Can a Loop Recorder Detect a Heart Attack? The Complete Answer

Key points
- Arrhythmias: Irregular heartbeats that can be too fast (tachycardia), too slow (bradycardia), or erratic.
- Atrial Fibrillation (AFib): A common arrhythmia that significantly increases the risk of stroke.
- Syncope (Fainting): To determine if an abnormal heart rhythm is causing fainting spells.
- Unexplained Palpitations: To correlate the feeling of a racing or fluttering heart with actual electrical events.
- Cryptogenic Stroke: To find hidden arrhythmias like AFib that may have caused a stroke.
If you have an implantable loop recorder or are considering one, you might wonder about its capabilities, especially during a cardiac emergency. A common and critical question is: can a loop recorder detect a heart attack?
The short and direct answer is no, a loop recorder is not designed to directly detect a heart attack.
While this may seem surprising, the reason lies in the fundamental difference between what a loop recorder monitors and what a heart attack is. A loop recorder is an electrical detective, while a heart attack is a plumbing crisis. This article will break down what a loop recorder does, how heart attacks are diagnosed, and explain the crucial—though indirect—role this device plays in your overall heart health.
Understanding the Loop Recorder's Primary Function
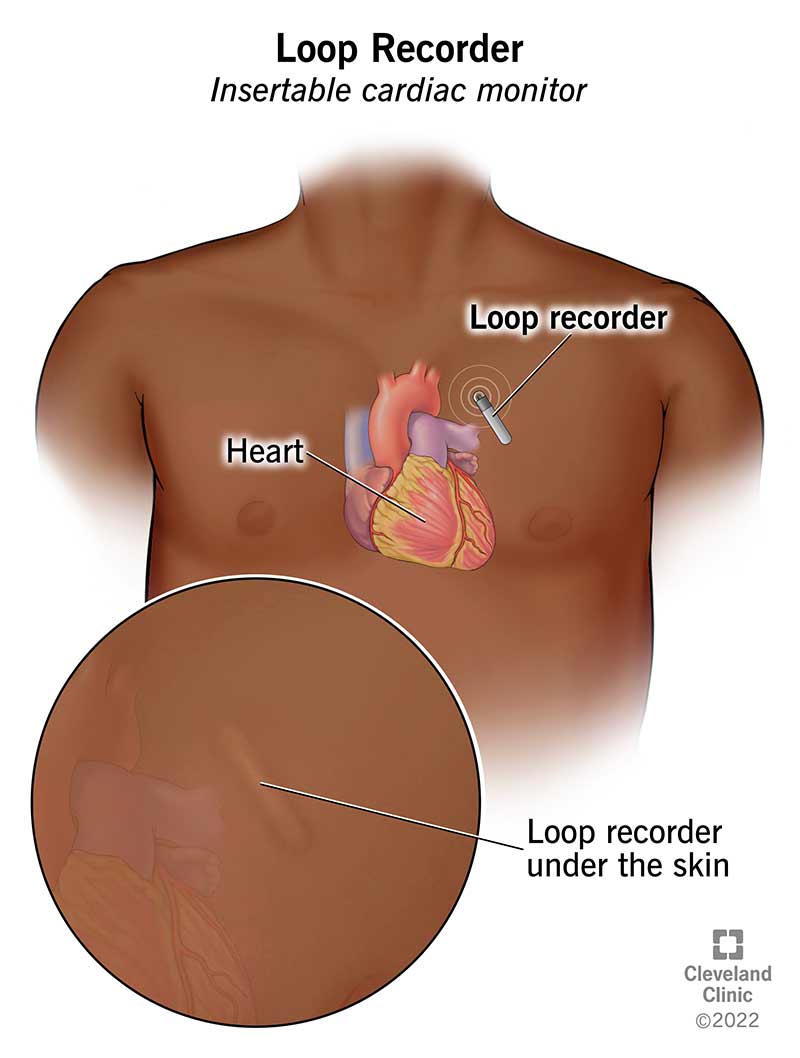
An implantable loop recorder (ILR), also known as an insertable cardiac monitor (ICM), is a small device, often the size of a USB stick, that is placed just under the skin of your chest. Its sole purpose is to continuously monitor and record your heart's electrical activity for up to three years.
Think of it as a long-term electrocardiogram (ECG). It's an invaluable diagnostic tool for capturing infrequent heart rhythm problems that shorter tests might miss.
According to experts at the Cleveland Clinic, cardiologists use loop recorders to identify the cause of unexplained symptoms and diagnose specific conditions, including:
- Arrhythmias: Irregular heartbeats that can be too fast (tachycardia), too slow (bradycardia), or erratic.
- Atrial Fibrillation (AFib): A common arrhythmia that significantly increases the risk of stroke.
- Syncope (Fainting): To determine if an abnormal heart rhythm is causing fainting spells.
- Unexplained Palpitations: To correlate the feeling of a racing or fluttering heart with actual electrical events.
- Cryptogenic Stroke: To find hidden arrhythmias like AFib that may have caused a stroke.
The device automatically records events when your heart rate goes above or below preset limits. You can also use a handheld activator to manually trigger a recording if you feel symptoms.
The term "loop" refers to how the device stores data. Unlike traditional monitors that erase old recordings, an ILR operates on a continuous loop buffer. It constantly records heart rhythm but only permanently saves data when a specific event is triggered—either automatically by programmed parameters or manually by the patient. This ensures that the exact sequence of electrical activity leading up to and following a symptomatic episode is captured in its entirety. Once the buffer is full, the oldest, non-episodic data is overwritten, allowing the device to function for years without running out of storage space.
Modern ILRs are equipped with sophisticated wireless transmission technology, typically using Bluetooth to communicate with a bedside transmitter or smartphone app. This enables remote patient monitoring (RPM), where encrypted data packets are automatically sent to a secure clinical server at regular intervals or after significant arrhythmic events. Your electrophysiology team can review these transmissions remotely, identifying trends or dangerous rhythms long before your next scheduled clinic visit. This real-time or near-real-time feedback loop transforms the ILR from a passive data collector into an active component of your cardiac care plan.
Why a Loop Recorder Cannot Directly Detect a Heart Attack
The key distinction lies in the nature of the problem. A loop recorder is designed to find electrical issues, but a heart attack (myocardial infarction) is a blood flow issue.
A heart attack occurs when a blockage, usually a blood clot, stops or severely reduces blood flow through a coronary artery. This deprives the heart muscle of oxygen, causing the tissue to be damaged or die.
As medical device manufacturer Medtronic clearly states, "No, an ICM, or loop recorder, can't detect a heart attack. An ICM only monitors the heart's rhythm."
While a severe heart attack can sometimes trigger a dangerous arrhythmia that the loop recorder would detect, the device is not built to identify the primary signs of a heart attack itself. The ILR uses a single pair of subcutaneous electrodes to capture a unidirectional electrical vector. While this is excellent for spotting rate and rhythm abnormalities like pauses, tachycardias, or AFib, it lacks the spatial resolution required to identify localized myocardial ischemia. Ischemic changes, such as ST-segment deviations or T-wave inversions, require a multi-lead configuration that maps the electrical activity across different anatomical planes of the heart. Without this comprehensive mapping, the subtle voltage shifts caused by reduced blood flow can easily be masked by normal respiratory variation, body position changes, or baseline signal noise.
Furthermore, heart attacks often develop gradually over hours as plaque ruptures and clot forms. During this prodromal phase, the heart's electrical rhythm frequently remains completely normal until the ischemia progresses enough to destabilize the cardiac conduction system. By then, significant muscle damage may already be occurring. An ILR's algorithms are specifically programmed to filter out non-arrhythmic data to preserve battery life and clinical relevance. It simply isn't calibrated to measure myocardial oxygenation, wall motion abnormalities, or biochemical markers of cell death—the true hallmarks of acute coronary syndrome.
How a Heart Attack Is Actually Diagnosed
Diagnosing a heart attack requires a different set of tools that provide a more detailed and immediate snapshot of the heart's condition. Emergency medical professionals rely on the following:
- 12-Lead Electrocardiogram (ECG/EKG): This is the gold standard for immediate diagnosis. Unlike the single-lead view of a loop recorder, a 12-lead ECG provides a comprehensive 3D view of the heart's electrical activity, allowing doctors to spot specific patterns (like ST-segment elevation) that indicate muscle damage from a lack of oxygen. The 12 leads look at the heart from multiple angles—frontal, horizontal, and sagittal—enabling clinicians to localize the affected coronary artery and determine the severity of the infarction.
- Blood Tests: When heart muscle is damaged, it releases specific proteins called cardiac markers into the bloodstream. Blood tests measuring troponin levels are highly accurate in confirming that a heart attack has occurred. Troponin I and Troponin T are regulatory proteins found almost exclusively in cardiac muscle cells. Even microscopic cell death causes a measurable spike in serum troponin. Modern high-sensitivity troponin assays can detect minuscule elevations within 1 to 3 hours of symptom onset, and serial testing over several hours helps differentiate acute myocardial infarction from other conditions that cause minor troponin leaks, such as myocarditis or heart failure exacerbation.
- Imaging Tests: An echocardiogram (ultrasound of the heart) can show if areas of the heart muscle are not contracting properly due to damage. Regional wall motion abnormalities are highly specific to ischemic territories. A coronary angiogram is an invasive procedure that uses X-ray imaging and contrast dye to visualize the coronary arteries directly, pinpointing the exact location and severity of the blockage. In many cases, percutaneous coronary intervention (PCI) is performed during the same session to deploy a stent and restore blood flow.
These methods are designed for acute, emergency situations, a role the long-term, diagnostic loop recorder is not meant to fill. The diagnostic pathway for myocardial infarction is highly time-sensitive, following established protocols like the TIMI (Thrombolysis in Myocardial Infarction) or GRACE risk scores, which integrate symptom duration, ECG findings, and biomarker levels to guide immediate therapeutic decisions.
The Important Indirect Role of a Loop Recorder in Heart Attack Scenarios
Just because a loop recorder can't detect a heart attack doesn't mean it's not valuable. In fact, it plays a vital indirect role in both preventing and managing complications related to heart attacks.
Before a Heart Attack: Identifying Risks
Some arrhythmias, like atrial fibrillation, can lead to the formation of blood clots in the heart. If a clot travels to a coronary artery, it can cause a heart attack. By detecting AFib early, a loop recorder allows your doctor to prescribe preventative treatments, such as blood-thinning medication, to reduce your risk.
Additionally, silent or subclinical arrhythmias identified by an ILR can prompt comprehensive cardiovascular risk assessments. Patients with documented bradyarrhythmias or frequent premature ventricular complexes (PVCs) may undergo advanced lipid profiling, coronary calcium scoring, or stress testing to evaluate underlying structural heart disease or coronary artery calcification. The ILR essentially acts as an early warning system, flagging electrical instability that often correlates with progressive vascular disease. Early intervention based on these electrical red flags—through statin therapy, blood pressure optimization, or antiplatelet agents—can significantly reduce the long-term probability of an acute coronary event.
After a Heart Attack: Monitoring for Complications
A heart attack can damage the heart's electrical system, making a person more susceptible to life-threatening arrhythmias. A loop recorder is an excellent tool for monitoring patients after a heart attack to ensure dangerous rhythms don't develop.
A case study published by the National Institutes of Health (NIH) highlights this. A patient with a previous heart attack collapsed, and his implanted loop recorder showed that the event was caused by a dangerous ventricular tachyarrhythmia. This data was critical for his doctors to implant a defibrillator (ICD) for secondary prevention.
Post-myocardial infarction scarring creates abnormal electrical pathways and areas of slowed conduction, forming the perfect substrate for re-entrant ventricular tachycardia. The first 48 hours post-MI carry the highest arrhythmic risk, but vulnerability persists for months to years as the heart remodels. While high-risk patients receive ICDs immediately, many fall into a "gray zone" where the benefit of an ICD isn't yet clear. In these cases, an ILR provides continuous surveillance. If the device captures sustained ventricular tachycardia, non-sustained runs, or profound conduction delays, clinicians can escalate therapy, adjust antiarrhythmic medications, or proceed with ICD placement before a catastrophic event occurs. This targeted monitoring strategy prevents unnecessary device implants while ensuring high-risk patients receive timely protection.
*Understanding Implantable loop recorders, British Heart Foundation*Patient Protocol: What to Do If You Have a Loop Recorder and Suspect a Heart Attack
This is the most important takeaway for anyone with an implantable cardiac device. The presence of a loop recorder does not change emergency protocol.
If you experience symptoms of a heart attack—such as chest pain, shortness of breath, pain radiating to your arms or jaw, or sudden sweating—you must call 911 immediately.
Do not wait for the loop recorder to trigger an alert or waste time trying to activate it. A heart attack is a time-sensitive medical emergency where every second counts. While you can activate the recorder if possible, your first and only priority should be to seek immediate medical help. The data from your device can be reviewed by your cardiologist later.
When emergency medical services (EMS) arrive, explicitly inform them that you have an implanted loop recorder. While ILRs do not interfere with defibrillators or standard emergency interventions, having this information in your medical chart and verbally communicated ensures seamless care. Once you are stabilized at the hospital, your cardiology team can interrogate the device using a specialized wand or programmer to download recent rhythm strips. This data can provide crucial context for your acute care team—for example, confirming whether your symptoms were accompanied by an arrhythmia, helping to rule out syncope, or establishing baseline rhythm prior to treatment. However, this data review is always performed after acute life-saving interventions have been initiated.
Additionally, keep a wallet card or set a medical ID on your smartphone indicating the device make, model, implantation date, and your cardiologist's contact information. This simple step dramatically reduces delays during emergency care and ensures that hospital technicians can properly interface with your specific device model during subsequent evaluations.
Loop Recorder Limitations and Considerations
To have a complete picture, it's important to understand the device's limitations. A loop recorder:
- Only records heart rhythm, not blood pressure or other vital signs.
- Requires a minor surgical procedure for implantation, which carries small risks of infection, pain, or bruising at the site.
- Has a limited battery life, typically around three years, after which it may need to be removed or replaced.
Beyond these foundational constraints, patients should be aware of several practical considerations. Subcutaneous ECG signals are more susceptible to myopotential interference—electrical noise generated by skeletal muscle contraction, especially in the chest and shoulder regions. Vigorous exercise, heavy lifting, or even prolonged stretching can occasionally mimic tachyarrhythmias, leading to false-positive alerts. Modern ILR algorithms have significantly improved noise rejection, but they aren't infallible. Patients are typically advised to avoid extreme upper body strain during the first few weeks of healing and to report unexplained alerts to their clinical team for algorithm adjustment.
Environmental electromagnetic interference, while rare with modern shielding, can theoretically occur near strong magnetic fields or high-voltage industrial equipment. Standard consumer electronics like microwaves, cell phones, and home security systems pose no risk. Additionally, while most ILRs are MRI-conditional, specific scanning protocols must be followed, and the device may need to be temporarily deactivated during the procedure. Always carry your device identification card and share it with radiology staff before any imaging studies.
Finally, psychological adjustment is an often-overlooked aspect of ILR therapy. Knowing a device is continuously monitoring your heart can trigger anxiety or somatic hyperawareness, particularly in patients who have experienced cardiac trauma. Open communication with your care team, combined with patient education on device functionality and data transmission schedules, helps normalize the experience and transforms the ILR from a source of worry into a tool of empowerment.
Living with an Implantable Loop Recorder: Remote Monitoring and Long-Term Management
Successful long-term management of an implantable loop recorder hinges on patient adherence, technological integration, and consistent clinical follow-up. The remote monitoring ecosystem that accompanies modern ILRs is designed to be seamless. Most systems require you to place a transmitter on your nightstand, which automatically syncs with your device while you sleep. If your clinic uses a smartphone-based platform, you'll download a dedicated app that pairs with the recorder via Bluetooth. Data uploads are encrypted and compliant with HIPAA regulations, ensuring your cardiac information remains secure.
Routine clinical visits typically occur every 3 to 6 months, though heavily monitored patients may have shorter intervals initially. During these appointments, your care team will assess battery status, lead impedance, signal quality, and review all transmitted episodes. They will adjust detection thresholds if necessary—raising the minimum rate threshold to reduce false tachycardia alerts from exercise, or fine-tuning pause detection parameters. Proper calibration significantly enhances the diagnostic yield and minimizes unnecessary clinic calls.
Lifestyle considerations for ILR patients are minimal. You can resume normal activities, travel internationally, exercise, and work without restrictions once the incision site has healed. Airport security scanners will not damage the device, but you may trigger the metal detector. Present your device card to security personnel and request a hand wand or pat-down instead. Avoid placing strong magnets directly over the implant site, as they can temporarily inhibit device transmissions or cause unintended mode switches, though this does not harm the device itself.
Nutrition, medication adherence, and cardiovascular risk factor modification remain the cornerstone of heart health management alongside ILR therapy. The recorder provides critical data, but it does not replace healthy lifestyle choices, blood pressure control, cholesterol management, or diabetes optimization. Treat the ILR as a diagnostic ally that informs your broader treatment strategy, not as a substitute for proactive medical care.
Frequently Asked Questions (FAQ)
1. Can a loop recorder directly detect a heart attack? No, a loop recorder cannot directly detect a heart attack. Its primary function is to monitor the heart's electrical rhythm to detect arrhythmias (irregular heartbeats), not to identify the blockages in blood flow that cause a heart attack.
2. What is the main purpose of an implantable loop recorder? The main purpose of a loop recorder is long-term, continuous monitoring of the heart's electrical activity. It is used to diagnose the cause of infrequent symptoms like fainting (syncope), palpitations, or dizziness, and to detect arrhythmias such as atrial fibrillation (AFib).
3. How is a heart attack officially diagnosed? A heart attack is diagnosed using a combination of methods, primarily a 12-lead electrocardiogram (ECG/EKG) to see specific electrical changes, blood tests to measure cardiac enzymes like troponin released from damaged heart muscle, and imaging tests like an echocardiogram or coronary angiogram to assess heart function and identify blockages.
4. What should I do if I have a loop recorder and think I'm having a heart attack? If you have a loop recorder and experience symptoms of a heart attack (such as chest pain, shortness of breath, or pain radiating to your arm or jaw), you must call 911 or your local emergency number immediately. Do not rely on the loop recorder for a diagnosis or alert. Seeking emergency medical care is the top priority.
5. Can I get an MRI with an implantable loop recorder? Most modern implantable loop recorders are MRI-conditional, meaning they can safely undergo MRI scans under specific conditions. However, the device may need to be temporarily programmed to an MRI-safe mode before the scan, and certain scanning parameters (like magnet strength and coil type) must be strictly controlled by the radiology team. Always consult your cardiologist and provide the device ID card to imaging staff beforehand.
6. Will my loop recorder notify me if something abnormal happens? The ILR automatically transmits data to your clinical team during scheduled remote monitoring sessions or immediately following high-priority arrhythmic events, depending on your clinic's setup. It does not typically emit audible alarms to warn the patient. Your doctor's office will contact you if they review the data and find something requiring immediate medical attention. You should still seek emergency care yourself if you experience severe symptoms, rather than waiting for a callback.
7. How long does the implantation procedure take, and what is the recovery time? The implantation is a minimally invasive outpatient procedure that typically takes 15 to 30 minutes under local anesthesia. A small incision is made in the left chest area, a subcutaneous tunnel is created, and the device is inserted. You can usually go home the same day. Recovery involves keeping the site clean and dry for a few days, avoiding heavy lifting or vigorous arm movements for about 1 to 2 weeks, and watching for signs of infection. Full healing and return to unrestricted activity generally occur within 2 to 3 weeks.
References
- Medical News Today - Loop recorder: What it is, why doctors use it, and more
- Cleveland Clinic - How Loop Recorders Work
- Mayo Clinic - Implantable loop recorder: A heart monitoring device
- Medtronic - Can an insertable cardiac monitor (ICM) detect a heart attack?
- National Institutes of Health (NIH) - Aborted sudden cardiac death in a patient with implantable loop recorder
Conclusion
In summary, an implantable loop recorder is a highly specialized diagnostic tool engineered for long-term cardiac rhythm monitoring, not for the acute detection of myocardial infarctions. The fundamental disconnect lies in physiology: ILRs track the heart's electrical pathways, while heart attacks stem from obstructed coronary blood flow and subsequent tissue ischemia. Relying on a loop recorder to identify a heart attack is clinically inappropriate and potentially dangerous, as the device lacks the multi-lead mapping, biomarker analysis, and real-time ischemic detection required for acute coronary diagnosis.
However, the value of an ILR in comprehensive cardiovascular care cannot be overstated. Its true strength resides in its ability to capture elusive arrhythmias, guide preventive therapies like anticoagulation for AFib, and monitor post-infarction electrical stability to prevent sudden cardiac events. When integrated into a broader, proactive heart health strategy and paired with prompt emergency response protocols, the implantable loop recorder becomes an indispensable ally in both diagnosing complex cardiac conditions and safeguarding long-term heart health. Always treat unexplained chest pain, pressure, or radiating discomfort as a medical emergency, call 911 immediately, and let your healthcare team utilize the ILR's data as part of your ongoing, longitudinal cardiac care.

About the author
Marcus Thorne, MD, is a board-certified interventional cardiologist and a fellow of the American College of Cardiology. He serves as the Chief of Cardiology at a major metropolitan hospital in Chicago, specializing in minimally invasive cardiac procedures.