Rosy Cheeks: From a Healthy Glow to a Health Concern

Key points
- Emotional Responses: Strong emotions like excitement, embarrassment, anxiety, or stress can trigger the sympathetic nervous system, causing a blush. This evolutionary response, known as erythrophobia in extreme cases, is linked to the fight-or-flight mechanism. The release of adrenaline and cortisol primes the cardiovascular system, inadvertently dilating facial capillaries. Unlike other areas of the body, facial blood vessels possess unique adrenergic receptors that respond to emotional cues, making the face the primary stage for involuntary emotional signaling.
- Physical Exertion and Environment: Exercise increases blood flow to cool the body down, resulting in a healthy flush. Similarly, exposure to cold weather causes the body to push warm blood to the skin's surface, while hot weather or a hot shower widens vessels to release heat. The face lacks insulating fat layers and has a high density of thermosensitive TRP (transient receptor potential) channels, making it particularly reactive to temperature shifts. Gradual acclimatization and proper layering can help moderate these environmental flushes.
- Food and Drink: Consuming spicy foods, hot beverages, or alcohol can cause temporary flushing. Capsaicin in chili peppers activates TRPV1 receptors, tricking the nervous system into releasing vasodilatory peptides. Similarly, hot liquids increase core temperature, prompting a cooling response. Some people experience an "alcohol flush reaction" due to an inherited enzyme deficiency that makes it difficult to metabolize alcohol, as noted by Healthline. This condition, common in East Asian populations, stems from an ALDH2 gene mutation that leads to acetaldehyde accumulation, causing rapid facial redness, nausea, and increased heart rate.
The Allure and Alarm of Rosy Cheeks: More Than Just a Blush
Rosy cheeks have a captivating duality. For centuries, they've been celebrated as a sign of robust health and vitality. In Charlotte Brontë’s novel Jane Eyre, the protagonist laments not having "rosy cheeks," a coveted trait of beauty. Fast forward to today, and a delicate flush is a staple on the red carpet, a sign of youthfulness and radiance. Yet, for many, that same redness can be a source of discomfort and concern—a "problematic flush" that signals anything from social anxiety to a chronic medical condition.
This phenomenon sits at the intersection of dermatology, neurology, and immunology. At its core, facial redness is a visible manifestation of cutaneous vasodilation. The facial skin is uniquely rich in blood vessels, and the neurovascular network governing these vessels is highly responsive to internal and external stimuli. When arterioles dilate, increased blood flow brings oxygen and nutrients closer to the epidermis, creating the characteristic pink or red hue. While this mechanism serves vital thermoregulatory and communicative functions, chronic or inappropriate activation can disrupt the skin barrier, cause psychological distress, and point to systemic pathology. Understanding when to celebrate a healthy glow and when to seek clinical intervention requires a nuanced approach to skin health.
This article delves into the multifaceted world of rosy cheeks, synthesizing information from leading health experts to help you differentiate a harmless blush from a health warning, explore management options, and understand the cultural perceptions behind this common phenomenon.
What Causes Rosy Cheeks? Differentiating Harmless Flushing from Health Concerns
Understanding the cause of your rosy cheeks is the first step toward managing them. The redness is caused by blood vessels near the skin's surface widening, allowing more blood to flow through. The key is to determine what's triggering this reaction. Facial vasodilation is primarily mediated by the autonomic nervous system, specifically through sympathetic adrenergic and cholinergic pathways, as well as local release of nitric oxide and neuropeptides like substance P. When these signaling pathways activate, smooth muscle cells in the vessel walls relax, leading to increased perfusion and visible erythema.
Benign and Temporary Causes of a Healthy Flush
In most cases, rosy cheeks are a temporary and harmless physiological response. This benign flushing typically resolves on its own once the trigger is removed. It's important to recognize that transient redness is a normal part of human physiology and often indicates a well-functioning circulatory and nervous system.
- Emotional Responses: Strong emotions like excitement, embarrassment, anxiety, or stress can trigger the sympathetic nervous system, causing a blush. This evolutionary response, known as erythrophobia in extreme cases, is linked to the fight-or-flight mechanism. The release of adrenaline and cortisol primes the cardiovascular system, inadvertently dilating facial capillaries. Unlike other areas of the body, facial blood vessels possess unique adrenergic receptors that respond to emotional cues, making the face the primary stage for involuntary emotional signaling.
- Physical Exertion and Environment: Exercise increases blood flow to cool the body down, resulting in a healthy flush. Similarly, exposure to cold weather causes the body to push warm blood to the skin's surface, while hot weather or a hot shower widens vessels to release heat. The face lacks insulating fat layers and has a high density of thermosensitive TRP (transient receptor potential) channels, making it particularly reactive to temperature shifts. Gradual acclimatization and proper layering can help moderate these environmental flushes.
- Food and Drink: Consuming spicy foods, hot beverages, or alcohol can cause temporary flushing. Capsaicin in chili peppers activates TRPV1 receptors, tricking the nervous system into releasing vasodilatory peptides. Similarly, hot liquids increase core temperature, prompting a cooling response. Some people experience an "alcohol flush reaction" due to an inherited enzyme deficiency that makes it difficult to metabolize alcohol, as noted by Healthline. This condition, common in East Asian populations, stems from an ALDH2 gene mutation that leads to acetaldehyde accumulation, causing rapid facial redness, nausea, and increased heart rate.
 Source: Getty Images
Source: Getty Images
Beyond these common triggers, certain skincare practices can inadvertently cause flushing. Over-exfoliation, particularly with high-percentage glycolic or salicylic acids, compromises the stratum corneum, leaving underlying vasculature exposed and reactive. Additionally, sudden changes in humidity or altitude can alter cutaneous blood flow as the body adjusts to varying oxygen levels and atmospheric pressure. For most individuals, these benign flushes subside within 30 to 90 minutes once the stimulus is removed, requiring no medical intervention beyond gentle soothing and hydration.
When Rosy Cheeks Signal an Underlying Medical Condition
If your facial redness is persistent, recurrent, or accompanied by other symptoms, it may be a sign of an underlying medical issue. It's crucial to pay attention to these patterns to seek timely care. Clinical differentiation relies on evaluating the duration of redness, its distribution pattern, associated symptoms like burning or scaling, and response to environmental factors. Persistent erythema that lasts for hours or days, or that appears alongside textural changes, warrants professional evaluation. Dermatologists often utilize standardized photography, patient diaries, and sometimes vascular imaging or skin biopsies to confirm diagnoses. Early intervention is particularly important for inflammatory conditions, as untreated chronic redness can lead to permanent vascular changes and compromised skin barrier function.
Rosacea: The Most Common Culprit
Rosacea is a chronic and progressive inflammatory skin condition that affects millions worldwide. It often begins as a tendency to flush easily but can evolve to include:
- Persistent facial redness, especially on the cheeks, nose, and forehead.
- Small, red, pus-filled bumps that resemble acne.
- Visible broken blood vessels (telangiectasia).
- A burning or stinging sensation.
- In some cases, thickening of the skin, particularly on the nose (rhinophyma).
The pathophysiology of rosacea involves complex neurovascular dysregulation, innate immune system overactivation, and an altered skin microbiome. Research has identified elevated levels of antimicrobial peptides like cathelicidin and the protease enzyme KLK5 in rosacea-prone skin, which contribute to inflammation and vascular instability. Additionally, Demodex folliculorum mites, which naturally inhabit human hair follicles, are often found in higher densities in rosacea patients, potentially triggering an inflammatory cascade. Clinically, rosacea is classified into four subtypes: erythematotelangiectatic (persistent redness and visible vessels), papulopustular (inflammatory bumps), phymatous (skin thickening), and ocular (eye involvement). The ocular subtype, often overlooked, presents with dryness, grittiness, and blepharitis, and requires coordinated care between dermatologists and ophthalmologists.
Diagnosing rosacea in skin of color can be challenging, as the redness may present as a dusky brown or violet hue, and there is a higher risk of post-inflammatory hyperpigmentation. Clinicians often rely more on patient-reported symptoms like stinging, scaling, and papular eruptions rather than visible erythema in Fitzpatrick skin types IV-VI. Misdiagnosis is common, with rosacea frequently mistaken for acne or lupus, leading to inappropriate treatments that exacerbate the condition.
Other Skin Conditions
While rosacea dominates the clinical landscape of persistent facial redness, several other dermatological conditions present similarly and require distinct management strategies.
- Acne: Widespread inflammatory acne can cause significant redness and irritation across the cheeks. The redness stems from the immune response to Cutibacterium acnes bacteria and the rupture of comedonal walls. Unlike rosacea, acne typically features prominent blackheads, whiteheads, and deeper cystic lesions that are not usually accompanied by immediate burning or temperature-sensitive flushing. Topical retinoids and benzoyl peroxide form the cornerstone of treatment, but they can initially increase redness and peeling.
- Contact Dermatitis & Eczema: Allergic reactions to skincare products or environmental irritants can cause red, itchy, and swollen skin. Atopic dermatitis (eczema) can also cause chronic red patches on the face. Allergic contact dermatitis is a type IV hypersensitivity reaction mediated by T-cells, often triggered by fragrances, preservatives like methylisothiazolinone, or certain botanical extracts. Facial eczema frequently presents with severe pruritus, lichenification, and fine scaling along the hairline or perioral region. Patch testing is the gold standard for identifying specific allergens.
- Sunburn: Overexposure to UV rays is a common cause of red, inflamed skin. UV radiation damages keratinocyte DNA, triggering the release of inflammatory prostaglandins and causing painful erythema within hours of exposure. Chronic sun damage, or photoaging, can also lead to persistent facial telangiectasias and mottled redness that requires targeted photoprotection and laser intervention.
- Perioral Dermatitis: Often misdiagnosed as rosacea or acne, this condition features small red papules clustered around the mouth, nose, and sometimes eyes. It is frequently triggered or worsened by prolonged topical corticosteroid use, heavy moisturizers, or fluoride-containing toothpaste. Treatment typically involves discontinuation of offending products and a course of topical or oral antibiotics.
Systemic and Internal Health Issues
Sometimes, rosy cheeks are an external sign of an internal issue. Facial flushing can serve as a clinical biomarker for systemic inflammation, endocrine disruption, or autonomic dysfunction. Recognizing these systemic links is essential for comprehensive patient care.
- Hormonal Changes: Hot flashes during menopause are a well-known cause of sudden, intense facial flushing. The decline in estrogen levels disrupts thermoregulatory centers in the hypothalamus, causing inappropriate vasodilation. These episodes can occur multiple times daily and are often accompanied by night sweats, sleep disturbances, and mood fluctuations. Hormone replacement therapy (HRT), SSRIs, or gabapentin may be prescribed for severe cases.
- Infections: Certain illnesses are known for causing a characteristic facial rash. Fifth disease, a common viral infection in children, is nicknamed "slapped cheek syndrome" for the bright red rash it causes on the cheeks. Caused by parvovirus B19, it typically follows mild flu-like symptoms and spreads via respiratory droplets. In immunocompromised individuals or pregnant women, monitoring is essential. Bacterial infections like scarlet fever can also lead to flushed cheeks. This Streptococcus pyogenes infection presents with a fine, sandpaper-like body rash, strawberry tongue, and circumoral pallor, requiring prompt antibiotic therapy to prevent rheumatic complications.
- Autoimmune Conditions: Lupus can cause a distinctive butterfly-shaped (malar) rash across the cheeks and bridge of the nose. Unlike rosacea, the lupus malar rash typically spares the nasolabial folds, is photosensitive, and may be accompanied by systemic symptoms like joint pain, fatigue, and renal involvement. Diagnosis involves antinuclear antibody (ANA) testing, anti-dsDNA assays, and complement level monitoring.
- Medication Side Effects: A wide range of medications, from blood pressure drugs to high doses of niacin (Vitamin B3), can list flushing as a side effect. Calcium channel blockers, ACE inhibitors, and nitrates induce vasodilation as part of their therapeutic mechanism. Niacin flush occurs through prostaglandin-mediated pathways and can be mitigated by premedicating with aspirin or using extended-release formulations. Other culprits include corticosteroids, certain antidepressants, and thyroid hormone replacements.
- Rare Conditions: In rare instances, persistent flushing can be a sign of more serious conditions like Cushing's syndrome or carcinoid tumors, which are typically accompanied by other significant symptoms. Carcinoid syndrome results from serotonin-secreting neuroendocrine tumors, causing episodic flushing, diarrhea, wheezing, and right-sided valvular heart disease. Mast cell activation syndrome (MCAS) and pheochromocytoma are additional rare causes, each requiring specialized endocrinological or immunological workups.
 Source: UNC Health Talk
Source: UNC Health Talk
Managing and Treating Red Cheeks: A Tailored Approach
The right management strategy depends entirely on the underlying cause of your rosy cheeks. A personalized approach, often guided by a dermatologist, yields the best results. Effective management blends barrier restoration, trigger avoidance, targeted pharmacotherapy, and procedural interventions when indicated. Patients should be counseled that facial redness rarely resolves overnight; consistency and patience are crucial, particularly for neurovascular conditions like rosacea.
At-Home Care and Lifestyle Adjustments
For many, managing redness begins with simple lifestyle changes. The foundation of at-home care revolves around minimizing cutaneous stress and supporting the skin's natural repair mechanisms.
- Gentle Skincare: Use a mild, non-abrasive cleanser and lukewarm water. Avoid harsh exfoliants, toners, and astringents. Look for formulations labeled "fragrance-free" and "non-comedogenic." Incorporate barrier-repairing ingredients such as ceramides, fatty acids, and cholesterol, which mimic the skin's natural lipid matrix. Niacinamide, at concentrations below 5%, can help strengthen the barrier and reduce transepidermal water loss, though higher concentrations may cause flushing in sensitive individuals. Limit cleansing to twice daily to prevent stripping natural oils.
- Sun Protection: Sun exposure is a major trigger for conditions like rosacea. Daily use of a broad-spectrum sunscreen with an SPF of 30 or higher is non-negotiable. Mineral sunscreens containing zinc oxide or titanium dioxide are often better tolerated by reactive skin than chemical filters like avobenzone or oxybenzone, which can generate heat upon UV absorption. Apply sunscreen 15 minutes before sun exposure, reapply every two hours, and consider tinted formulations containing iron oxides, which block visible light that can worsen hyperpigmentation and erythema.
- Identify and Avoid Triggers: Keep a diary to track flare-ups. Common triggers include spicy foods, alcohol, extreme temperatures, and stress. Avoiding them can significantly reduce flushing episodes. When using a trigger diary, note the specific time, environmental conditions, food/drink consumed, stress levels, and skincare products used prior to a flare. Over a 4-6 week period, patterns usually emerge, allowing for precise lifestyle modifications. Stress management techniques such as diaphragmatic breathing, progressive muscle relaxation, and cognitive behavioral therapy can dampen the sympathetic nervous system's overactive response.
Medical Treatments for Persistent Redness
If at-home care isn't enough, a doctor may recommend medical treatments. These interventions target specific pathways of inflammation, vascular reactivity, or microbial imbalance.
- Topical Medications: Creams and gels like brimonidine (Mirvaso) and oxymetazoline (Rhofade) work by constricting blood vessels to reduce redness. Brimonidine is an alpha-2 adrenergic agonist that provides rapid but temporary relief, while oxymetazoline offers sustained reduction with a lower risk of rebound erythema. Anti-inflammatory topicals like metronidazole and azelaic acid can help with the bumps associated with rosacea. Azelaic acid also possesses antimicrobial and keratolytic properties, making it effective for both papulopustular rosacea and comorbid hyperpigmentation. Ivermectin cream (Soolantra) has emerged as a highly effective option for reducing Demodex mite populations and associated inflammation.
- Oral Medications: Oral antibiotics, such as doxycycline, are often prescribed in low doses for their anti-inflammatory effects. Subantimicrobial dose doxycycline (40 mg) inhibits matrix metalloproteinases without disrupting the gut microbiome. For severe, refractory cases, oral isotretinoin may be considered at low doses to reduce sebaceous gland activity and inflammation, though it requires strict monitoring for teratogenicity and lipid changes.
- Laser and Light Therapy: Treatments like Intense Pulsed Light (IPL) can effectively reduce persistent redness and visible blood vessels. Vascular lasers, particularly pulsed dye laser (PDL) and Nd:YAG, target hemoglobin in dilated vessels, causing selective photothermolysis and vessel collapse. These procedures should be performed by an experienced professional, especially on skin of color, to minimize risks of hyperpigmentation. Pre- and post-treatment care includes strict sun avoidance, discontinuation of photosensitizing medications, and application of cooling gels. Typically, 3-5 sessions spaced 4-6 weeks apart yield optimal results, with maintenance treatments needed every 12-18 months.
Special Considerations for Diverse Demographics
Dermatology is not one-size-fits-all. Ethnicity, age, gender, and physiological life stages dramatically influence how redness presents and how it should be managed.
- Treating Rosy Cheeks in Skin of Color: As mentioned, diagnosis can be difficult. It is crucial to use gentle products and approach treatments like laser therapy with caution to prevent scarring or changes in pigmentation. Clinicians must account for higher risks of keloid formation and post-inflammatory hyperpigmentation. Topical azelaic acid and clindamycin are preferred first-line agents. When using energy-based devices, longer wavelengths (e.g., 1064 nm Nd:YAG) and lower fluences with extended pulse durations are utilized to safely target vasculature while sparing melanin-rich epidermal cells.
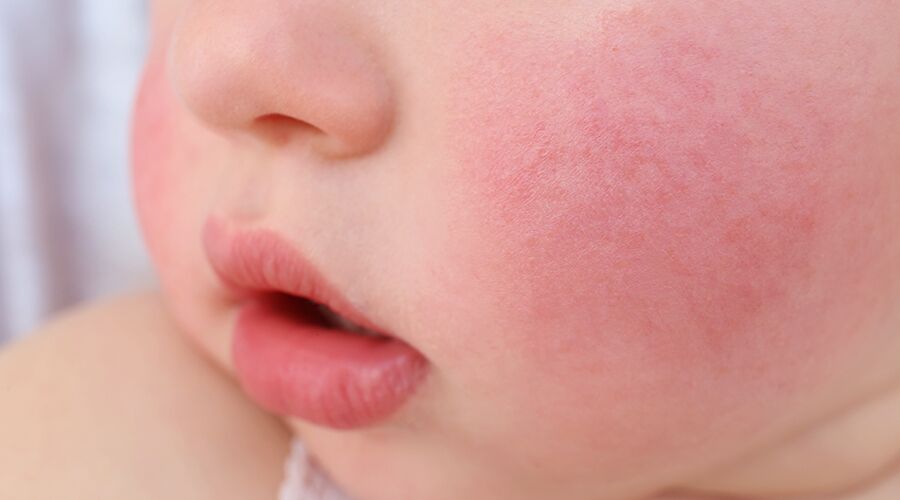
- Addressing Red Cheeks in Babies and Children: Red cheeks in young children are often caused by teething, infections like Fifth Disease, or skin sensitivity. Infant skin has a thinner stratum corneum and underdeveloped barrier function, making it highly susceptible to irritation from drool, friction, and harsh detergents. Management focuses on gentle moisturizers containing colloidal oatmeal or petroleum jelly, lukewarm baths, and treating the underlying illness when necessary. Always consult a pediatrician if you are concerned, especially if redness is accompanied by fever, lethargy, or feeding difficulties.
- Hormonal and Life Stage Variations: Pregnancy can induce melasma and vascular changes due to elevated estrogen and progesterone, often termed the "pregnancy mask." Men experiencing andropause may notice altered skin thickness and vascular responsiveness. Perimenopausal women frequently require combined hormonal and dermatological strategies to manage vasomotor flushing alongside declining skin collagen and hydration.
The Cultural View: A Healthy Glow or a Problematic Flush?
The perception of rosy cheeks is deeply rooted in our culture and psychology, creating a stark contrast between a desired "glow" and a stigmatized "flush." This duality influences how individuals perceive their own skin and how society interprets facial coloration. Throughout art history, Renaissance paintings frequently depicted healthy youth and nobility with pronounced vermilion cheeks, utilizing pigments like cinnabar or vermilion to symbolize blood vitality, fertility, and social standing. In contrast, pale complexions were often associated with illness, indoor confinement, or lower social class.
The Symbol of Health and Attractiveness
As highlighted by research summarized in Psychology Today, a rosy complexion is often perceived as a sign of good circulation, oxygenation, and overall health. This evolutionary cue links redness with vitality and fertility, making it an attractive feature. Modern evolutionary psychology suggests that facial coloration acts as an honest signal of cardiovascular fitness and immune competence. The beauty industry capitalizes on this, with blush being a cosmetic staple used to mimic this natural, healthy flush. Contemporary makeup trends, from the "clean girl" aesthetic to Korean glass skin routines, emphasize luminous, well-circulated-looking complexions, driving demand for tinted moisturizers, liquid cheek stains, and hydrating primers that enhance underlying vascularity without masking it.
The Stigma and Social Anxiety of Blushing
On the flip side, an involuntary and uncontrollable flush—blushing—can be a source of intense social anxiety. It makes a private emotion public, often leading to a vicious cycle where the fear of blushing itself becomes a trigger. This "problematic flush" is not seen as a sign of vitality but as a marker of discomfort, shame, or a lack of composure, causing significant psychological distress for many. Erythrophobia, the pathological fear of blushing, can severely impair professional interactions, romantic relationships, and public speaking engagements. Cognitive-behavioral therapy (CBT), exposure therapy, and in severe cases, beta-blockers or endoscopic thoracic sympathectomy (ETS), are employed to manage this condition. Normalizing facial redness as a universal human experience, rather than a flaw, is an ongoing cultural shift supported by dermatologists and mental health professionals alike.
Conclusion: Understanding Your Unique Glow
Rosy cheeks are a complex and personal experience. For some, they are a fleeting blush, a sign of a brisk walk or a moment of joy. For others, they are a chronic condition requiring careful management. The key is to pay attention to your body. By understanding the context—whether the redness is temporary or persistent, isolated or accompanied by other symptoms—you can determine whether it's a simple glow to be embraced or a signal to consult a healthcare professional.
Navigating facial redness requires a balance of self-advocacy and clinical guidance. Start by observing patterns, maintaining a gentle skincare routine, and documenting potential triggers. If over-the-counter adjustments fail, or if redness progresses to burning, textural changes, or systemic symptoms, seek evaluation from a board-certified dermatologist. Advances in targeted topicals, neurovascular modulators, and vascular lasers have transformed the prognosis for chronic erythema. With the right diagnostic clarity and treatment plan, individuals can achieve a comfortable, healthy complexion that aligns with their unique physiology. Whether you're managing a fleeting blush or a chronic dermatological condition, remember that facial redness is a natural human variation, not a defect, and with informed care, it can be effectively understood and managed.
References:
- Healthline: Rosy Cheeks, Rosacea, or Something Else? Tips for Identification
- Medical News Today: Warm, red, or rosy cheeks: Causes and what to do
- National Health Service (UK): Blushing
- Psychology Today: What Makes a Face Beautiful?
Frequently Asked Questions
How can I tell if my rosy cheeks are just blushing or something more serious like rosacea?
The primary differentiator lies in duration and accompanying symptoms. Benign blushing typically fades within 30 to 90 minutes once the emotional, thermal, or dietary trigger is removed. Rosacea, however, presents with persistent background redness that may last for hours, days, or weeks without fully resolving. Additionally, rosacea is often accompanied by secondary symptoms such as visible telangiectasias (spider veins), burning or stinging sensations, acne-like papules or pustules, and heightened sensitivity to skincare products. If your redness becomes a baseline condition rather than a transient reaction, or if it worsens despite trigger avoidance, it warrants professional dermatological evaluation.
What ingredients should I avoid in my skincare routine if I have sensitive, red-prone cheeks?
If your facial skin is prone to persistent redness or flushing, it is advisable to avoid formulations containing high concentrations of alcohol denat, synthetic fragrances, essential oils (like peppermint, eucalyptus, or citrus), and harsh physical exfoliants such as crushed nut shells or coarse salt. Additionally, strong chemical exfoliants like high-percentage glycolic acid (above 10%) or frequent salicylic acid peels can compromise the skin barrier. Sulfates (SLS/SLES) in cleansers can strip natural lipids, exacerbating erythema. Opt for fragrance-free, pH-balanced, and barrier-supportive formulations. When introducing active ingredients like retinoids or vitamin C, start with low concentrations and apply the "sandwich method" (moisturizer-actives-moisturizer) to mitigate irritation.
Can diet significantly impact facial redness and flushing?
Yes, diet plays a substantial role in modulating cutaneous vascular responses. Foods and beverages high in histamine (aged cheeses, fermented foods, processed meats, red wine) or tyramine can trigger neurovascular flushing in sensitive individuals. Spicy foods containing capsaicin directly stimulate TRPV1 pain and heat receptors, leading to vasodilation. Hot liquids increase core body temperature, prompting a thermoregulatory flush. Alcohol, particularly red wine and beer, contains vasodilatory compounds and sulfites that can exacerbate redness. Keeping a detailed food diary can help identify personal dietary triggers. Conversely, incorporating anti-inflammatory foods rich in omega-3 fatty acids, antioxidants, and polyphenols (such as leafy greens, fatty fish, and green tea) may help support overall skin barrier integrity and reduce baseline inflammation over time.
Are there effective natural or over-the-counter remedies for persistent red cheeks?
While natural remedies can complement clinical treatment, they rarely resolve chronic inflammatory or vascular conditions on their own. That said, several over-the-counter approaches have demonstrated efficacy. Centella asiatica (cica) and allantoin are clinically shown to soothe irritation and promote barrier repair. Green tea extract (EGCG) and licorice root extract possess anti-inflammatory and mild vasoconstrictive properties that can calm erythema. Colloidal oatmeal provides immediate relief from itching and burning by forming a protective film. For visible capillaries, topical vitamin K and arnica are marketed, though clinical evidence remains limited compared to prescription alpha-adrenergic agonists or laser therapy. Consistent use of mineral sunscreen remains the most effective OTC intervention for preventing UV-induced worsening of facial redness.
When should I see a dermatologist versus a primary care physician for rosy cheeks?
Primary care physicians are excellent for initial assessment, particularly when systemic causes like infections, hormonal fluctuations, or medication side effects are suspected. They can order basic blood work, manage common allergic reactions, and prescribe first-line treatments. However, you should seek a board-certified dermatologist if the redness is chronic, worsening, or unresponsive to initial therapies; if it is accompanied by textural changes like thickening, scaling, or pustules; if you require prescription-strength topicals, oral antibiotics, or procedural interventions like laser therapy; or if you suspect rosacea, lupus, or perioral dermatitis, which require specialized diagnostic criteria and nuanced management strategies. Dermatologists also have access to patch testing for contact allergens and advanced vascular imaging tools.

About the author
Elena Vance, MD, is a double board-certified dermatologist and pediatric dermatologist. She is an assistant professor of dermatology at a leading medical university in California and is renowned for her research in autoimmune skin disorders.