Decoding Alkaline Phosphatase Levels When Are They Dangerous?

Key points
- The liver (specifically in the cells lining the bile ducts, known as cholangiocytes, where it plays a crucial role in transporting substances across cell membranes and facilitating bile secretion)
- Bones (primarily produced by osteoblasts during the bone remodeling and mineralization process, helping to deposit calcium and phosphate into the bone matrix)
- The intestines (involved in nutrient absorption, lipid metabolism, and maintaining gut barrier integrity, though intestinal ALP contributes less to serum levels in most adults)
- The kidneys (concentrated in the proximal tubules, aiding in reabsorption and transport processes, though renal ALP rarely contributes significantly to blood tests unless severe kidney pathology is present)
- The placenta during pregnancy (produced by syncytiotrophoblast cells to support fetal-maternal nutrient exchange and regulate vascular function in the developing placenta)
If you've received a blood test result showing an abnormal alkaline phosphatase (ALP) level, it's natural to feel concerned and wonder what it means. The question "what level of alkaline phosphatase is dangerous?" is common, but the answer is more complex than a single number. An ALP result is a clue, not a diagnosis, and its significance depends heavily on your unique health profile.
This comprehensive guide will help you understand your ALP test results, breaking down what the numbers mean, why context is critical, and when you should be concerned. We will explore the physiological roles of this vital enzyme, how laboratory reference ranges are established, the clinical thresholds that trigger medical intervention, and the step-by-step diagnostic pathways your healthcare team may follow. Whether your levels are slightly elevated, dramatically high, or unexpectedly low, understanding the underlying mechanisms and next steps will empower you to have productive conversations with your medical providers.
What is Alkaline Phosphatase (ALP)?
Alkaline phosphatase (ALP) is an enzyme found in various tissues throughout your body. Enzymes are proteins that trigger essential chemical reactions. While researchers are still exploring its full range of functions, ALP is known to play a role in bone formation, nutrient transport, and fat digestion. Biochemically, ALP belongs to the hydrolase class of enzymes and functions optimally in an alkaline (basic) environment, which is how it earned its name. It requires zinc and magnesium as essential cofactors to maintain its structural integrity and catalytic activity. When cellular membranes in tissues like the liver or bone are disrupted or damaged, ALP leaks into the bloodstream, where it can be detected and quantified through standard venous blood draws.
High concentrations of ALP are found in:
- The liver (specifically in the cells lining the bile ducts, known as cholangiocytes, where it plays a crucial role in transporting substances across cell membranes and facilitating bile secretion)
- Bones (primarily produced by osteoblasts during the bone remodeling and mineralization process, helping to deposit calcium and phosphate into the bone matrix)
- The intestines (involved in nutrient absorption, lipid metabolism, and maintaining gut barrier integrity, though intestinal ALP contributes less to serum levels in most adults)
- The kidneys (concentrated in the proximal tubules, aiding in reabsorption and transport processes, though renal ALP rarely contributes significantly to blood tests unless severe kidney pathology is present)
- The placenta during pregnancy (produced by syncytiotrophoblast cells to support fetal-maternal nutrient exchange and regulate vascular function in the developing placenta)
Because it's present in many areas, an abnormal ALP level tells your doctor that further investigation is needed to pinpoint the source of the issue. Modern laboratory medicine often pairs the standard ALP test with additional hepatic and metabolic panels to narrow down whether the elevation stems from hepatobiliary dysfunction, accelerated bone turnover, or systemic conditions affecting multiple organ systems. Understanding the specific isoenzyme responsible for the elevation is a cornerstone of accurate clinical diagnosis and appropriate therapeutic intervention.
Understanding Normal Alkaline Phosphatase Ranges
One of the most confusing aspects of ALP levels is that there is no universal "normal" range. The reference range often varies between laboratories. This variability occurs because different laboratories use distinct analytical platforms, reagent manufacturers, and calibration standards. Furthermore, reference ranges are typically established by testing large cohorts of healthy individuals and determining the 2.5th to 97.5th percentiles of results, meaning 5% of perfectly healthy people will naturally fall outside these parameters.
Generally, a typical ALP range for adults is considered to be between 44 and 147 international units per liter (IU/L). Some labs may use a range of 30 to 130 IU/L. Your lab report will always specify its own reference range for comparison.
However, a "normal" level for you depends on several key factors.
Why 'Normal' Isn't Universal: Context is Everything
Interpreting ALP results requires clinicians to look beyond the printed numbers on a lab slip. Biological sex, recent dietary intake, circadian rhythms, and underlying chronic conditions all exert measurable influences on baseline ALP production and clearance. For instance, mild elevations are frequently observed in the late evening, and heavy meals—particularly those rich in fats or carbohydrates—can transiently spike intestinal ALP isoforms. Consequently, many clinicians prefer fasting blood draws when establishing a true baseline or monitoring progressive trends over time.
Age-Related Differences: Children and Adolescents
Children and teenagers who are still growing have naturally higher ALP levels than adults. This is completely normal and expected, as the enzyme is crucial for active bone development. Levels can be three to four times higher than the adult normal range without indicating a problem. During periods of rapid skeletal growth, such as infancy and puberty, osteoblast activity surges to lay down new bone matrix, directly correlating with higher circulating ALP. As skeletal maturity is reached and epiphyseal growth plates close, adult reference ranges become applicable.
Here are typical reference ranges by age, though they can vary:
| Age | Reference Range (U/L) |
|---|---|
| 1 month - 3 years | 90 - 180 |
| 3 - 10 years | 130 - 260 |
| 10 - 14 years | 130 - 340 |
| 14 - 18 years | 30 - 180 |
| Source: Gloucestershire Hospitals NHS Foundation Trust |
ALP Levels During Pregnancy
During pregnancy, especially in the third trimester, the placenta produces large amounts of ALP, causing blood levels to rise significantly—sometimes up to three times the normal adult limit. This is a normal part of a healthy pregnancy, though your doctor will monitor these levels. The placental isoform (often called Regan or PLAP isoenzyme) is genetically distinct from liver and bone variants. Postpartum, levels typically normalize within three to six weeks as placental clearance occurs and maternal physiology readjusts to the pre-conception state.
Variations Across Ethnic Groups
Recent research suggests that what is considered a "normal" ALP level can also vary by race and ethnicity. One study found that Hispanic individuals tend to have the highest normal ALP levels, followed by African Americans, whites, and then Asian Americans, who tend to have the lowest. This highlights the importance of interpreting lab results with population-specific data in mind. Genetic polymorphisms affecting enzyme expression, dietary patterns, baseline bone density, and regional disease prevalence all contribute to these demographic variations. Clinicians increasingly rely on ethnicity-adjusted reference intervals to prevent overdiagnosis in naturally higher-producing populations or underdiagnosis in lower-producing groups.
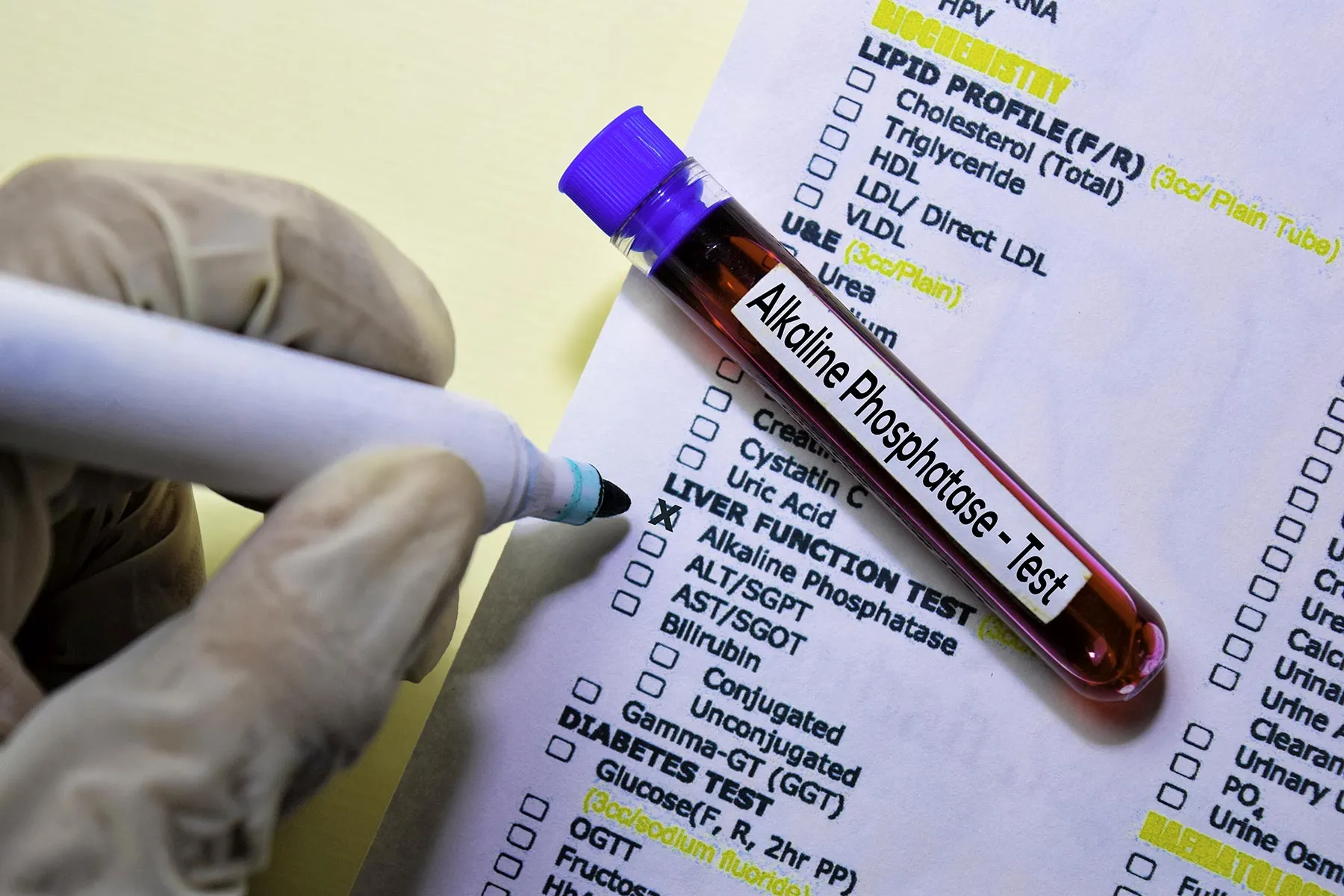 Image Source: WebMD - The liver and bones are the primary sources of ALP in the blood.
Image Source: WebMD - The liver and bones are the primary sources of ALP in the blood.
When Are High Alkaline Phosphatase Levels Dangerous?
While a single number can't define "danger," healthcare providers generally categorize elevated ALP levels by severity to guide their next steps. It's also important to consider the rate of change; a level that is rising rapidly over time is often more concerning than one that is stable, even if slightly elevated. In clinical practice, isolated mild elevations discovered incidentally are frequently monitored with repeat testing rather than triggering immediate invasive workups. Conversely, marked elevations accompanied by symptoms typically prompt urgent diagnostic imaging and specialist consultation.
Understanding the clinical trajectory of ALP is essential. Acute spikes often correlate with sudden biliary obstruction, medication-induced liver injury, or acute bone trauma. Chronic, persistent elevations usually point toward progressive conditions like primary biliary cholangitis, osteomalacia, or metastatic bone disease. Your healthcare provider will also evaluate the ratio of ALP to other liver enzymes (ALT, AST, GGT) to determine whether the hepatobiliary system or the skeletal system is driving the elevation.
- Mildly Elevated ALP (Slightly above 147 IU/L): A small increase might not be a cause for immediate alarm. It could be temporary or related to factors like a healing bone fracture or even eating a fatty meal before the test (especially for blood types O and B). Your doctor will likely recommend monitoring. Additional lifestyle factors such as recent intense weightlifting, smoking, or mild dehydration can also contribute to transient increases. In asymptomatic patients with stable mild elevations, clinicians often employ a "watchful waiting" approach, repeating the panel in 4 to 8 weeks to assess for natural resolution or progressive drift.
- Moderately Elevated ALP (~150 - 300 IU/L): This level warrants further investigation to determine the underlying cause, as it could signal a developing liver or bone condition. At this threshold, physicians typically order targeted follow-up testing, including GGT, comprehensive metabolic panels, lipid profiles, and vitamin D levels. If the elevation persists beyond 3 months or correlates with emerging clinical symptoms like pruritus (itching), right upper quadrant discomfort, or unexplained joint aches, referral to a gastroenterologist or endocrinologist may be initiated.
- Significantly High ALP (> 500 IU/L): Levels in this range are considered serious and require prompt medical evaluation to identify the source. Such elevations rarely occur without a clear pathological driver. Common culprits at this stage include obstructive biliary disease, infiltrative liver disorders, Paget's disease with active bone turnover, or metastatic malignancy. Patients are usually scheduled for cross-sectional imaging (ultrasound or CT), isoenzyme fractionation, and comprehensive bone density assessments within a short clinical window.
- Critically High ALP (> 1000 IU/L): This is often considered a medical emergency. Extremely high levels are typically associated with severe conditions like a major bile duct obstruction, widespread cancer in the liver or bones, Paget's disease of the bone, or sepsis. When levels breach this threshold, rapid clinical deterioration is possible, and immediate intervention—ranging from endoscopic retrograde cholangiopancreatography (ERCP) for biliary clearance to intravenous bisphosphonates for hypercalcemia and bone pain—is frequently required to prevent irreversible organ damage or life-threatening complications.
Pinpointing the Problem: Why the Source of High ALP Matters
Because ALP comes from different parts of the body, the most critical step after seeing a high result is determining its origin. A high ALP level from the liver carries different implications than one from the bones. Misattributing the source can lead to unnecessary testing, delayed diagnoses, and inappropriate treatments. Therefore, clinical algorithms prioritize source differentiation early in the diagnostic pathway.
Your doctor may order follow-up tests to do this:
- Gamma-Glutamyl Transferase (GGT) Test: GGT is another liver enzyme. If both ALP and GGT are high, the problem is almost certainly in the liver or bile ducts. If ALP is high but GGT is normal, the source is likely bone-related. GGT is highly sensitive to biliary epithelial damage and alcohol metabolism, making it an excellent confirmatory marker for hepatobiliary disease.
- ALP Isoenzyme Test: This test specifically separates the different types of ALP to identify whether they are coming from the liver, bone, or another source. Electrophoretic techniques or heat inactivation assays distinguish the thermally stable placental isoform from the more heat-labile liver and bone fractions, providing definitive source attribution without invasive procedures.
Beyond these primary tests, clinicians frequently incorporate additional diagnostic modalities:
- Comprehensive Hepatic Panel: Measuring bilirubin (total and direct), albumin, prothrombin time/INR, ALT, and AST to assess synthetic liver function and hepatocellular integrity.
- Calcium and Phosphate Metabolism Tests: Including intact parathyroid hormone (PTH), 25-hydroxyvitamin D, and serum calcium to evaluate bone mineralization dynamics.
- Imaging Studies: Abdominal ultrasound serves as a first-line, non-invasive visualization of liver architecture, bile ducts, and gallbladder. If biliary pathology is suspected but unclear, magnetic resonance cholangiopancreatography (MRCP) offers detailed mapping. For bone-sourced elevations, radionuclide bone scintigraphy (bone scan) or targeted X-rays/DEXA scans reveal areas of abnormal remodeling or microfractures.
Liver-Related Causes of High ALP
When the liver is the source, high ALP often points to conditions that block bile flow (cholestasis) or cause liver cell damage. The hepatobiliary system relies on unobstructed bile ducts to transport digestive enzymes, waste products, and conjugated bilirubin into the intestines. When this flow is impeded, pressure builds within the microscopic canaliculi and larger ductal structures, upregulating ALP synthesis and release into circulation.
- Bile Duct Obstruction: Gallstones, tumors, or scarring can block the bile ducts, causing ALP to leak into the bloodstream. This is one of the most common causes of very high ALP levels. Symptoms often include colicky abdominal pain, jaundice, clay-colored stools, and intense pruritus due to bile salt deposition in the skin.
- Liver Diseases: Conditions like cirrhosis (scarring), hepatitis (inflammation), and fatty liver disease can all raise ALP. Non-alcoholic fatty liver disease (NAFLD) and its progressive form, non-alcoholic steatohepatitis (NASH), are increasingly prevalent due to metabolic syndrome, insulin resistance, and obesity. Chronic viral hepatitis (B or C) induces persistent hepatocellular inflammation, gradually elevating ALP alongside transaminases.
- Cancers: Liver cancer or cancer that has spread (metastasized) to the liver can cause elevated levels. Primary hepatocellular carcinoma or cholangiocarcinoma directly disrupt hepatic architecture. Metastatic deposits from colorectal, pancreatic, breast, or lung primaries often infiltrate portal tracts, triggering localized ALP surges before other liver function tests become abnormal.
- Medications and Supplements: A wide range of drugs can stress the liver, including high doses of acetaminophen (Tylenol), statins, some antibiotics, and anti-seizure medications. Certain supplements, like kava and black cohosh, have also been linked to liver injury. Drug-induced liver injury (DILI) is a leading cause of acute ALP elevation, as many pharmaceuticals are metabolized via cytochrome P450 pathways and excreted through biliary routes, placing direct chemical stress on cholangiocytes.
Bone-Related Causes of High ALP
High bone-sourced ALP is linked to increased bone cell activity. Bone is a dynamic tissue constantly undergoing remodeling through the coupled actions of osteoclasts (bone resorption) and osteoblasts (bone formation). Any condition that accelerates this turnover cycle will elevate osteoblast-derived ALP. Clinicians differentiate bone-driven elevations by correlating ALP with calcium, phosphate, and vitamin D profiles, alongside imaging that highlights structural changes.
- Paget's Disease of the Bone: A condition causing abnormal bone breakdown and regrowth, leading to weak, enlarged bones and very high ALP levels. Often asymptomatic initially, it commonly affects the pelvis, spine, skull, and long bones. Over decades, disorganized bone matrix formation increases fracture risk, nerve compression, and secondary osteoarthritis. Bisphosphonates remain the cornerstone of therapy to suppress excessive turnover.
- Bone Metastases: Cancers that have spread to the bone, such as from prostate, breast, or lung cancer. Osteoblastic metastases (common in prostate cancer) stimulate excessive bone formation, directly spiking ALP. Osteolytic lesions (frequent in lung and breast cancers) trigger reactive bone repair that similarly elevates enzyme release. Bone scans and PET imaging are critical for staging and guiding targeted radiation or systemic therapies.
- Vitamin D Deficiency: Severe deficiency can lead to bone-softening conditions like osteomalacia, which increases ALP. Without adequate vitamin D, intestinal calcium absorption plummets, prompting compensatory secondary hyperparathyroidism and accelerated bone resorption. Chronic deficiency also impairs proper mineralization of newly formed osteoid, leaving uncalcified matrix that signals osteoblasts to work harder, further elevating ALP.
- Hyperparathyroidism: An overactive parathyroid gland can pull calcium from the bones, increasing bone turnover and ALP levels. Primary hyperparathyroidism, often caused by benign parathyroid adenomas, chronically elevates PTH, disrupting calcium homeostasis. Over time, this leads to cortical bone thinning, kidney stones, neuromuscular irritability, and persistent ALP elevation that typically normalizes after parathyroidectomy or pharmacologic management.
- Healing Fractures: The process of repairing a broken bone naturally increases bone cell activity and ALP. During the reparative phase, soft callus transitions to hard callus through robust osteoblastic activity. ALP peaks 2 to 6 weeks post-fracture and gradually declines as remodeling completes. Clinicians use this predictable timeline to monitor fracture healing progression and identify delayed unions or non-unions when levels plateau abnormally.
What About Dangerously Low Alkaline Phosphatase?
Though less common, abnormally low ALP levels can also be a sign of a health problem. A level below 20-30 IU/L may be considered dangerously low. While elevated ALP receives most clinical attention, profoundly reduced levels often indicate systemic enzymatic deficiency, severe nutritional deprivation, or rare genetic disorders affecting cellular metabolism and tissue integrity. Unlike high levels, low ALP rarely stems from acute organ failure but rather reflects chronic depletion or congenital enzyme dysfunction.
Causes of low ALP include:
- Hypophosphatasia: A rare genetic disorder that affects bone and tooth development. Caused by mutations in the ALPL gene encoding tissue-nonspecific ALP, this condition leads to poor bone mineralization, early loss of primary teeth, recurrent fractures, and in severe perinatal forms, life-threatening respiratory compromise due to a hypomineralized rib cage. Enzyme replacement therapy with asfotase alfa has revolutionized management for affected infants and children.
- Malnutrition: Deficiencies in zinc, magnesium, or protein can lower ALP. Since zinc is an essential catalytic cofactor for ALP structure and function, prolonged zinc deficiency—common in malabsorption syndromes, chronic alcoholism, or vegan diets lacking fortified foods—directly impairs enzyme synthesis. Severe protein-calorie malnutrition also suppresses hepatic and osteoblastic production capacity.
- Hypothyroidism: An underactive thyroid gland slows overall metabolic rate, reducing cellular turnover and enzymatic synthesis across multiple tissues. Low thyroid hormone levels decrease osteoblastic activity and hepatic metabolic output, resulting in consistently low-normal or frankly reduced ALP readings that typically normalize with levothyroxine replacement and achievement of euthyroid status.
- Wilson's Disease: A rare genetic disorder causing copper to build up in the body. Excess copper accumulates in the liver, brain, and corneas, directly inhibiting various metalloenzymes, including ALP. Paradoxically, while most liver diseases elevate ALP, fulminant Wilsonian hepatitis often presents with disproportionately low ALP relative to bilirubin and transaminases, serving as a crucial diagnostic clue.
- Pernicious Anemia: A deficiency in vitamin B12. Autoimmune destruction of gastric parietal cells impairs intrinsic factor production, preventing B12 absorption. Chronic B12 deficiency disrupts DNA synthesis and cellular maturation, reducing the production and release of various enzymes, including ALP. Neurological symptoms, macrocytic anemia, and gastrointestinal disturbances often precede noticeable ALP declines.
Next Steps and When to See a Doctor
An abnormal ALP level is a signal to consult your healthcare provider. It is not a diagnosis on its own. Your doctor will interpret the result in the context of your overall health, symptoms, and other lab tests. Navigating laboratory abnormalities can feel overwhelming, but adopting a structured approach ensures accurate diagnosis and timely intervention. Patients should compile a complete medication and supplement list, note any recent illnesses or dietary changes, and document symptom onset before their appointment.
Be sure to seek medical attention if your abnormal ALP level is accompanied by symptoms like:
- Yellowing of the skin or eyes (jaundice)
- Abdominal pain, especially on the upper right side
- Nausea or vomiting
- Dark-colored urine or light-colored stools
- Persistent fatigue or weakness
- Bone or joint pain
- Unexplained weight loss
Your doctor will determine the appropriate next steps, which may include repeating the blood test, conducting further liver or bone enzyme tests, or ordering imaging studies like an ultrasound, CT scan, or MRI to get a clearer picture of your health. In many cases, a multidisciplinary approach yields the best outcomes. Hepatologists manage complex biliary and parenchymal disorders, while rheumatologists, endocrinologists, or orthopedic specialists address bone metabolism and structural diseases. Genetic counseling may be recommended for suspected hereditary conditions like hypophosphatasia or familial benign hyperphosphatasemia.
Beyond diagnostic pathways, proactive lifestyle management plays a vital role in optimizing ALP levels and supporting overall organ health. Patients with mild, non-urgent elevations can benefit from adopting a Mediterranean-style diet rich in antioxidants, lean proteins, and anti-inflammatory fats, which supports hepatic detoxification and bone mineral density. Maintaining adequate hydration, limiting alcohol consumption, and avoiding unregulated herbal supplements reduce the toxic burden on the liver. For bone-related elevations, weight-bearing exercise, fall prevention strategies, and ensuring optimal vitamin D and calcium intake help stabilize bone turnover. Regular follow-up testing every 3 to 6 months allows clinicians to track trends, assess treatment efficacy, and adjust therapeutic strategies before complications arise. Open communication with your care team, coupled with adherence to prescribed monitoring schedules, remains the most reliable pathway to resolving ALP abnormalities and preserving long-term health.
Frequently Asked Questions
Can alkaline phosphatase levels fluctuate from day to day?
Yes, ALP levels can exhibit natural biological variation based on circadian rhythms, recent meals, hydration status, physical activity, and minor transient infections. Levels typically peak in the late afternoon and may rise temporarily after consuming high-fat meals due to increased intestinal isoform secretion. For this reason, clinicians prefer fasting morning blood draws when establishing baselines or tracking progressive changes. Minor fluctuations of 5-10% between consecutive tests are often clinically insignificant and reflect normal physiological variability rather than disease progression.
Should I fast before getting an ALP blood test?
While fasting is not strictly required for a standalone ALP measurement, many physicians recommend a 10-12 hour fast before comprehensive metabolic panels or hepatic function tests that include ALP. Eating, particularly meals high in lipids or carbohydrates, can transiently elevate intestinal ALP isoforms, potentially skewing results and prompting unnecessary follow-up testing. Fasting also standardizes the testing environment, allowing for more accurate comparisons with reference ranges and previous lab values. Always follow your laboratory's specific preparation instructions.
How long does it take for ALP levels to normalize after treating the underlying cause?
The timeline depends entirely on the root etiology and the severity of tissue damage. In acute conditions like gallstone obstruction successfully relieved via ERCP, ALP typically begins declining within days and may normalize within 2 to 4 weeks. For chronic conditions like primary biliary cholangitis, vitamin D deficiency-induced osteomalacia, or Paget's disease, normalization can take several months to over a year of consistent targeted therapy. Bone remodeling is inherently slower than hepatocellular turnover, meaning skeletal-related elevations generally persist longer on follow-up labs even after appropriate treatment initiation.
Do alcohol consumption and smoking affect alkaline phosphatase readings?
Yes, both lifestyle factors can significantly influence ALP levels. Chronic heavy alcohol consumption induces hepatic enzyme proliferation, directly upregulating ALP production and often causing concurrent GGT elevation even in the absence of overt cirrhosis. Similarly, tobacco smoke contains numerous hepatotoxic compounds that stimulate bile duct proliferation and impair detoxification pathways, leading to mild-to-moderate ALP increases in regular smokers. Reducing or eliminating these exposures often results in measurable decreases in enzyme levels within 6 to 12 weeks, alongside improved overall hepatic and cardiovascular markers.
Is a high ALP level a reliable standalone indicator of cancer?
No, an isolated high ALP level is not diagnostic of cancer and should never be interpreted as such without comprehensive clinical correlation. While malignancies involving the liver, bones, biliary tract, or metastatic disease frequently elevate ALP, countless benign conditions—including gallstones, vitamin deficiencies, healing fractures, pregnancy, and medication effects—produce identical laboratory findings. Cancer diagnosis requires histopathological confirmation, advanced imaging, tumor markers, and clinical staging. ALP merely serves as an initial screening indicator that prompts physicians to investigate underlying tissue pathology more thoroughly.
Conclusion
Understanding what level of alkaline phosphatase is dangerous requires moving beyond isolated numbers and embracing a holistic, clinically contextualized approach. ALP serves as a vital biomarker reflecting the functional status of the liver, bones, and several other organ systems, but its true diagnostic value emerges only when interpreted alongside patient history, physical examination findings, and complementary laboratory tests. Mild elevations frequently resolve spontaneously or stem from benign physiological states, while moderate to severe elevations—especially those exceeding 500 or 1000 IU/L—demand prompt, systematic evaluation to identify serious hepatobiliary, skeletal, or systemic pathologies.
The diagnostic journey typically begins with determining the enzyme's origin through GGT testing and isoenzyme fractionation, followed by targeted imaging, metabolic panels, and specialist referrals when necessary. Whether addressing biliary obstruction, managing bone turnover disorders, correcting nutritional deficiencies, or adjusting medication regimens, early intervention significantly improves outcomes and prevents irreversible tissue damage. Low ALP levels, though less commonly discussed, warrant equal attention as they can reveal rare genetic disorders, severe malnutrition, or endocrine dysfunction requiring specialized management.
Ultimately, an abnormal ALP result should be viewed as an actionable clinical signal rather than a definitive verdict. By partnering with healthcare providers, adhering to recommended follow-up testing, addressing modifiable lifestyle factors, and staying informed about the physiological mechanisms driving your results, you can navigate laboratory abnormalities with confidence and clarity. Regular monitoring, timely diagnostic workups, and personalized therapeutic strategies remain the gold standards for transforming a confusing lab value into a clear roadmap toward restored health and long-term wellness.

About the author
Fatima Al-Jamil, MD, MPH, is board-certified in gastroenterology and hepatology. She is an Assistant Professor of Medicine at a university in Michigan, with a clinical focus on inflammatory bowel disease (IBD) and motility disorders.