About External Hemorrhoids
Based on common user questions and search data, here are answers to other related concerns.
Can external hemorrhoids cause fever?
No, hemorrhoids themselves do not cause a fever. A fever accompanied by anal pain and swelling is a red flag for a complication, such as a perianal abscess (a pocket of pus), which requires urgent medical care. Fever indicates a systemic immune response to bacterial infection, which does not occur in uncomplicated venous swelling. If you develop a temperature above 100.4°F (38°C) alongside perianal symptoms, seek prompt medical attention, as untreated abscesses can lead to fistula formation or systemic sepsis.
Can hemorrhoids cause headaches?
Hemorrhoids do not directly cause headaches. However, in rare cases of chronic or severe bleeding, significant blood loss can lead to iron-deficiency anemia. One of the symptoms of anemia is headaches, along with fatigue, pallor, shortness of breath, tachycardia, and reduced exercise tolerance. If you experience recurrent bright red bleeding with bowel movements and subsequently develop unexplained headaches or profound fatigue, a complete blood count (CBC) and iron panel are warranted to assess for occult blood loss.
What about hemorrhoids in toddlers?
While less common, toddlers can get hemorrhoids, often due to constipation and straining. Treatment focuses on gentle, at-home care like ensuring adequate fiber and fluid intake and giving warm sitz baths. Always consult a pediatrician for diagnosis and to rule out other issues such as anal fissures, rectal prolapse, or rare congenital vascular anomalies. Pediatric management emphasizes dietary optimization, stool softeners approved for age, and positive toilet training practices to prevent withholding behaviors.
Are external hemorrhoids more common during pregnancy?
Yes, pregnancy significantly increases the risk of developing both internal and external hemorrhoids. The growing uterus exerts direct pressure on the pelvic veins and the inferior vena cava, impeding venous return from the lower body. Additionally, elevated progesterone levels cause smooth muscle relaxation in venous walls, making them more susceptible to dilation. Straining during labor further exacerbates this risk. Postpartum hemorrhoids are equally common but often improve gradually with conservative care, pelvic floor rehabilitation, and time. Pregnant patients should consult their obstetric provider before using any medicated creams.
How can I prevent external hemorrhoids from recurring?
Prevention hinges on reducing intra-abdominal pressure and maintaining optimal venous return. Key strategies include maintaining a high-fiber diet, staying consistently hydrated, exercising regularly (particularly cardiovascular activities like walking or swimming that promote bowel motility), avoiding heavy lifting with breath-holding (use the exhale-on-effort technique), responding promptly to bowel urges, and limiting prolonged sedentary periods. Incorporating daily core and pelvic floor strengthening can also improve anorectal support mechanics.
Can I exercise if I have symptomatic external hemorrhoids?
Yes, but with modifications. Low-impact activities like walking, swimming, and gentle cycling are generally well-tolerated and can improve circulation and bowel regularity. Avoid heavy weightlifting, deep squats, or high-impact exercises that spike intra-abdominal pressure until symptoms resolve. If an activity causes increased pain or swelling, scale back intensity or modify the movement. Listen to your body and prioritize recovery during acute flare-ups.
The Importance of a Professional Diagnosis
While this guide provides detailed visual descriptions, it is not a substitute for professional medical advice. Self-diagnosing based on pictures can be misleading and risky, as serious conditions like anal cancer, inflammatory bowel disease (Crohn's), sexually transmitted infections, and complex fistulas can mimic the symptoms of hemorrhoids. The human eye, even trained through photographs, cannot assess tissue elasticity, vascular integrity, internal prolapse, or microscopic pathology. Furthermore, visual assessment alone cannot determine the degree of sphincter dysfunction, rule out coexisting internal disease, or evaluate for systemic contributing factors like portal hypertension or coagulopathy.
If you are experiencing rectal bleeding, severe pain, or have a lump that concerns you, schedule an appointment with a healthcare provider. They can perform a physical examination to give you an accurate diagnosis and ensure you receive the safest and most effective treatment plan. A comprehensive evaluation typically begins with a thorough medical history and visual inspection of the perianal region. This is usually followed by a digital rectal examination (DRE) to assess sphincter tone, detect masses, and evaluate tenderness. Depending on findings, your provider may recommend anoscopy or proctoscopy for direct visualization of the distal rectum and anal canal. For patients with red-flag symptoms—such as unexplained weight loss, family history of colorectal cancer, age over 45-50, iron-deficiency anemia, or altered bowel habits—a full colonoscopy is strongly advised to evaluate the entire colon and exclude proximal pathology.
Conclusion
Navigating perianal symptoms can be daunting, but understanding what external hemorrhoids look like is a valuable first step toward effective management. From soft, skin-colored bumps that cause mild itching to dark, firm lumps signaling acute thrombosis, the visual spectrum of external hemorrhoids reflects underlying vascular changes that are often tied to lifestyle, diet, and bowel habits. While home care strategies like sitz baths, dietary fiber optimization, and OTC topical agents effectively resolve many mild cases, severe pain, rapid onset of hard dark lumps, or persistent bleeding warrant prompt medical evaluation. Accurate differentiation from conditions like anal fissures, abscesses, warts, or malignancy requires clinical expertise, as overlapping symptoms can easily lead to misdiagnosis. Prioritizing preventive habits, adopting healthy toilet practices, and seeking professional guidance when symptoms escalate ensures not only faster relief but also long-term anorectal health. Remember that photographs provide general reference, not clinical certainty—consulting a healthcare provider remains the safest, most reliable pathway to personalized care and lasting comfort.

About the author
Fatima Al-Jamil, MD, MPH, is board-certified in gastroenterology and hepatology. She is an Assistant Professor of Medicine at a university in Michigan, with a clinical focus on inflammatory bowel disease (IBD) and motility disorders.